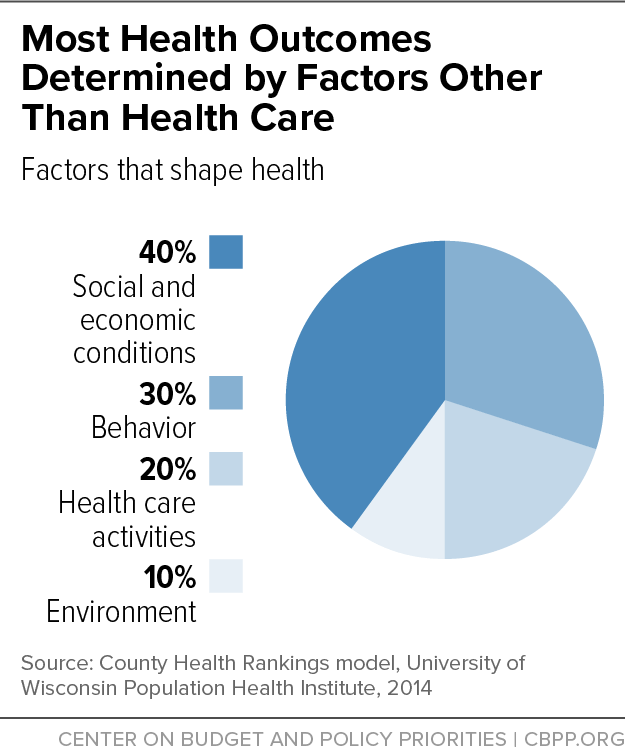Better State Budget, Policy Decisions Can Improve Health
End Notes
Support for this report was provided by the Robert Wood Johnson Foundation. The views expressed here do not necessarily reflect the views of the Foundation.
[1] “Health at a Glance, 2017,” Organisation for Economic Co-Operation and Development, November 10, 2017, http://www.oecd.org/health/health-at-a-glance-19991312.htm.
[2] Paula Braveman, Susan Egerter, and David R. Williams, “The Social Determinants of Health: Coming of Age,” Annual Review of Public Health, November 22, 2010, 32:381-398, https://www.annualreviews.org/doi/abs/10.1146/annurev-publhealth-031210-101218.
[3] Michael Gideon Marmot et al., “Health inequalities among British civil servants: the Whitehall II study,” The Lancet, June 8, 1991, 337(8754):1387-1393, https://www.ncbi.nlm.nih.gov/pubmed/1674771.
[4] Thomas McKeown, R. G. Record, and R. D. Turner, “An Interpretation of the Decline of Mortality in England and Wales during the Twentieth Century,” Population Studies, November 1975, 29(3):391-422, https://www.jstor.org/stable/2173935.
[5] J. Michael McGinnis, Pamela Williams-Russo, and James R. Knickman, “The Case for More Active Policy Attention to Health Promotion,” Health Affairs, March 1, 2002, 21(2):78-93, https://www.healthaffairs.org/doi/full/10.1377/hlthaff.21.2.78.
[6] Shyama Kuruvilla et al., “Success factors for reducing maternal and child mortality,” Bulletin of the World Health Organization 2014 (92)533-544, http://www.who.int/bulletin/volumes/92/7/14-138131/en/.
[7] Patrick L. Remington, Bridget B. Catlin, and Keith P. Gennuso, “The County Health Rankings: rationale and methods,” Population Health Metrics, April 17, 2015, https://pophealthmetrics.biomedcentral.com/articles/10.1186/s12963-015-0044-2. Note that the County Health Rankings model does not account for genetics and biology, which are not measurable or modifiable.
[8] See for example, Paula A. Braveman et al., “Socioeconomic Disparities in Health in the United States: What the Patterns Tell Us,” American Journal of Public Health, April 2010, 100 (S1): S186–S196. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2837459/.
[9] Data are only available by income for Black, Latinx, and white people. However, American Indians and Alaska Natives have lower incomes and are more likely to have incomes below the poverty level than whites. See: “Profile, American Indian/Alaska Native,” U.S. Department of Health and Human Services Office of Minority Health, last modified March 28, 2018, https://minorityhealth.hhs.gov/omh/browse.aspx?lvl=3&lvlid=62.
[10] National Center for Health Statistics, Health, United States, 2017: With Special Feature on Morality, See Table 45, “Respondent-assessed fair-poor health status, by selected characteristics: United States, selected years 1991–2016,” https://www.cdc.gov/nchs/data/hus/2017/045.pdf.
[11] See for example, Paulani Mui et al., “Ethnic Group Differences in Health Outcomes Among Asian American Men in California,” American Journal of Men’s Health, September 2017, 11(5):1406-1414, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5675204/.
[12] People who identify with a Latin American or Hispanic ethnicity may prefer to be identified in various ways including as Hispanic, Latino, Latina, Latinx, or with a more specific country of origin. In this report we use the gender-neutral term “Latinx.” We also use “Hispanic” where appropriate, for instance in cases when a data source uses that term.
[13] National Center for Health Statistics, op. cit.
[14] Although life expectancy for Latinx people is higher than for white people and higher than the U.S. average, the data include individuals born in the United States as well as individuals born outside the United States. Latinx individuals born in the United States tend to have lower life expectancy than those born outside the United States. A growing body of research explores other potential reasons for longer life expectancy among Latinx populations relative to what would be expected based on their income and education levels. See: Neil K. Mehta et al., “Life Expectancy Among U.S.-born and Foreign-born Older Adults in the United States: Estimates From Linked Social Security and Medicare Data,” Demography: August 2016, 53(4): 1109-1134, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5026916/; Paola Scommenga, “Exploring the Paradox of U.S. Hispanics’ Longer Life Expectancy,” Population Reference Bureau, July 12, 2013, https://www.prb.org/us-hispanics-life-expectancy/.
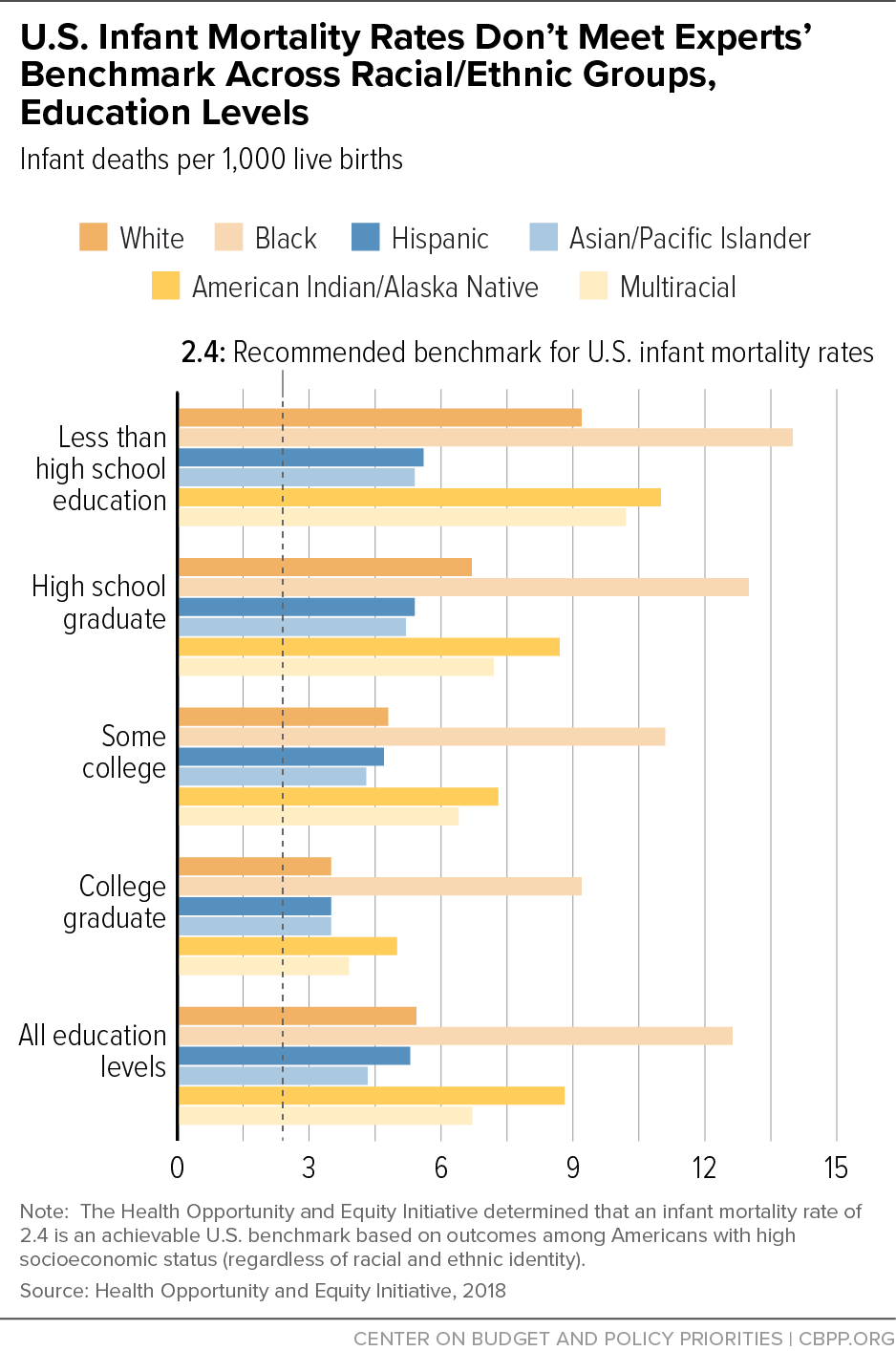
[15] Nadia Siddiqui et al., “The HOPE Initiative: Data Chartbook,” July 2018, http://www.nationalcollaborative.org/our-programs/hope-initiative-project/.
[16] State and local budget and policy decisions are often grouped together in this analysis, because states transfer a significant portion of their funding to localities to administer programs such as education and public health. Local expenditures often reflect budget or policy decisions made at the state level.
[17] U.S. Census Bureau, 2016 Annual Surveys of State and Local Government Finances, https://www.census.gov/programs-surveys/gov-finances.html.
[18] J. Mac McCullough, The Return on Investment of Public Health System Spending, AcademyHealth, June 21, 2018, https://www.academyhealth.org/publications/2018-06/return-investment-public-health-system-spending.
[19] Charlotte Gill et al., “Community-oriented policing to reduce crime, disorder and fear and increase satisfaction and legitimacy among citizens: a systematic review,” Journal of Experimental Criminology, December 2014, 10(4): 399-428, https://link.springer.com/article/10.1007/s11292-014-9210-y.
[20] J. Mac McCullough and Jonathon P. Leider, “Government Spending in Health and Nonhealth Sectors Associated with Improvement in County Health Rankings,” Health Affairs, November 2016, 35(11): 2037-2043, https://www.healthaffairs.org/doi/10.1377/hlthaff.2016.0708.
[21] Elira Kuka, “Quantifying the Benefits of Social Insurance: Unemployment Insurance and Health,” National Bureau of Economic Research Working Paper No. 24766, June 2018, https://www.nber.org/papers/w24766.
[22] “Health Insurance Coverage of the Nonelderly (0-64) with Incomes below 200% Federal Poverty Level (FPL), 2016” Kaiser Family Foundation, 2018, https://www.kff.org/other/state-indicator/nonelderly-up-to-200-fpl/; Samantha Artiga, Julia Foutz, and Anthony Damico, “Health Coverage by Race and Ethnicity: Changes Under the ACA,” Kaiser Family Foundation, January 26, 2018, https://www.kff.org/disparities-policy/issue-brief/health-coverage-by-race-and-ethnicity-changes-under-the-aca/.
[23] “Chart Book: The Far-Reaching Benefits of the Affordable Care Act’s Medicaid Expansion,” Center on Budget and Policy Priorities, October 2, 2018, https://www.cbpp.org/research/health/chart-book-the-far-reaching-benefits-of-the-affordable-care-acts-medicaid.
[24] Benjamin Sommers et al., “Three-Year Impacts of the Affordable Care Act: Improved Medical Care and Health Among Low-Income Adults,” Health Affairs epub ahead of print, May 2017, http://content.healthaffairs.org/content/early/2017/05/15/hlthaff.2017.0293.
[25] Chintan B. Bhatt and Consuelo M. Beck-Sagué, “Medicaid Expansion and Infant Mortality in the United States,” American Journal of Public Health, April 2018, 108 (4):565-567, https://www.ncbi.nlm.nih.gov/pubmed/29346003.
[26] Michael Karpman and Kyle J. Caswell, “Past-Due Medical Debt among Nonelderly Adults, 2012-15,” Urban Institute, March 2017, https://www.urban.org/research/publication/past-due-medical-debt-among-nonelderly-adults-2012-15.
[27] “Chart Book: The Far-Reaching Benefits of the Affordable Care Act’s Medicaid Expansion.”
[28] Ehren Dohler et al., “Supportive Housing Helps Vulnerable People Live and Thrive in the Community,” Center on Budget and Policy Priorities, May 31, 2016, https://www.cbpp.org/research/housing/supportive-housing-helps-vulnerable-people-live-and-thrive-in-the-community.
[29] Artiga, Foutz, and Damico, op. cit.
[30] McCullough and Leider, op. cit.
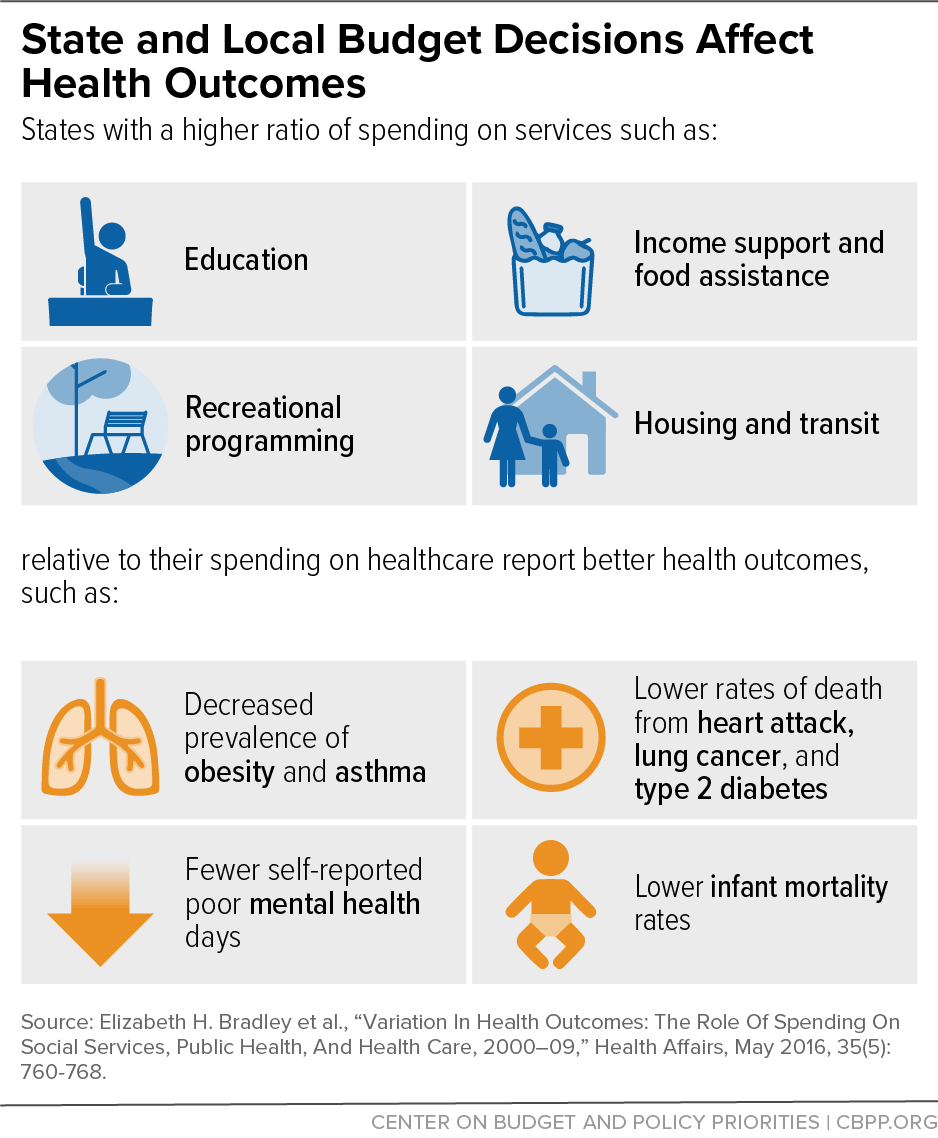
[31] Elizabeth H. Bradley et al., “Variation In Health Outcomes: The Role Of Spending On Social Services, Public Health, And Health Care, 2000–09,” Health Affairs, May 2016, 35(5): 760-768, https://www.healthaffairs.org/doi/10.1377/hlthaff.2015.0814.
[32] Michael Leachman, Kathleen Masterson, and Eric Figueroa, “A Punishing Decade for School Funding,” Center on Budget and Policy Priorities, November 29, 2017, https://www.cbpp.org/research/state-budget-and-tax/a-punishing-decade-for-school-funding; Bruce D. Baker, “Does Money Matter in Education? Second Edition,” Albert Shanker Institute, 2016, http://www.shankerinstitute.org/resource/does-money-matter-second-edition.
[33] “Why Education Matters to Health: Exploring the Causes,” Virginia Commonwealth University Center on Society and Health, February 13, 2015, https://societyhealth.vcu.edu/work/the-projects/why-education-matters-to-health-exploring-the-causes.html.
[34] Leachman, Masterson, and Figueroa, op. cit.
[35] Michael Mitchell et al., “Unkept Promises: State Cuts to Higher Education Threaten Access and Equity, “ Center on Budget and Policy Priorities, October 4, 2018, https://www.cbpp.org/research/state-budget-and-tax/unkept-promises-state-cuts-to-higher-education-threaten-access-and.
[36] Allison H. Friedman-Krauss et al., “The State of Preschool 2017: State Preschool Yearbook,” National Institute for Early Education Research, April 2018, http://nieer.org/state-preschool-yearbooks/yearbook2017.
[37] Wendy Collins Perdue, Lesley A. Stone, and Lawrence O. Gostin, “The Built Environment and Its Relationship to the Public’s Health: The Legal Framework,” American Journal of Public Health, September 2003, 93(9):1390-1394, https://ajph.aphapublications.org/doi/10.2105/AJPH.93.9.1390.
[38] Sara Zimmerman et al., “At the Intersection of Active Transportation and Equity,” Safe Routes to School National Partnership, 2015, https://www.saferoutespartnership.org/resources/report/intersection-active-transportation-equity.
[39] SO Griffin et al., “Effectiveness of fluoride in preventing caries in adults,” Journal of Dental Research, May 1, 2007, 86(5):410–414, https://www.ncbi.nlm.nih.gov/pubmed/17452559.
[40] National Water Fluoridation Statistics, 2014, Centers for Disease Control and Prevention, last updated August 19, 2016, https://www.cdc.gov/fluoridation/statistics/2014stats.htm.
[41] American Academy of Pediatrics, “Prevention of Childhood Lead Toxicity,” Pediatrics, July 2016, 138(1):e20161493, http://pediatrics.aappublications.org/content/138/1/e20161493; Bruce Lanphear et al., “Low-level Lead Exposure and Mortality in US Adults: A Population-Based Cohort Study,” The Lancet: Public Health, March 12, 2018, 3(4): e177-e184, https://www.thelancet.com/journals/lanpub/article/PIIS2468-2667(18)30025-2/fulltext.
[42] Elizabeth McNichol, “It’s Time for States to Invest in Infrastructure,” Center on Budget and Policy Priorities, August 10, 2017, https://www.cbpp.org/research/state-budget-and-tax/its-time-for-states-to-invest-in-infrastructure.
[43] Jennifer Beltrán, “Working-Family Tax Credits Lifted 8.9 Million People out of Poverty in 2017,” Center on Budget and Policy Priorities, https://www.cbpp.org/blog/working-family-tax-credits-lifted-89-million-people-out-of-poverty-in-2017.
[44] Examples include: William N. Evans and Craig L. Garthwaite, “Giving Mom a Break: The Impact of Higher EITC Payments on Maternal Health,” National Bureau of Economic Research, Working Paper No. 16296, August 2010, https://www.nber.org/papers/w16296; Hillary Hoynes, Doug Miller, and David Simon, “Income, the Earned Income Tax Credit, and Infant Health,” American Economic Journal: Economic Policy, 2015; 7(1): 172-211, https://www.aeaweb.org/articles?id=10.1257/pol.20120179.
[45] Jeannette Wicks-Lim and Peter S. Arno, “Improving population health by reducing poverty, New York’s Earned Income Tax Credit,” Social Science Medicine – Population Health, December 2017, 3:373-381, https://www.sciencedirect.com/science/article/pii/S2352827316300829.
[46] Raj Chetty, Nathaniel Hendren, and Lawrence F. Katz, “The Effects of Exposure to Better Neighborhoods on Children: New Evidence from the Moving to Opportunity Experiment,” American Economic Review, May 2015, 106(4): 855-902, https://opportunityinsights.org/paper/newmto/.
[47] The U.S. Department of Housing and Urban Development defines “extremely low-income families” as families whose incomes do not exceed the higher of the federal poverty level or 30 percent of area median income. See 42 U.S.C. § 1437a.
[48] “Three Out of Four Low-Income At-Risk Renters Do Not Receive Federal Rental Assistance,” Center on Budget and Policy Priorities, updated August 2017, https://www.cbpp.org/three-out-of-four-low-income-at-risk-renters-do-not-receive-federal-rental-assistance.
[49] Anna Bailey, Peggy Bailey, and Doug Rice, “Innovative Approaches to Providing Rental Assistance: States and Localities Seek To Support Health and Human Services Goals,” Cityscape, 2018, 20(2), https://www.huduser.gov/portal/periodicals/cityscpe/vol20num2/ch4.pdf.
[50] Will Fischer, “Low-Income Housing Tax Credit Could Do More to Expand Opportunity for Poor Families,” Center on Budget and Policy Priorities, August 28, 2018, https://www.cbpp.org/research/housing/low-income-housing-tax-credit-could-do-more-to-expand-opportunity-for-poor-families.
[51] Erica Williams and Samantha Waxman, “State Earned Income Tax Credits and Minimum Wages Work Best Together,” Center on Budget and Policy Priorities, updated February 7, 2018, https://www.cbpp.org/research/state-budget-and-tax/state-earned-income-tax-credits-and-minimum-wages-work-best-together.
[52] Arindrajit Dube, “Minimum Wages and the Distribution of Family Incomes,” IZA Institute of Labor Economics, February 2017, http://ftp.iza.org/dp10572.pdf; Brady P. Horn, Johanna Catherine Maclean, and Michael R. Strain, “Do Minimum Wage Increases Influence Worker Health?” Economic Inquiry, October 2017, 55(4): 1986-2007, https://onlinelibrary.wiley.com/doi/abs/10.1111/ecin.12453.
[53] George Wehby, Dhaval Dave, and Robert Kaestner, “Effects of the Minimum Wage on Infant Health,” National Bureau of Economic Research, Working Paper No. 22373, Revised March 2018, https://www.nber.org/papers/w22373; Juan Du and J. Paul Leigh, “Effects of Minimum Wages on Absence from Work Due to Illness,” The B.E. Journal of Economic Analysis & Policy, January 2018, 18(1), https://doi.org/10.1515/bejeap-2017-0097.
[54] Williams and Waxman, op. cit.
[55] LeaAnne DeRigne et al., “Paid sick leave and preventive health care service use among U.S. working adults,” Preventive Medicine, June 217, 99: 58-62, https://www.ncbi.nlm.nih.gov/pubmed/28189802; LeaAnne DeRigne, Patricia Stoddard Dare, and Linda Quinn, “Workers Without Paid Sick Leave Less Likely To Take Time Off For Illness Or Injury Compared To Those With Paid Sick Leave,” Health Affairs, March 2016, 35(3): 520-527, https://www.healthaffairs.org/doi/10.1377/hlthaff.2015.0965; Supriya Kumar et al., “Policies to Reduce Influenza in the Workplace: Impact Assessments Using an Agent-Based Model,” American Journal of Public Health, August 2013, 103(8):1406-1411, https://www.ncbi.nlm.nih.gov/pubmed/23763426.
[56] Heather Hill, “Paid Sick Leave and Job Stability,” Work and Occupations, May 2013, 40(2): 143-173, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3825168/.
[57] Jenna Stearns, “The effects of paid maternity leave: Evidence from Temporary Disability Insurance,” Journal of Health Economics, September 2015, 43: 85-102, https://www.sciencedirect.com/science/article/abs/pii/S0167629615000533; Rada K. Dagher, Patricia M. McGovern, and Bryan E. Dowd, “Maternity Leave Duration and Postpartum Mental and Physical Health: Implications for Leave Policies,” Journal of Health Politics, Policy and Law, April 2014, 39(2): 369-416, https://www.ncbi.nlm.nih.gov/pubmed/24305845.
[58] Linda Houser and Thomas P. Vartanian, “Pay Matters: The Positive Economic Impacts of Paid Family Leave for Families, Businesses and the Public,” Rutgers Center for Women and Work, January 2012, https://smlr.rutgers.edu/sites/default/files/images/CWW_Paid_Leave_Brief_Jan_2012_0.pdf.
[59] See for example, Paula A. Braveman et al., “Socioeconomic Disparities in Health in the United States: What the Patterns Tell Us,” American Journal of Public Health, April 2010, 100 (S1): S186–S196. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2837459/.
[60] Meg Wiehe et al., “Who Pays? A Distributional Analysis of the Tax Systems in All 50 States, Sixth Edition,” The Institute on Taxation and Economic Policy, October 2018, https://itep.org/whopays/.
[61] Elizabeth McNichol, “How State Tax Policies Can Stop Increasing Inequality and Start Reducing It,” Center on Budget and Policy Priorities, December 15, 2016, https://www.cbpp.org/research/state-budget-and-tax/how-state-tax-policies-can-stop-increasing-inequality-and-start. Many state income taxes are flat or nearly flat, and seven states do not have an income tax (Alaska, Florida, Nevada, South Dakota, Texas, Washington, and Wyoming).
[62] Michael Leachman et al., “Advancing Racial and Ethnic Equity with State Tax Policy,” Center on Budget and Policy Priorities, November 15, 2018, https://www.cbpp.org/research/state-budget-and-tax/advancing-racial-equity-with-state-tax-policy.
[63] Wesley Tharpe, “Raising State Income Tax Rates at the Top a Sensible Way to Fund Key Investments,” Center on Budget and Policy Priorities, February 7, 2019, https://www.cbpp.org/research/state-budget-and-tax/raising-state-income-tax-rates-at-the-top-a-sensible-way-to-fund-key.
[64] Elizabeth McNichol, “Strategies to Address the State Tax Volatility Problem,” Center on Budget and Policy Priorities, April 18, 2013, https://www.cbpp.org/research/strategies-to-address-the-state-tax-volatility-problem.
[65] Jesse Bricker et al., “Changes in U.S. Family Finances from 2013 to 2016: Evidence from the Survey of Consumer Finances,” Federal Reserve Bulletin, September 2017, 103(3), https://www.federalreserve.gov/econres/scfindex.htm.
[66] Elizabeth McNichol, “State Taxes on Capital Gains,” Center on Budget and Policy Priorities, December 11, 2018, https://www.cbpp.org/research/state-budget-and-tax/state-taxes-on-capital-gains; Elizabeth McNichol, “State Taxes on Inherited Wealth,” Center on Budget and Policy Priorities, December 12, 2018, https://www.cbpp.org/research/state-budget-and-tax/state-taxes-on-inherited-wealth; Michael Leachman and Samantha Waxman, “State ‘Mansion Taxes’ on Very Expensive Homes,” Center on Budget and Policy Priorities, January 24, 2019, https://www.cbpp.org/research/state-budget-and-tax/state-mansion-taxes-on-very-expensive-homes.
[67] Matthew Gardner et al., “3 Percent and Dropping: State Corporate Tax Avoidance in the Fortune 500, 2008 to 2015,” Institute on Taxation and Economic Policy, April 2017, https://itep.org/3-percent-and-dropping-state-corporate-tax-avoidance-in-the-fortune-500-2008-to-2015/.
[68] Timothy Bartik, “Who Benefits From Economic Development Incentives? How Incentive Effects on Local Incomes and the Income Distribution Vary with Different Assumptions about Incentive Policy and the Local Economy,” W.E. Upjohn Institute for Employment Research, Report No. 18-034, March 2018, https://research.upjohn.org/up_technicalreports/34/; Michael Mazerov, “A Majority of States Have Now Adopted a Key Corporate Tax Reform — ‘Combined Reporting,’” Center on Budget and Policy Priorities, revised April 3, 2009, https://www.cbpp.org/research/a-majority-of-states-have-now-adopted-a-key-corporate-tax-reform-combined-reporting.
[69] Iris J. Lav and Michael Leachman, “State Limits on Property Taxes Hamstring Local Services and Should Be Relaxed or Repealed,” Center on Budget and Policy Priorities, July 18, 2018, https://www.cbpp.org/research/state-budget-and-tax/state-limits-on-property-taxes-hamstring-local-services-and-should-be.
[70] Iris J. Lav, “Cigarette Tax Increases: Cautions and Considerations,” Center on Budget and Policy Priorities, revised July 11, 2002, https://www.cbpp.org/archiveSite/7-3-02sfp.pdf.
[71] U.S. Department of Health and Human Services, “The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General,” U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, January 2014, https://www.surgeongeneral.gov/library/reports/50-years-of-progress/full-report.pdf.
[72] Chuck Marr and Chye-Ching Huang, “Higher Tobacco Taxes Can Improve Health and Raise Revenue,” Center on Budget and Policy Priorities, updated March 19, 2014, https://www.cbpp.org/research/higher-tobacco-taxes-can-improve-health-and-raise-revenue.
[73] “State Cigarette Excise Taxes Rates & Rankings,” Campaign for Tobacco-Free Kids, September 18, 2018, https://www.tobaccofreekids.org/assets/factsheets/0097.pdf.