- Home
- Special Supplemental Nutrition Program F...
Policy Basics: Special Supplemental Nutrition Program for Women, Infants, and Children
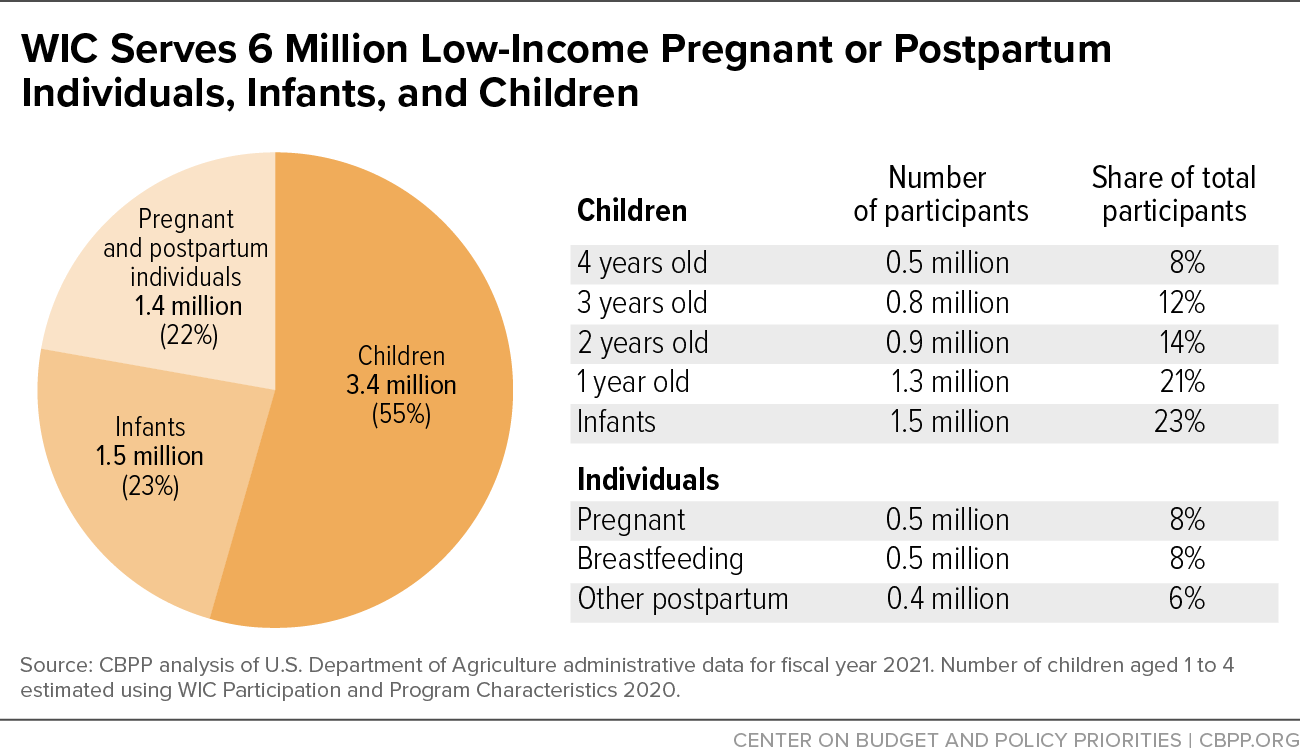
The Special Supplemental Nutrition Program for Women, Infants, and Children, popularly known as WIC, provides nutritious foods, counseling on healthy eating, breastfeeding support, and health care referrals to approximately 6 million low-income pregnant, postpartum, and breastfeeding individuals, infants, and children at nutritional risk — and leads to long-term benefits.
During the COVID-19 pandemic, operational changes have been made to WIC. Unless we indicate otherwise, this Policy Basics describes how WIC operates independent of the changes during the pandemic. The section “WIC Administration During the COVID-19 Pandemic” describes some of the key COVID-19 related changes.
Why Is WIC Important?
Infants and very young children can face lifelong cognitive and health consequences if they don’t get adequate nourishment. WIC aims to ensure that pregnant individuals get the foods they need to deliver healthy babies and that those babies are well-nourished as they grow into young children.
WIC participation contributes to healthier births, more nutritious diets, improved infant feeding practices, better health care for children, and higher academic achievement for students.
Extensive research over the last few decades shows that WIC works. WIC participation contributes to healthier births, more nutritious diets, improved infant feeding practices, better health care for children, and higher academic achievement for students.
How Is WIC Funded?
WIC is federally funded through the annual appropriations process; states are not required to contribute funds. Since 1997, Congress — on a bipartisan basis — has provided sufficient funding each year for WIC to serve all eligible applicants. The program receives approximately $5 billion to $6 billion annually.
Who Is Eligible for WIC?
Pregnant, postpartum, and breastfeeding individuals, infants, and children up to age 5 are eligible if they meet income guidelines and if a health care professional, such as a registered dietitian or nurse, or a trained nutrition paraprofessional, has determined them to be at “nutritional risk.” Generally, applicants who meet the income requirements have a medical or dietary condition that places them at nutritional risk.
All postpartum individuals who meet the income guidelines and nutritional risk criteria are eligible for WIC benefits for up to six months after childbirth; individuals who continue to breastfeed their infants beyond six months are eligible for WIC benefits for up to a year after childbirth. Young children receive WIC benefits for up to a year, after which eligibility must be redetermined.
Applicants who receive no other relevant means-tested benefits must have gross household income at or below 185 percent of the federal poverty level (currently $42,606 annually for a family of three) to qualify for WIC benefits. To simplify program administration, an applicant who already receives Supplemental Nutrition Assistance Program benefits (SNAP, formerly food stamps), Medicaid, or monthly Temporary Assistance for Needy Families cash assistance payments is automatically considered income-eligible for WIC, even if the program’s income limit is above 185 percent of poverty. More than three-quarters (77.2 percent) of people approved for WIC benefits receive one of these other benefits.
How Do Families Apply for WIC?
Pregnant individuals and parents of young children are often referred to WIC by their doctor or when they apply for Medicaid, SNAP, or other community services. They can also apply directly for WIC benefits at one of WIC’s 10,000 local clinics, located in community health centers, Indian Health Services clinics, hospitals, and local health departments. While many applicants contact WIC clinics by telephone to request services, state and local agencies are increasingly making applications or forms to request WIC benefits available online.
Applicants are scheduled for certification appointments to determine eligibility and food benefits, during which they are asked to provide documentation of where they live, their identity, and their income or receipt of other qualifying benefits. They also meet with a professional or paraprofessional for a nutrition assessment to identify nutritional risks. Federal rules require applicants to be present during these appointments, with exceptions for newborn infants, children with working parents, and individuals with health conditions that prevent them from attending in-person appointments. Under federal waivers provided during the pandemic, WIC agencies switched to conducting appointments by telephone or videoconference rather than in person to protect both participants and staff. Participants responded very favorably to remote appointment options, which not only protected their health but also reduced transportation, work schedule, and child care barriers associated with in-person appointments. When allowed under program rules, continuing and expanding practices to make WIC benefits and services easier for families to access and use may improve the reach and impact of the program in the coming years.
How Does WIC Provide Services?
The Department of Agriculture’s (USDA) Food and Nutrition Service oversees WIC at the federal level and provides funds to state health departments, Indian Tribal Organizations, Washington, D.C., and U.S. Territories to provide WIC benefits and administer WIC programs. States, in turn, allocate or use the funds to staff local WIC clinics that provide services and electronic benefit cards to purchase nutritious foods to participants. The services that local WIC clinics provide include individual nutrition counseling, nutrition classes, breastfeeding support, smoking cessation support, and referrals for health care and social services.
WIC provides specific foods chosen through a rigorous science-based process because they tend to be lacking in the diets of low-income women and young children.
What Foods Does WIC Provide?
WIC is not meant to provide the full array of foods that a pregnant individual or a young child needs. Instead, it provides specific types of foods chosen through a rigorous science-based process because they tend to be lacking in the diets of low-income women and young children. The program provides a limited number of foods — such as whole grain bread, baby food, infant formula, and milk — as well as separate “cash value benefits” that can be used only to buy fruits and vegetables. During 2021, the cash value benefit amount was increased to provide participants with additional fruits and vegetables, as described in the “WIC Administration During the COVID-19 Pandemic” section below, and USDA will have an opportunity to permanently increase the fruit and vegetable benefit when updating the rules for WIC food packages.
USDA revised the WIC food package in 2009 based on recommendations from the Institute of Medicine. The National Academies of Sciences, Engineering and Medicine completed another review of WIC foods in 2017 and recommended updates, including higher amounts for the cash value benefit for fruits and vegetables. In order to modify WIC’s food packages based on the recommendations, the USDA Food and Nutrition Service will go through a formal rulemaking process, with a proposed rule anticipated in 2022.
How Do Participants Receive WIC Foods?
Approximately 47,000 grocery stores nationwide have been approved to redeem WIC food benefits based on their prices and the variety of foods they offer. Participants select their WIC foods from the shelves and use WIC electronic benefit cards to pay at the register. The state WIC program then reimburses the store for the retail value of the WIC foods.
Over the past decade, WIC has transitioned from paper vouchers to electronic benefit cards to provide food benefits. The benefit cards simplify WIC transactions in the checkout line, eliminate the stigma of paying with paper vouchers, and allow for stronger program management and oversight. As of September 2022, participants in 49 states and D.C. and in most WIC programs in Indian Tribal Organizations and the territories receive electronic benefit cards to shop for WIC foods.
The transition to electronic benefit cards facilitates other modernization efforts to make shopping for WIC foods easier by employing options available to all consumers. When offered the opportunity to use self-checkout, curbside pick-up, drive-through windows, and special WIC food sections in stores, participants use these options and report favorable experiences with them. Both participants and grocers are eager for additional ways to make WIC shopping more equitable and convenient. USDA has initiated efforts to shift WIC toward online shopping platforms with grant-funded projects to test and evaluate online ordering, and to establish a congressionally required Task Force on Supplemental Foods Delivery. The Task Force ― composed of a broad range of stakeholders, including WIC providers, retail grocers, electronic benefit transfer processors, and food manufacturers — recommended integrating future online WIC shopping models into existing commercial platforms to ensure that WIC participants can access the same variety of online shopping options as other shoppers without stigma, added difficulty, or personal cost. Efforts to improve and modernize the WIC shopping experience are crucial for enabling participants to fully use their food benefits and maximize the health benefits from participating in WIC.
How Does WIC Support Infant Feeding?
WIC promotes breastfeeding as the optimal feeding choice for infants, unless it is inadvisable for medical reasons, so participants get the health, nutrition, and emotional benefits that research shows breastfeeding provides. WIC supports breastfeeding through education and peer counseling and by providing exclusively breastfeeding individuals with an enhanced food package, longer eligibility, and breast pumps. WIC provides infant formula for infants who are not breastfed.
How Does WIC Obtain Infant Formula?
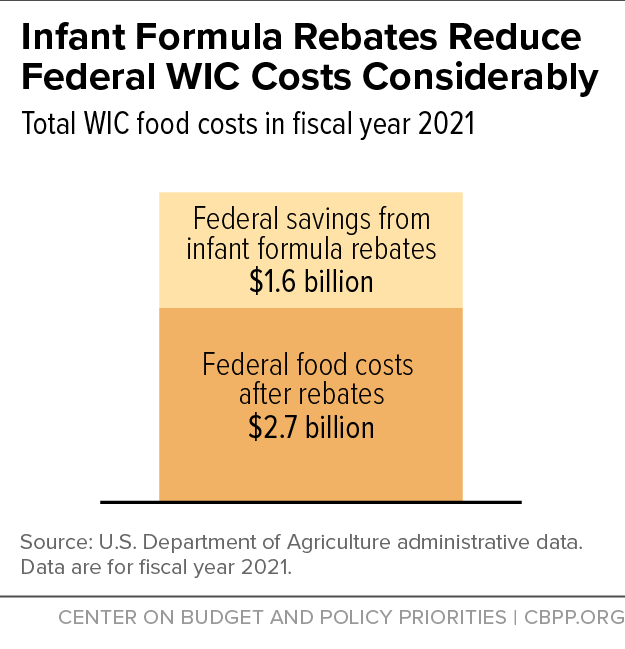
WIC uses a competitive bidding process in which infant formula manufacturers offer discounts, in the form of rebates, to state WIC programs in order to be selected as the sole formula provider to WIC participants in the state, except when families need specialized formula for medical reasons. To help families cope with the 2022 formula shortage precipitated by a safety recall, the federal government has temporarily expanded state flexibility over formula purchases by WIC participants. WIC purchases of infant formula account for more than half of U.S. formula consumption because WIC serves approximately 40 percent of all infants in the country.
This process, adopted through bipartisan legislation in 1989, saves the federal government $1 billion to $2 billion per year. As a result of these savings, WIC’s cost to the government is much lower than the full retail value of WIC benefits for program participants. These savings have played an important role in allowing WIC to serve all eligible applicants with the limited funding the program receives through the annual appropriations process.
How Much Do Households Receive in Food Benefits?
WIC provided an average value of $56.90 in food per participant per month in fiscal year 2021 (excluding the increase in the cash value benefit for fruits and vegetables during the latter portion of the fiscal year, described in the section on “WIC Administration During the COVID-19 Pandemic” below). The average monthly cost to the federal government, however, was much lower — $35.56 per participant — due to the infant formula discounts discussed above. Because many infants receive infant formula, which is the most expensive item WIC provides, the average monthly value of the WIC benefit for infants was over $130, while the average monthly value for pregnant and postpartum individuals and children was less than $40.
WIC Administration During the COVID-19 Pandemic
During the pandemic, state WIC agencies have had various flexibilities in program administration under federal waivers, including the flexibility to allow families to enroll or re-enroll without having to visit a WIC clinic and to issue benefits remotely. As a result, phone and video appointments for certification, nutrition counseling, and breastfeeding services have been routinely offered in lieu of in-person appointments.
WIC agencies have also set up various methods for applicants or participants to submit documents or photos of documents electronically, including email, text message, participant portals, document uploading tools, and WIC mobile apps. These document transmittal methods were permitted under program rules prior to the pandemic and will remain allowable once COVID-19 related waivers expire.
When the pandemic started, most states had transitioned from issuing paper food vouchers to issuing benefits electronically on cards in anticipation of an October 1, 2020, deadline; but a few states completed or initiated electronic benefit implementation during the pandemic. Electronic benefits are provided either on cards that allow vendors to access the participant’s allowable foods at the time of the sale (online) or on cards that have that information loaded on a chip (offline). During the pandemic, online cards facilitated adding benefits remotely; offline cards presented a challenge because participants needed to bring their cards to a clinic to have their benefits added.
Outreach and communication during the pandemic were also difficult, and some participants and potential applicants may not have been aware that services were being offered remotely while WIC clinics were closed. In addition, many state and local WIC agencies were impacted when staff were redeployed to pandemic-related duties, eroding their capacity to reach out to applicants and participants about how to access services and benefits remotely.
Despite WIC agency efforts to pivot to remote services during the pandemic, program participation declined in many states. Prior to the pandemic, WIC reached 57 percent of the low-income individuals who qualify nationwide. Overall participation during the pandemic has been lower than in recent years with great variation across states. Some states have experienced increases in participation during the pandemic while participation has declined in a number of states.
The declines in WIC participation are particularly concerning for households of color who have long experienced higher levels of food hardship ― often stemming from structural racism in education, housing, health care, and employment. In addition, pregnant individuals of color face higher risk of severe pregnancy-related health issues such as preeclampsia, and are more likely to have preterm births, low birth weight births, or births with late or no prenatal care ― all of which contribute to higher rates of maternal and infant mortality for families of color. Because WIC participation is associated with reduced risk of premature birth, low birth weight, and infant mortality, increasing the share of eligible families who participate in WIC across the board — and for pregnant people of color and their infants, who face greater health risks — can be part of a broader strategy to improve maternal and child health outcomes overall and mitigate racial and ethnic disparities in such outcomes.
Despite its significant challenges, the pandemic also presented opportunities for lasting program improvements. The American Rescue Plan Act provided WIC with funds to modernize the program, develop innovative service delivery models, and conduct robust outreach. WIC agencies can also apply lessons learned and adopt promising practices implemented during the pandemic to make ongoing improvements in operations.
The Rescue Plan also temporarily increased the amount of the monthly cash value benefit for fruits and vegetables to $35 per participant. Subsequent legislation continued to provide additional benefits for fruits and vegetables. Since October 2021, children receive $24 monthly, pregnant and postpartum individuals receive $43 monthly, and breastfeeding individuals receive $47 monthly. These increases are in effect through September 30, 2022. Early evidence indicates that families are purchasing the higher quantities of fruits and vegetables for their young children. USDA will have an opportunity to permanently increase the fruit and vegetable benefit to these levels, as recommended by the National Academies of Sciences, Engineering and Medicine, when updating the rules for WIC food packages.
Due to these changes and other robust relief efforts, including expanding the Earned Income Tax Credit and Child Tax Credit, expanding SNAP benefits, and getting food assistance to children missing out on school meals through Pandemic EBT (P-EBT), food insecurity did not surge during the pandemic the way it did during the Great Recession. Families with children experienced a temporary increase in food insecurity in 2020 before the rate fell to its lowest point in more than two decades. Expanding WIC participation could play an role in continuing to mitigate food hardship, especially for children in Black and Latino families, who face food insecurity at much higher rates than those in white households.
How Efficient Is WIC?
WIC leverages market forces to contain program costs. While food prices rose by 11 percent between fiscal year 2009 and 2019, WIC food costs fell by 4 percent.
The competitive bidding process used to procure infant formula, described above, leverages market forces to reduce WIC food costs. While overall food prices rose by 11 percent between fiscal year 2009 and 2019, WIC food costs fell by 4 percent. Between 2014 and 2019, food prices rose by 2 percent while WIC food costs fell by 6 percent. (The gap has been even wider in recent years but might reflect Covid-related changes in benefit redemptions.)
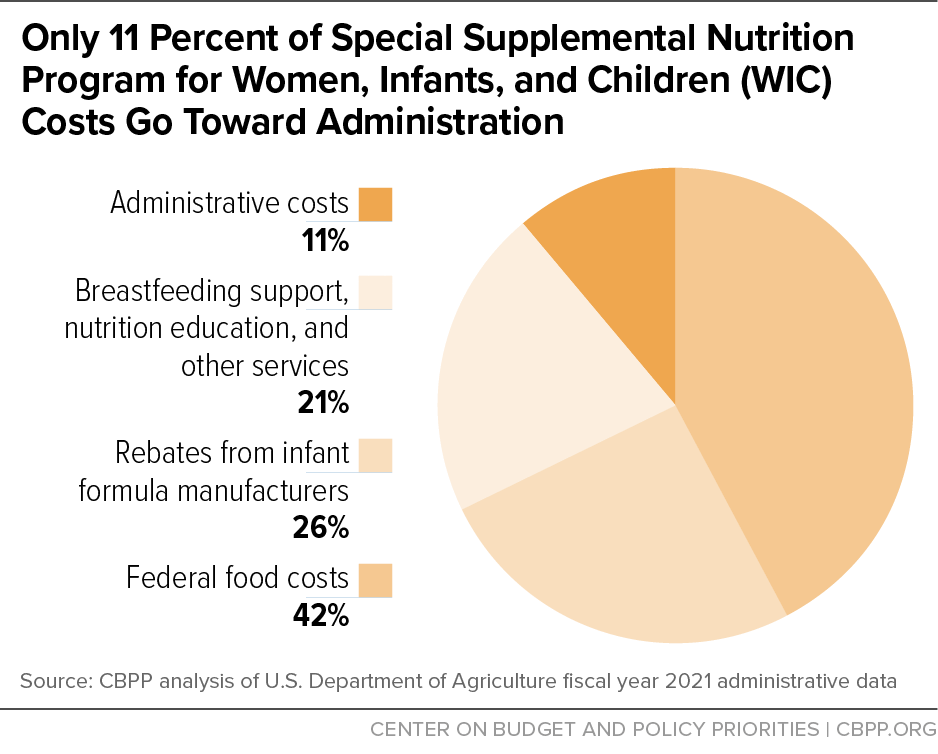
The remainder of WIC funds are devoted to the staff and overhead needed to provide nutrition education, breastfeeding support, and other services — a key part of the program’s success. WIC’s administrative costs have remained at about 6 to 11 percent of total program costs for two decades. By law, WIC funding per participant for nutrition services and administration combined may rise no faster than inflation.
How Effective Is WIC?
Extensive research shows that WIC contributes to positive developmental and health outcomes for low-income pregnant, postpartum, and breastfeeding individuals and young children. In particular, WIC participation is associated with:
- Healthier births. Prenatal WIC participation helps pregnant individuals give birth to healthier infants and helps lower infant mortality rates.
- More nutritious diets. WIC has helped reduce the prevalence of anemia, and strong evidence suggests that WIC participation increases infants’ and children’s intakes of some essential vitamins and minerals and improves infant feeding practices. The 2009 revisions to the WIC food package boosted participants’ purchases and consumption of fruits, vegetables, whole grains, and low-fat dairy products and enhanced the availability of healthy foods in low-income neighborhoods.
- Stronger connections to preventive health care. Children in families with low incomes participating in WIC are just as likely to be immunized as those from better off families, and are more likely to receive preventive medical care than other children in low-income families.
- Improved educational prospects. Children whose mothers participated in WIC while pregnant scored higher on assessments of mental development at age 2 than similar children whose mothers did not participate and have also been found to perform better on reading assessments later in school.
The Center on Budget and Policy Priorities is a nonprofit, nonpartisan research organization and policy institute that conducts research and analysis on a range of government policies and programs. It is supported primarily by foundation grants.