BEYOND THE NUMBERS
4,109 More Arkansans Lost Medicaid in October for Not Meeting Rigid Work Requirements
Some 4,109 Arkansas Medicaid beneficiaries lost coverage on October 1 for not reporting at least 80 hours of work or work-related activities for three months, the state reports. That brings the total to 8,462 beneficiaries who have lost coverage since the state implemented its rigid work requirement. These individuals are locked out of Medicaid for the rest of 2018 even if they report 80 hours of work or work-related activities in future months or become exempt from the requirement due to illness or other reasons.
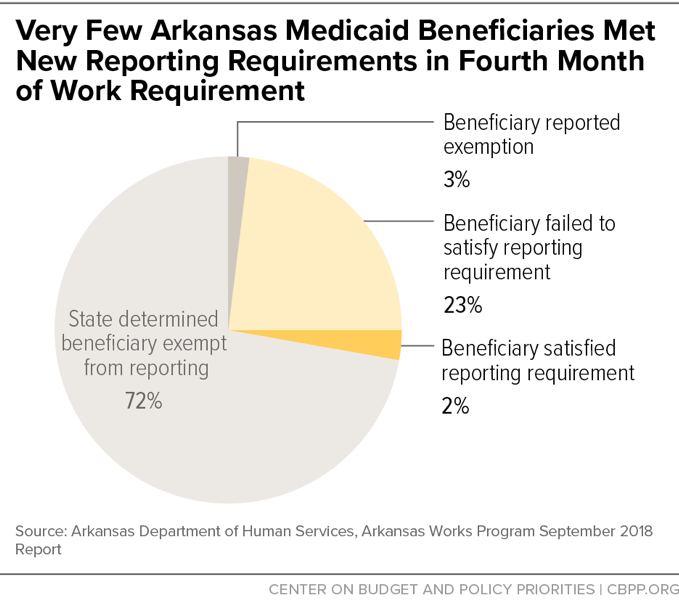
Over 16,000 beneficiaries (23 percent of those subject to the work requirement) didn’t report sufficient work hours in September (see chart). Almost 5,000 beneficiaries now have two months of non-compliance with the work requirement and will lose coverage if they don’t report 80 hours of work or work-related activities for another month this year. And another 7,500 have one month of non-compliance and will lose coverage if they have two more non-compliance months. Thousands of them will likely lose coverage in the coming months.
Good cause exemptions, which are available for beneficiaries who can’t comply or report compliance due to circumstances beyond their control, don’t appear to be protecting vulnerable beneficiaries. In September, Arkansas’ Medicaid agency granted only 140 good cause exemptions for August — though over 16,000 beneficiaries didn’t comply with the reporting requirement that month. Good cause exemptions were available for beneficiaries who couldn’t report due to a statewide computer outage that affected the online reporting portal on the last day to report compliance in September, but few beneficiaries apparently knew it was available. Like other provisions of the work requirement, beneficiaries bear the burden to know the exemption exists, understand that they qualify, and email a request to the agency, which may be hard for beneficiaries with limited Internet and email access.
A new Kaiser Family Foundation brief, based on interviews with state officials, health plans, providers, and beneficiary advocates, details some of the factors that are likely leading eligible Medicaid beneficiaries to slip through the cracks and lose coverage in Arkansas:
- Many beneficiaries are likely unaware that they face a work requirement. The state and health plans have conducted much of their outreach through phone calls, but the state has no phone numbers, or incorrect numbers, for many beneficiaries. Other outreach through social media or online videos didn’t likely reach beneficiaries without Internet access. Finally, the state’s notices contain incomplete information and aren’t available in Spanish.
- Many enrollees have trouble using the online portal to report exemption and compliance activities. Even if beneficiaries have Internet access and sufficient computer literacy — which many don’t — setting up an online account and reporting work hours requires multiple steps. And although the state has authorized “registered reporters” to log hours for beneficiaries, many beneficiaries aren’t using them because they don’t know about the service or may not understand the new work requirements.
- Beneficiaries are likely struggling to meet the rigid work requirements. Transportation is a major barrier to work, and there are few jobs in the state’s rural areas and for workers with low education levels. Medicaid funds can’t be used for work supports, which are key to overcoming barriers to work, and the number of beneficiaries seeking assistance from the Department of Workforce Services will likely strain the Department’s resources because the state hasn’t boosted its funding to meet this need. Further, although beneficiaries can comply with the work requirement by volunteering, that may not be practical for those with limited information about available opportunities and limited transportation options to do so.
As we’ve explained, research suggests that only a small minority of Medicaid beneficiaries potentially subject to the state’s work requirement aren’t already working and wouldn’t qualify for an exemption. The Arkansas experience thus far shows that many eligible beneficiaries who are working or qualify for an exemption are nevertheless getting caught up in the complex policy and restrictive reporting requirements and losing coverage.