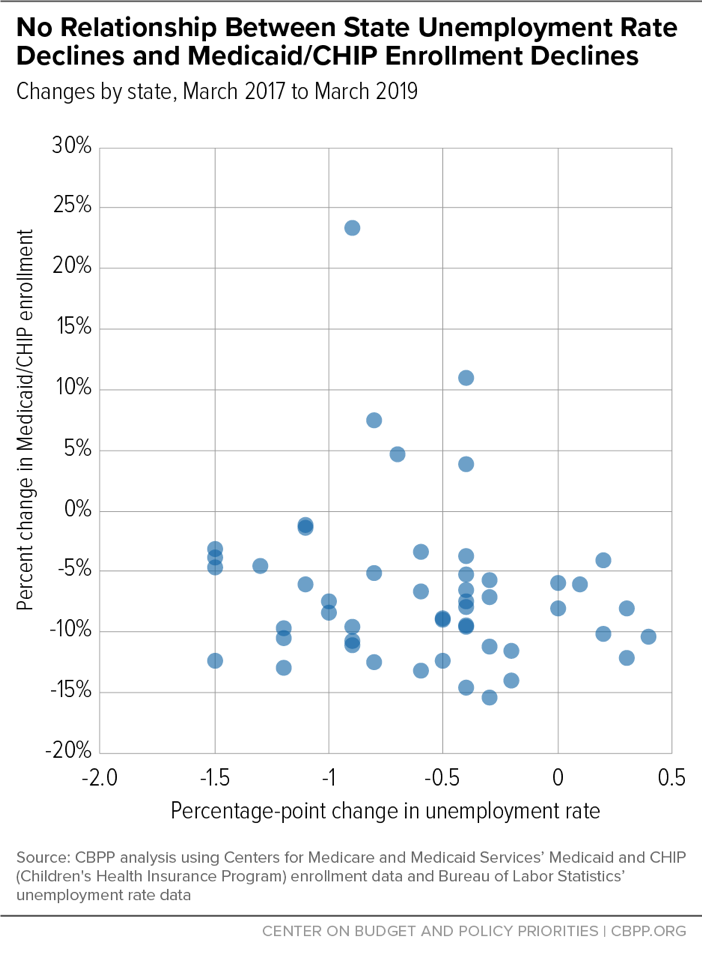
Research Note: Medicaid Enrollment Decline Among Adults and Children Too Large to Be Explained by Falling Unemployment
End Notes
[1] All estimates are based on administrative enrollment data collected from the states by the Centers for Medicare & Medicaid Services (CMS) and made publicly available (see https://www.medicaid.gov/medicaid/program-information/medicaid-and-chip-enrollment-data/index.html). March 2019 is the most recent month for which CMS has collected final total Medicaid enrollment data for each state and the District of Columbia. We adjust overall and adult enrollment data for Texas because the state altered the way it reports enrollment data for adults over the time period of our analysis. Specifically, we assume that the entire enrollment decline in the month (June 2017) in which the state changed its reporting method was attributable to the reporting change. This likely results in a slightly conservative estimate of Texas’ total enrollment decline.
[2] Tricia Brooks, Edwin Park, and Lauren Roygardner, “Medicaid and CHIP Enrollment Decline Suggests the Child Uninsured Rate May Rise Again,” Georgetown Center for Children and Families, May 2019, https://ccf.georgetown.edu/wp-content/uploads/2019/06/Enrollment-Decline.pdf.
[3] The enrollment-reduction figures for children and adults cited here add to less than the 1.7 million overall figure cited above because data disaggregated by age are available for only 48 states, while the overall data are available for all states.
[4] See https://twitter.com/SeemaCMS/status/1121478298561912832.
[5] “MACStats: Medicaid and CHIP Data Book,” Medicaid and CHIP Payment and Access Commission, December 2018, https://www.macpac.gov/wp-content/uploads/2018/12/December-2018-MACStats-Data-Book.pdf. See Exhibit 10 for a complete history of Medicaid enrollment trends.
[6] Brooks, Park, and Roygardner, op. cit.
[7] John Holahan and Bowen Garrett, “Rising Unemployment, Medicaid and the Uninsured,” Kaiser Family Foundation and the Urban Institute, January 2009, https://www.kff.org/wp-content/uploads/2013/03/7850.pdf. The authors find that Medicaid enrollment among children can be expected to rise by 0.79 percentage points for every 1 percentage-point increase in the unemployment rate, after controlling for all other factors that affect Medicaid enrollment among children. We assume, based on the method of the study, that every 1 percentage-point decline in the unemployment rate would cause Medicaid enrollment among children to fall by 0.79 percentage points. We then apply this finding to the actual unemployment-rate decline between February 2017 and February 2019 to estimate the Medicaid enrollment decline among children based on this decline.
[8] Robin Cohen, Emily Terlizzi, and Michael Martinez, “Health Insurance Coverage: Early Release of Estimates from the National Health Interview Survey, 2018,” Centers for Disease Control and Prevention, May 2019, https://www.cdc.gov/nchs/data/nhis/earlyrelease/insur201905.pdf.
[9] Jennifer Wagner, “Commentary: As Predicted, Arkansas’ Medicaid Waiver Is Taking Coverage Away from Eligible People,” Center on Budget and Policy Priorities, June 28, 2019, https://www.cbpp.org/health/commentary-as-predicted-arkansas-medicaid-waiver-is-taking-coverage-away-from-eligible-people.
[10] “Editorial: Medicaid Eligibility Crackdown Pushes Out Genuinely Needy Missouri Families,” St. Louis Post-Dispatch, February 14, 2019, https://www.stltoday.com/opinion/editorial/editorial-medicaid-eligibility-crackdown-pushes-out-genuinely-needy-missouri-families/article_f80939f4-ef45-5606-9b8b-ddb2b3819bf3.html.
[11] Hannah Katch et al., “Health Proposals in President’s 2020 Budget Would Reduce Health Insurance Coverage and Access to Care,” Center on Budget and Policy Priorities, April 19, 2019, https://www.cbpp.org/research/health/health-proposals-in-presidents-2020-budget-would-reduce-health-insurance-coverage.