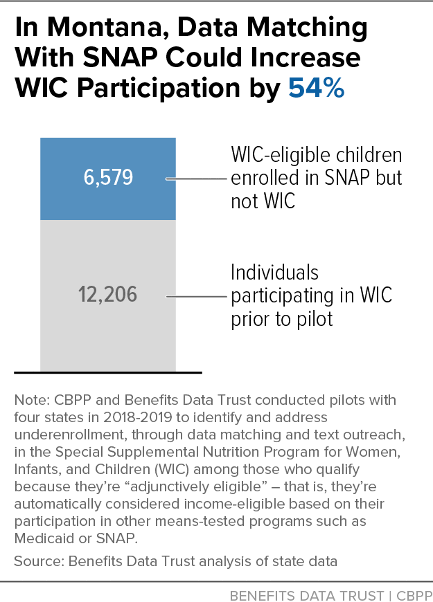- Home
- Food Assistance
- Using Data Matching And Targeted Outreac...
Using Data Matching and Targeted Outreach to Enroll Families With Young Children in WIC
Lessons Learned From State Pilots
Key Findings
- Data matching effectively identifies large numbers of adjunctively eligible families who are not participating in WIC
- Text outreach can positively impact WIC certification rates, particularly for Medicaid participants
- Texting is a practical mode of communicating with WIC-eligible families
- Parts of the WIC certification process pose barriers to adjunctively eligible families
- Data matching and text outreach are sustainable strategies and create opportunities for further cross-agency collaboration
The Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) provides millions of low-income families with pregnant and/or postpartum individuals, infants, or children up to age 5 access to nutritious foods, breastfeeding support, nutrition education, and referrals to health care and social services.[1] But a declining share of eligible families has participated over the past decade, despite the program’s well-documented dietary, health, and developmental benefits.[2] Missing out on sound nutrition in a child’s early years, a critical period of brain development, can have lasting negative consequences.[3] Evidence from randomized control trials indicates that using data from other programs to identify families eligible for WIC but not participating, and following up with text-based outreach to overcome WIC’s certification obstacles, can boost participation in this essential program.
Ideally all eligible families with a child under 5 would participate in Medicaid to receive consistent health care, the Supplemental Nutrition Assistance Program (SNAP, formerly food stamps) to be able to purchase food, and WIC to obtain key nutrition services and supplemental foods with nutrients that the diets of low-income women and young children tend to lack. Eligible families’ take-up of Medicaid and SNAP, while not universal, is much more robust than it is for WIC.[4] Over the past decade a declining share of eligible families have participated in WIC.[5] This has occurred despite Medicaid and SNAP participants being “adjunctively eligible” for WIC, that is, they are considered income-eligible for WIC and do not need to document their income to be enrolled.[6]
"Evidence from randomized control trials indicates that using data from other programs to identify families eligible for WIC but not participating, and following up with text-based outreach to overcome WIC’s certification obstacles, can boost participation in this essential program."
Adjunctive eligibility streamlines certification for WIC-eligible families by simplifying the eligibility determination process and can reduce administrative work for WIC staff by reducing the number of documents they need to review. The policy also signals that policymakers sought to facilitate WIC enrollment for families receiving Medicaid or SNAP. Nevertheless, the Department of Agriculture, which oversees WIC, has not attempted to measure whether states are successfully enrolling Medicaid or SNAP participants into WIC. It is also uncommon for state WIC programs to obtain data from Medicaid or SNAP to assess the extent to which they are reaching participants or to conduct targeted outreach. Because families participating in Medicaid or SNAP are eligible for WIC and have already sought out assistance, they appear to be a fruitful group for targeted WIC outreach.
In 2018 and 2019, the Center on Budget and Policy Priorities (CBPP) partnered with Benefits Data Trust (BDT), a national nonprofit that connects people in need to critical public benefits using data matching and targeted outreach, to launch pilot projects in four states. With teams from each state, we designed randomized waitlist control trials and evaluated interventions, to answer two key research questions:[7]
- What is the adjunctively eligible participation gap? That is, how many families receive benefits that confer adjunctive eligibility for WIC but are not enrolled in WIC?
- What is the impact of targeted, text-message-based outreach? Does it increase WIC enrollment for these adjunctively eligible families?
This report describes the pilot projects and synthesizes key findings, which suggest that this approach is feasible, sustainable, and, for certain groups, could increase the share of eligible families participating in WIC. The lessons learned could inform future initiatives to enroll Medicaid and SNAP participants in WIC or to conduct targeted, text-based outreach to facilitate access to this essential program.
Despite Proven Benefits, WIC Coverage Rate Has Declined for Nearly a Decade
Decades of research demonstrate WIC’s positive impact on the health and well-being of low-income families. Rigorous studies consistently demonstrate that WIC supports healthier pregnancies and births.[8] A growing body of research suggests that people who participate in WIC give birth to healthier infants than eligible non-participants.[9] In addition to improving outcomes at birth, WIC supports nutritious diets and promotes and supports breastfeeding, establishing healthful diets early in life. Moreover, WIC’s health impacts extend beyond nutrition as the program serves as a gateway to key health care services such as prenatal, obstetric, maternal, and pediatric care; dental care; and counseling for smoking cessation and drug and alcohol abuse.[10]
By supporting sound nutrition during critical periods of cognitive development, WIC helps mitigate the damaging effects that poverty can have on educational and social outcomes. Research shows that prenatal and early childhood participation in WIC is associated with improved cognitive development and academic achievement.[11] The research is also clear that receiving SNAP, WIC, and Medicaid in the early years has both short- and long-term benefits.[12] Therefore, it is important for every eligible child to get the full complement of benefits they qualify for, including SNAP, Medicaid, and WIC. In light of the high levels of hardship brought on by the COVID-19 pandemic, including food insecurity, it is more important than ever to ensure families are connected to all available economic and nutrition supports.[13]
Despite WIC’s many benefits, the share of eligible families participating in the program, or its “coverage rate,” has declined since 2011.[14] This nearly decade-long drop means that in 2017, the most recent year available, nearly 7 million eligible individuals were not receiving benefits and services that could demonstrably improve their health and well-being.[15]
State Pilots Tested Data Matching and Text-Based Outreach to Adjunctively Eligible Families
BDT and CBPP first collaborated with Colorado on a WIC pilot in 2018 to obtain SNAP data, measure the number of WIC-eligible participants who were not enrolled in WIC, conduct text-based outreach to this group, and assess the results. BDT and CBPP then collaborated from January 2019 through March 2020 with Massachusetts, Montana, and Virginia on similar pilots, obtaining SNAP and Medicaid data, as well as data from additional benefit programs to identify adjunctively eligible families and use texting to conduct targeted outreach to those who were not yet participating in WIC. In each pilot project, BDT and CBPP provided technical assistance and project management, but no funding, to state WIC agencies while the state agencies developed necessary data sharing agreements (DSAs) and conducted data matching. In two of the pilots BDT conducted the text-based outreach.
The pilots aimed to measure the extent to which families with children under the age of 5 who are enrolled in benefits that confer adjunctive eligibility for WIC (including Medicaid and SNAP) participate in WIC and to test the impact of text-based outreach strategies for these families who were eligible for WIC but not enrolled.
Each pilot followed the same general process from the outreach recipient’s perspective. First, the adjunctively eligible family received an outreach text encouraging them to schedule a WIC certification appointment. If the recipient responded to that text indicating interest in moving forward, their name then went onto a list for WIC staff to conduct follow-up calls. WIC staff then called interested individuals to schedule certification appointments for them. Finally, the individual attended their scheduled appointment to certify for WIC. After receiving technical assistance to launch pilots, Massachusetts and Montana decided to continue this model in ongoing operations and have expanded their data matches to include both SNAP and Medicaid for targeted outreach.
The pilots all shared certain features, which are described in the text box below.
Common Elements Across Data Matching and Text Outreach Pilots
- Data Share. Establish a data sharing agreement (DSA) and data transfer protocols between agencies.
- Data Match. Conduct a data match between WIC and at least one other means-tested program.
- Targeted Outreach. Use results of the data match to implement a targeted outreach campaign using texting to families eligible for but not enrolled in WIC.
- Custom Messaging. Craft customized engagement plans (documents that display the content and ordering of text outreach) containing messages to raise WIC awareness, reduce barriers to participation, and amplify the benefits of applying for WIC.
- Dynamic Communication. Use two-way texting to communicate with people responding that they would like to begin the WIC enrollment process.
- Follow-Up and Certify. Set up a process for WIC staff to follow up with families.
- Streamline Certification. Adopt simplified enrollment policies and processes for these adjunctively eligible families to streamline enrollment.
- Monitor Outcomes. Monitor text response rates and whether the recipient eventually enrolls in WIC.
- Evaluate Impact. Compare the WIC enrollment rate in a control group that did not receive texts to the rate for those who did.
While the four interventions and their outcomes differed in their details (see Table 1), five main observations were consistent across states, including:
- Substantial numbers of adjunctively eligible families are not participating in WIC. The data matches found large numbers of households enrolled in Medicaid, SNAP, and other programs that make them adjunctively eligible who are not participating in WIC. Data matching is an effective strategy for identifying these WIC-eligible families. Enrolling them in WIC would substantially increase WIC’s coverage rate.
- Targeted outreach can raise WIC certification rates. Evidence from Massachusetts and Virginia demonstrates that targeted text-based outreach can improve rates of WIC certification for segments of adjunctively eligible families. It would be useful to test variations on this targeted outreach approach to identify methods that more consistently increase certification rates for adjunctively eligible families.
- Texting is a viable, low-cost mode of communicating with WIC-eligible families. The texts sent out for each pilot successfully reached the vast majority of identified families and cost less than mail outreach.
- The WIC enrollment process poses barriers to interested eligible families. Among those who expressed interest in enrolling in WIC, only a subset completed the certification process, suggesting that aspects of certification policies and practices pose barriers to segments of eligible non-participating families. It would be useful to test mechanisms for helping more of the interested families complete the certification process.
-
Data-driven outreach is a sustainable way to reach WIC-eligible non-participants. These data sharing, data matching, and text outreach processes require an initial commitment of staff time to implement, but are not costly or burdensome once agencies incorporate them into their existing procedures. Agencies can adapt and build on these strategies according to their infrastructure and needs.
Massachusetts and Montana decided to continue this model in ongoing operations and have expanded their data matches to include both SNAP and Medicaid for targeted outreach.
The remaining sections of this report discuss these findings in greater detail and analyze the pilot methods to inform future policy and practice innovations involving matching data across programs, conducting targeted outreach, and streamlining WIC certifications.
| TABLE 1 | ||||
|---|---|---|---|---|
| Variations in Pilot Configurations in Colorado, Massachusetts, Montana, and Virginia | ||||
| Colorado | Massachusetts | Montana | Virginia | |
| Pilot Area | Partial state | Statewide | Partial state | Partial state |
| Program Data Matched With WIC | All SNAP households with a child under 5 | Recent Medicaid enrollees with a child under 5 | All SNAP households with a child under 5 | All SNAP, Medicaid, TANF, and foster care households with a pregnant person or a child under 5 |
| Pilot Size | 9,260 adjunctively eligible households not on WIC | 9,376 adjunctively eligible households not on WIC | 1,435 adjunctively eligible households not on WIC | 44,455 adjunctively eligible households not on WIC |
| Control Group Size | 2,821 households | 1,243 households | 628 households | 14,816 households |
| Streamlining Features |
|
|
|
|
Data Matches Identified Large Numbers of Families Adjunctively Eligible But Not Participating
The first step in each pilot was to establish a cross-agency data sharing agreement or to amend an existing agreement to suit the purposes of the pilot interventions. This process can be time consuming and resource intensive, especially for an initial agreement, but the pilot states agreed that the benefits of effective agreements are worth the effort.
One aspect of executing effective DSAs that can be especially nuanced is identifying the fields to be shared and the appropriate format for exchanging files. In general, each data element included in a DSA should have a specific purpose for being shared. Articulating the uses of data for each party included in the DSA will expedite legal review and enable the DSA to serve as a clear and effective guiding document. We approached this step by clearly articulating the intervention details, as well as the metrics and outcomes to be evaluated. In order to conduct text-based outreach, for example, it was necessary to include the exchange of phone number fields in the DSA.
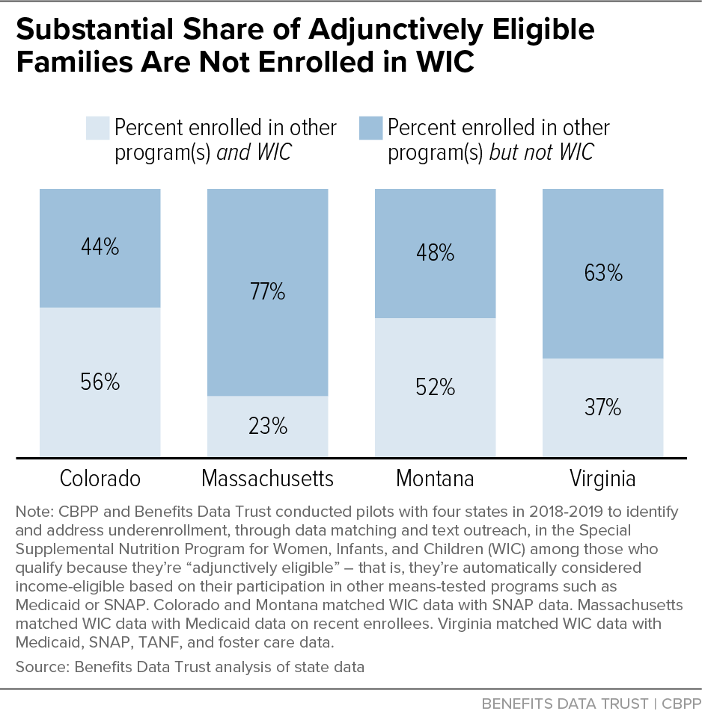
In each pilot, statewide data matching revealed large numbers of families enrolled in programs that make them adjunctively income eligible for WIC, but who were not participating. The matches found cross-program enrollment gaps ranging from 44 percent of WIC-eligible families on SNAP in Colorado not enrolled in WIC, to 77 percent of WIC-eligible recent Medicaid enrollees in Massachusetts not enrolled, as shown in Table 2 and Figure 1. Because Massachusetts matched WIC data with Medicaid data on recent enrollees, who might have had less time to apply for WIC, cross-enrollment across the full range of WIC-eligible Medicaid participants is likely higher.
| TABLE 2 | ||||
|---|---|---|---|---|
| WIC-Eligible Non-Participants Identified by Data Matches With Other Programs | ||||
| Colorado | Massachusetts | Montana | Virginia | |
| Program Data Matched With WIC | SNAP | Medicaid (recent enrollees) | SNAP | Medicaid, SNAP, TANF, Foster Care |
| WIC-Eligible & Enrolled in Program(s) Matched With WIC (Total) | 46,341 families | 39,715 families | 13,582 children | 158,875 families |
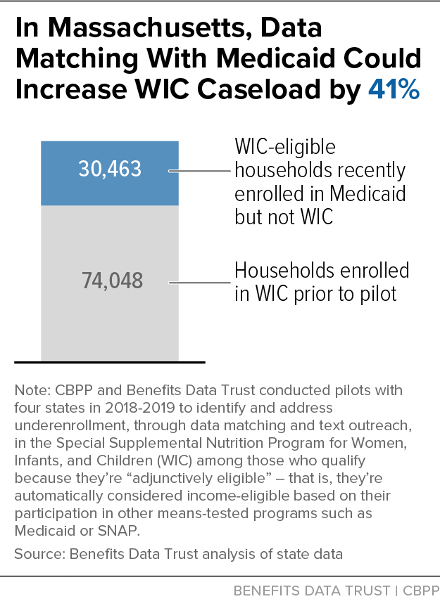
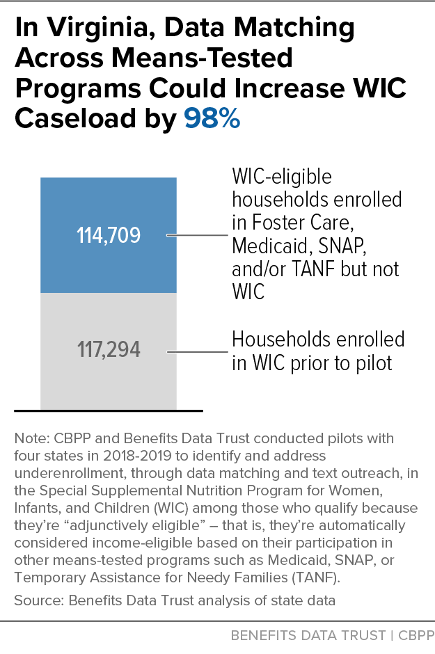
| WIC-Eligible & Enrolled in Program(s) Matched With WIC But Not in WIC | 20,191 families (44%) | 30,463 families (77%) | 6,579 children (48%) | 100,418 families (63%) |
This analysis demonstrates that data matching is an effective strategy for identifying large numbers of WIC income-eligible families. Furthermore, the large group of adjunctively eligible individuals identified through data matches represents a significant share of WIC-eligible non-participants, which policymakers can use to develop a strategy for substantially increasing WIC enrollment — ranging from a potential 28 percent increase in Colorado to a potential 98 percent increase in Virginia, as Figures 2-5 below illustrate.[16]
In summary, by conducting data matches across programs that confer adjunctive eligibility for WIC, states can:
- Identify the scale of participation gaps between WIC and other means-tested programs such as Medicaid and SNAP to demonstrate the value of cross enrollment;
- Identify many of the eligible individuals in a state that WIC is not yet reaching; and
- Develop strategies to boost WIC caseloads through targeted outreach and streamlined certification processes.
Text Outreach Can Increase WIC Certification Rates
The second key research question we explored through the four pilots was whether targeted outreach through a series of text messages to adjunctively eligible families increases WIC enrollment. Ultimately, while the results are mixed and not all outreach interventions resulted in certification increases, evidence from Massachusetts and Virginia indicates that text-based outreach can improve WIC certification rates for some adjunctively eligible families. Outcomes within and across states are summarized in Table 3.
| TABLE 3 | ||||
|---|---|---|---|---|
| Impact of Targeted Text Outreach on WIC Certification in CO, MA, MT, and VA | ||||
| Colorado | Massachusetts | Montana | Virginia | |
| Program Data Matched With WIC | SNAP | Medicaid | SNAP | Medicaid, SNAP, TANF, Foster Care |
| Number of Households in Intervention Group That Certified | 562 | 636 | 37 | 3,200 |
| WIC Certification Rate in Intervention Group | 6.1% | 6.8% | 2.6% | 7.4% |
| WIC Certification Rate in Control Group | 6.3% | 5.0% | 11.8% | 7.0% |
| Lift in Certifications Attributable to Outreach* | -3.1% | 36.0% | -77.9% | 5.7% |
*The differences in certification rates are statistically significant at p<.001 based on a chi-square test of independence.
The use of data from different programs across pilots allowed for a comparison. The results show that certifications were strongest among families who were initially enrolled in Medicaid. Massachusetts and Virginia results show that certification rates for Medicaid enrollees improve with text outreach; Massachusetts experienced a 36 percent increase in certifications in the intervention, but its control group might not represent a reliable baseline.[17] In Virginia, families on Medicaid were more likely than those receiving any other single benefit to take up WIC when they received text outreach; these families were 5 percent more likely to be certified for WIC than their control group counterparts.
Measuring certification outcomes also revealed that families who were enrolled in more than one program prior to the intervention were more likely to become certified for WIC through the pilot. Virginia’s pilot was the only one to include multiple programs. The Virginia evaluation demonstrated that individuals who were enrolled in more than one of the programs with which WIC data were matched prior to receiving pilot outreach were more likely to certify during the intervention than those enrolled in any single program. These families were 8.9 percent more likely to become certified for WIC than the control group, as shown in Table 4.
| TABLE 4 | |
|---|---|
| Virginia Families Receiving Medicaid or More Than One Benefit Were More Likely to Enroll in WIC as a Result of Outreach | |
| Original Benefit Enrollment | Lift in Certifications Attributable to Outreach |
| Medicaid Only (30,857 families) | +5.0% |
| SNAP Only (3,677 families) | -12.1% |
| Multiple Programs (24,266 families) | +8.9% |
| Any Benefit | +5.7% |
Note: The Virginia pilot also included TANF and foster care, which were significantly smaller than the SNAP, Medicaid, and multi-benefit groups. The group of 188 families receiving TANF enrolled in WIC at the same rate as the control group. The group of 283 families only participating in foster care were 14.8 percent more likely to certify for WIC as a result of outreach.
Across pilots, evaluations uncovered that SNAP households consistently did not experience an increase in certifications in the intervention groups compared to the control groups. In Colorado, where outreach was based only on a SNAP data match, the pilot intervention group became certified at roughly the same rate (6.1 percent) as the control group (6.3 percent). In Montana and Virginia, evaluations showed that SNAP participants were actually less likely to enroll in WIC after receiving outreach. One possible explanation for this unexpected finding, state staff speculated, is that because SNAP participants are already receiving a nutrition-related benefit, WIC’s supplemental foods aren’t as motivating. Further analysis is needed to understand this finding, which presents an opportunity to learn more from WIC-eligible families themselves about their decisions to participate or not, and also to track data on this group in future outreach interventions.
Looking forward, it would be useful to test variations on this targeted outreach approach to identify methods that more consistently increase certification rates for adjunctively eligible families. Interested families could be offered more assistance in navigating the certification process. For example, New York’s WIC program contracted with Hunger Solutions New York, a nonprofit anti-hunger organization, to identify families potentially eligible for WIC and help them navigate the enrollment process. Ten WIC Help Specialists, who worked at community-based organizations, conducted outreach, eligibility screening, and applicant assistance across 20 counties. They helped interested and likely eligible families find their local WIC clinic, schedule an appointment, and prepare the documents needed for certification. The WIC Help Specialists followed up to track whether the certification was completed and share feedback about the process with WIC staff.[18]
Alternatively, text messages could include links to an online appointment scheduler or an online application, which could simplify certification. Moreover, offering certification appointments via video call or telephone could improve attendance. In 2019 three local agencies in Vermont piloted offering mid-certification appointments by telephone; 80 percent of such appointments were kept in the pilot period, compared to 49 percent of in-person appointments.[19] Anecdotal evidence from waivers due to COVID-19 suggests that the ability to complete certifications remotely has improved certification appointment attendance rates. (Under the waivers, families may enroll or re-enroll in WIC without visiting a clinic and postpone providing certain health measurements.[20]) This strategy and others to make certification appointments more accessible for WIC applicants might also improve WIC access long term.
Texting Is a Viable, Low-Cost Mode of Communicating With WIC-Eligible Families
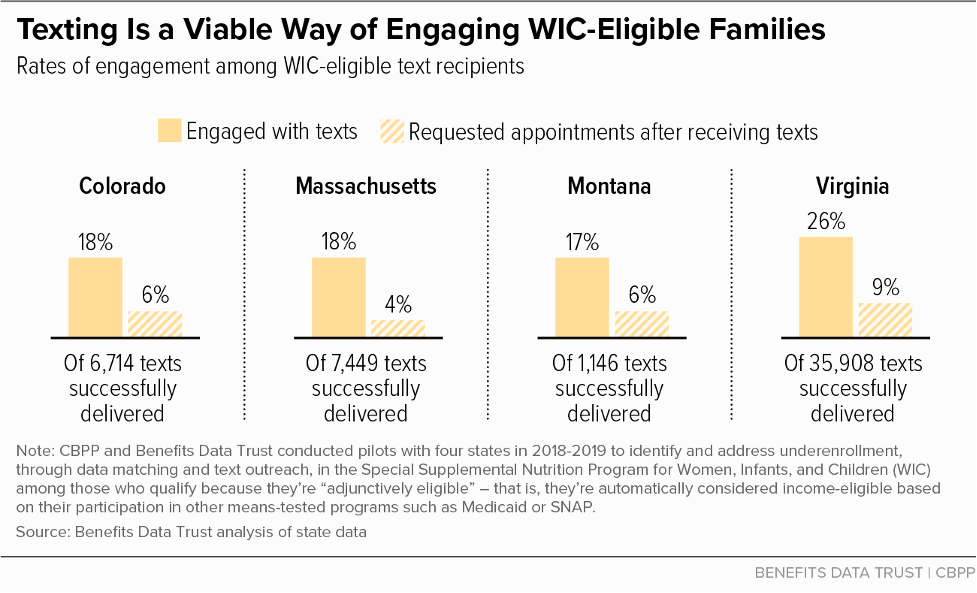
In addition to measuring the overall impact of text outreach on WIC certifications, pilot evaluations also monitored levels of engagement with text messages and found that texting is a viable way to reach WIC-eligible families. Because texting is a lower-cost method of outreach than mail, WIC agencies could employ it on an ongoing basis. We found that the vast majority of WIC-eligible families enrolled in other programs had mobile phones that could receive text messages: across states, close to 80 percent of the texts sent were successfully delivered.[21]
In addition to measuring rates of text message delivery, we also monitored text recipients’ level of engagement with the outreach messages. We considered any response other than those opting out of further messages — typically by responding “STOP” — an engagement with the texts. We found that levels of engagement differed across states, which was likely related to multiple factors that varied across pilots, including the program in which the text recipient was originally enrolled (SNAP, Medicaid, another program, or a combination of programs) and the messaging used in text outreach.
Importantly, the process each state followed to certify the pilot group also drove variations in text message content. For example, in most states, the outreach message asked recipients to reply “1” or “Yes” to receive a call from WIC staff to schedule a WIC certification appointment. In Massachusetts, however, segments of the intervention group received a link to an online form where they could enter their information and request a call from their local WIC program to schedule the appointment. Details about the text strategies and follow-up processes in each state are described in the Appendix.
Each state developed between two and four initial text messages with varying numbers of response options and varying numbers of follow-up messages. The content and order of messages were captured in an engagement plan. The initial text typically encouraged recipients to reply to begin the certification process, offered instructions for opting out of receiving messages, and sometimes included additional response options. Because we used dynamic two-way texting, the way individuals responded would determine the next text message they would receive through the engagement plan. Additional details on engagement plan content are available in the Appendix.
Families Were More Likely to Respond to Texts
That Mentioned Dollar Values and Familiar Benefit Programs
The Colorado pilot evaluation revealed an uptick in response rates to the third message, which mentioned a dollar figure for the value of WIC food benefits, and recipients continued to respond to the fourth message, which mentioned SNAP — an interesting result because response rates typically decrease with each additional message. Earlier messages focused on the health and nutrition benefits of WIC.
Given the Colorado findings, the other states mentioned the dollar value of WIC and referred to existing benefits in the first text, rather than focusing on health and nutrition, to maximize responses. In the case of Virginia, this shift in messaging, in combination with including individuals enrolled in not only SNAP but also Medicaid, TANF, and foster care, may have contributed to the pilot’s relatively higher rate of responses (26 percent compared to 18 percent in the other pilots).
While we observed this positive trend in responses to messages that mentioned dollar values and familiar programs, we did not conduct message tests in each pilot. Testing the effectiveness of different message content, number of messages, order of messages, and timing of messages is ripe for further exploration. a
a This kind of testing has been done in the context of appointment reminders. See Antonia Violante et al., “Learning How to Improve Retention in WIC,” ideas42, May 2020, http://ideas42.org/wp-content/uploads/2020/07/I42-1225_CA-WIC-Paper_May1.pdf
As Figure 6 shows, the share of families that received texts that engaged by responding with any option offered ranged from 18 percent to 26 percent across states. Among those responding, 22 percent to 34 percent requested WIC appointments. The varied response rates across pilots may reflect different strategies employed in each state’s engagement plan. See the Appendix for further details.
Additional text reminders throughout the certification process might improve the effectiveness of text outreach. If a family received personalized follow-up texts to help them navigate each step until they successfully certified, text-based support might result in a better conversion from interest to certification. Continued texting of this sort would require advanced integration across systems, since the system or person in charge of deploying texts would need to know each step a family completes in order to offer the right support on the next step in the process.
While texting appears to be an effective way of delivering information to potential applicants, it is far easier to respond to a text message indicating interest in enrolling in WIC than to complete the certification process. As described in the next section, most families that expressed interest in enrolling in WIC did not complete the process, which suggests that additional assistance or simplification would be helpful.
Aspects of WIC Certification Pose Barriers to Eligible Non-Participants
Among those who expressed interest in enrolling in WIC, only a subset completed the certification process, suggesting that aspects of certification policies and practices pose barriers to some eligible non-participating families.
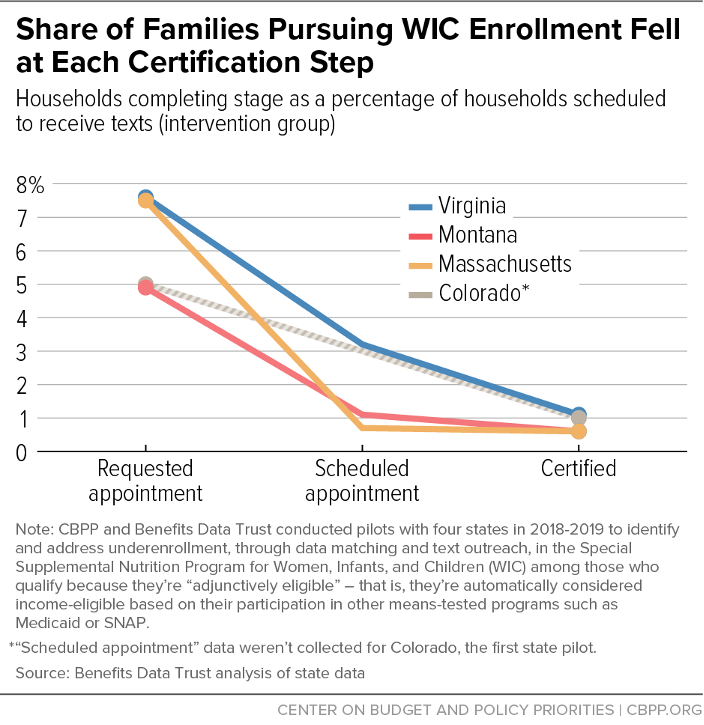
There are five major stages for families in the pilots, starting with being scheduled to receive texts and ending with becoming certified after completing an appointment with a local WIC agency. The stages must be completed in order, which means that each stage represents a potential drop-off point for families seeking WIC certification. Figure 7 illustrates the drop-off rate at different stages in the process where eligible families are required to take action in order to proceed. For example, many individuals who responded to a text by indicating that they wanted to receive a call to schedule an appointment dropped off before successfully scheduling the appointment. Other households scheduled a certification appointment but then did not show up. All pilot intervention applicants who attended certification appointments became certified.
The drop-off at each stage highlights the barriers posed by the WIC enrollment process and suggests that eliminating or simplifying the steps in the certification process could increase certification rates for participants in other programs as well as other eligible families. Key drop-off points included waiting for a call to schedule the appointment and, for those who scheduled an appointment, attending the appointment.
Future pilots, in combination with potential policy or operational changes, could help reduce these barriers and decrease the effort families need to devote to becoming certified. For example, if eligible families could schedule an appointment via text or online instead of awaiting a call, more families might successfully schedule appointments. If families were offered assistance in preparing for a certification appointment, they might be more likely to attend. If families could provide information and documents online prior to a certification appointment, the appointment itself could be shorter, which might increase the share of families that show up for their scheduled appointments. In addition, attending appointments in person can be difficult for families. If they could complete appointments by phone or video, more families might be able to successfully enroll in WIC.
Data Matching and Text Outreach Are Sustainable Strategies for Reaching WIC-Eligible Non-Participants
A key takeaway from these pilots was that data matching across state agencies and targeted text outreach are sustainable practices. Leadership across agencies also noted that these pilots strengthened cross-agency collaboration. These relationships can be beneficial in developing other interagency projects.
Massachusetts and Montana have decided to continue data matching and targeted text outreach, and both elected to include data from additional programs. This demonstrates that data matching and text-based outreach can be employed in ongoing operations. Once a data sharing agreement is in place, agencies can incorporate a process for sharing data and conducting text-based outreach into their routine activities. Bringing in a steady stream of new or returning families could help slow or reverse the decline in coverage rates.
Once these processes are implemented and incorporated into existing agency procedures, they are low-cost and relatively easy to administer. Agencies can build on these strategies and adapt them according to their infrastructure and needs. Some states are already conducting similar data matching and outreach projects and others are planning to launch this approach. State WIC programs can fund data matching and text-based outreach with their annual Nutrition Services and Administration grant or could apply for a one-time grant to establish these processes.[22]
Conclusion
By maximizing the use of data matching and technology to conduct targeted outreach and simplify the certification process, state WIC programs may be able to facilitate access to WIC, increase take-up by eligible families, and streamline agency operations at the state and local levels.
Pilots across four states — Colorado, Massachusetts, Montana, and Virginia — demonstrated that data matching with Medicaid, SNAP, and other programs identifies large numbers of eligible families who are not enrolled in WIC. They also showed that texting is an effective and sustainable way of reaching these families. By documenting where interested families dropped out of the enrollment process, the pilots also highlighted areas where simplifying and modernizing WIC’s certification process could help increase enrollment and retention for all eligible families.
While text-based outreach increased WIC enrollment for Medicaid participants and some other groups of adjunctively eligible families, the results were uneven for others. Therefore, it is important to continue exploring alternative methods that might more consistently result in WIC certification across adjunctively eligible groups. Moreover, now that the COVID-19 pandemic has required states to develop mechanisms of offering WIC services virtually, states will have an opportunity to retain certain modernizations and assess whether text-based outreach is more effective with these simplifications in place.
The Department of Agriculture or individual states could build on these pilots by regularly measuring the share of Medicaid and SNAP participants who are eligible for WIC but not participating and testing strategies to enroll them.[23]
Appendix: Outreach Text Follow-Up Processes in Each Pilot
Colorado WIC Pilot Process
The Colorado Department of Public Health and Environment (CDPHE) administers WIC statewide. At the local level, WIC is administered by 38 agencies that operate a total of 112 WIC clinics statewide.
CDPHE chose to match WIC enrollment data against SNAP data. Because BDT conducted the text outreach for this pilot, the state’s data sharing agreement had to include BDT. To launch the project, BDT amended an existing data sharing agreement (for ongoing SNAP outreach work) with the Colorado Department of Human Services (CDHS) — the agency that administers SNAP. Amending the agreement was a relatively simple process to navigate because of BDT’s ongoing partnership with the agency. BDT also had to secure a new data sharing agreement with CDPHE, which was a smooth process because of high-level buy-in at the agency.
BDT collaborated with CDPHE to select WIC agencies representing counties of various sizes for the pilot, and CDPHE coordinated with local agencies to determine which sites could handle a potential increase in workload as a result of the outreach. The counties selected serve just over half of the households identified by the data match.
The text engagement plan used in Colorado consisted of four initial outreach messages. These outreach messages included simple explanations of program eligibility, dietary counseling, and the potential monetary value of receiving WIC. BDT’s texting platform was programmed to send a different outreach message once a week for four weeks to recipients who had not yet elected to schedule an appointment with a WIC office or opted out of receiving text messages.
BDT’s texting platform sends “dynamic” text messages that offer recipients multiple response choices to questions and then automatically responds with a preset message. The first outreach text sent to each family also included an opt-out option, instructing text recipients that they could reply “Stop” at any time to stop receiving messages. For this pilot, individuals were sent messages that gave them the option to express interest in scheduling an appointment with a local WIC agency, ask for more information, or reply that they did not think they were eligible. BDT’s texting platform tracked these responses to identify the rate of recipient engagement with outreach messages.
When a recipient replied that they were interested in an appointment, their contact information was instantly added to the client record management (CRM) tool securely shared with participating WIC clinics. WIC staff used this CRM to call interested families and then updated each client’s status with one of the following options: 1st Message Left, 2nd Message Left, Unable to Leave Message, Appointment Scheduled, Missing Documents, Enrolled, Already Enrolled. When a status in the database changed, BDT’s texting platform automatically sent a corresponding text to the client reminding them to take action when appropriate or removed them from future outreach lists if additional outreach was no longer necessary.
Massachusetts WIC Pilot Process
The Massachusetts Department of Public Health (DPH) administers WIC statewide. At the local level, WIC is administered by 31 local agencies. DPH chose to match WIC enrollment data against Medicaid (called MassHealth in Massachusetts) rolls primarily because DPH already had a data sharing agreement between WIC and MassHealth to regularly receive a MassHealth file including individuals enrolled in the last quarter.
Massachusetts used its existing texting infrastructure (through Teletask) to send two-way texts to potentially eligible individuals who were enrolled in MassHealth and had a child under age 5 but were not enrolled in WIC.
DPH opted to run the pilot statewide with each local agency offering one of two pilot processes: a call back (referred to as the Call Group) or a link to an existing online form (referred to as the Link Group). The Massachusetts pilot was the only intervention to test offering different actions to schedule an appointment.
Massachusetts’ engagement plan contained a total of three outreach texts, the first of which was an introductory message notifying recipients they could opt out by responding “Stop” at any time and did not include a call to action. The second and third outreach messages had only one response option: the option for the Call Group was to reply “1” to receive a call back from their local WIC program. The Link Group’s reply option asked them to click a link to an online form where they could enter their contact information and request a call back to schedule an appointment. Nine agencies volunteered to be in the Call Group and the remaining 22 were assigned to the Link Group. This differs from the other pilots, which generally offered multiple response options, such as “Reply ‘2’ to learn more about WIC” that triggered additional interactive engagements.
After observing a drop-off from interest to successful certifications in the Colorado pilot, BDT and CBPP focused on how to reduce this drop-off in future pilots, beginning in Massachusetts. We primarily addressed this by developing special scripting alongside DPH that the WIC staff would then use during call-backs to inform families that because of their adjunctive eligibility, their certification would be simplified. The key simplification to certifications for the Massachusetts pilot was that families who were certified through the pilot process would only need to provide identification, but not other documents, such as proof of income, that are typically needed. This is because DPH was able to use the MassHealth ID obtained through the data match to confirm in advance of the certification appointment that the applicant was still participating in MassHealth, which documented adjunctive income eligibility and residency.
Montana WIC Pilot Process
The Montana Department of Public Health and Human Services (DPHHS) administers WIC statewide. At the local level, WIC is operated by 87 local agencies. For this pilot, Montana matched WIC enrollment data against SNAP data.
Like Massachusetts, Montana used Teletask to send two-way texts to potentially eligible individuals. To determine the pilot jurisdiction, DPHHS reached out to local agencies directly to inform them of the project and gauge interest in participating, then had interested agencies complete an application. DPHHS received applications back from 12 local agencies. After conducting the data match, DPHHS selected five agencies for the pilot, representing a range of small, medium, and relatively large caseloads.
Montana’s engagement plan contained a total of four messages. We originally planned on sending two outreach messages but added two more messages after observing low response rates early on. As in Colorado and Massachusetts, the first outreach text sent to each family also included an opt-out, instructing text recipients that they could reply “STOP” at any time to stop receiving messages. The sole call to action was “Reply YES to receive a call from your WIC clinic to get started,” which appeared in each engagement. Outreach texts also included the option to reply “MORE” for more information about WIC.
As in the Massachusetts pilot, we developed special scripting for WIC staff in Montana to follow when calling back clients who expressed interest via text to schedule their WIC certification appointments. DPHHS, BDT, and CBPP worked together to craft this scripting, which also instructed Montanans that they only needed to bring identification to their certification appointment, as was the case in Massachusetts.
Virginia WIC Pilot Process
The Virginia intervention was the most expansive of the pilots conducted. We worked with the Virginia Department of Health (VDH), which administers WIC, and the Virginia Department of Social Services (VDSS), which administers other state programs. At the local level, WIC is operated by 35 Local Health Districts.
The Virginia team decided to use multiple programs’ data to generate the largest possible list of adjunctively eligible families, including SNAP, Medicaid, and TANF. They also matched against foster care rolls. As VDH did not have two-way texting capabilities, BDT conducted the text outreach.
The pilot required a new DSA because the state agencies did not have existing agreements and because of BDT’s direct involvement conducting text outreach on VDH’s behalf. We executed a three-way DSA between VDH, VDSS, and BDT. VDSS matched the file of WIC households against their list of Medicaid, SNAP, TANF, and foster care households with a child under age 5, then sent the anonymized outcomes of this match in the form of de-identified phone numbers, which made up the outreach pool, to BDT.
Another unique component of the Virginia pilot was that VDH used a central help desk to call people who responded by text that they wanted to make a certification appointment, rather than having local agencies manage this process. The help desk scheduled appointments at the appropriate local agency for each client, which streamlined operations with local WIC agencies.
BDT used a series of four engagements, each with the same call to action as in the initial outreach (with slight rephrasing across engagements): “Reply 1 to get a call from WIC to get started.” Messages also included alternate options such as: “Reply 2 for more info on how WIC fits into your family’s lifestyle” and “Reply 3 if you don’t think you qualify.” In addition, because VDH used a central help desk with a single hotline phone number, we were able to include the number in engagement plans. Once someone requested a WIC appointment via text, they received a follow-up text including this phone number so that they could call the help desk themselves if they wanted to get started right away rather than waiting for a call back.
VDH initially expected to include all local WIC agencies in the pilot and presented the opportunity to local WIC Directors. Ultimately, 21 of 35 local agencies opted in (serving approximately 75 percent of Virginia’s WIC caseload). The local agencies that did not opt in were generally concerned about the additional workload associated with the pilot.
As in the Massachusetts and Montana pilots, BDT and CBPP worked with VDH to develop scripting for the WIC staff carrying out pilot operations. This served as a desk-guide for VDH help desk staff handling pilot client calls. Although applicants identified through the pilot were likely adjunctively eligible, this did not result in a streamlined certification process for them in this case, so the instructions they received for their appointment were the same as for other callers. The scripting document offered suggested responses for callers with legitimacy concerns and/or callers declining WIC due to common barriers or misconceptions. Input from frontline staff shaped the content of this document.
Tracking the COVID-19 Economy’s Effects on Food, Housing, and Employment Hardships
End Notes
[1] Jess Maneely is with Benefits Data Trust and Zoë Neuberger is with the Center on Budget and Policy Priorities.
[2] See Steven Carlson and Zoë Neuberger, “WIC Works: Addressing the Nutrition and Health Needs of Low-Income Families for 40 Years,” Center on Budget and Policy Priorities, revised March 29, 2017, https://www.cbpp.org/wicworks.
[3] See Sarah Jane Schwarzenberg, Michael K. Georgieff, and the Committee on Nutrition, “Advocacy for Improving Nutrition in the First 1000 Days to Support Childhood Development and Adult Health,” Pediatrics, No. 141, Vol. 2, February 2018, https://pediatrics.aappublications.org/content/141/2/e20173716.
[4] For information on participation by eligible individuals in Medicaid and SNAP, see Kaiser Family Foundation, “Medicaid & CHIP,” https://www.kff.org/state-category/medicaid-chip/medicaid-and-chip-participation-rates/; and U.S. Department of Agriculture, Food and Nutrition Service, “Trends in SNAP Participation Rates: Fiscal Year 2010-2017,” September 12, 2019, https://www.fns.usda.gov/snap/trends-supplemental-nutrition-assistance-program-participation-rates-fiscal-year-2010.
[5] Participation by eligible individuals in WIC declined from 64 percent in 2011 to 51 percent in 2017. See Zoë Neuberger, “Streamlining and Modernizing WIC Enrollment,” updated February 20, 2020, www.cbpp.org/wiccasestudies.
[6] Along with Medicaid and SNAP, individuals qualify by virtue of participation in Temporary Assistance for Needy Families cash assistance (TANF). While all income-eligible individuals also must be at nutritional risk to qualify for WIC, income-eligible families generally meet one of the nutritional risk criteria. For more details about the adjunct eligibility rules, see 7. C.F.R. § 246.7 (d)(2)(vi).
[7] A randomized waitlist control trial is an intervention design where participants are randomly assigned to either the intervention group or control group. The “waitlist” element of this design refers to the option for the control groups to receive the treatment at a later date.
A technical error during the Massachusetts intervention caused the Massachusetts control group to receive texts during the pilot before they were scheduled to. To simulate a control group, we used the next quarter of Medicaid data to withhold a control group from any text outreach initiatives and measure enrollment outcomes over a period similar to that of the pilot duration.
[8] See Carlson and Neuberger, op. cit.
[9] Ibid.
[10] Ibid.
[11] Ibid.
[12] See Douglas Almond, Hilary W. Hoynes, and Diane Whitmore Schanzenbach, “Inside the War on Poverty: The Impact of Food Stamps and Birth Outcomes,” Review of Economics and Statistics, May 2011, https://www.mitpressjournals.org/doi/pdfplus/10.1162/REST_a_00089; and CBPP, “Medicaid Works for Children,” January 19, 2018, https://www.cbpp.org/research/health/medicaid-works-for-children.
[13] See CBPP, “Tracking the COVID-19 Recession’s Effects on Food, Housing, and Employment Hardships,” updated December 18, 2020, https://www.cbpp.org/research/poverty-and-inequality/tracking-the-covid-19-recessions-effects-on-food-housing-and.
[14] See Neuberger, op. cit.
[15] See U.S. Department of Agriculture, Food and Nutrition Service, “WIC 2017 Eligibility and Coverage Rates,” April 9, 2020, https://www.fns.usda.gov/wic-2017-eligibility-and-coverage-rates.
[16] In Massachusetts and Virginia, analyses on the potential boost to WIC enrollment were conducted using WIC caseload data (see figures 3 and 5). In Colorado and Montana, these analyses were based on WIC participation, the subset of the caseload that is actively receiving food benefits (see figures 2 and 4).
[17] A technical error caused the original control group to receive texts during the intervention. To preserve our ability to evaluate the intervention, we newly created a control group using the next quarter of MassHealth data and withheld a group from text outreach initiatives following the pilot. We measured enrollment outcomes for this new control group over a period similar to that of the pilot duration. Though there are limitations to drawing conclusions, the intervention outcomes suggest that texting may be a viable strategy for reaching Medicaid participants who are adjunctively eligible for WIC, with an approximately 36 percent increase in enrollments compared to the modeled control.
[18] New York Hunger Solutions shared that over the course of two years, WIC Help Specialists conducted face-to-face outreach with more than 35,000 individuals potentially eligible for WIC, pre-screened more than 8,600 individuals, and referred more than 4,200 eligible individuals to WIC clinics, of whom more than 3,400 were then certified for benefits according to WIC agencies. Hunger Solutions New York maintains outreach materials used by WIC Help Specialists on WICHelpNY.org’s Resource Center, at https://hungersolutionsny.org/federal-nutrition-programs/wic/resources/, for statewide partner use.
[19] See Neuberger, op. cit.
[20] See U.S. Department of Agriculture, Food and Nutrition Service, “WIC - Physical Presence Waiver,” https://www.fns.usda.gov/disaster/pandemic/covid-19/wic-physical-presence-waiver.
[21] The percentages of texts sent in each state that were successfully delivered were: Colorado, 73 percent; Massachusetts, 79 percent; Montana, 80 percent; and Virginia, 81 percent.
[22] For example, a state could apply for dedicated WIC funds, such as operational adjustment funding or an infrastructure grant. See 42 U.S.C. § 1786(h)(10)(B)(i).
[23] There is already legislative interest in such measures. Legislation introduced in February 2020 directs the U.S. Departments of Agriculture (USDA) and Health and Human Services to develop a state-by-state measure of the share of pregnant women and children under 5 receiving SNAP and Medicaid who are not enrolled in WIC and directs states to develop annual cross-enrollment plans and referral practices, while providing competitive grants and technical assistance to support implementation. See the WIC Enrollment Collaboration Act of 2020, S. 3357, introduced by Senator Brown, February 27, 2020, https://www.congress.gov/116/bills/s3357/BILLS-116s3357is.pdf. In addition, the report accompanying the fiscal year 2021 House agriculture appropriations act directed USDA to publish state-level estimates of the percentage of pregnant women, infants, and children under 5 participating in Medicaid or SNAP but not WIC. See “Agriculture, Rural Development, Food and Drug Administration, and Related Agencies Appropriations Bill, 2021,” Report 116 446, July 13, 2020, page 73, https://www.congress.gov/116/crpt/hrpt446/CRPT-116hrpt446.pdf.
More from the Authors

Jess Maneely is with Benefits Data Trust.