Taking Away Medicaid for Not Meeting Work Requirements Harms Low-Wage Workers
Medicaid is a critical source of health coverage for working people in low-wage jobs, which often don’t offer health benefits. Sixty percent of adult Medicaid enrollees not receiving federal disability benefits through the Supplemental Security Income (SSI) program work. Of those who don’t work, half live in working families, and more than 80 percent report that they are in school or unable to work due to illness, disability, or caregiving responsibilities.
Now, the Trump Administration is allowing states to take away Medicaid coverage from people who don’t document that they work a specified number of hours each month. Contrary to a common misconception, this won’t just hurt non-working enrollees; it also will likely cause many working people to lose coverage.
For people with low-wage jobs, such as food services, construction, or retail, work hours often fluctuate from month to month, leaving them short of the required minimum in some months even as they exceed it in others. Low-wage jobs are also unstable, with frequent job losses that leave people unable to find work in some months. Also, some enrollees who meet work requirements may still lose coverage because they get tripped up by red tape and paperwork.
The Administration is allowing states to impose work requirements on adult Medicaid enrollees other than those who are 65 or older, pregnant, or qualify for Medicaid because they receive disability benefits through SSI. In Arkansas, the first state to implement such a policy, over 18,000 Medicaid beneficiaries lost coverage in 2018 due to the new requirements. While a federal court halted Arkansas’ policy, the Administration is continuing to approve similar policies in other states. Many of these policies require enrollees to document that they work or engage in other work activities (e.g., job training or volunteer work) for at least 80 hours per month unless they prove that they qualify for limited exemptions.
Working People with Unstable Jobs Will Lose Coverage
Approved and pending state work requirement policies reflect an assumption that people who want to work can find steady employment with regular work hours — an assumption out of step with the realities of today’s low-wage labor market.
Many Medicaid enrollees work in industries in which both employment and hours are volatile. The two industries that employ the most Medicaid enrollees potentially subject to work requirements are restaurants/food services and construction; many enrollees also work at grocery stores, department stores, and discount stores or provide home health or child care services. These industries generally have above-average rates of involuntary part-time work, where employees want full-time work but can’t get it. In the food service and retail industries, large shares of workers report fluctuating weekly hours; these industries also have above-average rates of irregular scheduling, in which employees are expected to be on call and available for much of the week but may receive well under 20 hours of work per week. The low-wage labor market is also characterized by frequent job loss. In the retail and construction industries, for example, job separation rates are well above private-sector averages. While many factors contribute to this high turnover, one is a lack of flexibility: workers may lose their job if an illness, family emergency, or breakdown in child care arrangements forces them to take even a short amount of time off from work.
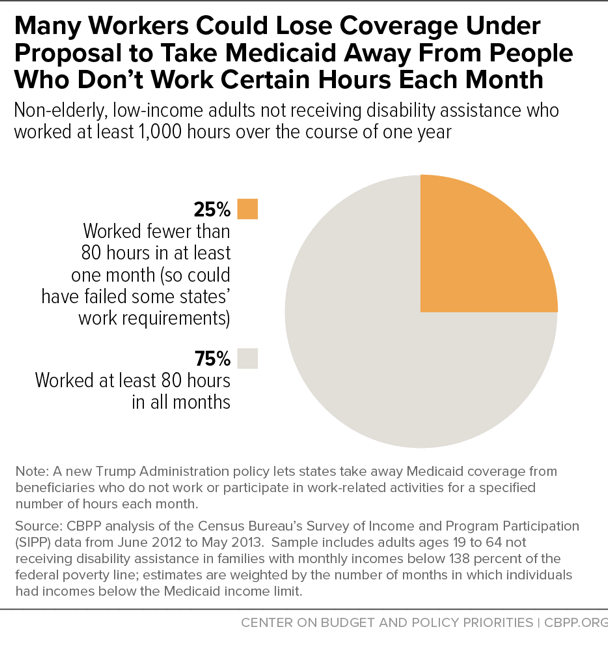
A large share of low-wage workers would be at risk of losing coverage under an 80-hour work requirement, analysis of 2012-2013 Survey of Income and Program Participation data shows. Among adults age 19 to 64 not receiving federal disability assistance and with incomes that would qualify them for Medicaid, most worked at least some of the year. But among those who were working, 46 percent worked fewer than 80 hours in at least one month. Even among those who worked at least 1,000 hours over the course of the year — or about 80 hours per month, on average — 25 percent would have failed to meet an 80-hour work requirement in at least one month. (See chart.) This means that if all states adopted such policies, millions of working people could lose coverage or face interruptions in coverage due to unstable employment or volatile work hours.
Other Workers Will Lose Coverage Due to Red Tape
On top of these challenges, some workers who comply with work requirements also will likely lose coverage due to paperwork requirements and other reporting burdens. To prove that they are in compliance, Medicaid enrollees may have to submit paystubs, timesheets, or other documents, potentially from multiple employers. This will be challenging for enrollees and create many chances for people to lose coverage due to inadvertent paperwork mistakes — theirs, their employer’s, or the state’s. Meeting reporting requirements may also involve taking time off from work to visit an eligibility office, waiting to get through to a caseworker, or using online portals that aren’t readily available to people who lack computers or Internet access.
Some states’ policies are even more onerous. Arkansas, for example, required enrollees to report their hours for the previous month by the fifth of each month; workers who missed that deadline were automatically treated as out of compliance for the month. These requirements almost certainly led some eligible workers to lose coverage.
Loss of Coverage Will Worsen People’s Health
Losing coverage worsens health for all groups, which is why physician organizations like the American Medical Association, American Academy of Family Physicians, American Academy of Pediatrics, and others oppose Medicaid work requirements. But coverage losses and interruptions in coverage are especially harmful for people with serious health needs, for whom loss of access to medications and other treatment can lead to serious deterioration in health, increased emergency room visits and hospitalizations, and higher health care costs, research has shown.
Low-income people have above-average rates of chronic conditions and other health challenges. Even working Medicaid enrollees — who are generally healthier than other enrollees — have high rates of serious health needs. For example, a study of working adults enrolled in Michigan’s Medicaid expansion found that more than half had a serious physical health condition such as heart disease, asthma, or diabetes, and 25 percent had a mental health condition, often depression.
Work Requirements Will Make It Harder for People to Keep Working
Among working people who gained coverage through Medicaid expansion in Ohio and Michigan, majorities reported that gaining coverage made them better at their jobs or made it easier for them to keep working. That probably reflects the fact that, for the many Medicaid enrollees with serious health conditions, Medicaid provides access to needed treatments that allow them to control these conditions and maintain employment.
In contrast, Medicaid work requirements are likely to set off a vicious cycle for some working enrollees. One common cause of job loss among low-wage workers is health problems, in part because, as noted, low-wage jobs offer little flexibility (most don’t provide sick leave, for example). In states with work requirements, health setbacks resulting in job loss may then lead to loss of coverage and access to treatment, making it far harder for people to regain health and employment. Similarly, loss of coverage due to failure to document enough hours of work may result in deteriorating health, causing job loss.
Thus, while the Administration argues that Medicaid work requirements will improve economic mobility, they are likelier to do the opposite — in addition to reducing coverage, access to care, and financial security and worsening health.