Matching Data Across Benefit Programs Can Increase WIC Enrollment
Greater WIC Participation Can Boost Health and Developmental Outcomes for Low-Income Pregnant Individuals and Young Children
Table of Contents
Overview
Why Is It Worthwhile to Enroll More Medicaid and SNAP Participants in WIC?
- How Medicaid Participants Can Benefit From Participating in WIC
- How SNAP Participants Can Benefit From Participating in WIC
- How Data Matching and Targeted Outreach Can Be Used to Increase WIC Enrollment
Sharing Data to Improve WIC Program Reach
- To What Extent Are Medicaid and SNAP Participants Not Participating in WIC?
- How Much of the Coverage Gap Could States Fill?
- How Can Other Programs’ Data Be Used to Streamline WIC Enrollment?
- What Impact Might Data-Driven Outreach Have on WIC Certifications?
Key Considerations When Developing a Data-Sharing Agreement
- Which Data Sources Will Be Used?
- How Often Will Data Be Shared?
- What Data Elements Will Be Shared?
- How Can States Avoid Reaching Out to Families Already Enrolled in WIC?
- What If a State’s WIC Program Is Administered by a Different Agency Than Medicaid or SNAP?
- How Can States Incorporate Data Sharing Into Ongoing Operations?
How Can a State Get Started?
Overview
The Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) works alongside Medicaid and the Supplemental Nutrition Assistance Program (SNAP, formerly food stamps) to help families weather financial distress, maintain health and wellness, and improve economic prospects. Although Medicaid and SNAP participants are automatically income-eligible for WIC, many don’t enroll. Pilot projects in four states have shown that matching data across programs to identify these families and conducting outreach to them can increase WIC enrollment.
WIC, which provides healthy foods, breastfeeding support, nutrition education, and referrals to health care and social services, plays a crucial role in improving long-term health outcomes for women, their infants, and young children.WIC, which provides healthy foods, breastfeeding support, nutrition education, and referrals to health care and social services, plays a crucial role in improving long-term health outcomes for women, their infants, and young children. Part of the nation’s nutrition safety net for over 45 years, WIC serves over 6 million pregnant and postpartum individuals, infants, and children through their fifth birthday. WIC provides food worth an average of about $147 per month for infants, $38 for pregnant and postpartum individuals, and $34 for children. A family eligible to participate must have gross income of no more than 185 percent of the federal poverty level (now $40,182 for a family of three) and be at nutritional risk.[1] To simplify eligibility determinations, an applicant who already receives SNAP, Medicaid, or Temporary Assistance for Needy Families cash assistance (TANF) is automatically considered income-eligible, or adjunctively eligible, for WIC.[2]
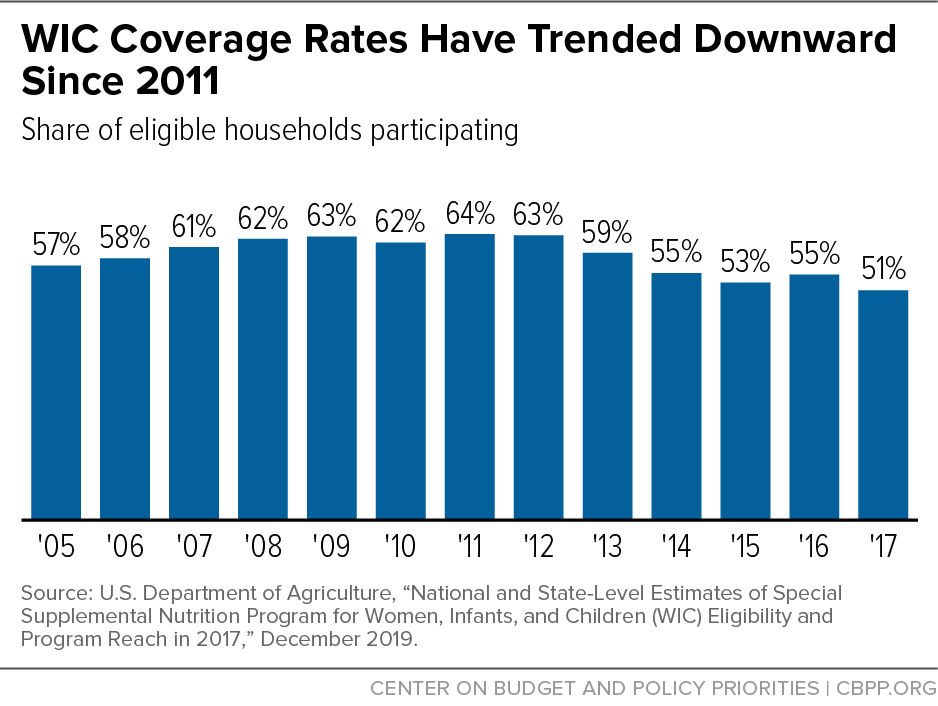
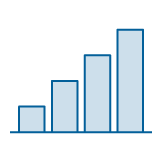
While not all eligible families participate in Medicaid and SNAP, take-up of these programs is much more robust than take-up of WIC. Over the past decade, the share of eligible families participating in WIC, referred to as the coverage rate, has fallen.[3] (See Figure 1.) Even during the pandemic, when food hardship has surged for families with children, WIC participation has grown more slowly than Medicaid or SNAP participation.[4] Enrolling more Medicaid and SNAP participants in WIC would be one way to help reverse this trend, while also improving the diets and health of those participants.
Pilot projects in Colorado, Massachusetts, Montana, and Virginia demonstrated that by matching data across programs to identify families enrolled in Medicaid or SNAP but not WIC, and conducting outreach to them, states can increase WIC enrollment for Medicaid participants — which may improve health and developmental outcomes — and provide additional food assistance to SNAP recipients. Effectively enrolling a greater share of Medicaid and SNAP participants in WIC could increase the share of eligible families participating in WIC. By increasing WIC’s coverage rate, states can support healthier pregnancies, improve birth outcomes, and improve child health and cognitive development for low-income families, potentially reducing striking racial disparities.
Moreover, for adjunctively eligible families, the WIC enrollment process can be further simplified by reducing duplicative paperwork for applicants and allowing WIC staff to focus on providing services. To modernize WIC outreach and streamline program administration, states can establish sound data-sharing agreements that enable targeted outreach and simplify the WIC enrollment process, facilitating integration of these improvements into regular business operations.
This brief describes how data sharing and matching can help achieve these goals and outlines key considerations for executing a data-sharing agreement.
Why Is it Worthwhile to Enroll More Medicaid and SNAP Participants in WIC?
Every eligible low-income family with a child under 5 years old would ideally participate in Medicaid to receive consistent health care; SNAP to be able to buy groceries; and WIC to obtain supplemental foods with essential nutrients, as well as nutrition education and breastfeeding support. Ensuring that low-income families with young children are enrolled in all three programs, to the extent they are eligible, has the potential to improve nutrition, health, and developmental outcomes. As different state agencies sometimes administer each of these programs, support from high-level policymakers can boost cross-program enrollment efforts. By comparing data across these programs, governors and other state policymakers can identify participation gaps between the programs (referred to here as enrollment gaps) and take concrete steps to increase cross-program enrollment, thus providing a more robust package of supports for low-income families.
How Medicaid Participants Can Benefit From Participating in WIC
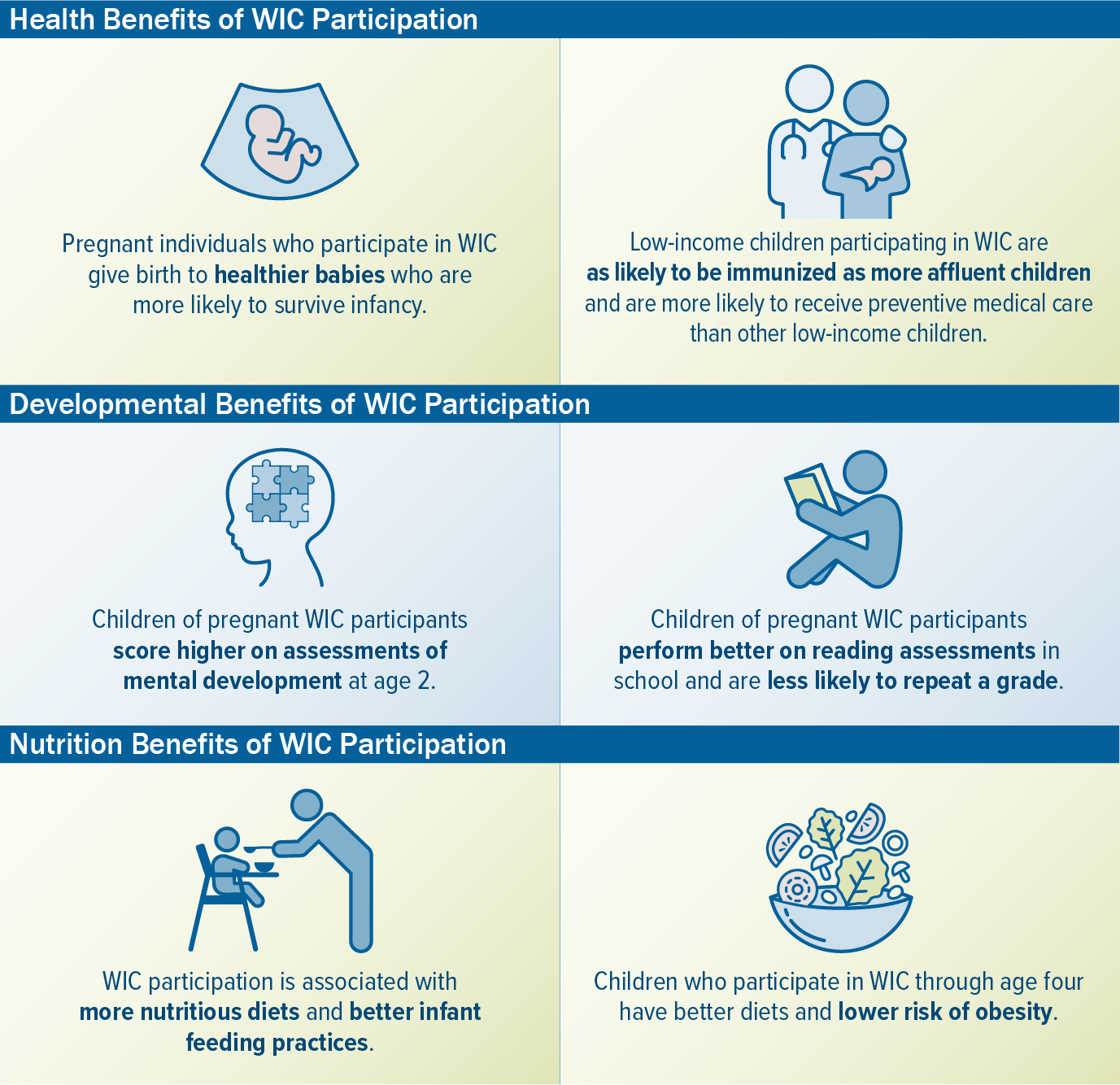
Enrolling pregnant individuals, infants, and young children who participate in Medicaid in WIC could help improve their diets, addressing a key social determinant of health, and could reduce health care costs.[5] Four decades of extensive research have found that participating in WIC improves nutrition and health.[6] WIC participation is associated with more nutritious diets and better infant feeding practices. Low-income children participating in WIC are as likely to be immunized as more affluent children and are more likely to receive preventive Medicaid care than other low-income children. Pregnant individuals who participate in WIC give birth to healthier babies who are more likely to survive infancy; the effects tend to be largest for children born to the most disadvantaged parents.[7]
The unfortunate reality is that people of color are at disproportionate risk of pregnancy-related and infant mortality as a result of long-standing inequities that often stem from structural racism. Black people are three times more likely to die as a result of pregnancy than white people. The infants of Black, Native Hawaiian, and other Pacific Islander women are at higher risk of preterm birth and low birth weight and are more than twice as likely to die as infants of white women. Connecting people who are at greater health risk as a result of pregnancy, and whose infants face greater risks, to WIC’s services, while increasing WIC coverage across the board, could play a role in a broader strategy to mitigate racial and ethnic disparities and to improve pregnancy and child health outcomes.[8]
How SNAP Participants Can Benefit From Participating in WIC
Food insecurity among children is associated with many adverse consequences for cognitive development as well as for school readiness, academic performance, and educational attainment; physical, mental, and social health; and behavior.[9] SNAP benefits are meant to reduce food insecurity by filling the gap between the money families have available to buy food and the amount needed for a basic heathy diet. But SNAP’s modest benefits are inadequate to fill the gap.[10] Enrolling SNAP participants in WIC would give them additional food benefits to help mitigate food insecurity.[11] These benefits are tailored to provide nutrients that tend to be lacking in the diets of low-income pregnant and postpartum individuals and young children. Moreover, WIC provides nutrition education, breastfeeding support, and referrals to other services beyond what SNAP is equipped to offer.
During the past year, food hardship due to the COVID-19 health and economic crises has grown at an alarming rate, disproportionately affecting households with children and communities of color.
- Nearly 1 in 7 children are in households where the children didn’t eat enough in the last seven days because the household couldn’t afford it, recent Census data showed.
- That translates to up to 9 million children, eight times the 1.1 million children in December 2019 who were living in households where the children didn’t get enough to eat at any point in the last 30 days.[12]
- Up to 25 percent of children in Black households and up to 23 percent in Latino households (based on the race or ethnicity of the parent) live in households where children didn’t eat enough in the last seven days because the household couldn’t afford it, compared to
7 percent of children in white households.[13]
Even short periods of food insecurity pose long-term risks for children. Increasing WIC coverage across the board, and especially increasing participation by families of color, could help reduce food hardship and mitigate racial and ethnic disparities.
How Data Matching and Outreach Can Be Used to Increase WIC Enrollment
States may wish to explore multiple avenues to strengthen cross-program enrollment, including:
- measuring the gap, specifically, of how many pregnant individuals and how many children under age 5 who participate in Medicaid or SNAP are not participating in WIC;
- sharing Medicaid and SNAP enrollment data with WIC so staff can conduct targeted outreach to eligible non-participants;
- adding WIC to multi-benefit online applications;
- strengthening referrals from Medicaid and other health care providers to WIC; and
- embedding WIC services into health care settings.
To explore the possibilities of the first two avenues of strengthening cross-program enrollment, the Center on Budget and Policy Priorities (CBPP) and Benefits Data Trust (BDT) partnered with Colorado, Massachusetts, Montana, and Virginia to launch pilots to measure how many people were adjunctively eligible for WIC but not enrolled, and to test whether outreach in the form of a series of text messages could help increase these families’ WIC enrollment.[14]
The remainder of this paper draws on lessons learned from conducting the pilots to describe: (1) the potential impact of data sharing as a strategy for addressing the downward trend in WIC coverage, including the results of the pilots; and (2) key considerations when developing a data-sharing agreement.
Data Sharing Creates Opportunities for More Cross-Agency Collaboration
State officials in the four states that we partnered with to conduct WIC data matching pilots noted that participating in the pilots fostered and strengthened cross-agency collaboration. These relationships can be beneficial in developing interagency solutions for expanding access to essential programs and ensuring families can easily access programs for which they are eligible, which can help them meet their basic needs and alleviate the lasting hardship of the COVID-19 pandemic.
“I’ve been with the state for seven years and the kind of collaboration between the health department and social services was something I never would have thought was possible in light of our silos, so I really appreciate all the work on data matching.”
— Health department official
“It was a great collaboration with the health department and the WIC program. Being able to reach out to our families using a different platform was great. And being able to get out of our own silos, talking to each other, was just awesome. I’m looking forward to being able to implement more cross-department initiatives.”
— Medicaid official
“Our state agencies are definitely aware of the potential of collaborating on data sharing and analysis to improve the effectiveness of our outreach efforts. The WIC, SNAP, and Medicaid programs are managed by three different state agencies. But we serve many of the same families and have mutual interest in finding better ways to reach and serve them. We really appreciated the opportunity to connect SNAP participants with the services and additional food benefits that WIC provides.”
— Social Services Research Director
“We were very pleased with the project, the people we were able to reach, and the people we were able to enroll in WIC. In our mind it was well worth the effort.”
— WIC official
“I’m excited that we used modern technology to reach out to Medicaid members. We know it’s effective because we immediately see an increase in applications to WIC.”
— WIC official
Sharing Data to Improve WIC Program Reach
Some WIC agencies have been experimenting with many forms of outreach to reverse the downward trend in WIC coverage. Because Medicaid and SNAP participants are adjunctively eligible for WIC and have already sought other forms of government assistance, they are a fruitful group for WIC outreach. Data matching allows states to measure the magnitude of the gap between Medicaid or SNAP participation and WIC, to identify individuals for outreach, and to simplify WIC enrollment processes for them.
Congress recently directed the Department of Agriculture (USDA) to publish state-level estimates of the percentage of pregnant individuals, infants, and children under 5 participating in Medicaid or SNAP but not WIC.[15] Once available, these estimates will offer more comprehensive data to inform WIC outreach strategies to reach adjunctively eligible families and will create a baseline against which to measure progress over time. In the meantime, the pilot results shed some light on the magnitude of the enrollment gap.
To What Extent Are Medicaid and SNAP Participants Not Participating in WIC?
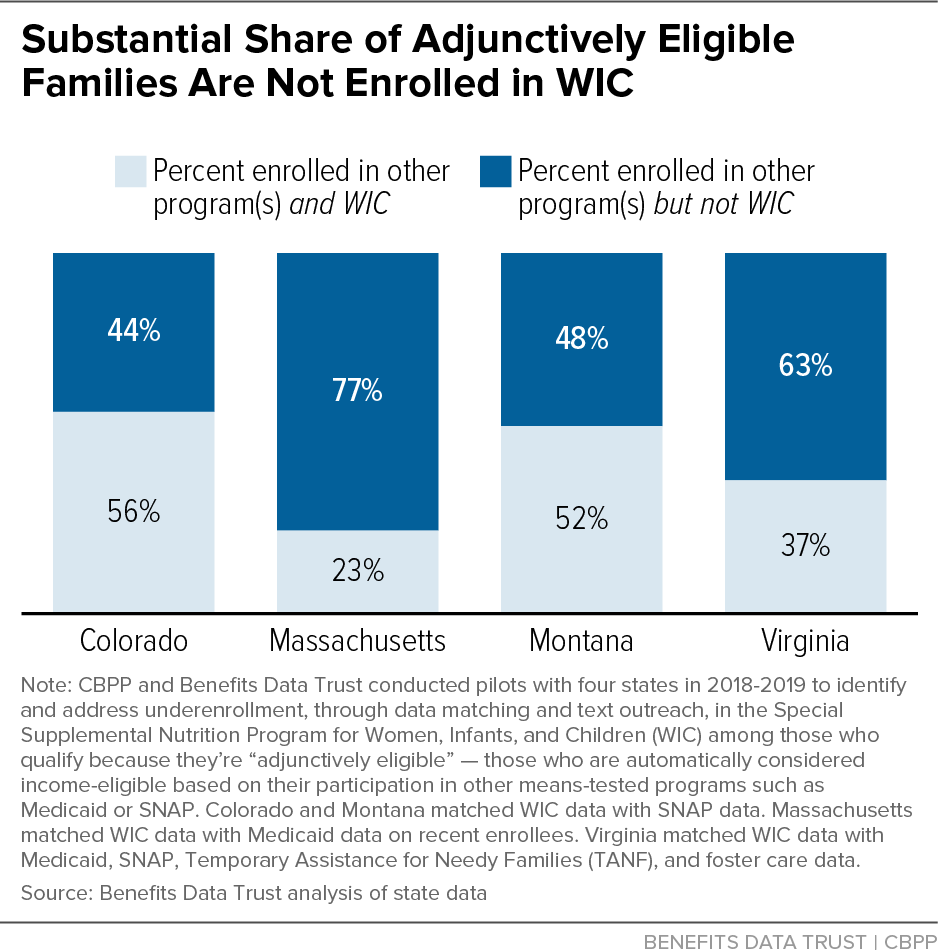
Once they had data-sharing agreements in place, Colorado, Massachusetts, Montana, and Virginia each conducted a baseline statewide data match to identify individuals participating in Medicaid and/or SNAP but not WIC.[16] The matches found cross-program enrollment gaps ranging from 44 percent of WIC-eligible families participating in SNAP in Colorado not enrolled in WIC to 77 percent of WIC-eligible recent Medicaid enrollees in Massachusetts not enrolled. (See Figure 2.) Because Massachusetts matched WIC data only with Medicaid data on recent enrollees, who thus might have had less time to apply for WIC, cross-program enrollment across the full range of WIC-eligible Medicaid participants is likely higher.
How Much of the Coverage Gap Could States Fill?
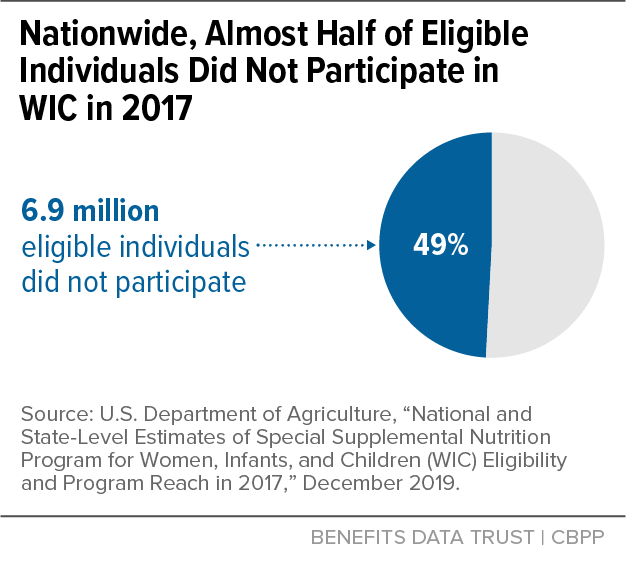
USDA estimated that 6.9 million eligible individuals, or about 49 percent, were not participating in WIC in 2017.[17] (See Figure 3.) The pilot projects showed that cross-program data matching can effectively identify many of these people at the individual level. Enrolling them in WIC would substantially increase WIC participation and help close the WIC coverage gap — that is, the gap between the number of individuals eligible for WIC and those participating. For example, if all the adjunctively eligible individuals identified through data matching in the pilot projects were to enroll in WIC, the impact on WIC enrollment would range from a potential 28 percent increase in Colorado to a potential 98 percent increase in Virginia.[18]
How Can Other Programs’ Data Be Used to Streamline WIC Enrollment?
Once states have identified Medicaid and SNAP participants who are not enrolled in WIC, states can offer them a simplified enrollment process. Enrollment for adjunctively eligible families can be streamlined in ways that promote easier access to this critical benefit for families as well as administrative efficiencies for staff. For example, confirming adjunctive eligibility through a data match before a certification appointment can eliminate the need for families to document income eligibility or enrollment in another program, since the WIC staff would already have access to that information. WIC’s other documentation requirements — identity and residence — may also be met by information obtained through the data match, reducing the documentation burden on WIC applicants. This, in turn, supports efficient program administration by reducing the amount of manual data entry and paperwork for WIC staff to process.
What Impact Might Data-Driven Outreach Have on WIC Certifications?
Evidence from Massachusetts and Virginia suggests that outreach in the form of text messages can positively impact WIC enrollment rates for adjunctively eligible families. Individuals identified through data matching as participating in another program but not WIC were sent a series of text messages encouraging them to request an appointment to enroll in WIC.
The results showed enrollment increases among families that were initially enrolled in Medicaid but not WIC. Families participating in Medicaid in Virginia were 5 percent more likely to be enrolled in WIC as a result of the pilot than families that did not receive text outreach through the pilot.[19] In addition, families that were enrolled in more than one program prior to the intervention were more likely to become certified for WIC through the pilot. In Virginia, families enrolled in more than one of the programs with which WIC data were matched were 8.9 percent more likely to become certified as a result of the pilot.
Families enrolled in SNAP but not WIC, however, did not enroll in WIC at a higher rate as a result of the pilots in Colorado, Montana, or Virginia. While the pilot evaluations did not identify a clear reason for this outcome, this finding illustrates the need to further explore how to effectively connect WIC-eligible families enrolled in SNAP to the WIC program.
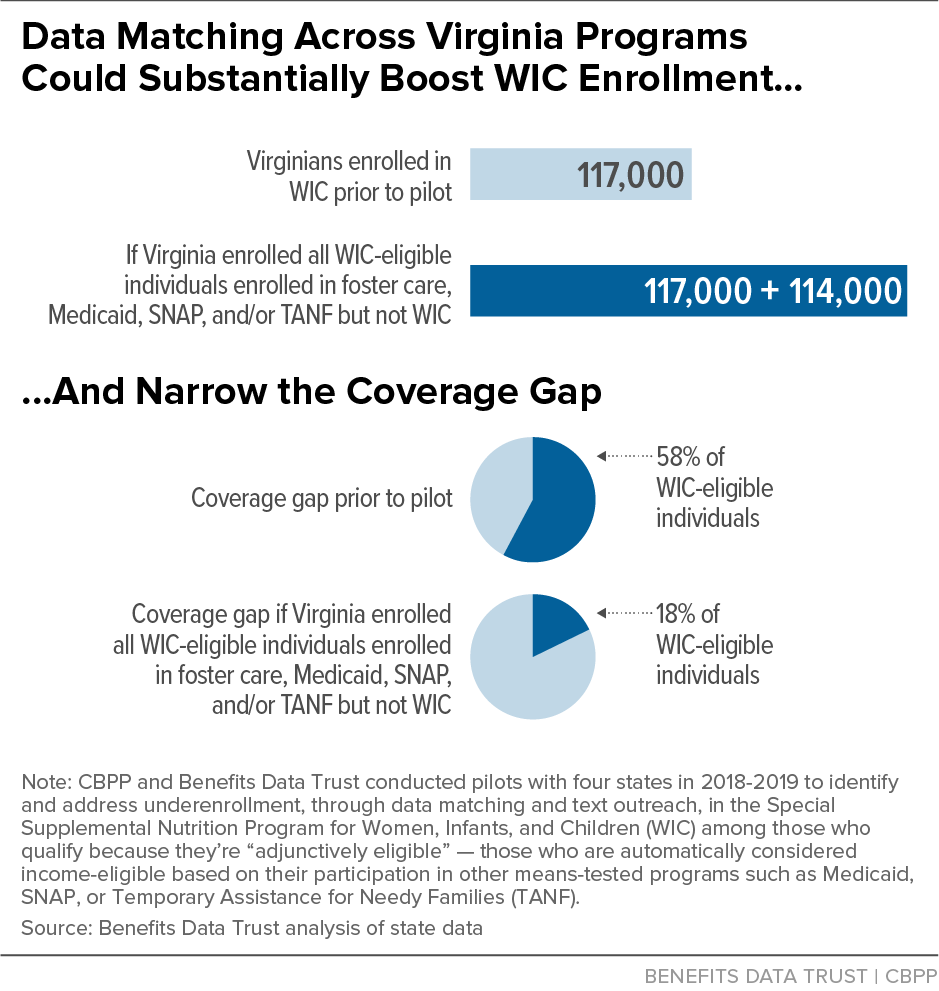
Enrolling All Adjunctively Eligible Families in Virginia in WIC Would Nearly Double the WIC Caseload and Close Most of the WIC Coverage Gap
The Virginia pilot implemented the most robust data match, comparing WIC data to SNAP, Medicaid, Temporary Assistance for Needy Families, and foster care data. USDA estimated that in 2017 more than 164,000 individuals were eligible for WIC in Virginia but not participating. The data match conducted during the pilot in 2019 identified more than 114,000 individuals who were adjunctively eligible for WIC but not participating. If Virginia enrolled these individuals in WIC, its WIC caseload would nearly double, reaching nearly 70 percent of the individuals who are eligible but not enrolled and shrinking the coverage gap from 58 percent of WIC-eligible individuals to 18 percent.
Source: Jess Maneely and Zoë Neuberger, “Using Data Matching and Targeted Outreach to Enroll Families With Young Children in WIC – Lessons Learned From State Pilots,” Benefits Data Trust and CBPP, January 5, 2021, www.cbpp.org/wicpilotreport and Kelsey Gray et al., “National and State-Level Estimates of Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) Eligibility and Program Reach in 2017,” U.S. Department of Agriculture, December 2019, https://fns-prod.azureedge.net/sites/default/files/resource-files/WICEligibles2017-Volume1.pdf.
Key Considerations When Developing a Data-Sharing Agreement
Securely Sharing Data Across Programs for the Purpose of WIC Outreach Is Allowable
SNAP
SNAP applicant and participant data may be disclosed for purposes of administration of other federal assistance programs and federally assisted state programs providing assistance on a means-tested basis.a
Medicaid
Medicaid applicant and participant data may be disclosed for purposes directly connected with administration of the Medicaid state planb and disclosure of protected health information by a Medicaid program is allowable where authorized by statute.c Federal law requires Medicaid state plans to include coordination with and referral to the state’s WIC program.d
a 7 USC § 2020(e)(8); 7 CFR § 272.1(c)(1).
b 42 USC § 1396a(a)(7)(A); 42 CFR § 431.300 et seq.
c 45 CFR § 164.512(k)(6)(i).
d 42 USC § 1396a(a)(11)(c); § 1396a(a)(53); 42 CFR § 441.61(c); 42 CFR § 431.635.
Sharing data from Medicaid, SNAP, and other programs that confer adjunctive eligibility with WIC enables targeted WIC outreach and streamlined enrollment, and extends the health and developmental benefits associated with participating in WIC to more families. Several states have demonstrated that this type of data sharing can be conducted securely, protecting families’ privacy while improving their access to essential benefits and services. Thinking through in advance how shared data will be used, as well as how the impact of those uses will be evaluated, will help states craft strong, secure, and flexible data-sharing agreements. This section describes some specific considerations that states may wish to consider as they develop data-sharing agreements.[20]
Which Data Sources Will Be Used?
When determining data sources, one key consideration is how the eligibility guidelines for another benefit aligns with WIC. Several means-tested programs confer adjunctive eligibility for WIC, making these programs excellent data sources for WIC outreach. Another key factor in identifying data sources is the structure of the data from the source program. For example, Medicaid is an individual benefit whereas SNAP is a household benefit. These different structures will matter when matching and using the data.
How Can Data Be Shared Securely?
Data security is an important consideration when sharing data. There are several methods available for securely transferring files and encrypting or de-identifying datasets while enabling targeted outreach. Consulting legal or compliance professionals, as well as data experts, can help ensure a data sharing agreement is both fully legally compliant and protects participants’ privacy.
How Often Will Data Be Shared?
Data used for outreach needs to be “fresh.” If the data is too dated, it may no longer be accurate: a family might have moved, changed phone numbers, or become ineligible. This is one reason it is important to determine how often data will be shared between programs at the onset of the project. When drafting a data-sharing agreement, allowing for more frequent transfers (such as weekly) could be helpful, even if transfers at that frequency will not always be needed.
Data Elements to Be Shared Securely for Targeting WIC Outreach and Evaluating Outcomesa
- First & last name
- Date of birth of mother
- Date of birth of child
- Primary phone number
- Cell phone number
- Preferred language
- Address, including FIPSb and ZIP codes
- Email address
- Race of mother
- Ethnicity of mother
- Race of child
- Ethnicity of child
- Sex of child
- Medicaid program identifier
- SNAP program identifier
- Other program identifier
- Unique household identifier
a This list is not exhaustive.
b Federal Information Processing Standards, which are designed to make data more consistent across various data systems.
What Data Elements Will Be Shared?
Key considerations when drafting an effective and compliant data-sharing agreement are which information needs to be exchanged (such as name, phone number, address, race, age, language, etc.) and how the data will be shared securely. For these reasons, it is beneficial to draft agreements with the full scope of the initiative in mind — from identifying eligible households, to conducting outreach, to completing an evaluation of the initiative’s outcomes — to ensure that all necessary data fields are included in the data-sharing agreement. For example, if an outreach initiative would be more effective in a family’s preferred language, it is important to include this information in the agreement and matching process. If it would be helpful to evaluate an intervention’s effectiveness by any key demographics, such as age, geographic location, ethnicity, or race, it is important to incorporate these elements into the agreement and match. Deciding project logistics and evaluation plans such as these upfront and using the plan to draft agreements can help reduce the likelihood that agreements will need to be amended.
We learned this lesson by trial and error in our pilot. In one state, our original data-sharing agreement provided local WIC agencies with phone numbers for calling to schedule appointments. When local agency staff were being trained before implementation, we realized that not having the name of the individual they would be calling would be a hinderance. The data-sharing agreement had to be amended to allow local WIC agencies to receive names before calling to schedule appointments. From this experience and others, we have learned that bringing the individuals who will perform key processes into the project early on can help ensure that the data-sharing agreement is tailored to outreach plans.
How Can States Avoid Reaching Out to Families Already Enrolled in WIC?
After receiving data from another program, the first step to avoid conducting outreach to families already enrolled in WIC is the initial data match. This match is important because receiving outreach could be bothersome and confusing to families if they are already participating in WIC. States might need to experiment with matching criteria to ascertain which data elements work well in a matching algorithm, address common inconsistencies (such as spelling variations in names or transposed numbers in a birthday), and strike the right balance between inadvertently contacting individuals who are already enrolled in WIC and incorrectly removing someone from the outreach list who is not.[21]
If the initial match is conducted too far in advance of outreach, some families may be on the outreach list that have enrolled in WIC on their own since the original match. These families could be removed from the list through a list “cleaning” process.
What If a State’s WIC Program Is Administered by a Different Agency Than Medicaid or SNAP?
Agency configurations vary across states, and it is common for means-tested programs to be administered by multiple agencies. In most cases, WIC is administered by a different agency than the one that administers Medicaid or SNAP. This can lengthen the process of obtaining necessary approvals from state legal and compliance oversight authorities. Despite these challenges, each pilot state and several other state WIC agencies have successfully executed memorandums of understanding and data-sharing agreements. When conducting legal reviews, compliance overseers have consistently found sharing data and using the results of data matching for targeted WIC outreach to be permitted under existing program regulations.
How Can States Incorporate Data Sharing Into Ongoing Operations?
Once a data-sharing agreement is in place, a regular process for exchanging data and conducting text-based outreach can be incorporated into agencies’ routine activities. Establishing this business process could be helpful to slow or reverse the decline in WIC coverage by bringing in a steady stream of new or returning families.
Massachusetts and Montana have decided to continue data matching and targeted text outreach after their pilot projects ended, and both elected to include data from additional programs, demonstrating that data matching and text-based outreach can be employed in ongoing operations.[22] These strategies can be built upon and adapted according to agency infrastructure and needs. States that have operationalized this practice report that once processes are implemented and incorporated into existing agency procedures, they are cost-effective and relatively easy to administer.
| How Can A State Get Started?[23] | |
|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
End Notes
[1] For more information on how WIC operates, see CBPP, “Policy Basics: Special Supplemental Nutrition Program for Women, Infants, and Children,” updated April 26, 2017, https://www.cbpp.org/cms/index.cfm?fa=view&id=5268.
[2] While all income-eligible individuals also must be at nutritional risk to qualify for WIC, income-eligible families generally meet one of the nutritional risk criteria. For more details about the adjunctive eligibility rules, see 7. C.F.R. § 246.7 (d)(2)(vi).
[3] See Kelsey Gray et al., “National and State-Level Estimates of Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) Eligibility and Program Reach in 2017,” U.S. Department of Agriculture, December 2019, https://fns-prod.azureedge.net/sites/default/files/resource-files/WICEligibles2017-Volume1.pdf.
[4] A comparison of WIC participation to Medicaid and SNAP participation during 2020 will be included in a forthcoming CBPP report by Lauren Hall and Zoë Neuberger.
[5] See Roch A. Nianogo et al., “Economic evaluation of California prenatal participation in the Special Supplemental Nutrition Program for Women, Infants and Children (WIC) to prevent preterm birth,” Preventative Medicine, Vol. 124, July 2019, https://www.sciencedirect.com/science/article/abs/pii/S0091743519301355?via%3Dihub.
[6] For more information about the research evidence on WIC’s effectiveness, see Steven Carlson and Zoë Neuberger, “WIC Works: Addressing the Nutrition and Health Needs of Low-Income Families for More Than Four Decades,” CBPP, updated January 27, 2021, www.cbpp.org/wicworks.
[7] The most disadvantaged parents include, in various studies, those who are Black, very young, or enter prenatal care relatively late or not at all.
[8] Centers for Disease Control and Prevention, “Racial and Ethnic Disparities Continue in Pregnancy-Related Deaths,” September 5, 2019, https://www.cdc.gov/media/releases/2019/p0905-racial-ethnic-disparities-pregnancy-deaths.html.
[9] See Brynne Keith-Jennings, Catlin Nchako, and Joseph Llobrera, “Food Hardship Rose Steeply in Pandemic and Remains High, Especially Amongst Children and Households of Color,” CBPP, forthcoming.
[10] See Steven Carlson, Brynne Keith-Jennings, and Joseph Llobrera, “Policy Brief: More Adequate SNAP Benefits Would Help Millions of Participants Better Afford Food,” CBPP, July 30, 2019, https://www.cbpp.org/research/food-assistance/more-adequate-snap-benefits-would-help-millions-of-participants-better-0; and Brynne Keith-Jennings Joseph Llobrera, and Stacy Dean, “Links of the Supplemental Nutrition Assistance Program With Food Insecurity, Poverty, and Health: Evidence and Potential,” American Journal of Public Health, December 2019, https://ajph.aphapublications.org/doi/full/10.2105/AJPH.2019.305325.
[11] See Carlson and Neuberger, op. cit.
[12] See CBPP, “For Nearly 1 in 9 Adults with Children, Household Lacked Sufficient Food in Last 7 Days, https://www.cbpp.org/for-1-in-9-adults-with-children-household-lacked-sufficient-food-in-last-7-days; and CBPP, “Tracking the COVID-19 Recession’s Effects on Food, Housing, and Employment Hardships,” updated April 22, 2021, https://www.cbpp.org/research/poverty-and-inequality/tracking-the-covid-19-recessions-effects-on-food-housing-and.
[13] CBPP analysis of Census Bureau Household Pulse Survey microdata for March 17-29, 2021.
[14] The details of these pilot interventions and results are explained in Jess Maneely and Zoë Neuberger, “Using Data Matching and Targeted Outreach to Enroll Families With Young Children in WIC,” CBPP, January 5, 2021, www.cbpp.org/wicpilotreport. CBPP and BDT subsequently conducted a workshop series for seven additional states that developed workplans to launch or expand data matching and targeted text-based outreach.
[15] See House of Representatives, Agriculture, Rural Development, Food and Drug Administration, and Related Agencies Appropriations Bill, 2021, Report 116 446, July 13, 2020, p. 73, https://www.congress.gov/116/crpt/hrpt446/CRPT-116hrpt446.pdf.
[16] Data-sharing agreements are discussed in the next section.
[17] See Kelsey Gray et al., op. cit.
[18] See Maneely and Neuberger, op. cit., Figures 2-5.
[19] Families participating in Medicaid in Massachusetts were 36 percent more likely to enroll in WIC as a result of the pilot, but this pilot’s control group may not represent a reliable baseline. See Maneely and Neuberger, op. cit., Table 3 and Note 17.
[20] Data-sharing agreements are sometimes abbreviated as DSAs and are sometimes referred to as Data Use Agreements or DUAs.
[21] In the context of conducting data matching to automatically enroll children in households receiving SNAP benefits for free school meals, a decade of concerted effort and investment have yielded marked improvements in data matching. Nationwide, the share of students who are successfully automatically enrolled has increased from 68 percent to 92 percent. See USDA, Food and Nutrition Service, “Direct Certification in the National School Lunch Program: State Implementation Progress Report to Congress - School Year 2015-2016 & School Year 2016-2017,” October 2018, Figure 1, https://fns-prod.azureedge.net/sites/default/files/resource-files/NSLPDirectCertification2016.pdf.
[22] Colorado and Virginia do not have texting capacity. BDT conducted the texting for their pilots; these states have not yet developed the capacity to conduct texting on an ongoing basis.
[23] In the fall of 2021, CBPP and BDT will publish a toolkit with resources to assist state WIC agencies interested in exploring cross-program data matching for targeted WIC outreach.