Policy Brief: Modernizing SNAP Benefits Would Help Millions Better Afford Healthy Food
End Notes
[1] For more on SNAP benefit adequacy and the Thrifty Food Plan, see Steven Carlson, Joseph Llobrera, and Brynne Keith-Jennings, “More Adequate SNAP Benefits Would Help Millions of Participants Better Afford Food,” CBPP, updated July 15, 2021, https://www.cbpp.org/research/food-assistance/more-adequate-snap-benefits-would-help-millions-of-participants-better.
[2] Andrea Carlson et al., “Thrifty Food Plan, 2006,” Center for Nutrition Policy and Promotion, USDA, April 2007, https://fns-prod.azureedge.net/sites/default/files/usda_food_plans_cost_of_food/TFP2006Report.pdf.
[3] Maeve Gearing, Sujata Dixit-Joshi, and Laurie May, “Barriers That Constrain the Adequacy of Supplemental Nutrition Assistance Program (SNAP) Allotments: Survey Findings,” USDA, Food and Nutrition Service, June 2021, https://www.fns.usda.gov/snap/barriers-constrain-adequacy-snap-allotments.
[4] James P. Ziliak, “Modernizing SNAP Benefits,” Hamilton Project, Brookings Institution, May 2016, http://www.hamiltonproject.org/assets/files/ziliak_modernizing_snap_benefits.pdf.
[5] These estimates were calculated for the 1999 TFP; estimates for the 2006 TFP have yet to be calculated, in large part because USDA did not develop comparable recipes for the last update. See Diego Rose, “Food Stamps, the Thrifty Food Plan, and Meal Preparation: The Importance of the Time Dimension for US Nutrition Policy,” Journal of Nutrition Education and Behavior, 39(4): 226–232, 2007, https://www.sciencedirect.com/science/article/pii/S1499404607004708; George Davis and Wen You, “Not enough money or not enough time to satisfy the Thrifty Food Plan? A cost difference approach for estimating a money-time threshold,” Food Policy, 36(2):101-107, 2011, https://www.sciencedirect.com/science/article/pii/S0306919210000941.
[6] Karen Hamrick and Ket McClelland, “Americans’ Eating Patterns and Time Spent on Food: The 2014 Eating & Health Module Data,” USDA Economic Research Service, July 2016, https://www.ers.usda.gov/publications/pub-details/?pubid=80503; and Christian Raschke, “Food stamps and the time cost of food preparation,” Review of Economics of the Household, 10(2): 259-275, 2012, https://link.springer.com/article/10.1007/s11150-011-9128-3. SNAP participants, on average, also spend 55 minutes grocery stopping once every seven days. The authors do not discuss reasons why SNAP participants spend more time preparing food. One potential factor may be that a greater share of food purchases among SNAP participants are for foods to be prepared at home, which require more time preparing. For example, a 2017 study found that 74 percent of SNAP households’ food purchasing is for food-at-home spending, compared to 65 percent for eligible non-participant households and 62 percent for all U.S. households. Laura Tiehen, Constance Newman, and John Kirlin, “The Food-Spending Patterns of Households Participating in the Supplemental Nutrition Assistance Program: Findings From USDA’s FoodAPS,” USDA Economic Research Service, August 2017, https://www.ers.usda.gov/webdocs/publications/84780/eib-176.pdf?v=42962.
[7] Ziliak, op. cit.
[8] Angela M. Babb et al., “An examination of medically necessary diets within the framework of the Thrifty Food Plan,” Ecology of Food and Nutrition, 58(3): 236-246, 2019, https://doi.org/10.1080/03670244.2019.1598978.
[9] The 2006 TFP market baskets did not meet the recommendations for vitamin E and potassium for some age-gender groups and did not meet the recommendations for sodium for most age-gender groups. See “Thrifty Food Plan, 2006,” Center for Nutrition Policy and Promotion, USDA, April 2007, https://www.fns.usda.gov/thrifty-food-plan-2006-report.
[10] According to the most recent USDA data, 28 percent of households redeem at least 90 percent of their benefits within seven days of issuance; 53 percent redeem at least 90 percent within 14 days. See Laura Castner et al., “Benefit Redemption Patterns in the Supplemental Nutrition Assistance Program in Fiscal Year 2017,” Insight Policy Research, September 2020, https://www.fns.usda.gov/snap/benefit-redemption-patterns-snap-fy-2017#:~:text=On%20average%2C%20SNAP%20households%20had,before%20receiving%20their%20next%20issuance. The cyclical pattern may vary considerably across SNAP households. One study attributes the benefit cycle to a minority (39 percent) of SNAP households that spend two-thirds of their monthly benefits within the first four days. The larger remaining group of SNAP participants, in contrast, spend only one-sixth early in the month. See Jeffrey Dorfman et al., “Re-examining the SNAP benefit cycle allowing for heterogeneity,” Applied Economic Perspectives and Policy, 41(3): 404-433, 2019, https://onlinelibrary.wiley.com/doi/10.1093/aepp/ppy013. Another study found a cyclical pattern of weekly food spending in a sample of low-income households in Minneapolis-St. Paul shortly after they enrolled in a nutrition assistance program modeled after SNAP but not before. See Sruthi Valluri et al., “Trends in cyclical food expenditures among low-income households receiving monthly nutrition assistance: results from a prospective study,” Public Health Nutrition, 24(3): 1-8, 2020, https://www.cambridge.org/core/journals/public-health-nutrition/article/abs/trends-in-cyclical-food-expenditures-among-lowincome-households-receiving-monthly-nutrition-assistance-results-from-a-prospective-study/517FA05377A2A86C4612A5BA5A961A96.
[11] In one of the earliest studies on this issue, participants who do their major grocery shopping infrequently (about 40 percent of households receiving food stamps) consumed fewer calories four weeks after receiving benefits than in each of the first three weeks. Another study from the same period estimates that consumption (again measured by calorie intake) fell by roughly 9 to 12 percent over the course of a month. Parke Wilde and Christine Ranney, “The monthly Food Stamp cycle: shopping frequency and food intake decisions in an endogenous switching regression framework,” American Journal of Agricultural Economics, 82(1): 200–213, 2000, https://onlinelibrary.wiley.com/doi/abs/10.1111/0002-9092.00016. Wilde and Ranney found that 42 percent of households receiving food stamps conducted a major grocery shopping trip once per month or less frequently. These households were more likely than other low-income households to be infrequent shoppers due to transportation difficulties, time constraints, or stigma associated with food stamps. Jesse Shapiro, “Is there a Daily Discount Rate? Evidence from the Food Stamp Nutrition Cycle,” Journal of Public Economics, 89(2-3): 303-325, 2005, http://www.brown.edu/Research/Shapiro/pdfs/highfreq111703.pdf. More recent studies affirm these results. Adults participating in SNAP consume about 38 percent fewer calories per day in the last two days of the month than in the rest of the month, and about 25 percent less relative to their estimated energy requirement. Jessica Todd, “Revisiting the Supplemental Nutrition Assistance Program cycle of food intake: Investigating heterogeneity, diet quality, and a large boost in benefit amounts,” Applied Economic Perspectives and Policy, 37(3): 437-458, 2015, https://academic.oup.com/aepp/article-abstract/37/3/437/8261.
[12] Karen Hamrick and Margaret Andrews, “SNAP participants’ eating patterns over the benefit month: a time use perspective,” PloS One, 11(7): e0158422, 2016, http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0158422; Todd, op. cit.
[13] One study found that a SNAP household is 11 percentage points likelier to be classified as food insecure near the end of or at the beginning of the benefit month than in the rest of the month. Christian Gregory and Travis Smith, “Salience, food security, and SNAP receipt,” Journal of Policy Analysis and Management, 38(1): 124-154, 2019, https://onlinelibrary.wiley.com/doi/epdf/10.1002/pam.22093. Gregory and Smith’s finding that SNAP households have a higher propensity to report food hardships at the end of the benefit month is consistent with the existing literature on the benefit cycle, but they also found that the propensity to report food hardships was higher at the beginning of the month as well. They suggest that recent experiences of hardships at the end of the month may still be fresh in recipients’ minds even after they have received benefits, or that SNAP households may feel they need to justify receiving SNAP benefits.
[14] Anne Byrne and David Just, “The other half: an examination of monthly food pantry cycles in the context of SNAP benefits,” Applied Economic Perspectives and Policy, January 2021, https://onlinelibrary.wiley.com/doi/abs/10.1002/aepp.13150; and Linlin Fan et al., “The use of charitable food assistance among low‐income households in the United States,” Journal of the Academy of Nutrition and Dietetics, 121(1): 27–35, 2020, https://jandonline.org/article/S2212-2672(20)30995-3/fulltext.
[15] Hilary Seligman et al., “Exhaustion of food budgets at month’s end and hospital admissions for hypoglycemia,” Health Affairs, 33(1): 116-123, 2014, https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2013.0096; and Sanjay Basu, Seth Berkowitz, and Hilary Seligman, “The monthly cycle of hypoglycemia: an observational claims-based study of emergency room visits, hospital admissions, and costs in a commercially insured population,” Medical Care, 55(7): 639-645, 2017, https://journals.lww.com/lww-medicalcare/fulltext/2017/07000/The_Monthly_Cycle_of_Hypoglycemia__An.1.aspx. Neither study accounts for differences between the calendar month and the SNAP issuance cycle (most states stagger issuance of SNAP benefits over several days of each month), so it is difficult to attribute the results solely to the timing of SNAP benefits; other factors — such as receipt of monthly paychecks — may also be at work.
[16] Anna Gassman-Pines and Laura Bellows, “Food instability and academic achievement: a quasi-experiment using SNAP benefit timing,” American Educational Research Journal, 55(5): 897-927, 2018, http://journals.sagepub.com/doi/10.3102/0002831218761337; Chad Cotti, John Gordanier, and Orgill Ozturk, “When does it count? The timing of food stamp receipt and educational performance,” Economics of Education Review, 66: 40-50, 2018, https://www.sciencedirect.com/science/article/abs/pii/S0272775718303649; Lisa Gennetian et al., “Supplemental Nutrition Assistance Program (SNAP) benefit cycles and student disciplinary infractions,” Social Service Review, 90(3): 403-33, 2016, https://www.journals.uchicago.edu/doi/abs/10.1086/688074; and Timothy Bond et al., “Hungry for Success? SNAP Timing, High-Stakes Exam Performance, and College Attendance,” National Bureau of Economic Research, January 2021, https://www.nber.org/papers/w28386.
[17] Elaine Waxman, Craig Gundersen, and Megan Thompson, “How Far Do SNAP Benefits Fall Short of Covering the Cost of a Meal?” Urban Institute, February 2018, https://www.urban.org/sites/default/files/publication/96661/how_far_do_snap_benefits_fall_short_of_covering_the_cost_of_a_meal_2.pdf.
[18] Mark Nord and Mark Prell, “Food Security Improved Following the 2009 ARRA Increase in SNAP Benefits,” USDA Economic Research Service, April 2011, https://www.ers.usda.gov/webdocs/publications/44837/7469_err116.pdf?v=7982.4.
[19] Mark Nord, “Effects of the decline in the real value of SNAP benefits from 2009 to 2011,” USDA Economic Research Service, August 2013, https://www.ers.usda.gov/publications/pub-details/?pubid=45102; Bhagyashree Katare and Jiyoon Kim, “Effects of the 2013 SNAP benefit cut on food security,” Applied Economic Perspectives and Policy, 39(4): 662–681, 2017, https://onlinelibrary.wiley.com/doi/10.1093/aepp/ppx025.
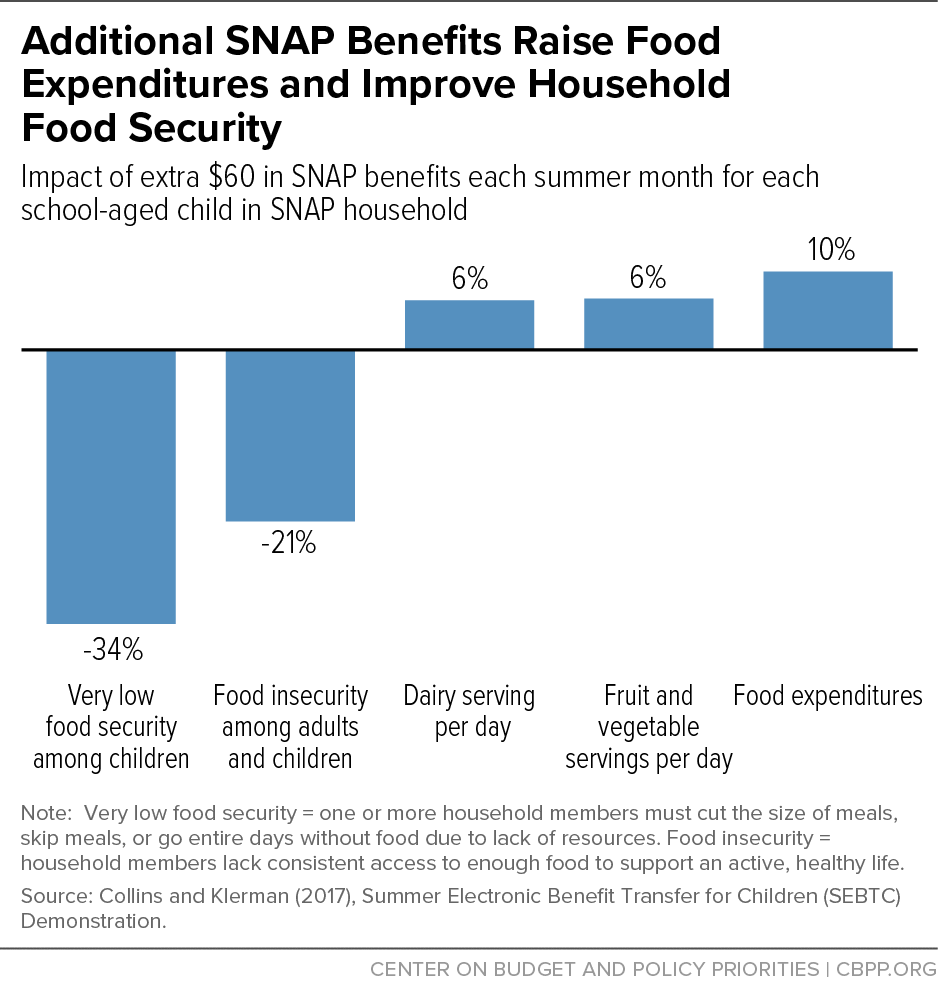
[20] Ann Collins and Jacob Klerman, “Improving nutrition by increasing Supplemental Nutrition Assistance Program benefits,” American Journal of Preventive Medicine, 52(2S2): S179-S185, 2017, https://www.sciencedirect.com/science/article/pii/S0749379716303890.
[21] Lauren Bauer et al., “The Effect of Pandemic EBT on Measures of Food Hardship,” Hamilton Project, July 2020, https://www.hamiltonproject.org/assets/files/P-EBT_LO_7.30.pdf. The American Rescue Plan of 2021 ensures that states can provide P-EBT benefits for the full duration of the public health emergency, including during the summer.
[22] National Academies of Sciences, Engineering, and Medicine, “A Roadmap to Reducing Child Poverty,” Washington, D.C.: The National Academies Press, February 2019, https://www.nap.edu/catalog/25246/a-roadmap-to-reducing-child-poverty.
[23] Taryn Morrissey and Daniel Miller, “Supplemental Nutrition Assistance Program participation improves children’s health care use: an analysis of the American Recovery and Reinvestment Act’s natural experiment,” Academic Pediatrics, 20(6): 863-870, 2020, https://www.sciencedirect.com/science/article/abs/pii/S1876285919304619; and Katelin Hudak and Elizabeth Racine, “Do additional SNAP benefits matter for child weight? Evidence from the 2009 benefit increase,” Economics & Human Biology, 41: 100966, 2020, https://www.sciencedirect.com/science/article/pii/S1570677X20302367.
[24] This study uses data that predate the Affordable Care Act’s Medicaid expansion for adults. The health-related findings are also not driven by children lacking health insurance, as children in households participating in SNAP are likely eligible for Medicaid or the Children’s Health Insurance Program, and the authors found no relationship between SNAP purchasing power and the likelihood a child has no insurance. The authors hypothesize that parental stress and bandwidth may explain the relationship between SNAP and child check-ups, but cannot directly test this in the study. Erin Bronchetti, Garret Christensen, and Hilary Hoynes, “Local food prices, SNAP purchasing power, and child health,” Journal of Health Economics, 68: 102231, 2019, https://www.sciencedirect.com/science/article/abs/pii/S0167629619304151.
[25] For example, poverty rates were twice as high for Black (18.8 percent) and Hispanic people (15.7 percent) as non-Hispanic white people (7.3 percent) in 2019; the poverty rate among Asian Americans and Pacific Islanders (10.2 percent) was 40 percent higher. Jessica Semega et al., “Income and Poverty in the United States: 2019,” U.S. Census Bureau, September 2020, https://www.census.gov/library/publications/2020/demo/p60-270.html. Non-Hispanic Black households were more than twice as likely — and Hispanic households twice as likely — to be food insecure in 2019 (19.1 percent and 15.6 percent, respectively) as non-Hispanic white households (7.9 percent). Very low food security among children, while rare, is five times more likely among non-Hispanic Black households than among non-Hispanic white households (1.7 vs 0.3 percent). Alisha Coleman-Jensen et al., “Household Food Security in the United States in 2019,” USDA Economic Research Service, September 2020, https://www.ers.usda.gov/publications/pub-details/?pubid=99281.
[26] Hayden Stewart, Diansheng Dong, and Andrea Carlson, “Why Are Americans Consuming Less Fluid Milk? A Look at Generational Differences in Intake Frequency,” USDA Economic Research Service, May 2013, https://ageconsearch.umn.edu/record/262223/; and Carlson et al., op. cit.
[27] Andrea Wiley, Re-imagining Milk: Cultural and Biological Perspectives, London and New York: Routledge, 2015 as cited in Angela Babb, “America’s ‘Thrifty Food Plan’: hunger, mathematics, and the valuation of nutrition assistance,” Annals of the American Association of Geographers, 110(4): 983-1004, 2020, https://www.tandfonline.com/doi/abs/10.1080/24694452.2019.1664889.