Medicaid Is Key to Building a System of Comprehensive Substance Use Care for Low-Income People
End Notes
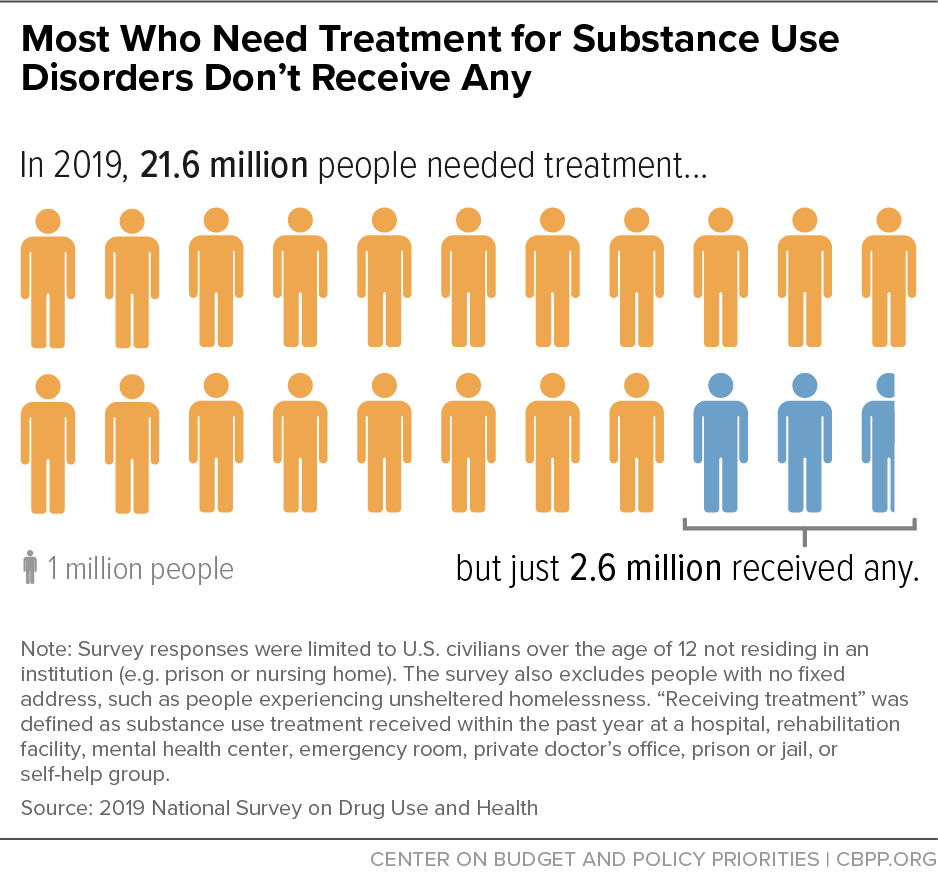
[1] Substance Abuse and Mental Health Services Administration, “Key Substance Use and Mental Health Indicators in the United States: Results from the 2019 National Survey on Drug Use and Health,” September 2020, https://www.samhsa.gov/data/sites/default/files/reports/rpt29393/2019NSDUHFFRPDFWHTML/2019NSDUHFFR1PDFW090120.pdf.
[2] See Laura Radel et al., “Substance Use, the Opioid Epidemic, and the Child Welfare System: Key Findings from a Mixed Methods Study,” Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services, March 2018, https://aspe.hhs.gov/system/files/pdf/258836/SubstanceUseChildWelfareOverview.pdf; Marjorie Baldwin, Steven Marcus, & Jeffrey De Simone, “Job Loss Discrimination and Former Substance Use Disorders,” July 2010, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2885482/.
[3] M.B. Esser et al., “Deaths and Years of Potential Life Lost from Excessive Alcohol Use: United States, 2011-2015,” Centers for Disease Control and Prevention, 2020, https://www.cdc.gov/mmwr/volumes/69/wr/mm6939a6.htm.
[4] The increase in overdose deaths is largely being driven by synthetic opioids such as fentanyl, cocaine, and stimulants such as methamphetamine. F.B. Ahmad, L.M. Rossen, & P. Sutton, “Provisional Drug Overdose Death Counts,” Centers for Disease Control and Prevention, 2020, https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm. See also Josh Katz, Abby Goodnough, and Margo Sanger-Katz, “In Shadow of Pandemic, U.S. Drug Overdose Deaths Resurge to Record,” New York Times, July 15, 2020, https://www.nytimes.com/interactive/2020/07/15/upshot/drug-overdose-deaths.html.
[5] Health coverage plans offered through the Affordable Care Act’s marketplace must cover behavioral health services that are comparable to the plan’s physical health coverage, thereby providing access to coverage for substance use disorder treatment. However, the particular services, medications, and cost-sharing requirements in marketplace plans vary considerably. States can enforce parity laws to improve marketplace coverage of substance use services and can use grants to fill treatment funding gaps. Rebecca Peters and Erik Wengle, “Coverage of Substance-Use Disorder Treatments in Marketplace Plans in Six Cities,” Urban Institute, June 2016, https://www.urban.org/sites/default/files/publication/81856/2000838-Coverage-of-Substance-Use-Disorder-Treatments-in-Marketplace-Plans-in-Six-Cities.pdf.
[6] Angélica Meinhofer and Allison E. Witman, “The Role of Health Insurance on Treatment for Opioid Use Disorders: Evidence from the Affordable Care Act Medicaid Expansion,” Journal of Health Economics, Volume 60, July 2018, https://www.sciencedirect.com/science/article/abs/pii/S0167629617311530.
[7] Center on Budget and Policy Priorities, “Health Reform’s Medicaid Expansion,” https://www.cbpp.org/health-reforms-medicaid-expansion.
[8] Jesse Cross-Call, “Medicaid Expansion Has Helped Narrow Racial Disparities in Health Coverage and Access to Care,” October 21, 2020, https://www.cbpp.org/research/health/medicaid-expansion-has-helped-narrow-racial-disparities-in-health-coverage-and.
[9] Kaiser Family Foundation, “Who Could Medicaid Expansion Reach in All States?” January 23, 2020, http://files.kff.org/attachment/fact-sheet-medicaid-expansion-US.
[10] Tara Straw, et al., “Health Provisions in American Rescue Plan Act Improve Access to Health Coverage During COVID Crisis,” Center on Budget and Policy Priorities, March 11, 2021, https://www.cbpp.org/research/health/health-provisions-in-american-rescue-plan-act-improve-access-to-health-coverage.
[11] American Society of Addiction Medicine, “The ASAM Criteria,” https://www.asam.org/resources/the-asam-criteria/about.
[12] Medicaid and CHIP Payment and Access Commission (MACPAC), “Recovery Support Services for Medicaid Beneficiaries with a Substance Use Disorder,” July 2019, https://www.macpac.gov/wp-content/uploads/2019/07/Recovery-Support-Services-for-Medicaid-Beneficiaries-with-a-Substance-Use-Disorder.pdf.
[13] U.S. Department of Health and Humans Services, Office of the Surgeon General, “Facing Addiction in America: The Surgeon General’s Report on Alcohol, Drugs, and Health,” November 2016, https://addiction.surgeongeneral.gov/sites/default/files/surgeon-generals-report.pdf; MACPAC, 2019.
[14] MACPAC, “Report to Congress on Medicaid and CHIP, Chapter 4: Access to Substance Use Disorder Treatment in Medicaid,” June 2018, https://www.macpac.gov/publication/june-2018-report-to-congress-on-medicaid-and-chip/.
[15] Jesse Cross-Call, “House Bill Gives States Incentive to Quickly Expand Medicaid, Cover Millions of Uninsured,” Center on Budget and Policy Priorities, February 25, 2021, https://www.cbpp.org/research/health/house-bill-gives-states-incentive-to-quickly-expand-medicaid-cover-millions-of.
[16] The 1915(i) option allows states to provide home- and community-based services (HCBS) to individuals who don’t meet the standards for receiving care in an institution such as a nursing home. This option is particularly important for people with SUDs who don’t qualify for HCBS waiver programs requiring individuals to show they would be eligible for institutional care covered by Medicaid but for the provision of HCBS. Because Medicaid generally doesn’t cover care in institutions for people with SUDs, these beneficiaries were shut out of HCBS waivers. Section 1915(i) allows states to target HCBS to individuals with SUDs and tailor their benefit package to suit their needs.
[17] MACPAC, 2018. Note that while the ASAM criteria categorize “outpatient” and “intensive outpatient” as two different levels of care on the continuum, these two groups of services can both be provided under Medicaid state plan amendments without any demonstration waivers.
[18] MACPAC, 2018.
[19] MACPAC, 2019.
[20] Ibid. CMS recently issued updated guidance on how states can use Medicaid to cover housing-related services and other services that can address social determinants of health. Centers for Medicare & Medicaid Services letter to state health officials (21-001), “Opportunities in Medicaid and CHIP to Address Social Determinants of Health (SDOH),” January 7 2021, https://www.medicaid.gov/federal-policy-guidance/downloads/sho21001.pdf. For more information on supportive housing, see Ehren Dohler, et al., “Supportive Housing Helps Vulnerable People Live and Thrive in the Community,” Center on Budget and Policy Priorities, May 31, 2016, https://www.cbpp.org/research/housing/supportive-housing-helps-vulnerable-people-live-and-thrive-in-the-community.
[21] MACPAC, 2019.
[22] Medicaid’s institution for mental disease exclusion prohibits federal Medicaid funds from paying for substance use treatment delivered in treatment facilities with more than 16 beds to patients ages 21 through 64.
[23] Centers for Medicare & Medicaid Services, “Strategies to Address the Opioid Epidemic,” November 1, 2017, https://www.medicaid.gov/federal-policy-guidance/downloads/smd17003.pdf.
[24] Kaiser Family Foundation, “Medicaid Waiver Tracker: Approved and Pending Section 1115 Waivers by State,” October 9, 2019, https://www.kff.org/medicaid/issue-brief/medicaid-waiver-tracker-approved-and-pending-section-1115-waivers-by-state/#Table5.
[25] CMS, “Report to Congress: 2018 SUD Data Book,” January 2021, https://www.medicaid.gov/medicaid/data-systems/downloads/2018-sud-data-book.pdf.
[26] Centers for Medicare & Medicaid Services, 2017: “CMS encourages states to maintain their current funding levels for a continuum of services, and this initiative should not reduce or divert state spending on mental health and addiction treatment services as a result of available federal funding for services in [institutions for mental disease.]”
[27] SUPPORT for Patients and Communities Act, 2018, P.L. 115-271.
[28] See Centers for Medicare & Medicaid Services letter to state Medicaid directors (19-0003), November 6, 2019, https://www.medicaid.gov/federal-policy-guidance/downloads/smd19003.pdf.
[29] See Idaho’s approved state plan amendment, approved April 7, 2020, https://www.medicaid.gov/State-resource-center/Medicaid-State-Plan-Amendments/Downloads/ID/ID-19-0023.pdf.
[30] MACPAC, 2019.
[31] Lisa-Clemans-Cope et al., “Experiences of three states implementing the Medicaid health home model to address opioid use disorder — Case studies in Maryland, Rhode Island, and Vermont,” Journal of Substance Abuse Treatment, Vol. 83, 2017, https://www.journalofsubstanceabusetreatment.com/article/S0740-5472(17)30195-2/pdf.
[32] Substance Abuse and Mental Health Services Administration, “Crisis Services: Effectiveness, Cost-Effectiveness, and Funding Strategies,” U.S. Department of Health and Human Services, 2014, https://www.nasmhpd.org/sites/default/files/SAMSHA%20Publication%20on%20Effectiveness%20%26%20Cost-Effectiveness%20of%2C%20and%20Funding%20Strategies%20for%2C%20Crisis%20Services%206-5-14_8.pdf.
[33] Julie Tate, Jennifer Jenkins, and Steven Rich, “990 People Have Been Shot and Killed by Police in the Past Year,” Washington Post, Updated March 11, 2021, https://www.washingtonpost.com/graphics/investigations/police-shootings-database/?itid=lk_inline_manual_3; Amam Z Saleh et al., “Deaths of People with Mental Illness During Interactions with Law Enforcement,” International Journal of Law and Psychiatry, May-June 2018, https://pubmed.ncbi.nlm.nih.gov/29853001/.
[34] See William Hoagland et al., “Tracking FY2019 Federal Funding to Combat the Opioid Crisis,” Bipartisan Policy Center, September 2020, https://bipartisanpolicy.org/wp-content/uploads/2020/09/BPC-Opioids-Report_RV6-1.pdf; Ellen Weber and Arka Gupta, “State Medicaid Programs Should follow the ‘Medicare Model’: Remove Prior Authorization Requirements for Buprenorphine and Other Medications to Treat Opioid Use Disorders,” Legal Action Center, July 2019, https://www.lac.org/resource/state-medicaid-programs-should-follow-the-medicare-model-remove-prior-authorization-requirements-for-buprenorphine-and-other-medications-to-treat-opioid-use-disorders.
[35] Weber and Gupta.
[36] MACPAC, 2018.
[37] Health Resources and Services Administration, “National Projection of Supply and Demand for Selected Behavioral Health Practitioners: 2013-2025,” November 2016, https://bhw.hrsa.gov/sites/default/files/bureau-health-workforce/data-research/behavioral-health-2013-2025.pdf; James Maxwell, Angel Bourgoin, and Zoe Lindenfeld, “Battling the Mental Health Crisis Among the Underserved Through State Medicaid Reforms,” Health Affairs, February 10, 2020, https://www.healthaffairs.org/do/10.1377/hblog20200205.346125/full/.
[38] Christine Vestal, “How Severe is the Shortage of Substance Abuse Specialists?” Pew Stateline, April 1, 2015, https://www.pewtrusts.org/en/research-and-analysis/blogs/stateline/2015/4/01/how-severe-is-the-shortage-of-substance-abuse-specialists; MACPAC, 2018; Substance Abuse and Mental Health Services Administration, “Behavioral Health Workforce Report,” December 2020, https://www.samhsa.gov/sites/default/files/behavioral-health-workforce-report.pdf.
[39] Peggy Bailey, “Better Integration of Medicaid and Federal Grant Funding Would Improve Outcomes for People with Substance Use Disorders,” Center on Budget and Policy Priorities, April 9, 2018, https://www.cbpp.org/research/health/better-integration-of-medicaid-and-federal-grant-funding-would-improve-outcomes-for.
[40] John O’Brien et al., “State Approaches to Developing the Residential Treatment Continuum for Substance Use Disorders,” Technical Assistance Collaborative, Inc., March 2019, https://www.tacinc.org/resource/state-approaches-to-developing-the-residential-treatment-continuum-for-substance-use-disorders/..Christina Andrews et al., “Despite Resources From The ACA, Most States Do Little To Help Addiction Treatment Programs Implement Health Care Reform,” Health Affairs, Vol. 34:5, May 2015, https://www.healthaffairs.org/doi/pdf/10.1377/hlthaff.2014.1330.
[41] Centers for Medicare & Medicaid Services, “Substance Use Disorder Prevention that Promotes Opioid Recovery and Treatment for Patients and Communities (SUPPORT) Act: Section 1003: Demonstration Project to Increase Substance Use Provider Capacity,” https://www.medicaid.gov/medicaid/benefits/bhs/support-act-provider-capacity-demos/index.html?utm_source=Connecting+the+Dots&utm_campaign=2d583f697c-EMAIL_CAMPAIGN_2019_09_13_08_35&utm_medium=email&utm_term=0_c4fccaa672-2d583f697c-.
[42] Government Accountability Office, “Medicaid: States’ Changes to Payment Rates for Substance Use Disorder Services,” January 2020, https://www.gao.gov/products/gao-20-260 ; see also MACPAC, “Report to Congress on Medicaid and CHIP,” June 2017, https://www.macpac.gov/wp-content/uploads/2017/06/June-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf.
[43] See for example Katherine Hayes et al., “Integrating Clinical and Mental Health: Challenges and Opportunities,” Bipartisan Policy Center, January 2019, https://bipartisanpolicy.org/wp-content/uploads/2019/03/Integrating-Clinical-and-Mental-Health-Challenges-and-Opportunities.pdf; Dana Foney and Shannon Mace, “Factors that Influence Access to Medication-Assisted Treatment,” University of Michigan Behavioral Health Workforce Research Center and the National Council for Behavioral Health, August 2019, http://www.behavioralhealthworkforce.org/wp-content/uploads/2019/10/Factors-that-Influence-MAT_Full-Report.pdf; Steve Melek, Stoddard Davenport and T.J. Gray, “Addiction and mental health vs. physical health: Widening disparities in network use and provider reimbursement,” Milliman, November 19, 2019, http://assets.milliman.com/ektron/Addiction_and_mental_health_vs_physical_health_Widening_disparities_in_network_use_and_provider_reimbursement.pdf; and Lisa Clemans-Cope et al., “Leveraging Medicaid to Address Opioid and Substance Use Disorders in Maine: Ten State Policy Options from an Expedited Review,” Urban Institute, June 2019, https://www.urban.org/sites/default/files/publication/100443/2019.06.20_mainecare_report_final_7.pdf.
[44] O’Brien et al.; Government Accountability Office.
[45] MACPAC, 2018. See also Commonwealth of Virginia, Department of Medical Assistance Services, “Addiction and Recovery Treatment Services (ARTS): Benefit and Reimbursement Structure Before and After ARTS,” https://cdn.vox-cdn.com/uploads/chorus_asset/file/10767475/Medicaid_ARTS_Rates__Before_and_After.0.pdf.
[46] Peter Cunningham et al., “Addiction and Recovery Treatment Services: Access and Utilization during the First Year (April 2017 – March 2018),” Virginia Commonwealth University, August 2018, https://hbp.vcu.edu/media/hbp/policybriefs/pdfs/ARTSone-yearreport_8.9.18_Final.pdf.
[47] Government Accountability Office.
[48] Ibid.
[49] Clemans-Cope et al., 2019.
[50] Ibid.
[51] Ellen Bouchery, Rebecca Morris, and Jasmine Little, “Examining Substance Use Disorder Treatment Demand and Provider Capacity in a Changing Health Care System: Initial Findings Report,” U.S. Department of Health and Human Services Office of the Assistant Secretary for Planning and Evaluation, September 2015, pp. 52-53, https://aspe.hhs.gov/system/files/pdf/203761/ExamSUD.pdf.
[52] “Here’s What It Would Cost to Fix the Opioid Crisis, According to 5 Experts,” Money, November 27, 2017, https://money.com/cost-fix-opioid-crisis/.
[53] Bailey.
[54] National Council for Behavioral Health, “Demand for Mental Health and Addiction Services Increasing as COVID-19 Pandemic Continues to Threaten Availability of Treatment Options,” September 9, 2020, https://www.thenationalcouncil.org/press-releases/demand-for-mental-health-and-addiction-services-increasing-as-covid-19-pandemic-continues-to-threaten-availability-of-treatment-options/.
[55] F.B. Ahmad, L.M. Rossen, and P. Sutton, “Provisional Drug Overdose Death Counts,” National Center for Health Statistics, 2021, https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm.
[56] G. William Hoagland et al., “Tracking Federal Funding to Combat the Opioid Crisis,” Bipartisan Policy Center, March 2019, https://bipartisanpolicy.org/wp-content/uploads/2019/03/Tracking-Federal-Funding-to-Combat-the-Opioid-Crisis.pdf; Christine Vestal, “Opioid Money Has Helped, But States Want More,” Pew Stateline, January 30, 2019, https://www.pewtrusts.org/en/research-and-analysis/blogs/stateline/2019/01/30/opioid-money-has-helped-but-states-want-more; Rachana Pradhan and Brianna Ehley, “Hundreds of Millions in State Opioid Cash Left Unspent,” Politico, March 19, 2018, https://www.politico.com/story/2018/03/19/opioid-crisis-funding-unspent-468658; Abby Goodnough, “States Are Making Progress on Opioids. Now the Money That’s Helping Them May Dry Up,” New York Times, July 16, 2019, https://www.nytimes.com/2019/07/16/health/opioids-grants-treatment-addiction.html?smid=tw-nytimes&smtyp=cur.
[57] National Association of State Alcohol and Drug Abuse Directors, “How States Are Using State Targeted Response (STR) and State Opioid Response (SOR) Funds to Make a Difference,” March 2020, https://nasadad.org/wp-content/uploads/2020/04/STR_SOR_-Treatment-Initiatives-3.30.pdf.
[58] By enhancing premium tax credits for 2021 and 2022, the American Rescue Plan Act will eliminate or reduce premiums for millions of marketplace enrollees. Straw et al.
[59] Clemans-Cope et al., 2019; G. William Hoagland et al., 2019.
[60] Governor Tom Wolf, “Wolf Administration Awards $15 Million in Housing Grants to Help Individuals Battling Opioid Use Disorder,” Commonwealth of Pennsylvania, March 27, 2019, https://www.governor.pa.gov/newsroom/wolf-administration-awards-15-million-in-housing-grants-to-help-individuals-battling-opioid-use-disorder/; see also National Association of State Alcohol and Drug Abuse Directors, “Pennsylvania: Use of STR/SOR Grant Funds to Address the Opioid Crisis,” September 2019, https://nasadad.org/pennsylvania-str-sor-profile/.
[61] National Association of State Alcohol and Drug Abuse Directors, “Pennsylvania: Use of STR/SOR Grant Funds to Address the Opioid Crisis,” September 2019, https://nasadad.org/pennsylvania-str-sor-profile/.
[62] Hoagland et al., 2019.
[63] Hoagland et al., 2020.
[64] Preliminary research finds that people with lived experience with the substance use treatment system report that quality-of-life improvements, connection to a support network, improved mental health, and having basic needs taken care of are important outcomes that they want for themselves, in addition to staying alive and stopping substance use. Community Catalyst “Peers Speak Out: Improving Substance Use Treatment Outcomes During COIVD-19,” December 2020, https://communitycatalyst.app.box.com/v/PeersSpeakOutInitialFindings.
[65] Rajita Sinha, “Chronic Stress, Drug Use, and Vulnerability to Addiction,” Annals of the New York Academy of Sciences, July 2018, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2732004/.
[66] National Alliance to End Homelessness, “Homelessness and Racial Disparities,” October 2020, https://endhomelessness.org/homelessness-in-america/what-causes-homelessness/inequality/.
[67] Shana F. Sandberg et al., “Hennepin Health: A Safety-Net Accountable Care Organization for the Expanded Medicaid Population,” Health Affairs, November 2014, https://www.healthaffairs.org/doi/pdf/10.1377/hlthaff.2014.0648.
[68] Peggy Bailey, “Housing and Health Partners Can Work Together to Close the Housing Affordability Gap,” Center on Budget and Policy Priorities, January 17, 2020, https://www.cbpp.org/research/housing/housing-and-health-partners-can-work-together-to-close-the-housing-affordability.
[69] Center on Budget and Policy Priorities staff, “American Rescue Plan Act Will Help Millions and Bolster the Economy,” updated March 15, 2021, https://www.cbpp.org/research/poverty-and-inequality/american-rescue-plan-act-will-help-millions-and-bolster-the-economy.
[70] Douglas Rice, Stephanie Schmit, and Hannah Matthews, “Child Care and Housing: Big Expenses with Too Little Help Available,” Center on Budget and Policy Priorities and CLASP, April 26, 2019, https://www.cbpp.org/research/housing/child-care-and-housing-big-expenses-with-too-little-help-available.
[71] Alicia Mazzara, “Interactive Graphic: Highlighting the 3 out of 4 At-Risk Renters Who Don’t Get Rental Assistance,” Center on Budget and Policy Center, March 6, 2017, https://www.cbpp.org/blog/interactive-graphic-highlighting-the-3-out-of-4-at-risk-renters-who-dont-get-rental-assistance.
[72] Will Fischer, “For Struggling Renters: Housing Vouchers for All Who Need Them,” Center on Budget and Policy Priorities, February 1, 2021, https://www.cbpp.org/blog/for-struggling-renters-housing-vouchers-for-all-who-need-them.
[73] Washington’s section 1115 wavier: https://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Waivers/1115/downloads/wa/wa-medicaid-transformation-ca.pdf.
[74] Centers for Medicare & Medicaid Services letter to state health officials (21-001).
[75] Hannah Katch, “Medicaid Can Partner With Housing Providers and Others to Address Enrollees’ Social Needs,” Center on Budget and Policy Priorities, updated January 27, 2020, https://www.cbpp.org/research/health/medicaid-can-partner-with-housing-providers-and-others-to-address-enrollees-social.