The new House Build Back Better legislation would make meaningful progress in covering millions of people who lack health coverage by closing the Medicaid coverage gap and reducing premiums for people buying coverage through the Affordable Care Act (ACA) marketplaces. While these provisions are temporary, both would last through 2025 and would provide a strong foundation to further expand coverage, address racial and ethnic health inequities, and improve people’s health and economic well-being.
Under the proposal, more than 2 million uninsured adults with incomes below the poverty line would be able to enroll in ACA marketplace plans beginning in January 2022 without paying any premiums. By quickly making coverage available to this group — 60 percent of whom are people of color and none of whom currently have a path to coverage because they live in states that have refused to adopt the ACA’s Medicaid expansion — Build Back Better would achieve a top priority of civil rights and health equity leaders, who have emphasized its importance in reducing persistent racial inequities in health care and health outcomes.[1] Closing the coverage gap is a key component of efforts to reduce high and increasing rates of deaths and severe health complications among Black people who give birth.[2] And it will deliver coverage to large numbers of older adults and people who have disabilities and chronic health conditions.
The continuation of increased premium tax credits would allow more people who previously couldn’t afford marketplace coverage to enroll and would reduce premium costs for many others. The Build Back Better legislation would extend through 2025 temporary premium tax credit enhancements that were enacted in the American Rescue Plan for 2021 and 2022. These enhancements were likely a major reason for this year’s record marketplace enrollment; over 2.8 million people signed up during special enrollment periods in the federal and state-based marketplaces. Extending the Rescue Plan enhancements would help sustain these gains and reach additional uninsured people.
People with incomes below the poverty line generally aren’t eligible for premium tax credits under current law. People with incomes between 100 and 138 percent of the poverty line (or about $13,000 to $18,000 in yearly income for a single adult and about $22,000 to $30,000 for a family of three) who would be eligible for Medicaid if their states adopted the expansion can receive premium tax credits and enroll in marketplace plans, and many do. But the combination of states’ refusal to expand Medicaid and the federal floor on premium tax credit eligibility set at 100 percent of the poverty line creates a coverage gap for adults with incomes below the poverty line who aren’t eligible under other Medicaid categories, such as categories that provide coverage to very low-income parents and people with health conditions that meet a narrow definition of “disability.”
Under the Build Back Better legislation, people with incomes below the poverty line who are not eligible for Medicaid under their state’s rules would become eligible for premium tax credits, giving them a new pathway to affordable coverage in the marketplace. Enhancements would be made to marketplace plans to ensure that people with very low incomes who would be eligible for Medicaid if their state adopted the expansion have access to affordable health care. All people who would be eligible for Medicaid if their states had expanded, including those with incomes between 100 and 138 percent of the poverty line, would be eligible to enroll in the enhanced plans. With the enhancements:
- People wouldn’t pay a premium because premium tax credits would be enough to cover the full cost. This would begin in 2022.
- The plans would have very low deductibles and other cost-sharing charges to make sure that people can get the health care they need without unaffordable out-of-pocket costs. The actuarial value of the plans — the percentage of total average costs of covered benefits that the plan pays — would be set at 99 percent beginning in 2023, which translates to minimal cost sharing. In 2022, people with incomes below the poverty line would receive plans with a 94 percent actuarial value, the same as marketplace plans now available to people with incomes between 100 and 150 percent of the poverty line.
- Low-paid workers would be eligible for financial assistance even if they have an offer of employer coverage. Beginning in 2022, the legislation would ensure that people who would be eligible for Medicaid if their state adopted the expansion can enroll in marketplace coverage even if they have an employer offer of coverage. This mirrors how state Medicaid programs work — someone with an offer of employer coverage can choose to enroll in Medicaid, which has much lower costs than even heavily subsidized employer plans, which is particularly important for very low-income people. Eliminating any barrier to coverage based on an offer of employer coverage for people with the lowest incomes is critical because the general marketplace eligibility rules mean that many people who have an offer of employer coverage are barred from receiving premium tax credits for marketplace coverage even though the employer coverage isn’t truly affordable for them or their families.[3]
- People could enroll at any time during the year. As with Medicaid, people would not be restricted to enrolling during designated marketplace enrollment periods, starting in 2022.
- The plans would add benefits to more closely align with Medicaid. Beginning in 2024, the plans would cover the costs of transportation to medical appointments for people who couldn’t otherwise get the care they need. This would be in addition to emergency medical transportation, which marketplace plans already cover. Beginning in 2024, the plans also would cover family planning services and supplies, and people would have free choice of participating family planning providers regardless of whether the providers are in their managed care network.
These enhancements are critical to ensuring that people with incomes below or near the poverty line, whose financial resources for premiums, deductibles, and co-payments as well as transportation are extremely limited, have access to coverage that meets their needs.
Closing the coverage gap is an important step in undoing the effects of structural racism. A large body of evidence suggests that coverage will improve outcomes for conditions that have a greater impact on communities of color and bring increased financial security and protection from medical debt, which affects people of color at a higher rate. Most of the states that have refused to adopt the Medicaid expansion are located in the South and have above-average shares of Black and brown residents.[4] (See Appendix Table 1.)
While Build Back Better would provide a federal path to coverage for people who lack it — which is critically important — a state-administered Medicaid program that integrates the expansion population with other enrollees will continue to hold many advantages.
First, states that adopt the Medicaid expansion reduce the number of people who have to shift between the state Medicaid program and the marketplace. For example, in a state that has adopted the Medicaid expansion, when a child receiving Medicaid turns 19, they can remain in Medicaid. But in a non-expansion state, where low-income adults get their coverage in the marketplace rather than through Medicaid, that 19-year-old would have to shift to the marketplace even if their income remains very low. Similarly, a parent whose income falls from 120 percent of the poverty line to 25 percent of the poverty line due to a job loss can remain in Medicaid in an expansion state but would have to shift from marketplace to Medicaid coverage in a non-expansion state. In addition, parents and children are more likely to be in the same plan in expansion states because they are both eligible for Medicaid, while in non-expansion states, many parents of children in Medicaid will be in marketplace coverage if the coverage gap proposal is enacted.
State-administered Medicaid coverage also lets states develop approaches that connect health care to housing and other community-based services, which is especially important for people with mental illness or substance use disorders and people experiencing homelessness. Moreover, expansion has produced savings in several areas of state budgets by reducing costs for uncompensated care and providing federal matching funds for behavioral health and other services previously funded with state dollars, among other things. Because Medicaid coverage is broader in some areas than marketplace coverage, some of these benefits will remain larger for expansion states.[5]
In most expansion states, the benefits from expansion will outweigh any possible financial benefit they would get from dropping expansion, and the Build Back Better bill would make expansion even more valuable. States that have expanded would receive a 3 percentage point increase in the amount the federal government pays toward a state’s expenditures (known as the “federal medical assistance percentage” or FMAP) for expansion in 2023 through 2025, bringing the federal share to 93 percent.
To further encourage expansion, non-expansion states would still qualify for the financial incentive enacted in the American Rescue Plan if they expand. For the first two years of expansion, they would receive a two-year, 5 percentage point increase in the state’s FMAP for all groups other than those eligible through expansion, amounting to a large financial benefit.
Finally, the bill would reduce the federal funding going to non-expansion states that helps pay for uncompensated care provided to uninsured people. Medicaid expansion has been shown to significantly reduce uncompensated care. Hospital uncompensated care decreased sharply immediately after ACA coverage provisions took effect, with declines from 2013 to 2015 that were several times larger in expansion states than non-expansion states.[6] In Louisiana, which expanded Medicaid in 2016, expansion was associated with a 33 percent reduction in uncompensated care costs as a share of total operating expenses, with an even greater reduction of 55 percent for rural hospitals.[7] Reducing federal funds for uncompensated care avoids having the federal government provide funding intended for uncompensated care that is no longer actually uncompensated.
Expanding Premium Tax Credits Would Increase Private Coverage
The Build Back Better legislation would extend the Rescue Plan’s premium tax credit enhancements through 2025, instead of letting them expire after 2022. The enhancements eliminate or reduce premiums for millions of marketplace enrollees to ensure that people don’t spend more than 8.5 percent of their income on premiums, with lower income people paying far less.
Under the Rescue Plan, people with income between 100 and 150 percent of the poverty line (about $13,000 to $19,000 for a single person and $26,500 to nearly $40,000 for a family of four in the 2022 coverage year) pay no premiums for a benchmark plan, after accounting for premium tax credits, and other families pay a capped share of income toward health coverage.[8] These improvements to premium tax credits help almost everyone enrolled in marketplace coverage, except for higher-income people whose premiums are already less than 8.5 percent of their incomes.
The ACA made insurance more affordable for many people, yet as of 2019 the uninsured rate for lower-income people eligible for the most generous subsidies remained high: 14.1 percent of people with incomes between 138 and 250 percent of the poverty line were uninsured, compared to 3.1 percent for people with incomes above 500 percent of the poverty line.[9] Uninsured people at all income levels cite cost as the greatest barrier to coverage. In states that have improved financial assistance beyond the federal subsidies available, uninsured rates are low and access to care has improved.[10]
The Rescue Plan premium tax credit improvements have proven helpful in encouraging people, particularly low-income people, to access marketplace coverage. During this year’s six-month special enrollment period at HealthCare.gov (the federal marketplace), 45 percent of the people who newly selected a plan had incomes at or below 150 percent of the poverty line and 74 percent had incomes at or below 250 percent of poverty (about $32,000 for a single person).[11] The federal marketplace has increased support for health enrollment navigators, who provide one-on-one help with applying and enrolling, from $10 million to $91.5 million for the 2022 coverage year. These navigators focus outreach to people with lower incomes and other disproportionately underserved populations.[12]
Enhanced premium tax credits could also help improve racial equity in private health coverage enrollment.[13] Before the Rescue Plan was enacted, an estimated 11.2 million people were eligible for a premium tax credit but uninsured, according to federal estimates. About half of this group were people of color, including 30 percent who were Latino; 14 percent who were Black; 3 percent who were Asian, Native Hawaiian, or Pacific Islander; 1 percent who were American Indian/Alaska Native; and 2 percent who were multiracial or “some other race.”[14] All racial and ethnic groups would likely see large declines in the number of uninsured non-elderly adults; Black adults would see the largest gains, with more than 1 in 3 uninsured Black people gaining coverage, the Urban Institute estimates.[15]
The Build Back Better legislation would extend the Rescue Plan’s reduced premiums for marketplace enrollees, making coverage markedly more affordable through 2025. With the Rescue Plan’s changes, in 2021:[16]
- A single individual making $18,000 pays zero net premium rather than $54 per month (3.6 percent of income) and qualifies for the most generous subsidies for deductibles and other cost-sharing amounts.
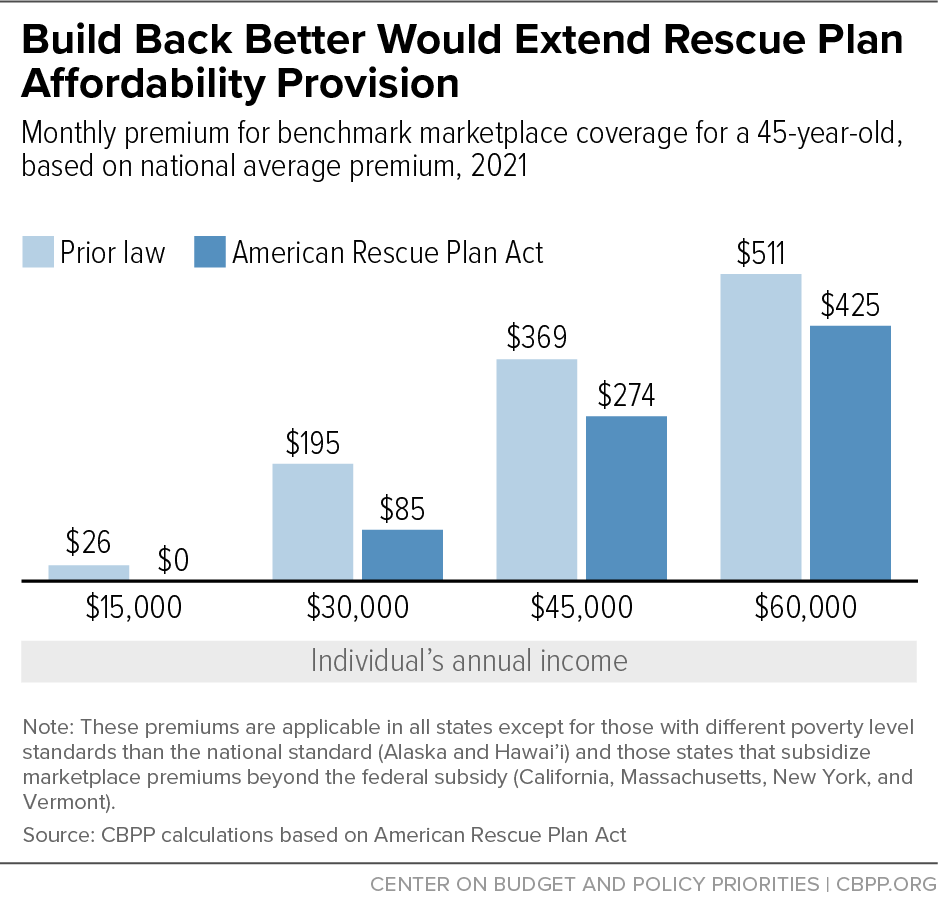
- A single individual making $30,000 pays $85 rather than $195 per month in premiums (3.4 instead of 7.8 percent of income) and qualifies for a plan with reduced deductibles and other cost-sharing amounts. (See Figure 1.)
- A family of four making $50,000 pays $67 rather than $252 per month in premiums for benchmark coverage (1.6 instead of 6.0 percent of their income) and qualifies for generous cost-sharing reductions.[17]
- A family of four making $75,000 pays $340 rather than $588 per month in premiums for benchmark coverage (5.4 instead of 9.4 percent of their income).
The ACA’s health insurance marketplaces have been a critical source of coverage for older people, who rely on the individual market more than other age groups.[18] That’s because many older adults who don’t have access to coverage through their job want health insurance ― 84 percent of people aged 55 to 64 have a pre-existing condition[19] ― but find it unaffordable without the ACA’s help. Older people account for nearly 29 percent of marketplace enrollees, even though they are only roughly 13 percent of the total population. And adults 55 and older accounted for 22 percent of new HealthCare.gov enrollees in the six-month special enrollment period that ended August 15.[20]
Because of the Rescue Plan’s expanded premium tax credits, 2 million current enrollees and 1.3 million uninsured people who are aged 55 to 64 and live in the 36 states that use HealthCare.gov are eligible for a marketplace plan with a monthly net premium of $50 or less or, for more than half of them, a $0 premium.[21] Any eligible marketplace enrollee making $25,000 now pays $38 rather than the previous $132 per month in premiums (1.84 instead of 6.33 percent of income) for a benchmark silver plan.
In addition to increasing the premium tax credit amounts, the Rescue Plan also expands who is eligible for a premium tax credit in a way that significantly benefits older people, by allowing people with incomes above 400 percent of the poverty line ($52,000 for a single person) to receive a premium tax credit if their premiums exceed 8.5 percent of their income. Before the Rescue Plan, people with income above that threshold weren’t eligible for financial help and had to pay the full premium, even if they faced excessive premium burdens.
This “cliff” particularly affected older people, whose premiums are much higher as a share of income than younger people because the ACA allows insurers to charge older people higher “sticker price” premiums. In 2021, the average unsubsidized premium for marketplace coverage ranged from $787 to $1,058 per month for 55- to 64-year-olds, versus $353 to $428 for 21- to 34-year-olds.[22]
Extending the Rescue Plan’s 8.5 percent income cap on premiums is also important to middle-income people who live in areas with high premiums.[23] The cap targets the most assistance to people with high premium burdens. For example, marketplace benchmark coverage for a 40-year-old in Charleston, West Virginia earning $55,000 a year (431 percent of the poverty line for a single person) costs about $731 per month, more than 1.5 times the national average. Prior to the Rescue Plan, this person wasn’t eligible for any help paying their premium. With the premium tax credit provided under the Rescue Plan, this person gets a monthly premium discount of $341, bringing their premium down to $390 per month.[24] In lower-cost states, a person of the same age with the same income doesn’t receive a premium tax credit because their premium is already below 8.5 percent of their income. And the premium tax credit enhancement automatically phases out at higher income levels because premiums are generally less than 8.5 percent of income for high-income people.
Providing premium tax credits to limit premium liability to no more than 8.5 percent of income for middle-income households helps other people who might otherwise have trouble affording coverage. For example, in 2021:
- A typical 60-year-old making $60,000 has seen their premiums cut by more than half, or $535 per month. Instead of paying $960 per month in premiums for benchmark coverage, or 19 percent of income, the consumer pays $425, or 8.5 percent of their income.
- A typical family of four with income of $110,000 has seen their premiums cut almost in half, by $666 per month. Instead of paying $1,445 per month in premiums for benchmark coverage, or nearly 16 percent of their income, the family pays $779, or 8.5 percent of their income, with the premium tax credit making up the difference.
By closing the coverage gap, the Build Back Better legislation would quickly provide coverage to people who have been shut out because their states have refused to expand Medicaid. It would enhance that coverage to better align with Medicaid and recognize the financial realities of very low-income households and provide incentives to encourage more states to adopt the Medicaid expansions. The proposal’s extension of improved premium tax credits would make marketplace coverage more accessible and affordable for millions of people.
The Build Back Better coverage expansions and improvements would last through 2025 and Congress will need to extend them to maintain these coverage gains.
| APPENDIX TABLE 1 |
| State |
Total |
Asian |
Black |
Latino |
Other |
White |
| Total, non-expansion states |
2,211,000 |
29,000 |
617,000 |
613,000 |
60,000 |
893,000 |
| Alabama |
137,000 |
* |
53,000 |
* |
* |
75,000 |
| Florida |
425,000 |
6,000 |
109,000 |
118,000 |
12,000 |
179,000 |
| Georgia |
275,000 |
* |
130,000 |
24,000 |
* |
114,000 |
| Kansas |
44,000 |
* |
* |
8,000 |
4,000 |
26,000 |
| Mississippi |
110,000 |
* |
59,000 |
* |
* |
44,000 |
| North Carolina |
207,000 |
* |
68,000 |
19,000 |
12,000 |
106,000 |
| South Carolina |
105,000 |
* |
42,000 |
* |
* |
55,000 |
| South Dakota |
16,000 |
* |
* |
* |
6,000 |
9,000 |
| Tennessee |
119,000 |
* |
31,000 |
5,000 |
* |
79,000 |
| Texas |
766,000 |
14,000 |
118,000 |
422,000 |
12,000 |
200,000 |
| Wyoming |
7,000 |
* |
* |
* |
* |
5,000 |