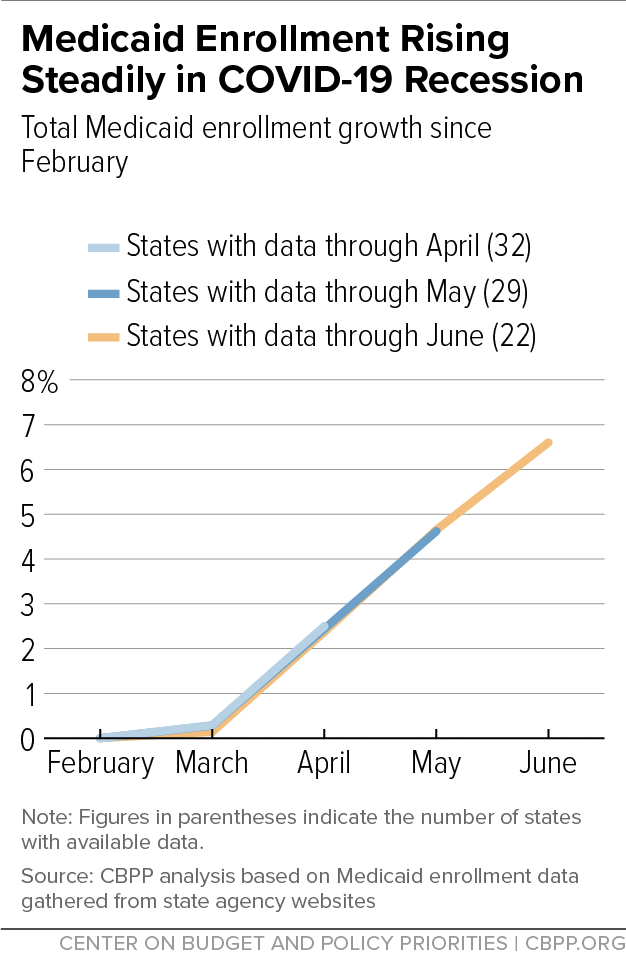
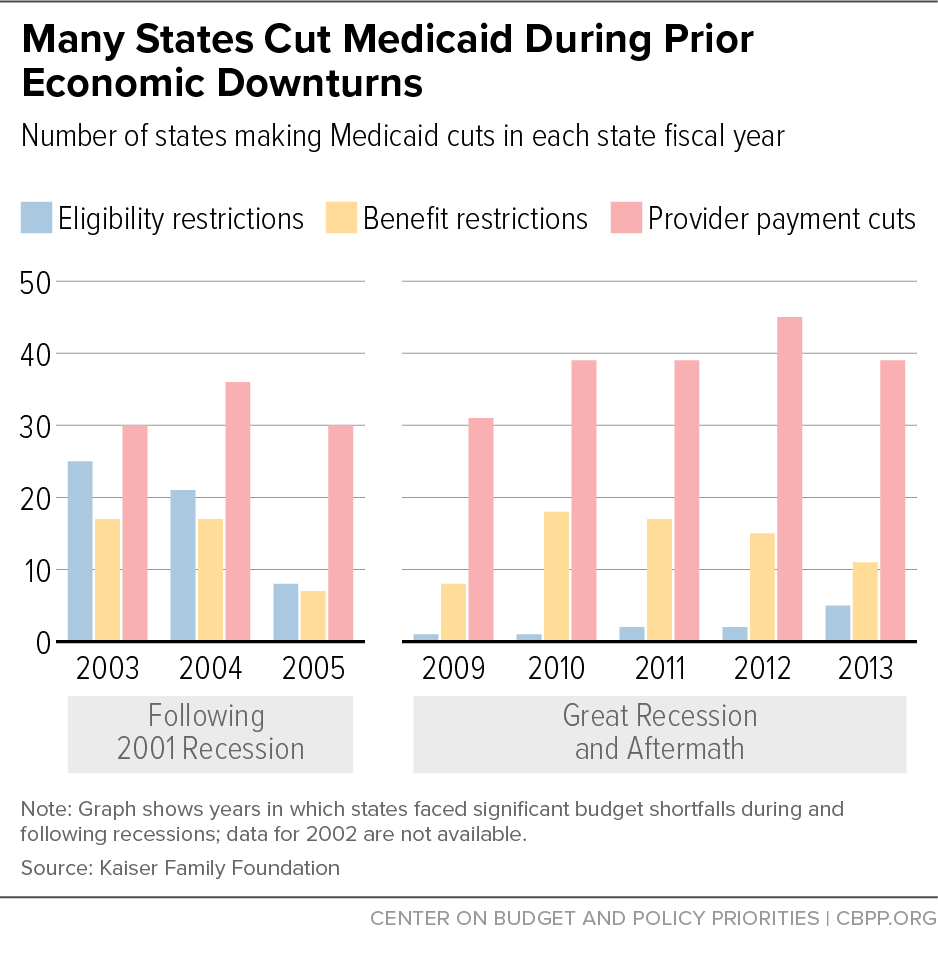
With Need Rising, Medicaid Is at Risk for Cuts
End Notes
[1] Our enrollment analysis draws upon and updates by Joan Alker and Tricia Brooks, “Medicaid Enrollment Increases Show Surprisingly Wide Variability Among States,” Georgetown Center for Children and Families, July 2, 2020, https://ccf.georgetown.edu/2020/07/02/medicaid-enrollment-increases-show-surprisingly-wide-variability-among-state/. For additional details, see the appendix.
[2] CBO’s forecast is here: https://www.cbo.gov/publication/56442. The Urban Institute analysis provides estimates for Medicaid growth assuming a 15 or 20 percent unemployment rate; we extrapolate the figures for a 10 percent unemployment rate. Bowen Garrett and Anuj Gangopadhyaya, “How the COVID-19 Recession Could Affect Health Insurance Coverage,” Urban Institute, May 2020, https://www.urban.org/sites/default/files/publication/102157/how-the-covid-19-recession-could-affect-health-insurance-coverage_0.pdf.
[3] Gia Gould, “Early Evidence Suggests Increased Medicaid Enrollment Due to COVID-19,” National Academy for State Health Policy, June 1, 2020, https://www.nashp.org/early-evidence-suggests-increased-medicaid-enrollment-due-to-covid-19/.
[4] We evaluate Medicaid, SNAP, and unemployment insurance monthly enrollment from November 2007 through December 2009. We use Centers for Medicare & Medicaid Services’ monthly Medicaid enrollment data (https://www.cms.gov/Research-Statistics-Data-and-Systems/Computer-Data-and-Systems/MedicaidDataSourcesGenInfo/MSIS-Tables), U.S. Department of Agriculture Food and Nutrition Service SNAP enrollment data (https://www.fns.usda.gov/pd/supplemental-nutrition-assistance-program-snap) and Department of Labor unemployment insurance claims data (https://oui.doleta.gov/unemploy/claims.asp).
[5] See also Alker and Brooks, op. cit., which our analysis draws on and updates, and Elizabeth Hinton et al., “Data Note: Growth in Medicaid MCO Enrollment During the COVID-19 Pandemic,” Kaiser Family Foundation, July 16, 2020, https://www.kff.org/coronavirus-covid-19/issue-brief/data-note-growth-in-medicaid-mco-enrollment-during-the-covid-19-pandemic/.
[6] While enrollment increases are likely driven mainly by economic conditions, the Families First Coronavirus Response Act’s requirement that states pause Medicaid terminations while they receive additional federal funding is contributing to the overall increases as well, mainly by keeping eligible people from losing coverage due to paperwork requirements and to their income fluctuations from month to month. See Judith Solomon, “Continuous Coverage Protections in Families First Act Prevent Coverage Gaps by Reducing ‘Churn,’” Center on Budget and Policy Priorities, July 16, 2020, https://www.cbpp.org/research/health/continuous-coverage-protections-in-families-first-act-prevent-coverage-gaps-by.
[7] Matt Broaddus, “Research Note: Medicaid Enrollment Decline Among Children and Adults Too Large to Be Explained by Falling Unemployment,” Center on Budget and Policy Priorities, July 17, 2019, https://www.cbpp.org/research/health/medicaid-enrollment-decline-among-adults-and-children-too-large-to-be-explained-by.
[8] These figures include Maine and Virginia (which implemented their Medicaid expansions beginning in 2019) and Utah (which fully implemented its Medicaid expansion beginning in 2020). In these states, expansion enrollment may be growing in part because it had not yet reached steady levels. All three states, however, have seen a sharp acceleration in growth rates since the recession began. And excluding these states has little effect on our findings; without them, expansion enrollment would have grown by 9.5 percent between February and June.
[9] Jessica Schubel, “States Are Leveraging Medicaid in Response to COVID-19,” Center on Budget and Policy Priorities, updated July 14, 2020, https://www.cbpp.org/research/health/states-are-leveraging-medicaid-to-respond-to-covid-19.
[10] Elizabeth McNichol and Michael Leachman, “States Continue to Face Large Shortfalls Due to COVID-19 Effects,” Center on Budget and Policy Priorities, updated July 7, 2020, https://www.cbpp.org/research/state-budget-and-tax/states-continue-to-face-large-shortfalls-due-to-covid-19-effects.
[11] Congressional Budget Office, “Preliminary Estimate of the Effects of H.R. 6201, the Families First Coronavirus Response Act,” April 2, 2020, https://www.cbo.gov/system/files/2020-04/HR6201.pdf.
[12] State of Arizona, “JLBC Staff – June Budget Update,” June 19, 2020, p. 5, https://www.azleg.gov/jlbc/061920junebudgetupdate.pdf; State of California, “California State Budget 2020-21,” p. 54, http://www.ebudget.ca.gov/FullBudgetSummary.pdf; State of Colorado, “Budget Package and Long Bill Narrative,” May 26, 2020, p. 48, https://leg.colorado.gov/sites/default/files/fy20lbnarrative.pdf; State of Georgia, “HB 793 - FY 2021 Appropriations Bill,” p. 40, https://opb.georgia.gov/hb-793-fy-2021-appropriations-bill; State of Louisiana, “Overall House Floor - Solution to SGF Shortfalls,” p. 1, https://house.louisiana.gov/housefiscal/hac/State%20Budget%20Summary%20-%20House%20Floor%20After%20HAC%205-22-20.pdf; State of Nevada, “Nevada COVID-19 Fiscal Report,” July 6, 2020, p. 24, http://gov.nv.gov/uploadedFiles/govnewnvgov/Content/News/Press/2020_attachments/Nevada_COVID-19_Fiscal_Report.pdf; State of Utah, “Medicaid and CHIP Caseload, Inflation and Program Changes,” https://cobi.utah.gov/2020/1/issues/15239.
[13] Health Access California, “2020 Budget Scorecard,” June 23, 2020, https://health-access.org/wp-content/uploads/2020/06/Health-Access-2020-Budget-Scorecard_6.23.20.pdf.
[14] Governor Gavin Newsom, Letter to Senate Majority Leader Mitch McConnell and Minority Leader Chuck Schumer, June 26, 2020, https://drive.google.com/file/d/1-83dGWGRSvd7F3cXZ2z_4rm_SCgikMMb/view?usp=sharing
[15] Colorado Consumer Health Initiative, “2020 Legislative Summary,” https://cohealthinitiative.org/wp-content/uploads/2020/06/2020-Legislative-Scorecard_FINAL_6.24.20-reduced-size.pdf. See also Markian Hawryluk, “Colorado, Like Other States, Trims Health Programs Amid Health Crisis,” Kaiser Health News, July 10, 2020, https://khn.org/news/colorado-like-other-states-trims-health-programs-amid-health-crisis/.
[16] Governor Ron DeSantis, “2020 Veto List,” June 29, 2020, https://www.flgov.com/2020/06/29/governor-ron-desantis-signs-the-fiscal-year-2020-2021-budget/. See Line Item 249 for vetoes of three line items regarding provider rate increases. See also Carl Lisciandrello and Mark Schreiner, “Gov. DeSantis Vetoes $1 Billion From Florida Budget, Citing ‘Difficult Circumstances,’” News Service of Florida, June 29, 2020, https://wusfnews.wusf.usf.edu/post/gov-desantis-vetoes-1-billion-florida-budget-citing-difficult-circumstances.
[17] Nevada Assembly Bill 3, July 18, 2020, https://www.leg.state.nv.us/App/NELIS/REL/31st2020Special/Bill/7127/Text.
[18] State of Utah, “Compendium of Budget Information,” https://cobi.utah.gov/2020/1/issues.
[19] State of Tennessee, “Conference Committee Report on House Bill No. 2922 / Senate Bill No. 2931 / CC0023,” http://www.capitol.tn.gov/Bills/111/CCRReports/CC0023.pdf. See also Shannon Smith, “TennCare postpartum care expansion cut from revised state budget,” WBIR, June 8, 2020, https://www.wbir.com/article/life/tenncare-postpartum-care-expansion-cut-from-revised-state-budget/51-8587612b-7c73-4566-b5e2-be7f524ace0d.
[20] Office of Financial Management, “Budget Savings Options 2020 – Health Care Authority,” State of Washington, https://ofm.wa.gov/sites/default/files/public/budget/statebudget/savings/107HCA-HBE.pdf.
[21] Nevada Assembly Bill 3, July 18, 2020, https://www.leg.state.nv.us/App/NELIS/REL/31st2020Special/Bill/7127/Text.
[22] Wes Ventiecher, “California’s largest state worker union accepts two furlough days in pay cut deal with Newsom,” Sacramento Bee, June 20, 2020, https://www.sacbee.com/news/politics-government/the-state-worker/article243680447.html.
[23] Stacey Barchenger and Dustin Racioppi, “Gov. Murphy signs revamped bill to furlough workers as CARES money runs out,” NorthJersey.com, July 3, 2020, https://www.northjersey.com/story/news/2020/07/03/gov-phil-murphy-signs-bill-furlough-workers-stimulus-money-runs-out-cares-act/5367424002/.
[24] Governor Jay Inslee, “Furloughs and General Wage Increases,” June 17, 2020, https://www.governor.wa.gov/sites/default/files/directive/20-08%20Furloughs%20and%20General%20Wage%20Increases%20%28tmp%29.pdf.
[25] Erin Cox, “Hogan hires former campaign manager to help solve a budget crisis,” Washington Post, July 2, 2020, https://www.washingtonpost.com/local/md-politics/hogan-hires-former-campaign-manager-the-same-week-he-pitched-cutting-employee-pay-to-solve-a-budget-crisis/2020/07/02/cea6acfc-bcab-11ea-80b9-40ece9a701dc_story.html.
[26] Dan Boyd, “State hiring freeze likely first of many budget cuts,” Albuquerque Journal, April 24, 2020, https://www.abqjournal.com/1447131/state-hiring-freeze-first-of-many-likely-budget-cuts-ex-governor-were-going-to-have-to-reduce-expenditures.html.
[27] Andrew Tobias, “DeWine Administration Announces Employee Pay Cuts to Help Fill $25 Billion Ohio Budget Hole,” Cleveland.com, updated June 2, 2020, https://www.cleveland.com/open/2020/06/dewine-administration-announces-employee-pay-cuts-to-help-fill-25-billion-ohio-budget-hole.html.
[28] Tennessee Department of Finance and Administration, “Lee Administration Releases Plan to Balance Tennessee Budget,” June 4, 2020, https://www.tn.gov/finance/news/2020/6/4/lee-administration-releases-plan-to-balance-tennessee-budget.html.
[29] Alan Suderman, “Virginia Governor Orders Hiring Freeze, Agency Heads to Look for Cuts,” NBC News, April 4, 2020, https://www.nbcwashington.com/news/local/virginia-governor-orders-hiring-freeze-agency-heads-to-look-for-cuts/2262982/.
[30] Michael Leachman, “Contrary to Arguments, States Need More Federal Relief,” Center on Budget and Policy Priorities, May 6, 2020, https://www.cbpp.org/blog/contrary-to-arguments-states-need-more-federal-relief.
[31] Aviva Aron-Dine et al., “Larger, Longer-Lasting Increases in Federal Medicaid Funding Needed to Protect Coverage,” Center on Budget and Policy Priorities, May 5, 2020, https://www.cbpp.org/research/health/larger-longer-lasting-increases-in-federal-medicaid-funding-needed-to-protect.
[32] Ted Lutterman, “The Impact of the State Fiscal Crisis on State Mental Health Systems,” NASMHPD Research Institute, March 2012, http://www.nri-inc.org/media/1102/2012-the-impact-of-the-state-fiscal-crisis-on-state-mental-health-systems-lutterman.pdf.
[33] William Wan and Heather Long, “‘Cries for Help:’ Drug Overdoses Are Soaring During the Coronavirus Pandemic,” Washington Post, June 1, 2020, https://www.washingtonpost.com/health/2020/07/01/coronavirus-drug-overdose/.
[34] Markian Hawryluk, “Colorado, Like Other States, Trims Health Programs Amid Health Crisis,” Kaiser Health News, July 10, 2020, https://khn.org/news/colorado-like-other-states-trims-health-programs-amid-health-crisis/.
[35] Governor Ron DeSantis, “2020 Veto List,” June 29, 2020, https://www.flgov.com/2020/06/29/governor-ron-desantis-signs-the-fiscal-year-2020-2021-budget/. See Line Item 376 for vetoes of 19 line items for grants for services and programs related to behavioral health, substance use, crisis intervention, and people experiencing homelessness.
[36] State of Georgia, “HB 793 - FY 2021 Appropriations Bill,” https://opb.georgia.gov/hb-793-fy-2021-appropriations-bill. See also Alex Welch, “House and Senate Approve Georgia’s FY 2021 Budget,” Georgia Budget and Policy Institute, June 26, 2020, https://gbpi.org/2021-budget-proposal-update/.
[37] State of Utah, “Compendium of Budget Information,” https://cobi.utah.gov/2020/1/issues.
[38] Office of Financial Management, “Budget Savings Options 2020 – Health Care Authority,” State of Washington, https://ofm.wa.gov/sites/default/files/public/budget/statebudget/savings/107HCA-HBE.pdf and Office of Financial Management, “Budget Savings Options 2020 – Department of Social and Health Services,” State of Washington, https://ofm.wa.gov/sites/default/files/public/budget/statebudget/savings/300DSHS.pdf.
[39] Lauren Weber et al., “Hollowed-Out Public Health System Faces More Cuts Amid Virus,” Kaiser Health News, July 1, 2020, https://khn.org/news/us-public-health-system-underfunded-under-threat-faces-more-cuts-amid-covid-pandemic/.
[40] See, for example, Michael Leachman, “To Support Education, Congress Should Provide Substantial Fiscal Relief to States and Localities,” Testimony Before the House Committee on Education and Labor, Center on Budget and Policy Priorities, June 15, 2020, https://www.cbpp.org/state-budget-and-tax/to-support-education-congress-should-provide-substantial-fiscal-relief-to.
[41] http://dhss.alaska.gov/HealthyAlaska/Pages/dashboard.aspx
[42] https://www.azahcccs.gov/Resources/Downloads/PopulationStatistics/2020/July/AHCCCSPopulationbyCategory.pdf
[43] https://humanservices.arkansas.gov/newsroom/toolkits
[44] https://www.colorado.gov/pacific/hcpf/premiums-expenditures-and-caseload-reports
[45] https://data.ct.gov/Health-and-Human-Services/DSS-Medical-Benefit-Plan-Participation-by-Month-CY/f7bp-3wsx
[46] https://ahca.myflorida.com/medicaid/Finance/data_analytics/eligibles_report/index.shtml
[47] https://www.illinois.gov/hfs/MedicalProviders/cc/Pages/TotalCCEnrollmentforAllPrograms.aspx
[48] https://www.in.gov/fssa/ompp/4881.htm
[49] https://dhs.iowa.gov/ime/about/performance-data/MC-monthly-reports
[50] https://www.kdheks.gov/hcf/medicaid_reports/default.htm
[51] https://chfs.ky.gov/agencies/dms/dafm/Pages/statistics.aspx
[52] http://www.ldh.la.gov/HealthyLaDashboard/
[53] https://www.maine.gov/dhhs/data-reports/mainecare-expansion
[54] https://md-medicaid.org/eligibility/index.cfm
[55] https://www.michigan.gov/mdhhs/0,5885,7-339-71547_4860-15064--,00.html
[56] https://www.dhs.state.mn.us/main/idcplg?IdcService=GET_DYNAMIC_CONVERSION&RevisionSelectionMethod=LatestReleased&dDocName=dhs16_141529
[57] https://medicaid.ms.gov/resources/
[58] https://dss.mo.gov/mis/clcounter/history.htm
[59] https://dphhs.mt.gov/helpplan/medicaidexpansiondashboard
[60] https://www.dhhs.nh.gov/ombp/medicaid/enrollment-data.htm
[61] https://www.state.nj.us/humanservices/dmahs/news/reports/
[62] https://www.hsd.state.nm.us/LookingForInformation/medicaid-eligibility.aspx
[63] https://www.health.ny.gov/health_care/managed_care/reports/enrollment/monthly/
[64] https://medicaid.ncdhhs.gov/reports/dashboards
[65] https://medicaid.ohio.gov/RESOURCES/Reports-and-Research/Caseload-Reports
[66] http://www.okhca.org/research.aspx?id=17502
[67] https://www.oregon.gov/oha/HSD/OHP/Pages/Reports.aspx?wp2504=p:1#g_c0f44780_17ac_4f72_ab1b_ae94d4742b9e
[68] https://dss.sd.gov/keyresources/medasst_statistics.aspx
[69] https://www.tn.gov/tenncare/information-statistics/enrollment-data.html
[70] https://hhs.texas.gov/about-hhs/records-statistics/data-statistics/healthcare-statistics
[71] State health agency data as of July 10, 2020.
[72] https://www.dmas.virginia.gov/#/deidentifiedreports
[73] https://www.hca.wa.gov/about-hca/client-eligibility-data-dashboard
[74] https://dhhr.wv.gov/bms/Members/Managed%20Care/MCOreports/Pages/default.aspx