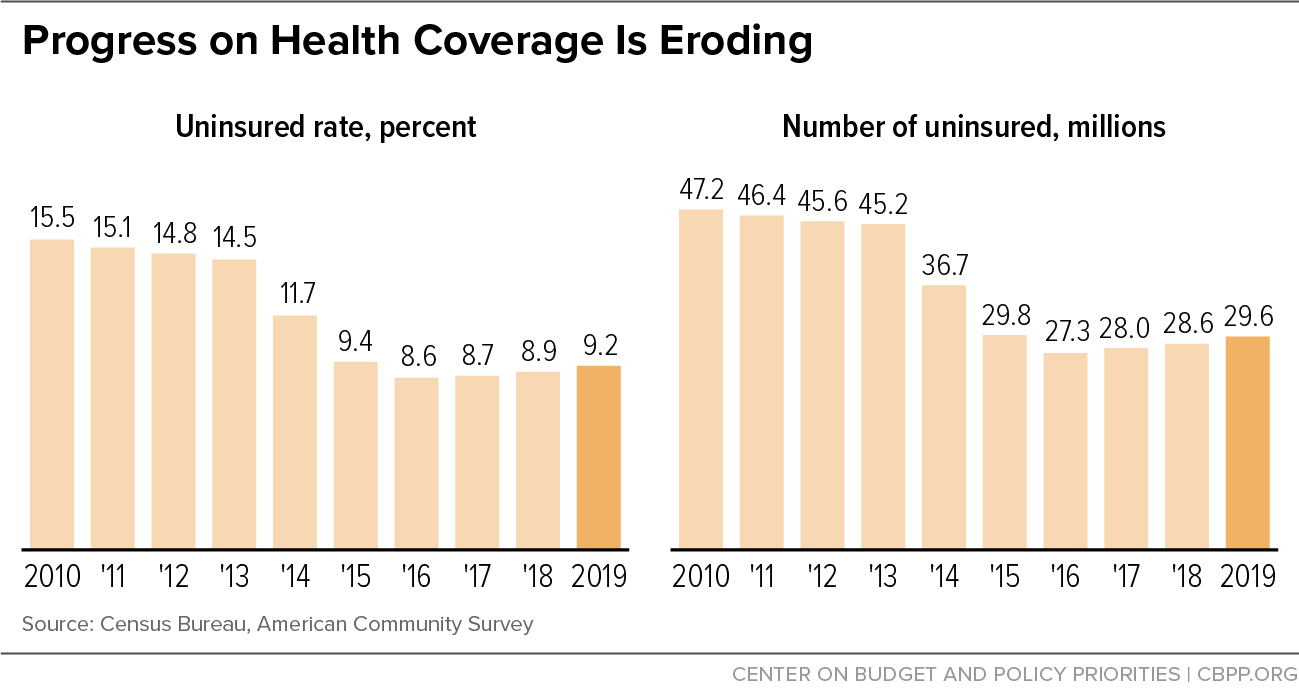
Uninsured Rate Rose Again in 2019, Further Eroding Earlier Progress
End Notes
[1] Katherine Keisler-Starkey and Lisa N. Bunch, “Health Insurance Coverage in the United States: 2019,” Census Bureau, September 2020, https://www.census.gov/content/dam/Census/library/publications/2020/demo/p60-271.pdf.
[2] The uninsured rate among only those people under age 65 has increased slightly more, from 10.0 percent in 2016 to 10.8 percent in 2019.
[3] CPS data for 2019 were collected in February through April 2020. Census noted the challenges of data collection during this time and the significantly higher non-response rate, especially among lower-income people, creating the potential for bias in the sample that would impact CPS results. Thus, the Census report published today stated, “[This report] primarily uses the ACS 1-year estimates to examine coverage for key population and to compare changes in coverage between 2018 and 2019. ACS 1-year estimates data were collected during 2019, and thus, data collection occurred before the COVID-19 pandemic.”
[4] The NHIS shows that the uninsured rate rose to 10.3 percent in 2019 from 9.4 percent in 2018. While changes in the NHIS methodology could have affected the results, CDC’s initial testing shows that even with these changes, the 2019 estimates of the uninsured rate for non-elderly adults can be compared to estimates from previous years. For the CDC’s explanation of the 2019 NHIS questionnaire redesign, see https://www.cdc.gov/nchs/data/nhis/earlyrelease/EReval202005-508.pdf.
[5] Jennifer Haley et al., “One in Five Adults in Immigrant Families with Children Reported Chilling Effects on Public Benefit Receipt in 2019,” Urban Institute, June 18, 2020, https://www.urban.org/research/publication/one-five-adults-immigrant-families-children-reported-chilling-effects-public-benefit-receipt-2019.
[6] Matt Broaddus, “Research Note: Medicaid Enrollment Decline Among Adults and Children Too Large to Be Explained by Falling Unemployment,” Center on Budget and Policy Priorities, July 17, 2019, https://www.cbpp.org/research/health/medicaid-enrollment-decline-among-adults-and-children-too-large-to-be-explained-by.
[7] Centers for Medicare & Medicaid Services, “Medicaid & CHIP Enrollment Data,” https://www.medicaid.gov/medicaid/national-medicaid-chip-program-information/medicaid-chip-enrollment-data/index.html.
[8] Centers for Medicare & Medicaid Services, “Trends in Subsidized and Unsubsidized Enrollment,” August 12, 2019, https://www.cms.gov/CCIIO/Resources/Forms-Reports-and-Other-Resources/Downloads/Trends-Subsidized-Unsubsidized-Enrollment-BY17-18.pdf.
[9] Council of Economic Advisers, “2017 Economic Report of the President,” December 15, 2016, https://obamawhitehouse.archives.gov/sites/default/files/docs/2017_economic_report_of_president.pdf.
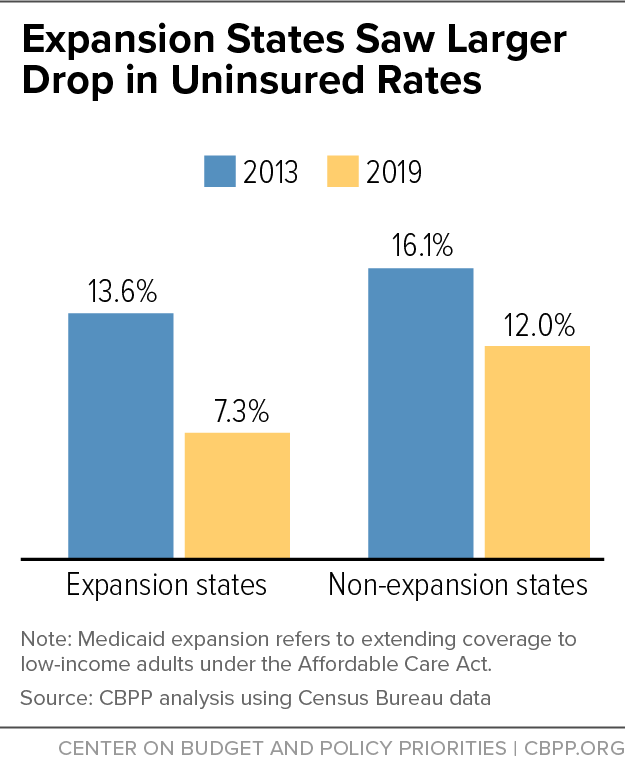
[10] CBPP analysis using ACS data for 2013 through 2018. Medicaid expansion states are defined as states that had implemented the ACA Medicaid expansion to low-income adults by January 2018.
[11] Matt Broaddus, “Medicaid Enrollment Continues to Rise,” Center on Budget and Policy Priorities, September 9, 2020, https://www.cbpp.org/blog/medicaid-enrollment-continues-to-rise.
[12] Sarah Lueck and Matt Broaddus, “Emergency Special Enrollment Period Would Boost Health Coverage Access at a Critical Time,” Center on Budget and Policy Priorities, July 30, 2020, https://www.cbpp.org/research/health/emergency-special-enrollment-period-would-boost-health-coverage-access-at-a-critical.
[13] Linda Blumberg et al., “State-by-State Estimates of the Coverage and Funding Consequences of Full Repeal of the ACA,” Urban Institute, March 2019, https://www.urban.org/sites/default/files/publication/100000/repeal_of_the_aca_by_state.pdf.