BEYOND THE NUMBERS
Social Security Disability Insurance (DI) aids people who, because of a severe medical impairment, can no longer support themselves by working — a catastrophe that can happen to anyone. Contrary to uninformed claims, DI eligibility criteria are stringent:
- Solid work history. DI applicants must have worked for at least one-fourth of their adult lives and in at least five of the last ten years to earn insured status.
- Severe impairment. Applicants must suffer from a severe, medically determinable physical or mental impairment that’s expected to last 12 months or result in death. Evidence must come from acceptable medical sources and consist of clinical facts and findings, not just opinion. The Social Security Administration (SSA) orders its own examination where necessary.
- Inability to do substantial work. The impairment must prevent the applicant from performing “substantial gainful activity,” currently defined as earning $1,090 per month. That’s equivalent to working less than full time at the minimum wage, or about 40 percent of median earnings for full-time workers with a high school diploma but no college. The law specifically requires that the applicant's impairment must render him not just unable to do his past work, but unable — considering his age, education, and work experience — to do any other kind of work, regardless of whether that work exists in his immediate area or whether he’d be hired.
- Waiting period. DI is not for the temporarily disabled. A worker’s impairment must last for at least five months before the applicant can qualify for DI. Sick leave, private insurance, family help, or savings might tide people over this waiting period; Supplemental Security Income may be available for some of the poorest.
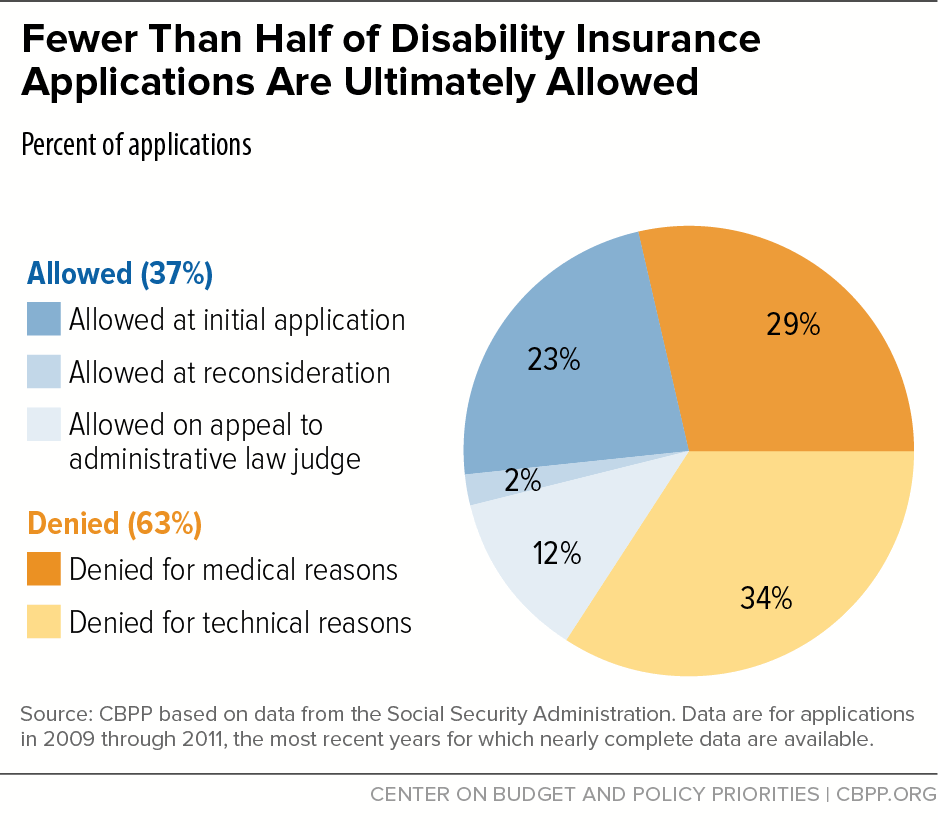
SSA weeds out applicants who are technically disqualified (chiefly because they lack insured status) and sends the rest to each state’s disability determination service (DDS) for medical evaluation. If denied there, the applicant may appeal. Typical processing times at the DDS level are three to four months, and processing times at the appeal (hearing) level typically exceed one year. Ultimately, fewer than 40 percent of 2009-2011 applicants (including those that don’t pass initial screening) were awarded benefits (see graph) — and there’s evidence that the rate has fallen since then.
DI recipients are subject to periodic “continuing disability reviews” to verify that they are still disabled. Those reviews save about $10 in benefits for each $1 they cost. Nevertheless, congressional parsimony has hampered SSA’s ability to conduct these reviews on schedule.
In short, applying for DI requires most workers to go without a paycheck for many months in order to seek a benefit that’ll replace (on average) about half of their past earnings, with a big risk that they’ll be rejected, and — if they succeed — regular reviews to ensure that they remain eligible. (Also, DI recipients qualify for Medicare, but only after a two-year wait.) Those aren’t features of a lax program.