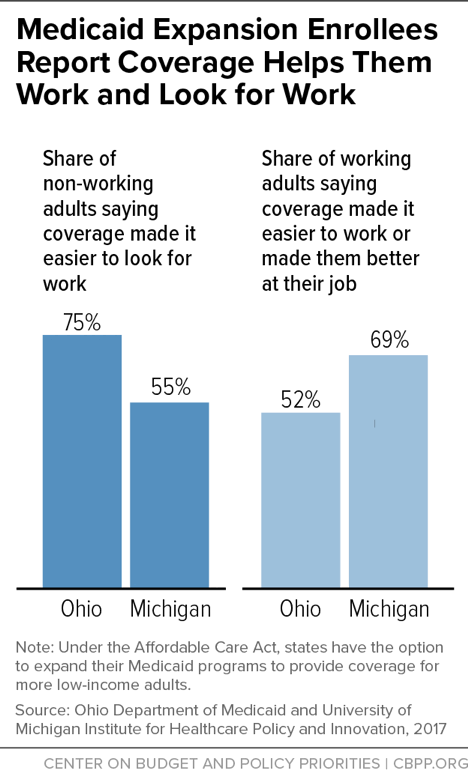Executive Summary: Taking Medicaid Coverage Away From People Not Meeting Work Requirements Will Reduce Low-Income Families’ Access to Care and Worsen Health Outcomes
Centers for Medicare & Medicaid Services (CMS) guidance issued in January 2018 allows states — for the first time — to take Medicaid coverage away from people not engaging in work or work-related activities for a specified number of hours each month. CMS has already approved work requirement policies in Kentucky, Indiana, Arkansas, and New Hampshire — although a federal court vacated its approval of Kentucky’s proposal — and other states are seeking approval for similar approaches. The guidance follows unsuccessful attempts by congressional Republicans to allow states to tie Medicaid eligibility to work as part of bills to “repeal and replace” the Affordable Care Act (ACA).
State proposals for Medicaid work requirements will cause many low-income adults to lose health coverage, including people who are working or are unable to work. State proposals for Medicaid work requirements will cause many low-income adults to lose health coverage, including people who are working or are unable to work due to mental illness, opioid or other substance use disorders, or serious chronic physical conditions, but who cannot overcome various bureaucratic hurdles to document that they either meet work requirements or qualify for an exemption from them. These coverage losses will not only reduce access to care and worsen health outcomes, but will likely make it more difficult for many people to find or keep a job. Thus, Medicaid work requirements may be self-defeating on their own terms.
CMS argues that work requirements will “promote better… health” because they will increase employment and thereby improve health and well-being.[2] These claims, however, are not based on evidence and do not withstand scrutiny.
-
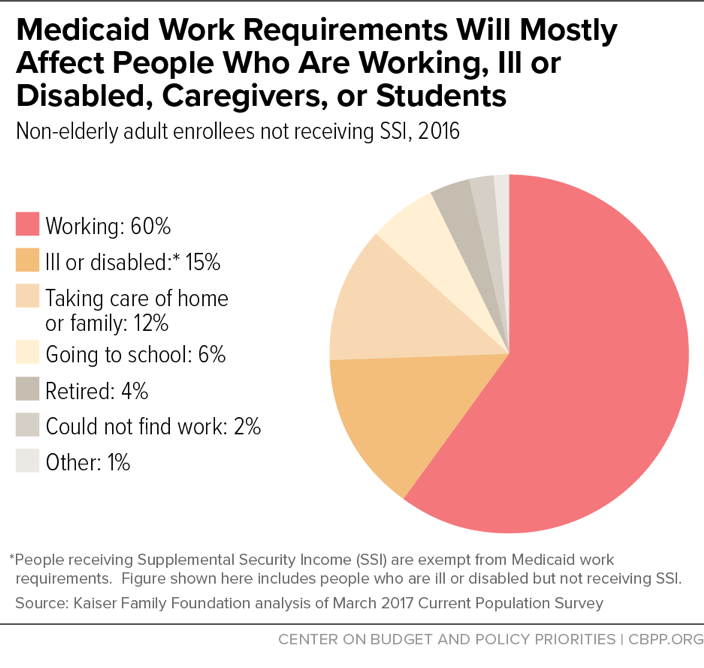
Work requirements will make it harder for most adult beneficiaries — the lion’s share of whom are already working or are ill, disabled, caregivers, or in school — to get and stay covered. Supporters of work requirements generally say that these policies target only people who are not working, actively seeking work, caregivers, in school, or unable to work because of an illness or disability. The CMS guidance, however, allows states to apply work requirements to nearly all non-elderly adult Medicaid enrollees, except pregnant women and some people with disabilities. Of the roughly 25 million people nationally who could be subject to work requirements, 60 percent are already working (see Figure 1), and 79 percent have at least one worker in the family. Of those who aren’t themselves working, more than 80 percent are in school or report an illness, disability, or caregiving responsibilities that keep them from working. Yet states could require most of these 25 million enrollees to meet burdensome paperwork and documentation requirements to prove that they are working or volunteering sufficient hours each month or meet the criteria for an exemption.
The unfortunate reality is that, for the large majority of enrollees who are already working or face serious barriers to employment, work requirements have little or no possible benefit. But they will add red tape and bureaucratic hurdles that will cause some of these people to lose coverage. Documentation and paperwork requirements have been repeatedly shown to reduce enrollment in Medicaid across the board,[3] and people with serious mental illness or physical impairments may face particular challenges in meeting these new documentation and paperwork requirements.
Bearing out these concerns, studies of state Supplemental Nutrition Assistance Program (SNAP, formerly known as food stamps) and Temporary Assistance for Needy Families (TANF) programs have found that state errors in administering work requirements are common, and people with disabilities, serious illnesses, and substance use disorders may be disproportionately likely to lose benefits, even when they should be exempt. Other enrollees could lose coverage because they are between jobs even though they are actively seeking work, or because their disability or illness— while a serious obstacle to work — does not meet the specific criteria for an exemption laid out in a state’s policies.
Still other enrollees may lose or see interruptions in coverage because their work hours fluctuate from month to month, sometimes falling below required thresholds. Fluctuating hours are particularly common in the two industries with the largest number of Medicaid enrollees: restaurant/food services and construction. Among working low-income adults who could be subject to Medicaid work requirements, nearly half would fail to meet an 80-hour-per-month work requirement like Kentucky’s in at least one month during the year.
Overall, a substantial majority of those losing coverage due to work requirements would be people who are working or who should qualify for exemptions, but fail to overcome the new documentation requirements and other hurdles to maintain their coverage, a recent Kaiser Family Foundation analysis concluded.
-
Work requirements are unlikely to promote employment and may be counterproductive. The CMS guidance offers no evidence that Medicaid work requirements will increase employment. As discussed below, research on work requirements in other programs finds that they generally have only modest and temporary effects on employment, failing to increase long-term employment or reduce poverty.
Results in Medicaid are likely to be just as disappointing, and could be worse, for several reasons. First, as noted, most of those affected by the requirements are either already working or face major barriers to work. Second, Medicaid enrollees targeted by work requirement proposals already have a strong incentive to work: without working, they can get health care but usually little other assistance, and they generally are very poor. Enrollees who are seemingly able to work but aren’t employed typically lack not motivation, but work supports such as job search assistance, job training, child care, and transportation assistance; they may also face challenges such as an undiagnosed substance use disorder, domestic violence, the need to care for an ill family member, or a housing crisis. State Medicaid programs generally are not well equipped to provide or connect families with work support services, which are already oversubscribed in most states. Moreover, the CMS guidance does not require states to offer any work supports in tandem with instituting work requirements — in fact, it prohibits them from using federal Medicaid funding to do so.
Finally, health coverage is itself an important work support. As a Kaiser Family Foundation review of the available research concludes, “access to affordable health insurance has a positive effect on people’s ability to obtain and maintain employment.”[4] Having health care helps people work and look for work, and taking it away will likely make it harder for some to keep and find work. For example, among non-working adults gaining coverage through the ACA’s Medicaid expansion in Ohio and Michigan, majorities said having health care made it easier to look for work. And among working adults, majorities said coverage made it easier for them to work or made them better at their jobs. (See Figure 2.) Moreover, health problems are a common cause of job loss; for example, a person coping with diabetes or depression may lose his or her job because the condition worsens. If job loss also leads to loss of health care and access to treatment, people will only find it harder to get back on their feet.
-
The primary effect of work requirements will be less access to care, worse health outcomes, and less financial security. States themselves project significant coverage losses from work requirements, with Kentucky estimating that 15 percent of all adult Medicaid enrollees — at least 97,000 people — will lose coverage due to work requirements and other provisions of its waiver. As discussed below, studies of both the ACA’s Medicaid expansion and pre-ACA coverage expansions find that they increased access to care — including preventive care, mental health and substance use treatment, and appropriate management of chronic conditions — and improved enrollees’ financial security and health outcomes. For those losing coverage due to work requirements, these gains will be reversed.
Moreover, two groups for whom coverage losses and interruptions in coverage are especially harmful — people with serious chronic health conditions, including mental illness, and people with substance use disorders — make up a large fraction of those likely to lose coverage due to work requirements. An Ohio study found that nearly one-third of adults enrolled through the ACA Medicaid expansion have a substance use disorder, while 27 percent have been diagnosed with at least one serious physical health condition, such as diabetes or heart disease, just since enrolling in Medicaid. A Michigan study found that among non-working Medicaid expansion enrollees, 72 percent have a serious chronic physical health condition, while 43 percent have a mental health condition, often depression.
For people with these conditions, even the temporary loss of access to medications or other treatment could be harmful or sometimes catastrophic. This is one reason why major physician organizations — including the American Medical Association, American Academy of Family Physicians, American Academy of Pediatrics, American College of Obstetricians and Gynecologists, American College of Physicians, American Osteopathic Association, and American Psychiatric Association — oppose Medicaid work requirements.[5]
Medicaid Criteria Changes Don’t Ensure Waivers Will Further Program Objectives
Policy Basics
Health
End Notes
[1] The full report is available at https://www.cbpp.org/research/health/taking-medicaid-coverage-away-from-people-not-meeting-work-requirements-will-reduce.
[2] CMS letter to state Medicaid directors (18-002), January 11, 2018, https://www.medicaid.gov/federal-policy-guidance/downloads/smd18002.pdf.
[3] Margot Sanger-Katz, “Hate Paperwork? Medicaid Recipients Will Be Drowning In It,” New York Times, January 18, 2018, https://www.nytimes.com/2018/01/18/upshot/medicaid-enrollment-obstacles-kentucky-work-requirement.html.
[4] Larisa Antonisse and Rachel Garfield, “The Relationship Between Work and Health: Findings from a Literature Review,” Kaiser Family Foundation, August 7, 2018, https://www.kff.org/medicaid/issue-brief/the-relationship-between-work-and-health-findings-from-a-literature-review/.
[5] American Medical Association, “Physicians Oppose Harmful Changes to Medicaid, Benefits Rules,” November 14, 2017, https://wire.ama-assn.org/ama-news/physicians-oppose-harmful-changes-medicaid-benefits-rules; America’s Frontline Physicians: Statement on Medicaid Work Requirements, January 12, 2018, https://www.acog.org/About-ACOG/News-Room/Statements/2018/Americas-Frontline-Physicians-Statement-on-Medicaid-Work-Requirements.
More from the Authors

Areas of Expertise

Areas of Expertise