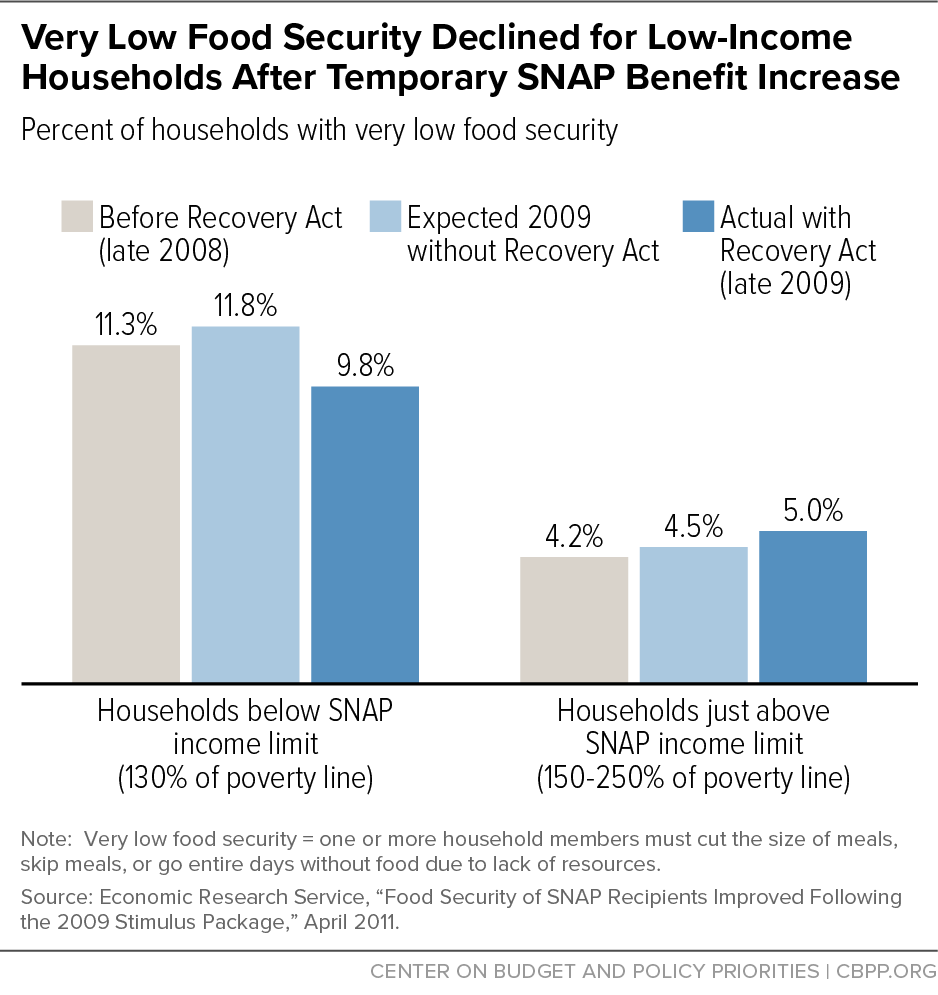More Adequate SNAP Benefits Would Help Millions of Participants Better Afford Food
End Notes
[1] Fiscal year 2019 is the last full year prior to the onset of the COVID-19 pandemic and provides a better measure of the structural adequacy of SNAP benefits than more recent years. Because of temporary increases in SNAP benefits enacted in response to the pandemic, the average benefit in fiscal year 2020 ($1.75) includes emergency SNAP allotments provided under the Families First Coronavirus Response Act.
[2] Dottie Rosenbaum et al., “Food Assistance in American Rescue Plan Act Will Reduce Hardship, Provide Economic Stimulus,” Center on Budget and Policy Priorities, May 7, 2021, https://www.cbpp.org/research/food-assistance/food-assistance-in-american-rescue-plan-act-will-reduce-hardship-provide; CBPP, “Tracking the COVID-19 Recession’s Effects on Food, Housing, and Employment Hardships,” updated July 12, 2021, https://www.cbpp.org/research/poverty-and-inequality/tracking-the-covid-19-recessions-effects-on-food-housing-and; Brynne Keith-Jennings et al., “Number of Families Struggling to Afford Food Rose Steeply in Pandemic and Remains High, Especially Among Children and Households of Color,” Center on Budget and Policy Priorities, April 27, 2021, https://www.cbpp.org/research/food-assistance/number-of-families-struggling-to-afford-food-rose-steeply-in-pandemic-and.
[3] Most of this research was conducted prior to the onset of the COVID-19 pandemic. While the response to the pandemic included significant investments in food assistance programs to mitigate the extraordinarily high levels of hunger and hardship, the relief is temporary and does not address more fundamental shortcomings in the adequacy of SNAP benefits. Thus, the research cited in this paper remains highly relevant and reflects the adequacy of SNAP benefits when temporary nutrition assistance measures end if action isn’t taken to update the Thrifty Food Plan.
[4] Laura Castner et al., “Benefit Redemption Patterns in the Supplemental Nutrition Assistance Program in Fiscal Year 2017,” Insight Policy Research, September 2020, https://www.fns.usda.gov/snap/benefit-redemption-patterns-snap-fy-2017#:~:text=On%20average%2C%20SNAP%20households%20had,before%20receiving%20their%20next%20issuance.
[5] Erin Bronchetti, Garret Christensen, and Benjamin Hansen, “Variation in Food Prices and SNAP Adequacy for Purchasing the Thrifty Food Plan,” University of Kentucky Center for Poverty Research Discussion Paper Series, 2016, https://uknowledge.uky.edu/cgi/viewcontent.cgi?referer=https://scholar.google.com/&httpsredir=1&article=1117&context=ukcpr_papers.
[6] Julie Caswell and Ann Yaktine, eds., Supplemental Nutrition Assistance Program: Examining the Evidence to Define Benefit Adequacy, Institute of Medicine and National Research Council, Washington, D.C.: National Academies Press, 2013, https://fns-prod.azureedge.net/sites/default/files/ops/IOMSNAPAllotments.pdf.
[7] While all these factors are potentially important, we focus this research review on the adequacy of SNAP’s maximum allotments and on the TFP on which those allotments are based, largely because existing research offers evidence on both the adequacy of the TFP and the consequences of increasing SNAP benefits. Other features of the program’s basic design, such as its benefit reduction rate, deductions from gross income, and nutrition education, can also affect adequacy, but less is known about how well these features align with the circumstances of low-income households in the 21st century and the consequences of potential alternatives.
A notable exception is Joshua Leftin et al., “Examination of the Effect of SNAP Benefit and Eligibility Parameters on Low-Income Households,” Decision Demographics and Mathematica Policy Research, October 2017, https://fns-prod.azureedge.net/sites/default/files/ops/SNAPBEP.pdf. It concludes that SNAP deductions generally reflect the actual expenditures of low-income households eligible for those deductions, but many other households have large expenses that current rules do not allow them to claim. For example, while households may deduct out-of-pocket medical expenses exceeding $35 per month for health care for elderly or disabled members, data from the Consumer Expenditure Survey show that low-income households with no elderly or disabled members who report health care expenditures (about 47 percent of such households) incur nearly $225 per month in non-reimbursed medical expenses, on average.
[8] The Food Research and Action Center (FRAC) has also reviewed the research on SNAP benefit adequacy. See “Initiatives to Make SNAP Benefits More Adequate Significantly Improve Food Security, Nutrition, and Health,” February 2019, http://frac.org/wp-content/uploads/snap-initiatives-to-make-snap-benefits-more-adequate.pdf; and “Replacing the Thrifty Food Plan in Order to Provide Adequate Allotments for SNAP Beneficiaries,” December 2012, http://frac.org/wp-content/uploads/thrifty_food_plan_2012.pdf.
[9] The TFP market basket for each age-gender group (such as female adults aged 19-50) consists of food amounts for 29 food categories. The cost of each TFP market basket is adjusted for inflation by applying the consumer price index (CPI) that corresponds to each of the food categories that make up the TFP. For example, the CPI for breakfast cereals is applied to the cost of the TFP food category “whole grain cereals.” The updated costs of the food categories are then added up to arrive at the new cost of the TFP market basket.
[10] While the technical details of the TFP’s mathematical approach have received relatively little scrutiny by outside experts, some critics have proposed simpler theoretical models that are arguably easier to interpret than the USDA formulation. See Parke Wilde and Joseph Llobrera, “Using the Thrifty Food Plan to assess the cost of a nutritious diet,” Journal of Consumer Affairs, 43(2): 274-304, 2009, https://onlinelibrary.wiley.com/doi/pdf/10.1111/j.1745-6606.2009.01140.x; Angela Babb, Daniel Knudsen, and Scott Robeson, “A critique of the objective function utilized in calculating the Thrifty Food Plan,” PloS One, 14(7): e0219895, 2019, https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0219895; and Angela Babb, “America’s ‘Thrifty Food Plan’: Hunger, mathematics, and the valuation of nutrition assistance,” Annals of the American Association of Geographers, 110(4): 983-1004, 2020, https://www.tandfonline.com/doi/abs/10.1080/24694452.2019.1664889.
[11] “HEI Scores for Americans,” Food and Nutrition Service, USDA, January 2019, https://www.fns.usda.gov/hei-scores-americans.
[12] Andrea Carlson et al., “Thrifty Food Plan, 2006,” Center for Nutrition Policy and Promotion, USDA, April 2007, https://fns-prod.azureedge.net/sites/default/files/usda_food_plans_cost_of_food/TFP2006Report.pdf.
[13] Adam Drewnowski and Petra Eichelsdoerfer, “Can low-income Americans afford a healthy diet?” Nutrition Today, 44(6): 246-249, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2847733/; and Wilde and Llobrera, op. cit. While whole milk is largely omitted, lower-fat milk products are overrepresented.
[14] James P. Ziliak, “Modernizing SNAP Benefits,” The Hamilton Project, Brookings Institution, May 2016, http://www.hamiltonproject.org/assets/files/ziliak_modernizing_snap_benefits.pdf.
[15] Maeve Gearing, Sujata Dixit-Joshi, and Laurie May, “Barriers That Constrain the Adequacy of Supplemental Nutrition Assistance Program (SNAP) Allotments: Survey Findings, USDA, Food and Nutrition Service, June 2021, https://www.fns.usda.gov/snap/barriers-constrain-adequacy-snap-allotments.
[16] Households make decisions on what to produce and what to consume within the constraints of their budget and available time. See Gary Becker, “A Theory of the Allocation of Time,” Economic Journal, 75(299): 493-517, 1965, https://www.jstor.org/stable/2228949 for an economic model of household production that formalizes the cost of time.
[17] The average retail price for canned black beans as purchased in a grocery store is lower than the price of dried beans ($0.95 vs $1.40 per pound in 2016), but the average cost of canned beans “as consumed” after discarding the liquid content is double that of dried beans after rehydrating and cooking ($0.56/cup vs $0.24/cup). See USDA Economic Research Service, Fruit and Vegetable Prices, https://www.ers.usda.gov/data-products/fruit-and-vegetable-prices/fruit-and-vegetable-prices/#Vegetables.
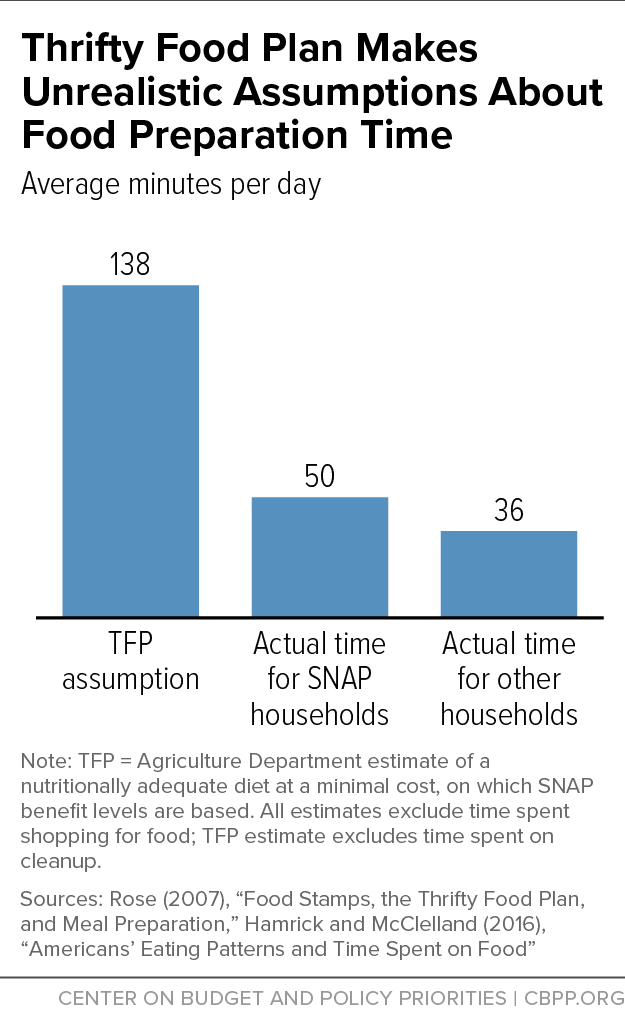
[18] Michelle Ver Ploeg et al., “Access to Affordable and Nutritious Food — Measuring and Understanding Food Deserts and Their Consequences: Report to Congress,” USDA Economic Research Service, June 2009, https://www.ers.usda.gov/publications/pub-details/?pubid=42729; Karen Hamrick et al., “How Much Time Do Americans Spend on Food?” USDA Economic Research Service, November 2011, https://www.ers.usda.gov/publications/pub-details/?pubid=44609.
[19] George Davis and Wen You, “The Time Cost of Food at Home: General and Food Stamp Participant Profiles,” Applied Economics, 42(20): 2537-2552, 2010, https://www.tandfonline.com/doi/abs/10.1080/00036840801964468; George Davis and Wen You, “The Thrifty Food Plan Is Not Thrifty When Labor Cost Is Considered,” Journal of Nutrition, 140(4): 854-857, 2010, https://academic.oup.com/jn/article/140/4/854/4743306; and Christian Raschke, “Food stamps and the time cost of food preparation,” Review of Economics of the Household, 10(2): 259-275, 2012, https://link.springer.com/article/10.1007/s11150-011-9128-3.
[20] Ziliak, op. cit.
[21] These estimates were calculated for the 1999 TFP; estimates for the 2006 TFP have yet to be calculated, in large part because USDA did not develop comparable recipes for the last update. See Diego Rose, “Food Stamps, the Thrifty Food Plan, and Meal Preparation: The Importance of the Time Dimension for US Nutrition Policy,” Journal of Nutrition Education and Behavior, 39(4): 226–232, 2007, https://www.sciencedirect.com/science/article/pii/S1499404607004708; George Davis and Wen You, “Not enough money or not enough time to satisfy the Thrifty Food Plan? A cost difference approach for estimating a money-time threshold,” Food Policy, 36(2):101-107, 2011, https://www.sciencedirect.com/science/article/pii/S0306919210000941.
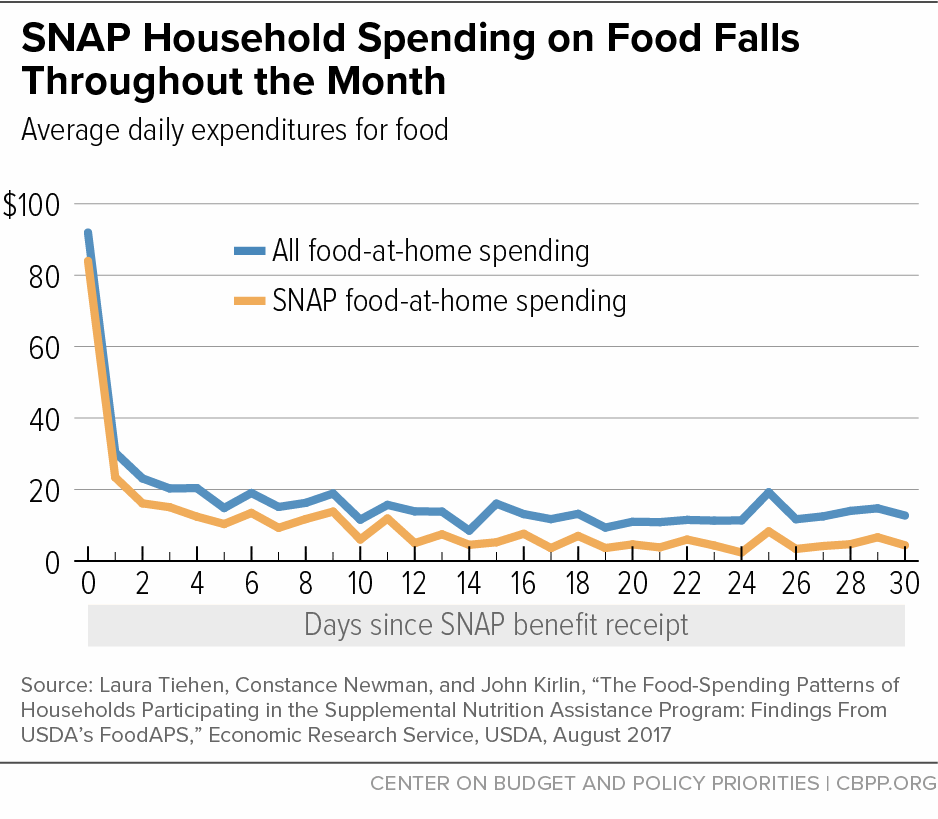
[22] Karen Hamrick and Ket McClelland, “Americans’ Eating Patterns and Time Spent on Food: The 2014 Eating & Health Module Data,” USDA Economic Research Service, July 2016, https://www.ers.usda.gov/publications/pub-details/?pubid=80503; and Raschke, op. cit. SNAP participants, on average, also spend 55 minutes grocery stopping once every seven days. The authors do not discuss reasons why SNAP participants spend more time preparing food. One potential factor may be that a greater share of food purchases among SNAP participants are for foods to be prepared at home, which require more time preparing. For example, a 2017 study found that 74 percent of SNAP households’ food purchasing is for food-at-home spending, compared to 65 percent for eligible non-participant households and 62 percent for all U.S. households. Laura Tiehen, Constance Newman, and John Kirlin, “The Food-Spending Patterns of Households Participating in the Supplemental Nutrition Assistance Program: Findings From USDA’s FoodAPS,” USDA Economic Research Service, August 2017, https://www.ers.usda.gov/webdocs/publications/84780/eib-176.pdf?v=42962.
[23] The 2006 TFP market baskets did not meet the recommendations for vitamin E and potassium for some age-gender groups and did not meet the recommendations for sodium for most age-gender groups. See “Thrifty Food Plan, 2006,” Center for Nutrition Policy and Promotion, USDA, April 2007, https://www.fns.usda.gov/thrifty-food-plan-2006-report.
[24] Ziliak, op. cit.
[25] Angela M. Babb et al., “An examination of medically necessary diets within the framework of the Thrifty Food Plan,” Ecology of Food and Nutrition, 58(3): 236-246, 2019, https://doi.org/10.1080/03670244.2019.1598978.
[26] According to the most recent USDA data, 28 percent of households redeem at least 90 percent of their benefits within 7 days of issuance; 53 percent redeem at least 90 percent within 14 days. See Laura Castner et al., op. cit. The cyclical pattern may vary considerably across SNAP households. One study attributes the benefit cycle to a minority (39 percent) of SNAP households that spend two-thirds of their monthly benefits within the first four days. The larger remaining group of SNAP participants, in contrast, spend only one-sixth early in the month. See Jeffrey Dorfman et al., “Re-examining the SNAP benefit cycle allowing for heterogeneity,” Applied Economic Perspectives and Policy, 41(3): 404-433, 2019, https://onlinelibrary.wiley.com/doi/10.1093/aepp/ppy013. Another study found a cyclical pattern of weekly food spending in a sample of low-income households in Minneapolis-St. Paul shortly after they enrolled in a nutrition assistance program modeled after SNAP but not before. See Sruthi Valluri et al., “Trends in cyclical food expenditures among low-income households receiving monthly nutrition assistance: results from a prospective study,” Public Health Nutrition, 24(3): 1-8, 2020, https://www.cambridge.org/core/journals/public-health-nutrition/article/abs/trends-in-cyclical-food-expenditures-among-lowincome-households-receiving-monthly-nutrition-assistance-results-from-a-prospective-study/517FA05377A2A86C4612A5BA5A961A96.
[27] Carole Trippe and Daisy Ewell, “An Analysis of Cash Food Expenditures of Food Stamp Households,” Memorandum 466 prepared for the USDA Food and Nutrition Service under contract FNS-02-030-TNN / 43-3198-3-3724, August 15, 2007; Tiehen, Newman, and Kirlin, op. cit.
[28] Many states stagger the issuance of SNAP benefits over multiple days at the beginning of the month. As a result, the SNAP “benefit month” does not always coincide with the calendar month. It is important that researchers control for this difference to separate the impacts of the SNAP benefit cycle from the impacts of other monthly cycles (such as the receipt of Social Security, cash assistance payments, or earned income). The strongest studies capture the length of time since the most recent SNAP issuance rather than time since the beginning of the month.
[29] Tiehen, Newman, and Kirlin, op. cit.; Travis Smith et al., “The Effects of Benefit Timing and Income Fungibility on Food Purchasing Decisions Among Supplemental Nutrition Assistance Program Households,” American Journal of Agricultural Economics, 98(2): 564–80, 2016, https://onlinelibrary.wiley.com/doi/10.1093/ajae/aav072; Michael Kuhn, “Causes and Consequences of the Calorie Crunch,” University of Kentucky Center for Poverty Research Discussion Paper Series, DP2016-11, 2016, https://uknowledge.uky.edu/ukcpr_papers/112/. Related research suggests that introducing EBT substantially reduced the expenditure cycle among households with children. Food expenditures for a household with one adult and two children, for example, were $19 higher in the fourth week of the benefit cycle after EBT was implemented; this increase was made possible by a reduction in the large spending spike in the first week. See Michael Kuhn, “Cyclical Food Insecurity and Electronic Benefit Transfer,” unpublished manuscript, April 2018, https://pages.uoregon.edu/mkuhn/pdfs/k_comb.pdf.
[30] Justine S. Hastings and Ebonya L. Washington, “The first of the month effect: consumer behavior and store responses,” American Economic Journal: Economic Policy, 2(2): 142-162, 2010, https://www.aeaweb.org/articles?id=10.1257/pol.2.2.142; and Rebecca Franckle et al., “Supermarket purchases over the Supplemental Nutrition Assistance Program benefit month: a comparison between participants and nonparticipants,” American Journal of Preventive Medicine, 57(6): 800-807, 2019, https://www.sciencedirect.com/science/article/abs/pii/S0749379719303496.
[31] In general, this research deals with prices “generated” by households due to changes in shopping behavior, financial constraints, or quality substitutions. It does not deal directly with changes in prices set by retailers.
[32] Mary Zaki and Jessica Todd, “Price consciousness at the peak of ‘impatience’,” Journal of Human Resources, February 10, 2021, http://jhr.uwpress.org/content/early/2021/02/03/jhr.59.1.0121-11411.abstract.
[33] Purya Valizadeh, Travis Smith, and Michele Ver Ploeg, “Do SNAP households pay different prices throughout the benefit month?” Applied Economic Perspectives and Policy, October 2020, https://onlinelibrary.wiley.com/doi/abs/10.1002/aepp.13094.
[34] Timothy Beatty and Xinzhe Cheng, “Food price variation over the SNAP benefit cycle,” prepared for presentation at the Annual Meeting Agricultural and Applied Economics Association, July 31-August 2, 2016, https://ageconsearch.umn.edu/record/236012/.
[35] Parke Wilde and Christine Ranney, “The monthly Food Stamp cycle: shopping frequency and food intake decisions in an endogenous switching regression framework,” American Journal of Agricultural Economics, 82(1): 200–213, 2000, https://onlinelibrary.wiley.com/doi/abs/10.1111/0002-9092.00016. Wilde and Ranney found that 42 percent of households receiving food stamps conducted a major grocery shopping trip once per month or less frequently. These households were more likely than other low-income households to be infrequent shoppers due to transportation difficulties, time constraints, or stigma associated with food stamps. Jesse Shapiro, “Is there a Daily Discount Rate? Evidence from the Food Stamp Nutrition Cycle,” Journal of Public Economics, 89(2-3): 303-325, 2005, http://www.brown.edu/Research/Shapiro/pdfs/highfreq111703.pdf.
[36] Jessica Todd, “Revisiting the Supplemental Nutrition Assistance Program cycle of food intake: Investigating heterogeneity, diet quality, and a large boost in benefit amounts,” Applied Economic Perspectives and Policy, 37(3): 437-458, 2015, https://academic.oup.com/aepp/article-abstract/37/3/437/8261.
[37] Jessica Todd and Christian Gregory, “Changes in Supplemental Nutrition Assistance Program real benefits and daily caloric intake among adults,” Food Policy, August 2018, https://onlinelibrary.wiley.com/doi/10.1093/aepp/ppu039.
[38] Kuhn, 2016, op. cit.
[39] Karen Hamrick and Margaret Andrews, “SNAP participants’ eating patterns over the benefit month: a time use perspective,” PloS One, 11(7): e0158422, 2016, http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0158422; Todd, op. cit.
[40] Christian Gregory and Travis Smith, “Salience, food security, and SNAP receipt,” Journal of Policy Analysis and Management, 38(1): 124-154, 2019, https://onlinelibrary.wiley.com/doi/epdf/10.1002/pam.22093. Gregory and Smith’s finding that SNAP households have a higher propensity to report food hardships at the end of the benefit month is consistent with existing literature on the benefit cycle, but they also found that the propensity to report food hardships was higher at the beginning of the month as well. They suggest that recent experiences of hardships at the end of the month may still be fresh in recipients’ minds even after they have received benefits, or that SNAP households may feel they need to justify receiving SNAP benefits.
[41] James Weinstein, Katie Martin, and Ann Ferris, “Household food security varies within month and is related to childhood anemia,” Journal of Hunger & Environmental Nutrition, 4(1): 48-61, 2009, https://www.tandfonline.com/doi/abs/10.1080/19320240802706833.
[42] Eric Calloway et al., “Monthly SNAP benefit duration and its association with food security, hunger-coping, and physiological hunger symptoms among low-income families,” Journal of Applied Research on Children, 6(2), 2015, https://digitalcommons.library.tmc.edu/childrenatrisk/vol6/iss2/5/.
[43] The HEI is a measure of diet quality used to assess how well a set of foods aligns with key recommendations of the Dietary Guidelines for Americans. The maximum possible score is 100, though the typical American diet falls well short of the ideal. See Eliza Whiteman, Benjamin Chrisinger, and Amy Hillier, “Diet quality over the monthly Supplemental Nutrition Assistance Program cycle,” American Journal of Preventive Medicine, 55(2): 205-212, 2018, https://www.sciencedirect.com/science/article/pii/S0749379718317343; Amy Hillier et al., “The Influence of SNAP Participation and Food Environment on Nutritional Quality of Food at Home Purchases,” University of Kentucky Center for Poverty Research Discussion Paper Series, DP2016-10, 2016, https://uknowledge.uky.edu/ukcpr_papers/111/; and Michael Kuhn, “Who feels the calorie crunch and when? The impact of school meals on cyclical food insecurity,” Journal of Public Economics 166: 27-38, 2018, https://www.sciencedirect.com/science/article/abs/pii/S0047272718301452. All three studies use national data on food purchases. A third study, based on a small sample of women receiving SNAP benefits in Texas, found even larger reductions in the HEI four weeks after benefit receipt. See Namrata Sanjeevi and Jeanne Freeland-Graves, “Monthly variations in dietary intake of women participating in the Supplemental Nutrition Assistance Program,” Journal of the Academy of Nutrition and Dietetics, 119(2): 261-271, 2019, https://www.sciencedirect.com/science/article/pii/S221226721830755X.
[44] Smith et al., op. cit.
[45] Todd, op. cit. and Anna Kharmats et al., “Relation between the Supplemental Nutritional Assistance Program cycle and dietary quality in low-income African Americans in Baltimore, Maryland,” American Journal of Clinical Nutrition, 99(5): 1006-1014, 2014, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3985207/. The latter study is based on a small, non-random sample that is not easily generalized to a larger population.
[46] Anika Schenck-Fontaine, Anna Gassman-Pines, and Zoelene Hill, “Use of informal safety nets during the Supplemental Nutrition Assistance Program benefit cycle: how poor families cope with within-month economic instability,” Social Service Review, 91(3): 456-487, September 2017, https://www.journals.uchicago.edu/doi/pdfplus/10.1086/694091. This study is based on a small, non-random sample of predominately African American families that is not easily generalized to a larger population.
[47] Calloway et al., op. cit.
[48] Agustina Laurito and Amy Ellen Schwartz, “Does school lunch fill the ‘SNAP gap’ at the end of the month?” Southern Economic Journal, 86(1): 49-82, 2019, https://onlinelibrary.wiley.com/doi/abs/10.1002/soej.12370.
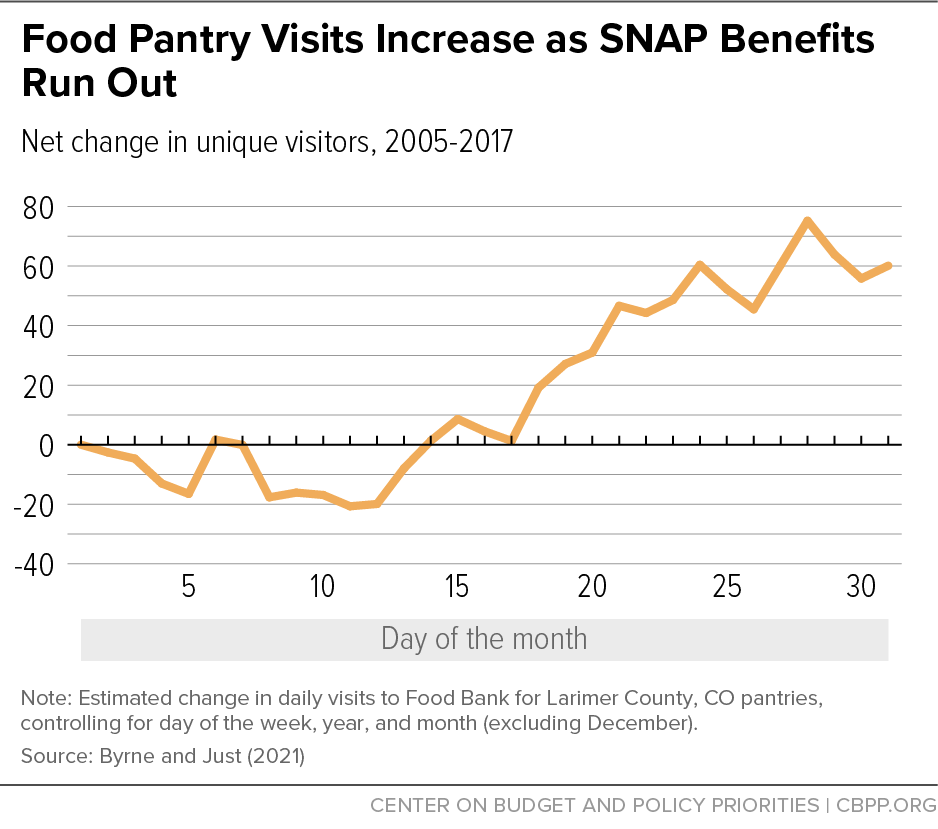
[49] Anne Byrne and David Just, “The other half: an examination of monthly food pantry cycles in the context of SNAP benefits,” Applied Economic Perspectives and Policy, January 2021, https://onlinelibrary.wiley.com/doi/abs/10.1002/aepp.13150; and Linlin Fan et al., “The use of charitable food assistance among low‐income households in the United States,” Journal of the Academy of Nutrition and Dietetics, 121(1): 27–35, 2020, https://jandonline.org/article/S2212-2672(20)30995-3/fulltext.
[50] Anna Gassman-Pines and Laura Bellows, “Food instability and academic achievement: a quasi-experiment using SNAP benefit timing,” American Educational Research Journal, 55(5): 897-927, 2018, http://journals.sagepub.com/doi/10.3102/0002831218761337; Chad Cotti, John Gordanier, and Orgul Ozturk, “When does it count? The timing of food stamp receipt and educational performance,” Economics of Education Review, 66: 40-50, 2018, https://www.sciencedirect.com/science/article/abs/pii/S0272775718303649; Lisa Gennetian et al., “Supplemental Nutrition Assistance Program (SNAP) benefit cycles and student disciplinary infractions,” Social Service Review, 90(3): 403-33, 2016, https://www.journals.uchicago.edu/doi/abs/10.1086/688074; and Timothy Bond et al., “Hungry for Success? SNAP Timing, High-Stakes Exam Performance, and College Attendance,” National Bureau of Economic Research, January 2021, https://www.nber.org/papers/w28386.
[51] Keenan Marchesi, “The Impact of the SNAP Distribution Cycle on Student Non-Cognitive Outcomes,” unpublished manuscript, December 2019, https://www.clarku.edu/departments/economics/wp-content/blogs.dir/5/files/sites/130/2019/12/KMarchesi_JMP_ForPosting.pdf.
[52] Bita Farkhad, Chad Meyerhoefer, and James Dearden, “The within-month pattern of medical care utilization among SNAP households,” prepared for Agricultural & Applied Economics Association Annual Meeting, July 2017, https://ageconsearch.umn.edu/record/258361/files/Abstracts_17_05_24_11_45_07_15__128_180_43_235_0.pdf. This study, which looked at SNAP benefits and health care consumption among one- and two-parent households, found that the decline in medical care use occurs mainly in two-parent households; and Eliza Kinsey et al., “Chronic disease self-management during the monthly SNAP cycle,” Current Developments in Nutrition, 3(Supplement 1): nzz051-P04, 2019, https://academic.oup.com/cdn/article/3/Supplement_1/nzz051.P04-193-19/5517923. This study is based on a small, non-random sample of African American women that is not easily generalized to a larger population.
[53] Hilary Seligman et al., “Exhaustion of food budgets at month’s end and hospital admissions for hypoglycemia,” Health Affairs, 33(1): 116-123, 2014, https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2013.0096; and Sanjay Basu, Seth Berkowitz, and Hilary Seligman, “The monthly cycle of hypoglycemia: an observational claims-based study of emergency room visits, hospital admissions, and costs in a commercially insured population,” Medical Care, 55(7): 639-645, 2017, https://journals.lww.com/lww-medicalcare/fulltext/2017/07000/The_Monthly_Cycle_of_Hypoglycemia__An.1.aspx. Neither study accounts for differences between the calendar month and the SNAP issuance cycle (most states stagger issuance of SNAP benefits over several days of each month), so it is difficult to attribute the results solely to the timing of SNAP benefits; other factors — such as receipt of monthly paychecks — may also be at work.
[54] Irma Arteaga, Colleen Heflin, and Leslie Hodges, “SNAP benefits and pregnancy-related emergency room visits,” Population Research and Policy Review, 37(6): 1031-1052, 2018, https://link.springer.com/article/10.1007/s11113-018-9481-5; Colleen Heflin et al., “Childhood injuries and food stamp benefits: an examination of administrative data in one US state,” BMC Pediatrics, 20(1): 1-8, 2020, https://bmcpediatr.biomedcentral.com/articles/10.1186/s12887-020-02084-y#citeas; and Chad Cotti, John Gordanier, and Orgul Ozturk, “Hunger pains? SNAP timing and emergency room visits,” Journal of Health Economics, 71, 102313, 2020, https://www.sciencedirect.com/science/article/abs/pii/S0167629619301316.
[55] While the study did not control for household income or expenses, the study sample was limited to SNAP households also participating in Medicaid in Missouri, which had very stringent household income limits (in most cases, households had incomes below 33 percent of the poverty line). The authors explain that their results are biased downward (households with larger benefits, after adjusting for household size, have lower levels of income or higher expenses, along with other unobserved factors correlated with health disadvantage). The protective effect of larger SNAP benefits compensated for the negative selection among households with higher SNAP benefits. See Colleen Heflin, Leslie Hodges, and Peter Mueser, “Supplemental Nutrition Assistance Program benefits and emergency room visits for hypoglycaemia,” Public Health Nutrition, 20(7): 1314-1321, 2017, https://www.cambridge.org/core/journals/public-health-nutrition/article/supplemental-nutrition-assistance-progam-benefits-and-emergency-room-visits-for-hypoglycaemia/D8A24285B12FC9B6C03069CAE62DC90A; Chinedum Ojinnaka and Colleen Heflin, “Supplemental Nutrition Assistance Program size and timing and hypertension-related emergency department claims among Medicaid enrollees,” Journal of the American Society of Hypertension (2018), https://doi.org/10.1016/j.jash.2018.10.001; and Colleen Heflin et al., “SNAP benefits and childhood asthma,” Social Science & Medicine, 220: 203-211, 2019, https://www.sciencedirect.com/science/article/abs/pii/S0277953618306294.
[56] The Families First Coronavirus Response Act enacted in March 2020 allows states to issue temporary emergency allotments up to the maximum benefit that a SNAP household can receive. More recently, Congress temporarily raised maximum allotments for all households to 115 percent of the June 2020 value of the TFP between January and September 2021. There are no assessments of the impact of these changes yet.
[57] As noted above, USDA sets SNAP benefits for Alaska, Hawaiʻi, Guam, and the Virgin Islands differently from the rest of the country because the cost of food is different in these areas. Thus, these areas experienced different benefit increases than the rest of the United States. Because Hawaiʻi’s Thrifty Food Plan exceeded Recovery Act levels beginning in fiscal year 2013, its SNAP benefits were already set higher than Recovery Act levels, so its residents did not experience a cut when the Recovery Act provision expired in November 2013. SNAP households in Alaska, Guam, and the Virgin Islands experienced a benefit cut in November 2013 that was the same in proportional terms, but slightly different in dollar terms, from the cut in the 48 other states and the District of Columbia.
[58] Todd, op. cit.
[59] Todd and Gregory, op. cit.
[60] Elaine Waxman, Craig Gundersen, and Megan Thompson, “How Far Do SNAP Benefits Fall Short of Covering the Cost of a Meal?” Urban Institute, February 2018, https://www.urban.org/sites/default/files/publication/96661/how_far_do_snap_benefits_fall_short_of_covering_the_cost_of_a_meal_2.pdf.
[61] George Davis, Wen You, and Yangliang Yang, “Are SNAP benefits adequate? A geographical and food expenditure decomposition,” Food Policy, 95: 101917, 2020, https://www.sciencedirect.com/science/article/abs/pii/S0306919220301214.
[62] If SNAP households can identify and shop at the store with the lowest food cost in their area, the fraction that can afford the TFP rises above 90 percent. This assumption, however, is unlikely to hold for many SNAP households. The median size of the counties in this study is over 600 square miles, making it extremely unlikely that shoppers could identify and travel to the lowest-cost store. Even if they could, they would incur significant travel costs, which may outweigh their savings on food. See Bronchetti, Christensen, and Hansen, op. cit. See also Garret Christensen and Erin Bronchetti, “Local food prices and the purchasing power of SNAP benefits,” Food Policy, 95: 101937, 2020, https://www.swarthmore.edu/sites/default/files/assets/documents/user_profiles/ebronch1/FoodAPSPaper_Revision_2019.12.17_compiled.pdf.
[63] Qingxiao Li and Metin Çakır, “Thrifty Food Plan panel price index and the real value of SNAP benefits,” prepared for presentation at the 2020 Agricultural & Applied Economics Association Annual Meeting, Kansas City, Missouri, July 26-28, 2020, https://ssrn.com/abstract=3669951.
[64] Christian Gregory and Alisha Coleman-Jensen, “Do high food prices increase food insecurity in the United States?” Applied Economic Perspectives and Policy, 35(4): 679-701, 2013, https://onlinelibrary.wiley.com/doi/10.1093/aepp/ppt024.
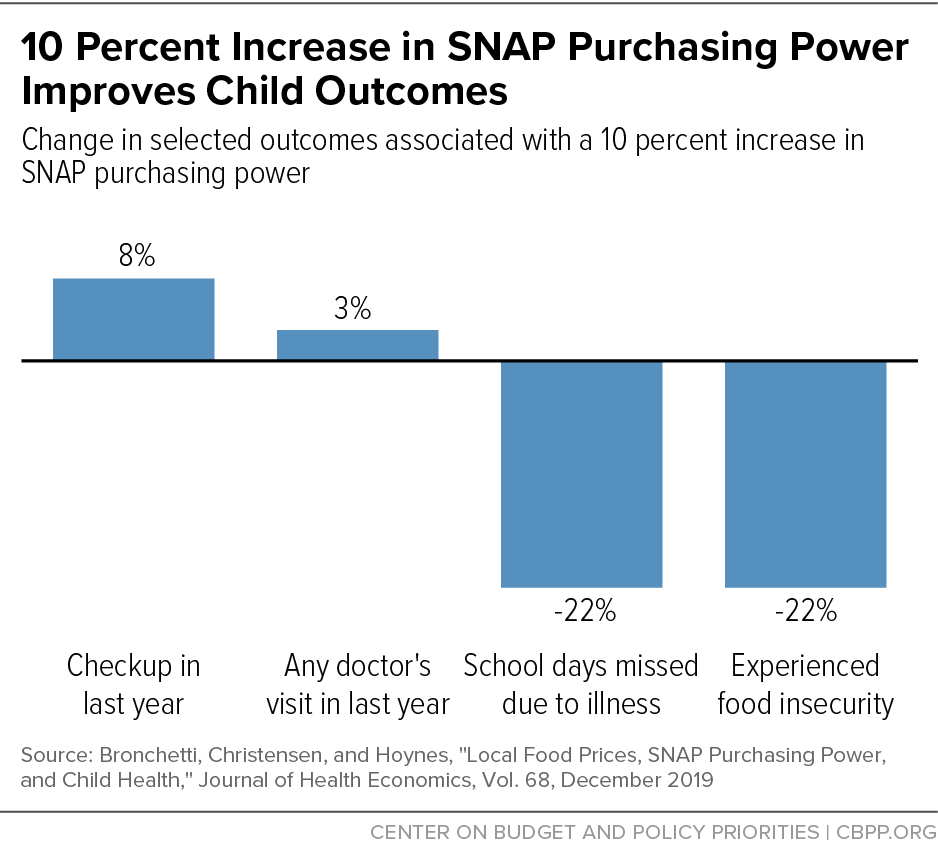
[65] These studies are based on survey data that predate the Affordable Care Act’s Medicaid expansion for adults. In Erin Bronchetti, Garret Christensen, and Hilary Hoynes, “Local food prices, SNAP purchasing power, and child health,” Journal of Health Economics, 68: 102231, 2019, https://www.sciencedirect.com/science/article/abs/pii/S0167629619304151, the authors use National Health Interview Survey data from 1999 to 2010, while Bronchetti, Christensen, and Hansen, op. cit. use National Household Food Acquisition and Purchase Survey data from 2012.
[66] Laura Castner and James Mabli, “Low-Income Household Spending Patterns and Measures of Poverty,” Mathematica Policy Research, April 2010, https://fns-prod.azureedge.net/sites/default/files/SpendingPatterns.pdf.
[67] Increasing SNAP benefits would have different effects depending on participants’ current spending on food and their outstanding needs. Many households would increase overall food spending, some could buy a similar quantity of food but shift toward buying more nutritious products, and others could shift non-SNAP income currently spent on food to other basic needs. An estimated 15 to 30 percent of SNAP households may be “extra-marginal,” meaning their SNAP benefits equal or exceed what they report spending on food at home. Households may be extra-marginal if they do not need more food than what they can purchase with SNAP benefits, or if they do need more food than what they can purchase with their SNAP benefits but their income is so low that they must spend all of it meeting other basic needs and have no income available for food. See David Johnson et al., “Assessing the effectiveness of SNAP by examining extramarginal participants,” University of Michigan Institute for Social Research Population Studies Center, April 2018, https://www.psc.isr.umich.edu/pubs/abs/14834. Research shows high rates of food insecurity for SNAP households with the lowest incomes, suggesting that current benefits are inadequate for these households. A benefit increase would likely make a meaningful difference in the lives of most participating households.
[68] Mark Nord and Mark Prell, “Food Security Improved Following the 2009 ARRA Increase in SNAP Benefits,” USDA Economic Research Service, April 2011, https://www.ers.usda.gov/webdocs/publications/44837/7469_err116.pdf?v=7982.4; Charlotte Tuttle, “The stimulus act of 2009 and its effect on food-at-home spending by SNAP participants,” USDA Economic Research Service, August 2016, https://www.ers.usda.gov/publications/pub-details/?pubid=74689; Pourya Valizadeh and Travis Smith, “How did the American Recovery and Reinvestment Act affect the material well-being of SNAP participants? A distributional approach,” Applied Economic Perspectives and Policy, 42(3): 455-476, 2019, https://onlinelibrary.wiley.com/doi/abs/10.1093/aepp/ppy039.
[69] Jiyoon Kim, “Do SNAP participants expand non-food spending when they receive more SNAP benefits? — Evidence from the 2009 SNAP benefits increase,” Food Policy 65(64): 9-20, 2016, https://www.sciencedirect.com/science/article/pii/S0306919216304341. These results are similar to research showing that participating in SNAP substantially increases spending on housing and utilities, education and other enrichment activities, and transportation. See Lorenzo Almada and Jaehyun Nam, “The effects of SNAP on non-food expenditure: an instrumental variables approach,” unpublished manuscript, 2016, https://data.ers.usda.gov/FANRP-ridge-project-summaries.aspx?type=2&summaryId=270.
[70] Mark Nord, “Effects of the decline in the real value of SNAP benefits from 2009 to 2011,” USDA Economic Research Service, August 2013, https://www.ers.usda.gov/publications/pub-details/?pubid=45102.
[71] Jiyoon Kim, Matthew Rabbitt, and Charlotte Tuttle, “Changes in Low-income households’ spending and time use patterns in response to the 2013 sunset of the ARRA-SNAP benefit,” Applied Economic Perspectives and Policy, 42(4): 2020, https://onlinelibrary.wiley.com/doi/abs/10.1093/aepp/ppz007.
[72] Gregory Bruich, “The effect of SNAP benefits on expenditures: New evidence from scanner data and the November 2013 benefit cuts,” Harvard University, unpublished manuscript, 2014, http://scholar.harvard.edu/files/bruich/files/bruich_2014b.pdf.
[73] Nord and Prell, op. cit.
[74] Nord and Prell, op. cit. This study concluded that the SNAP benefit increase “played a substantial role in the improvement” of low-income households’ food security improvements from 2008 to 2009. During this time, the odds of low food security among this population declined by about 20 percent, and the odds of food insecurity declined by about 11 percent among all low-income households. Because these improvements are concentrated among SNAP households, which make up about half of low-income households, these effects were likely much greater.
The data available at this time so far suggests that food insecurity increased markedly during the COVID-19 pandemic and economic fallout. The additional nutritional benefits appeared to have helped, but not enough to reverse the trend toward higher levels of food insecurity. This may be in part because the initial increase in food assistance provided was not well targeted and the poorest households didn’t get additional assistance, some of the benefits took a long time to roll out, and the nature of the crisis — which affected a very large group of households and disrupted school as well as employment — may have taken a larger toll. There are also questions about the comparability of the survey data. Additional data and research in the coming years will help to understand the nature of hardship during the pandemic. See Brynne Keith-Jennings et al., op cit.
[75] Nord, op. cit.
[76] Among households that participated less frequently in the prior 12 months, food insecurity increased by 7 percent and very low food security increased by 9 percent. Bhagyashree Katare and Jiyoon Kim, “Effects of the 2013 SNAP benefit cut on food security,” Applied Economic Perspectives and Policy, 39(4): 662–681, 2017, https://onlinelibrary.wiley.com/doi/10.1093/aepp/ppx025.
[77] These researchers found no significant difference in the prevalence of food insecurity among participants in low-cost areas. See Xinzhe Cheng, Young Jo, and Jiyoon Kim, “Heterogeneous impact of supplemental nutrition assistance program benefit changes on food security by local prices,” American Journal of Preventive Medicine, 58(3): e97-e103, 2020, https://www.sciencedirect.com/science/article/abs/pii/S0749379719304787.
[78] Lorenzo Almada and Ian McCarthy, “It’s a cruel summer: Household responses to reductions in government nutrition assistance,” Journal of Economic Behavior & Organization, 143(11): 45-57, 2017, http://www.sciencedirect.com/science/article/pii/S0167268117302330.
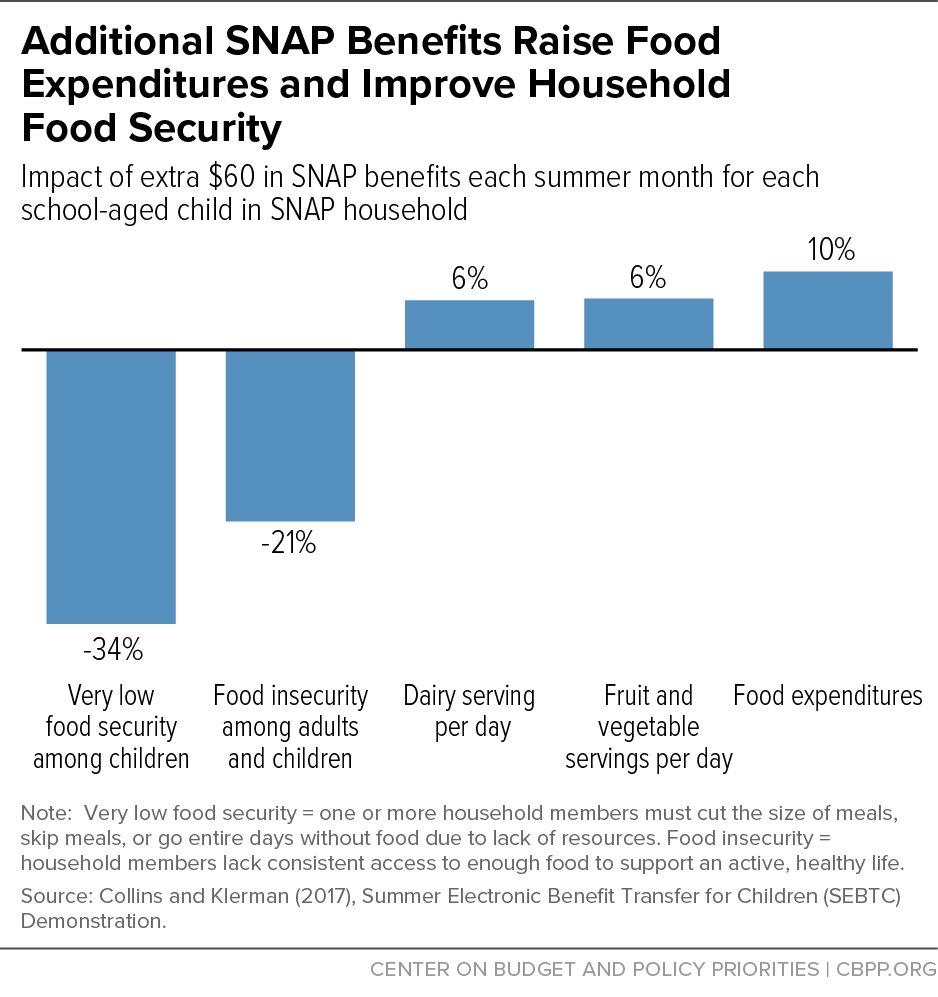
[79] The demonstration initially provided a monthly benefit of $60 in the summer of 2012 and then compared the relative effectiveness of a smaller benefit ($30) in the summers of 2013 and 2014. The results suggested that both increases produced similar improvement in the most severe form of food insecurity among children. See Ann Collins and Jacob Klerman, “Improving nutrition by increasing Supplemental Nutrition Assistance Program benefits,” American Journal of Preventive Medicine, 52(2S2): S179-S185, 2017, https://www.sciencedirect.com/science/article/pii/S0749379716303890.
[80] Zoë Neuberger, “Recovery Legislation Could Help End Summer Childhood Hunger,” CBPP, June 30, 2021, https://www.cbpp.org/research/food-assistance/recovery-legislation-could-help-end-summer-childhood-hunger.
[81] Gregory Chojnacki et al., “A randomized controlled trial measuring effects of extra Supplemental Nutrition Assistance Program (SNAP) benefits on child food security in low-income families in rural Kentucky,” Journal of the Academy of Nutrition and Dietetics, 121(1): S9-S21, 2021, https://www.sciencedirect.com/science/article/pii/S2212267220305426; and Phillip Gleason et al., “Measuring the effects of a demonstration to reduce childhood food insecurity: A randomized controlled trial of the Nevada Healthy, Hunger Free Kids project,” Journal of the Academy of Nutrition and Dietetics, 121(1): S22-S33, 2021, https://www.sciencedirect.com/science/article/pii/S2212267220302094.
The research teams identified several reasons why these demonstrations did not find the expected improvements in food security status comparable to previous research. Improving local economies may have made it easier for some households to meet their food needs even without the projects’ benefits. In addition, the benefit increase may have been targeted to households that were less likely to face food insecurity to begin with. Families typically address the nutritional needs of very young children before those of older children and adults, for example, so modest increases in food assistance may be unlikely to translate into further improvements in food security among these children. In addition, some have noted that the standard measure of food security, where a household is either food secure or not, does not capture the effects of improvements that lessen food hardship even if they fall short of completely lifting households out of food insecurity. Incorporating measures of the depth and severity of food insecurity would allow for a more nuanced assessment of potential improvements in food insecurity status due to higher benefits. See Craig Gundersen, “A consideration of the Evaluation of Demonstration Projects to End Childhood Hunger (EDECH),” Journal of the Academy of Nutrition and Dietetics, 121(1): S78-S80, 2021, https://jandonline.org/article/S2212-2672(20)30547-5/fulltext.
[82] Lauren Bauer et al., “The Effect of Pandemic EBT on Measures of Food Hardship,” Hamilton Project, July 2020, https://www.hamiltonproject.org/assets/files/P-EBT_LO_7.30.pdf. The American Rescue Plan of 2021 ensures that states can provide P-EBT benefits for the full duration of the public health emergency, including during the summer.
[83] Geetha Waehrer, Partha Deb, and Sandra L. Decker, “Did the 2009 American Recovery and Reinvestment Act affect dietary intake of low-income individuals?” Economics & Human Biology, 19: 170-183, 2015, https://www.sciencedirect.com/science/article/pii/S1570677X1500060X; and Katelin Hudak, Elizabeth Racine, and Lisa Schulkind, “An increase in SNAP benefits did not impact food security or diet quality in youth,” Journal of the Academy of Nutrition and Dietetics. 121(3): 507-519, 2020, https://www.sciencedirect.com/science/article/abs/pii/S2212267220313198.
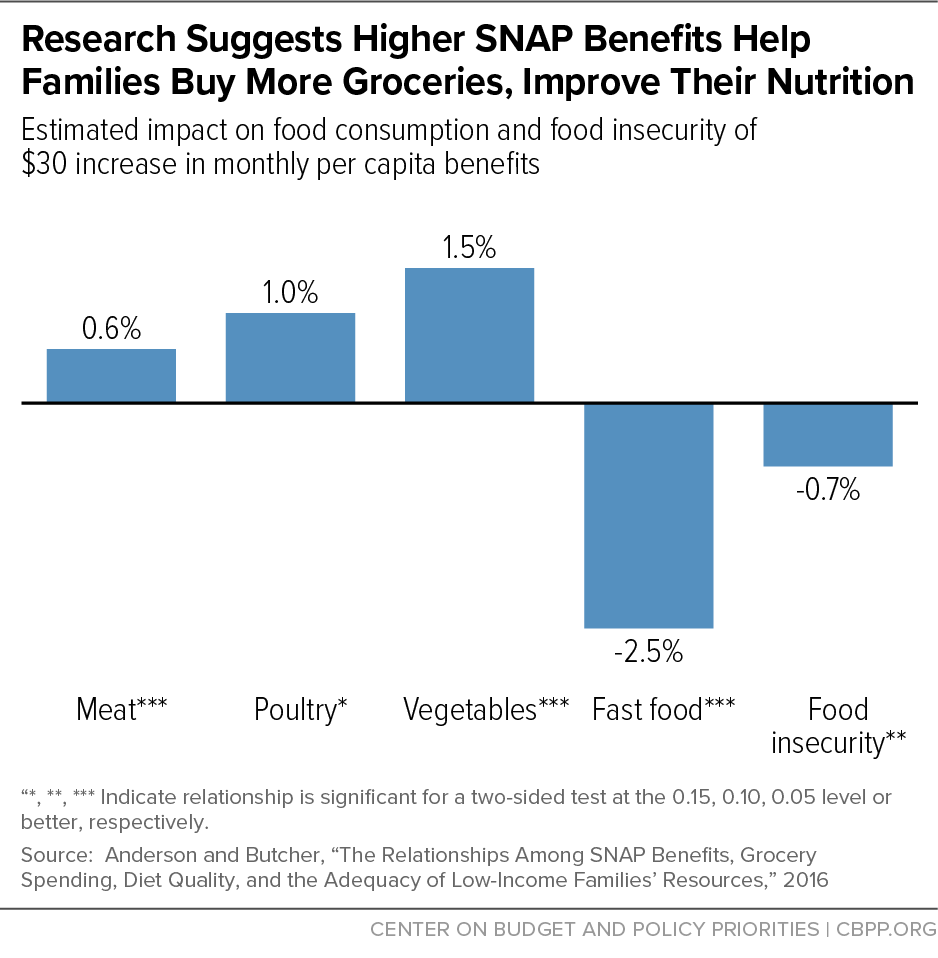
[84] Patricia Anderson and Kristin Butcher, “The Relationships Among SNAP Benefits, Grocery Spending, Diet Quality, and the Adequacy of Low-Income Families’ Resources,” CBPP, June 14, 2016, https://www.cbpp.org/research/food-assistance/the-relationships-among-snap-benefits-grocery-spending-diet-quality-and#:~:text=Despite%20SNAP's%20reach%2C%20questions%20remain,per%20month%20among%20SNAP%20recipients. There is also some evidence that raising food expenditures — both out of pocket and from SNAP benefits — is associated with increases in fruit and vegetable consumption. See Namrata Sanjeevi and Jeanne Freeland-Graves, “Association of grocery expenditure relative to Thrifty Food Plan Cost with diet quality of women participating in the Supplemental Nutrition Assistance Program,” Journal of the Academy of Nutrition and Dietetics, 118(12): 2315-2323, 2018, https://www.sciencedirect.com/science/article/pii/S2212267218307640. This study is based on a small, non-random sample of primarily Hispanic women in central Texas that is not easily generalized to a larger population.
[85] Rebecca Cleary, Clare Cho, and Becca Jablonski, “SNAP Benefit Allotments and Dietary Quality,” prepared for presentation at the 2018 Agricultural & Economics Association Annual Meeting, August 2018.
[86] Chelsea Rose et al., “Small increments in diet cost can improve compliance with the Dietary Guidelines for Americans,” Social Science & Medicine, 266: 113359, 2020, https://www.sciencedirect.com/science/article/abs/pii/S0277953620305785.
[87] Maeve Gearing, Sujata Dixit-Joshi, and Laurie May, “Barriers That Constrain the Adequacy of Supplemental Nutrition Assistance Program (SNAP) Allotments: Survey Findings,” USDA, Food and Nutrition Service, June 2021, https://www.fns.usda.gov/snap/barriers-constrain-adequacy-snap-allotments.
[88] Most children in families with low incomes were eligible for Medicaid and the Children’s Health Insurance Program (CHIP) even before the Affordable Care Act. In the study sample, approximately 6 percent of low-income children had delayed care due to cost. Three percent and 4 percent of children in low-income households and low-income single-parent households, respectively, reported needing health care but not being able to afford it. Taryn Morrissey and Daniel Miller, “Supplemental Nutrition Assistance Program participation improves children’s health care use: an analysis of the American Recovery and Reinvestment Act's natural experiment,” Academic Pediatrics, 20(6): 863-870, 2020, https://www.sciencedirect.com/science/article/abs/pii/S1876285919304619; and Katelin Hudak and Elizabeth Racine, “Do additional SNAP benefits matter for child weight? Evidence from the 2009 benefit increase,” Economics & Human Biology, 41: 100966, 2020, https://www.sciencedirect.com/science/article/pii/S1570677X20302367.
[89] Rajan Sonik, Susan Parish, and Monika Mitra, “Inpatient Medicaid usage and expenditure patterns after changes in Supplemental Nutrition Assistance Program benefit levels,” Preventing Chronic Disease, 15: e120, 2018, https://europepmc.org/articles/pmc6178899. These results, based on national data on hospital admissions, are consistent with earlier research based on admissions in Massachusetts following the Recovery Act increases. See Rajan Sonik, “Massachusetts inpatient Medicaid cost response to increased Supplemental Nutrition Assistance Program benefits,” American Journal of Public Health, 106(3): 443–448, 2016, https://ajph.aphapublications.org/doi/full/10.2105/AJPH.2015.302990.
[90] Elizabeth March et al., “Boost to SNAP Benefits Protected Young Children’s Health,” Children’s HealthWatch, October 2011, https://childrenshealthwatch.org/wp-content/uploads/SNAPincrease_brief_October2011.pdf. A child was considered “well” if she was not overweight or underweight and her parents reported her to be in good health, developing normally for her age, and never hospitalized.
[91] The authors hypothesize that parental stress and bandwidth may explain the relationship between SNAP and child check-ups, but cannot directly test this in the study. See Bronchetti, Christensen, and Hoynes, op. cit.
[92] National Academies of Sciences, Engineering, and Medicine, A Roadmap to Reducing Child Poverty. Washington, D.C.: The National Academies Press, February 2019, http://sites.nationalacademies.org/dbasse/bcyf/reducing_child_poverty/index.htm. While the authors discuss two SNAP expansions (which would expand the maximum benefit by 20 and 30 percent), they also propose a 35 percent benefit increase as part of a package that would reduce child poverty by 50 percent (which they term the “means-tested supports and work poverty reduction package”).
[93] Chuck Marr et al., “American Rescue Plan Act Includes Critical Expansions of Child Tax Credit and EITC, CBPP, March 12, 2021, https://www.cbpp.org/research/federal-tax/american-rescue-plan-act-includes-critical-expansions-of-child-tax-credit-and; CBPP, “Make Child Tax Credit Improvements Permanent in Upcoming Recovery Legislation,” June 21, 2021, https://www.cbpp.org/blog/make-child-tax-credit-improvements-permanent-in-upcoming-recovery-legislation.
[94] For example, poverty rates were twice as high for Black (18.8 percent) and Hispanic people (15.7 percent) as non-Hispanic white people (7.3 percent) in 2019; the poverty rate among Asian Americans and Pacific Islanders (10.2 percent) was 40 percent higher. Jessica Semega et al., Income and Poverty in the United States: 2019, U.S. Census Bureau, September 2020, https://www.census.gov/library/publications/2020/demo/p60-270.html. Non-Hispanic Black households were more than twice as likely — and Hispanic households twice as likely — to be food insecure in 2019 (19.1 percent and 15.6 percent, respectively) as non-Hispanic white households (7.9 percent). Very low food security among children, while rare, is five times more likely among non-Hispanic Black households than among non-Hispanic white households (1.7 vs 0.3 percent). Coleman-Jensen et al., op. cit.
[95] SNAP households with a Black head of household accounted for 12.4 percent of U.S. households in 2018 but 26.6 percent of households participating in SNAP. Similarly, households headed by a Hispanic or Latino (of any race) individual accounted for 13.5 percent of households and 22.3 percent of SNAP households. Households headed by an American Indian or Alaska Native individual made up 0.7 percent of households but 1.5 percent of SNAP households. Households with a white head of household, in contrast, accounted for 76.0 percent of households but only 59.3 percent of SNAP households. Households headed by an Asian individual made up 4.9 percent of U.S. households but 2.9 percent of SNAP households. See Tracy Loveless, “Supplemental Nutrition Assistance Program (SNAP) Receipt for Households: 2018,” U.S. Census Bureau, June 2020, https://www.census.gov/library/publications/2020/demo/acsbr20-01.html.
[96] Craig Gundersen, Brent Kreider, and John V. Pepper, “Reconstructing the Supplemental Nutrition Assistance Program to more effectively alleviate food insecurity in the United States,” Russell Sage Foundation Journal of the Social Sciences, 4(2): 113–130, 2018, https://www.jstor.org/stable/pdf/10.7758/rsf.2018.4.2.06.pdf.
[97] Andrea Wiley, Re-imagining Milk: Cultural and Biological Perspectives, London and New York: Routledge 2015 as cited in Angela Babb, “America’s ‘Thrifty Food Plan’: hunger, mathematics, and the valuation of nutrition assistance,” Annals of the American Association of Geographers, 110(4): 983-1004, 2020, https://www.tandfonline.com/doi/abs/10.1080/24694452.2019.1664889.
[98] Hayden Stewart, Diansheng Dong, and Andrea Carlson, “Why Are Americans Consuming Less Fluid Milk? A Look at Generational Differences in Intake Frequency,” Economic Research Service, USDA, May 2013, https://ageconsearch.umn.edu/record/262223/; and Andrea Carlson et al., op. cit.
[99] Gundersen, Kreider, and Pepper, op. cit.; Anderson and Butcher, op. cit. For comparison, the average SNAP benefit per person in fiscal year 2018 was $125 per month or $29 per week.
[100] The authors estimate a national average cost of a low-income meal by using the food spending reported by low-income but food-secure households in the Current Population Survey. This national cost of a meal is then adjusted at the county level using the county-level cost of a TFP market basket. See Waxman, Gundersen, and Thompson, op. cit.
[101] Ziliak, op. cit.; Craig Gundersen, Elaine Waxman, and Amy Crumbaugh, “An examination of the adequacy of supplemental nutrition assistance program (SNAP) benefit levels: impacts on food insecurity,” Agricultural and Resource Economics Review, 48(3): 433-447, 2019, https://www.cambridge.org/core/journals/agricultural-and-resource-economics-review/article/an-examination-of-the-adequacy-of-supplemental-nutrition-assistance-program-snap-benefit-levels-impacts-on-food-insecurity/59160A1F2A28CFA2DB686516C144B388; and Gundersen, Kreider, and Pepper., op. cit.