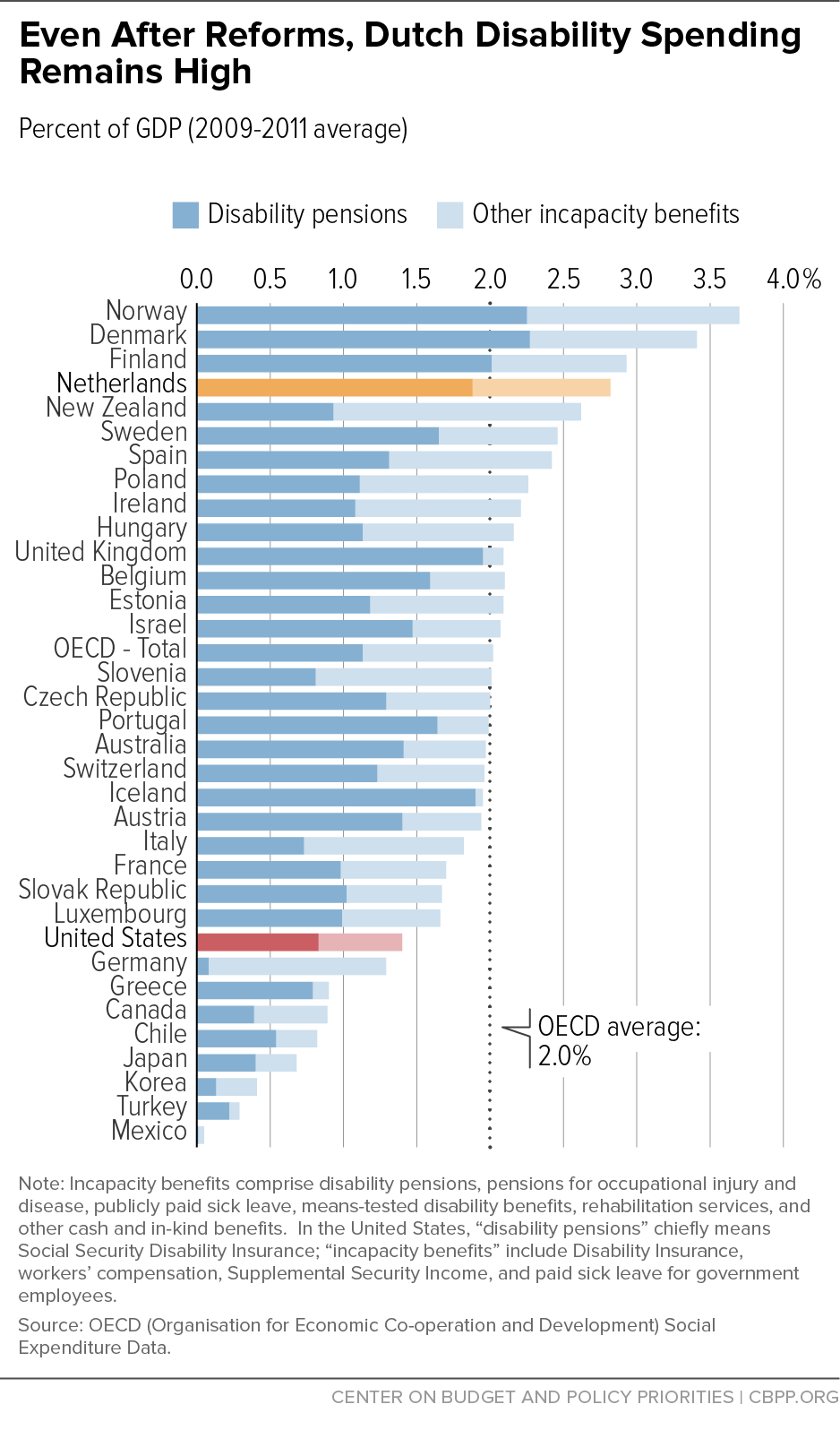In the 30 years from 1980 to 2010, the number of workers receiving Social Security Disability Insurance (DI) increased by 187 percent.[1] The addition of 5.3 million people to the DI rolls resulted primarily from demographic factors that were long anticipated: an increase in the U.S. population of over 80 million, entry into the labor force of over 25 million women, and the aging of the baby boom generation. Although DI expansion had long been expected, the increase nevertheless spurred some critics to call for restructuring the DI program to reduce its costs. Some of these critics cite the Netherlands as a model for action.[2] This paper examines the relevance of the Dutch experience as a blueprint for U.S. DI reform, with a particular focus on the potential for cost savings.
Dutch disability insurance is one component of a comprehensive national system that also covers short-term work incapacity (sickness), vocational rehabilitation, maternity, and health care. Dutch DI benefits cover partial and temporary as well as full, permanent impairment, replace high portions of workers’ past wages, and are financed by employers (without worker contributions).
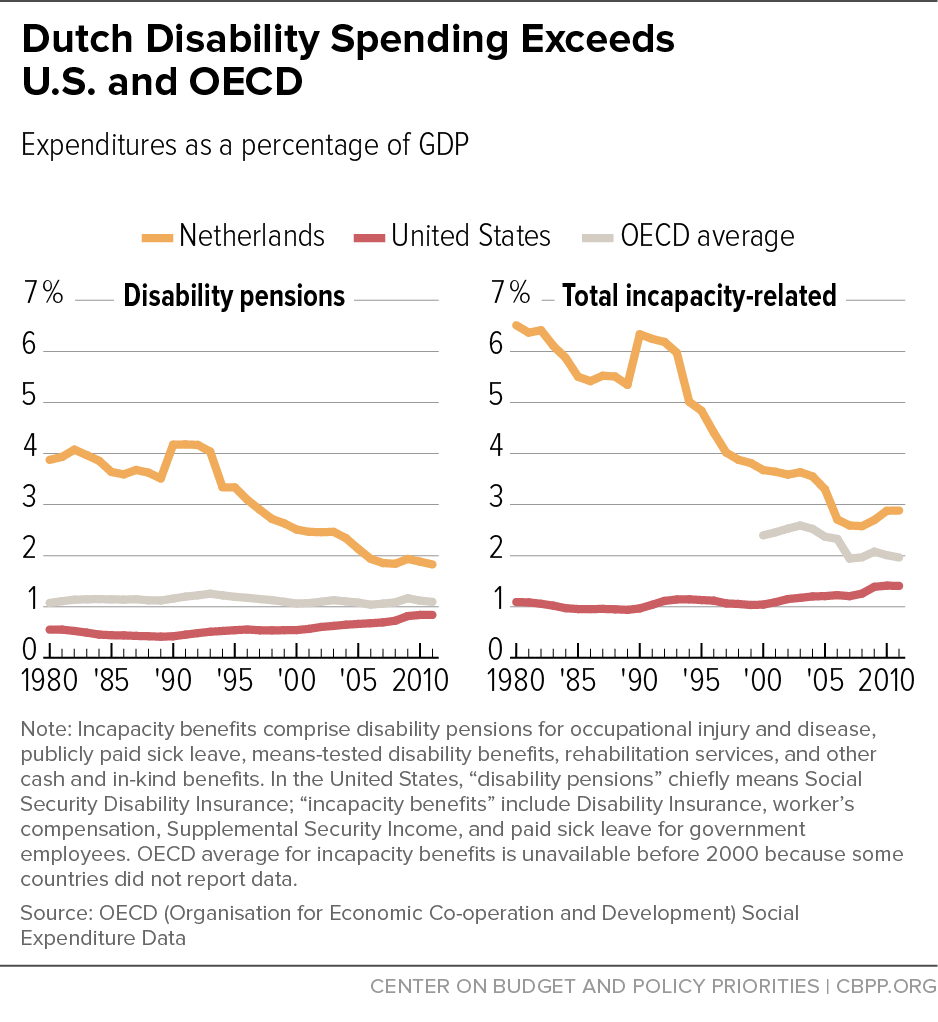
At its peak in 1990, Dutch spending on disability pensions had climbed above 4 percent of gross domestic product (GDP), or more than four times the current U.S. DI rate.[3] (See Figure 1.) By 2010 the Dutch had reversed this expansion through a wide variety of program changes. In the early to mid-1980s, they reduced benefits modestly and restricted eligibility. When expenditures started to rise again, the Dutch shifted the costs of sickness benefits to employers and extended benefit duration (1996). Subsequently (1998), the government shifted a portion of the costs of disability benefits to individual employers and introduced experience rating of employer DI contributions to reflect rates of disability in individual firms.[4] In a new round of program restructuring (2002), the Dutch required employers to rehabilitate and accommodate their sick workers (the Gatekeeper Protocol). In 2004, they extended the duration of employer-provided sick pay (from one to two years) and applied employer mandates for rehabilitation and accommodation to this full period. Only at the conclusion of this two-year period do employees become eligible to apply for DI benefits. In 2006, the Dutch government enacted new incentives and penalties for workers with partial disabilities, aimed at inducing them to remain in, or return to, employment. Appendix 1 provides a chronology of the main policy changes in Dutch disability insurance.
Proponents of restructuring the U.S. DI program along the lines of the Dutch paradigm call for requiring workers with health problems to undergo rehabilitation and make efforts to return to work before applying for DI benefits.[5] Some suggest as well experience-rating employer DI contributions so that individual firms shoulder the benefit costs of their own employees more directly and thus have stronger incentives to keep them at work.[6]
This discussion explores the feasibility of these proposals. Part I looks at the factors that caused Dutch spending to rise. Part II provides additional details on the policy changes that the Dutch adopted to reverse this expansion, and Part III examines available evidence on the actual impact of these changes (as distinct from their goals). Part IV looks at recurrent mentions of the Dutch reforms in the U.S. media and policy discourse, comparing them with actual Dutch performance in the post-reform period. The final section draws on the preceding ones to assess the relevance of the Dutch reforms for the United States.
The analysis finds much that is positive about the Dutch disability insurance system, including more adequate benefits and stronger support for rehabilitation, provided sooner with respect to the onset of illness or disability than typically occurs in the United States. At the same time, the paper identifies three problematic aspects of the Dutch reforms that typically do not surface in current U.S. political discourse. These include: (1) increased employer reluctance to hire workers with health problems; (2) increased unemployment among people with disabilities; and (3) an increase in temporary employment, coupled with higher rates of sickness and disability among these workers. The paper also identifies differences between the Dutch and U.S. DI systems that would make U.S. adoption of certain features of the former costly, unworkable, or unattractive. These include, among others, different drivers of program growth, different initial conditions for reform, and different attitudes toward the use of employer mandates to achieve broad social objectives.
In 1967, the Dutch government established a new program of disability insurance by merging two existing schemes, one for occupational disease and injury and a second for disability whose cause is unrelated to work. The merger incorporated many features of the preexisting occupational disease and injury scheme that were, as is typical worldwide, more generous than disability insurance for the workforce at large. As a result, all Dutch workers acquired insured status from the first day of employment, with no prior contribution requirement or waiting period. The new program provided partial, temporary, and full disability benefits, including compensation for as little as 15 percent loss of earnings capacity. Benefit levels were high, replacing 80 percent of wages for full disability. Eligibility criteria were defined broadly and included a range of subjective symptoms.[7]
From the new program’s early days, the doctors who made eligibility determinations relied less on medical evidence and more heavily on workers’ own reports of their health.[8] Furthermore, as a result of court decisions, it soon became administrative practice to certify unemployed, partially disabled persons as fully disabled.[9] This made it unnecessary to assess lost earnings capacity beyond the minimum 15 percent, at which point a worker was entitled to full benefits.
A reliable pathway to a disability pension was provided by a national program covering short-term work incapacity, or sickness insurance. These benefits were available to Dutch workers from the first day of an illness, and eligibility could continue for one year. Sickness benefits replaced 80 percent of lost wages, but employer supplements negotiated in collective agreements boosted the replacement rate to 100 percent for most workers.[10] Workers who remained on sickness benefits for a full year were transferred to disability pensions without rigorous reassessment.[11]
Unsurprisingly, the combination of generous benefits and easy access fueled rapid program expansion. With encouragement from employers, many older workers took advantage of this pathway to early de facto retirement. Similarly, many workers in public jobs with low pay and high stress (e.g., health care and education) sought and obtained disability benefits.[12] Between the introduction of the new program in 1967 and 1980, disability insurance recipients as a percentage of the population age 20-64 increased from about 3.5 percent to over 8 percent.[13] Program spending approached 4 percent of GDP in 1980, more than triple the OECD average (1.1 percent) and more than six times the U.S. level (0.6 percent) at the time.[14] These trends made the Netherlands an international outlier on disability expenditures and earned it the title, “the sick man of Europe.”
The Dutch reached their current disability scheme following a policy path with many twists and turns. Starting in the early 1980s, the Dutch took a variety of approaches to cost reduction and made several mid-course corrections when expected savings did not materialize. The early efforts (1982-1985) included new restrictions on eligibility and modestly reduced benefits. By the early 1990s, it was clear that these measures had achieved only brief successes in reducing costs. Following a consensus reached with trade unions and employer associations, the government adopted more radical reforms. It shifted to individual employers the full cost of sick pay and a portion of the cost of disability pensions. In a subsequent round of reforms beginning in the early 2000s, it required employers to retain sick workers for two years and follow a detailed regulatory regime to rehabilitate them and provide workplace accommodations. In 2006, it created provisions — rewards and penalties — to encourage beneficiaries with partial impairments to continue working. (See Appendix 1.) As a result, today the Dutch disability and sickness programs differ from their predecessors in terms of (1) benefits and eligibility, (2) financing, and (3) employer mandates to rehabilitate sick workers and keep them in employment.
Benefits and Eligibility
Whereas earlier, public sickness benefits replaced 80 percent of wages (100 percent with employer supplements), today they replace 70 percent (with employer supplements, they average 85 percent per year over two years).[15]
Whereas earlier, eligibility for a disability pension was virtually automatic after one year of sickness benefits, today eligibility is only possible after two years. During these two years, each firm must finance the costs of its workers’ sickness benefits and rehabilitation (see below). In addition, each worker receiving a sickness benefit must participate in an employer-financed rehabilitation program.
Whereas earlier, not only fully disabled workers but also those with a loss of earnings capacity of just 15 percent received benefits equaling 80 percent of prior wages, today:
- Workers with a full permanent disability receive benefits that replace 75 percent of wages.[16]
- Workers with a full temporary disability receive 70 percent of prior wages.
- Workers with a partial disability (redefined upwards as capacity loss of 35-79 percent) receive 70 percent of the difference between previous and current wages.[17] According to this formula, for each euro earned a partially disabled worker loses €0.70 in benefits.
If the partially disabled do not earn at a rate equal to at least half their remaining capacity, their benefits are eventually cut.[18] This reduction is achieved by substituting the minimum wage for the worker’s previous wage in the benefit formula.
Whereas earlier, disability determinations took account of the actual availability of particular jobs similar to the claimant’s past employment, such considerations no longer apply in today’s award decisions. Certification for disability no longer takes into account the absence of common skills such as command of the Dutch language or basic use of a computer.[19] Workers under age 45 who were already drawing a pension were subject to recertification (during 2004-2009) under the new eligibility standards. (Appendix 2 describes the procedure whereby the Dutch Social Insurance Institute assesses a claimant’s eligibility.)
Whereas earlier, sickness and disability were financed by collective arrangements that pooled risks and resources across large sectors of the economy, today's employers bear greater individual responsibility. Individual employers must finance the sickness benefit for up to two years, as well as pay experience-rated contributions to finance the first ten years of DI benefits for their employees who become partially or temporarily disabled. (The cost of benefits for the fully and permanently disabled is still financed by a uniform tax that applies to all employers.)
Employers of all sizes, large and small, must shoulder these costs. However, not all employees are covered. For the first five years of a new work contract employer mandates generally exclude employees with disabilities.[20] For these workers, sickness and disability benefits are instead financed collectively and provided by the Dutch Social Insurance Institute. Temporary employees are similarly excluded from individual employer mandates to finance both sickness and disability benefits — like the disabled, temporary workers receive these benefits from the Social Insurance Institute. However, this exclusion will soon be eliminated: Parliament recently took action to make employers responsible, as of 2016, for workers on temporary and flexible contracts. Employers will have to pay for sickness for periods of up to two years, and, through individual experience rating, finance partial and temporary DI pensions.[21] This change is further discussed in Part III.
The employer mandate to finance temporary and partial disability benefits includes an opt-out.[22] Employers may finance their obligations by paying contributions to the public system or, alternatively, via self-financing and the purchase of private insurance. Following what is known as the “polluter pays” principle, public disability contributions are experience rated to reflect the extent of past awards of disability pensions to each employer’s workforce.[23] The private insurance that employers may purchase is even more heavily experience rated.[24]
Employer Mandates: The Gatekeeper Protocol
The preservation of a worker's connection to employment is a key theme in the Dutch reform narrative, and the Gatekeeper Protocol is the pivotal instrument in this design. (See Box 1, “The Gatekeeper Protocol.”) In order to promote sick employees’ return to work, the protocol requires employers to monitor sick leave; hold a sick worker’s job open for two years; develop, finance, and implement plans for rehabilitation; pay for certain medical treatments; make workplace accommodations; and find new jobs for those workers for whom the employer no longer has commensurable employment. In performing some of the required tasks, employers must contract with private companies for assistance.
The Gatekeeper Protocol was adopted to reduce state costs of sick leave and to stem the conversion of sick workers to disability status. It requires employers to contract for the provision of a set of prescribed occupational health services, including risk assessment, socio-medical guidance on rehabilitation of sick employees, and voluntary periodic psycho-social examinations. Employers must engage a company doctor who evaluates sickness reports and refers workers to other medical specialists as the doctor considers needed. If the company doctor recommends treatment that is not covered by national health insurance — e.g., treatment for chronic back pain or psychological problems, or mediation of conflicts — the employer must cover the cost.
Employers must also provide via a private health agency rehabilitation and accommodation for sick employees that includes:
- an initial assessment and prognosis (at six weeks);
- a vocational plan for return to work (at eight weeks);
- appointment of a case manager;
- an evaluation with detailed plans for the rehabilitation in the second year of illness (at 12 months);
- a reintegration report that summarizes efforts and reasons for failure (toward the end of the second year).
The rehabilitation plan is binding on both the employer and employee and is enforceable in court. Employers who cannot accommodate employees must contract with a private agency to attempt to find them other work.
If an employer fails to adhere to the Gatekeeper Protocol, the national Social Insurance Institute can reject its workers' disability pension applications and require the employer to continue to finance sickness benefits for as much as one year beyond the two-year mandate.
Source: Ilene Zeitzer, “The Challenges of Disability Pension Policy: Three Western European Case Studies of the Battle Against the Numbers,” in Elaine Fultz, ed., Reforming Worker Protections: Disability Pensions in Transformation (Budapest: International Labor Organization, 2002), p. 240.
III. Expectations and Experience
The sequence of reforms just described was eventually effective in reducing Dutch sickness and disability spending.[25] Between 1980 and 2011, spending declined by more than half in relation to GDP: sickness benefits fell from 2.6 percent to 1.1 percent, and disability pensions fell from 3.9 percent to 1.8 percent. (See Table 1.) These reductions reflect a 25 percent decline in the rate of short-term work absence, a remarkable decline of over 60 percent in new disability awards, and a 25 percent decline in total disability insurance caseloads (see Table 2).[26] Employment rates among older workers also increased, suggesting that the path to early retirement via disability became less used.[27]
| TABLE 1 |
|---|
| |
1980 |
1985 |
1990 |
1995 |
2000 |
2005 |
2009 |
2010 |
2011 |
|---|
| Disability pensions |
3.9 |
3.6 |
4.2 |
3.3 |
2.5 |
2.1 |
1.9 |
1.9 |
1.8 |
| Sickness benefits and mandated paid sick leave |
2.6 |
1.9 |
2.2 |
1.5 |
1.2 |
1.2 |
0.8 |
1.0 |
1.1 |
However, cost reduction was not the only impact of the Dutch reforms, and several other developments in the post-reform period match reform objectives less well. Three of these stand out as particularly relevant for U.S. observers seeking to draw lessons from Dutch experience: (1) the limited impact of new work incentives and supports for DI recipients; (2) rising unemployment rates among disabled workers; and (3) a major expansion of the temporary workforce together with higher-than-average rates of sickness and disability among such workers.
The limited impact of new work incentives and supports. While a comprehensive analysis of the Dutch work incentives for the partially disabled has yet to be completed, there are several indications that their impact is limited. First, the fraction of DI beneficiaries who are subject to these work incentives is small. An explanatory note that accompanied legislation creating the program for non-permanent and partially disabled workers, effective in 2006, predicted that just 14 percent of new beneficiaries would be classified as having full, non-permanent disabilities and thus not required to work.[28] Contrary to expectations, the fraction so classified ranges from 53-70 percent of new benefit awards each year.[29] The fraction of new program awards, therefore, that could be classified as partially disabled, and thus subject to the work incentives and penalties, turned out to be correspondingly smaller. In reality, only about one quarter of those awarded disability benefits since 2006 have been found partially disabled.[30]
| TABLE 2 |
|---|
| Year |
DI program caseload |
|---|
| 1970 |
200,000 |
| 1980 |
510,000 |
| 1990 |
680,000 |
| 1993 |
750,000 |
| 1997 |
700,000 |
| 2000 |
740,000 |
| 2002 |
800,000 |
| 2005 |
700,000 |
| 2010 |
600,000 |
| 2040 (projection) |
370,000 |
Second, and equally at odds with the Dutch reform narrative, is a low level of effort to rehabilitate workers with full, non-permanent disabilities. While the national Social Insurance Institute can require all beneficiaries with potential for rehabilitation to participate in a reintegration program, in practice it does so in only 10-15 percent of cases.[31] The combined effect of fewer-than-expected DI beneficiaries subject to work incentives on the one hand and low rates of effort to rehabilitate the much larger group of fully but non-permanently disabled on the other means that about two-thirds of those awarded benefits under the reformed Dutch disability program are neither subject to work incentives nor placed in a rehabilitation program.
Third, even when financial work incentives apply, they are weak. The Dutch work supplement for the partially disabled imposes a €0.70 benefit reduction for each euro earned. This steep tax rate is more a penalty than a work incentive. In many cases, collective agreements provide supplemental benefits that offset the cut in public benefits for those who do not work.[32] The procedure for determining the level of partial disability and, as a consequence, how much a partially disabled worker is required to earn is complex (see Appendix 2), and reportedly difficult for even highly educated beneficiaries to understand.[33]
Finally, the long waiting period for DI, during which Dutch workers receive sickness benefits, means that when a worker is finally awarded a DI benefit, his or her work skills and readiness to return to work are likely to have eroded. Noting this phenomenon, Koning and Lindeboom point to similarities between the challenges of encouraging return to work in the Netherlands’ partial disability program and those encountered under the U.S. Ticket to Work program.[34]
Declining employment among people with disabilities. While the Dutch reforms have made employer-provided rehabilitation more widely available for sick workers, they have not boosted employment rates for people with disabilities.[35] On the contrary, whereas in 2000 approximately 50 percent of the disabled were employed, in 2014 just one in three worked 12 hours per week or more.[36] Unemployment among the disabled, meanwhile, rose from about 5 percent in 2001 to 16 percent in 2013 (while unemployment among the non-disabled rose from 3.5 percent to 7.6 percent).[37] While there is no direct proof, some analysts hypothesize a link between these losses and employers’ reluctance to hire people with health impairments, given the employers’ individual liability for financing their employees’ sickness and disability benefits.[38]
Problems associated with temporary employment. In past years, employer efforts to circumvent their individual liability for sickness benefits, rehabilitation, and experience-rated DI benefits have fueled a significant increase in temporary labor contracts.[39] (As described previously, benefits for these workers are financed collectively by employers and provided by the Social Insurance Institute.)
In recent years, these temporary workers have been awarded sickness and disability benefits in disproportionate numbers.[40] This increase cannot be explained solely by the increase in temporary employment, which is smaller than the increase in disability awards.[41] It suggests rather that individual employer liability for sickness, rehabilitation, and disability has made employers reluctant to hire workers with health problems on regular contracts. As a result, such workers have become concentrated in temporary jobs.
In an effort to stem the escalating sickness and disability costs associated with temporary employment, the Dutch Parliament voted to eliminate the exclusion of these jobs from individual employer mandates for sickness benefits and experience rating of disability contributions, effective in 2016.[42] It seems likely that this approach will discourage employers from substituting temporary for permanent workers, but it is less clear whether employers will be able to influence sickness and disability rates in a population with a disproportionate share of health problems.
Moreover, Parliament’s action has evoked protests by employers, who argue that their sickness and disability-related costs are excessive. These complaints are fueling a debate in which the Netherlands’ heavy reliance on employers to achieve broad social objectives is coming under increasing challenge. Dutch policymakers are reportedly considering how to redesign incentives to curb sickness and disability in ways that are less costly for employers. Reviewing these developments, Koning and Lindeboom note: “This pattern raises concerns about the success of experience rating, as well as the notion that employers should play a key role in a program for the well-being of workers.”[43]
U.S. advocates of the Dutch model tend to emphasize its objectives. This focus has sometimes overshadowed information on results achieved during implementation, leading to a skewed picture of the Dutch reforms in U.S. political discourse. One of the most common claims is that the Dutch reforms have made work rather than cash benefits the dominant expectation and form of support for people with disabilities. Such radical transformation was indeed a reform objective, but, with two-thirds of new beneficiaries neither encouraged financially to return to work nor supported with a rehabilitation program, it is clear that this goal has not yet been achieved.
| TABLE 3 |
|---|
| |
1980 |
1985 |
1990 |
1995 |
2000 |
2005 |
2009 |
2010 |
2011 |
|---|
| Netherlands |
3.9 |
3.6 |
4.2 |
3.3 |
2.5 |
2.1 |
1.9 |
1.9 |
1.8 |
| OECD |
1.1 |
1.1 |
1.2 |
1.2 |
1.1 |
1.1 |
1.2 |
1.1 |
1.1 |
| U.S. |
0.6 |
0.4 |
0.4 |
0.5 |
0.5 |
0.7 |
0.8 |
0.8 |
0.8 |
A second such claim is that Dutch expenditure reductions result primarily from “changing the signals” so that employers bear sickness and disability program costs more directly. However, the Gatekeeper Protocol imposes direct requirements on employers — legal mandates, not economic “signals.” Quantitative analyses of reform impacts show that the Gatekeeper Protocol accounts for nearly twice the reduction in new benefit awards as the employer incentives resulting from experience rating.[44] Moreover, Philip de Jong, often acknowledged as the conceptual father of the Dutch reforms, attributes the substantial increase in employer efforts to retain incapacitated workers to the detailed regulations in the Gatekeeper Protocol; he calls this a major lesson of the Dutch experience.[45] Yet the key role of employer regulation in the Dutch reforms is a lesson that is largely passed over in U.S. discourse.
Box 2: Netherlands’ Efficiency in Targeting Disability Pensions to the Least Healthy Applicants
A recent comparison of ten European Union countries and the United States explored the efficiency of government disability programs in screening applicants so as to avoid Type 1 error — providing benefits to healthy recipients — and Type II error — denying benefits to unhealthy applicants.
The results showed that the Dutch do not restrict benefits to the most disabled to the same extent as does the United States. In the United States, just 23 percent of those drawing DI fall above the bottom health quintile in the country, whereas in the Netherlands, 43 percent do.
Among the 11 countries in the comparison, the United States had by far the highest percentage of beneficiaries in the lowest health quintile. The United States was one of only four countries whose percentage exceeded 60 percent and one of just two exceeding 70 percent.
Source: Enrica Croda, Jonathan Skinner, and Laura Yasaitis, “An International Comparison of the Efficiency of Government Disability Programs” (Cambridge, MA: National Bureau of Economic Research, 2013), pp. 1, 29
A third skewed representation of the Dutch experience asserts that the reforms effectively addressed the country’s disability spending problem. This claim is embedded in titles like: “How the New Dutch Model Cured the Dutch Disease.” Spending is indeed lower today than in past years, but it is still quite high by international standards — half again the OECD average and double the U.S. rate (see Table 3 and Figure 2).[46] Furthermore, benefits still replace 70-75 percent of pre-disability wages, and the Dutch continue to be less efficient in targeting pensions to the least healthy applicants compared to the U.S. DI program. (See Box 2, “Netherlands’ Efficiency in Targeting Disability Pensions to the Least Healthy Applicants.”) While government projections suggest that the Dutch reforms will realize further savings in future years, the country is also experiencing a steep rise in disabilities among young people disabled from childhood, primarily due to mental impairments. Projected spending increases in the disability benefit that covers this group fully offset projected DI gains.[47] Together, these figures belie claims that Dutch disability spending is now at levels that would be considered sustainable in the U.S. context.
The preceding pages reveal important advantages of the Dutch model. Workers receive more generous benefits for both sickness and disability than do their American counterparts, as well as far more support from their employers for rehabilitation and continuing work. Moreover, this support is provided sooner after the onset of sickness or disability, which, other things being equal, increases the probability of successful return to work. The Dutch have also persistently redesigned the disability system and achieved impressive savings. However, as shown, these savings were accompanied by deleterious side effects. Were the Dutch reform strategy implemented in the U.S. context, its results would be far more costly, less workable, and less attractive, as described below.
Notwithstanding their success in reducing DI outlays, the Dutch continue to spend at twice the U.S. rate in relation to GDP. In addition, the fraction of the working-age population receiving DI benefits is 50 percent higher.[48] Given these large differences, it is difficult to view the Netherlands as providing a blueprint for U.S. cost containment.
In addition, Dutch DI program expansion was driven by generous benefits and easy access and was therefore more easily reversed than in the United States. Caseloads in the Netherlands rose sharply after the 1967 reform that combined two programs and took the most generous features of each. These features included universal coverage of the workforce, high rates of wage replacement, broad eligibility criteria, and benefits for full, partial, and temporary disability. In the United States, by contrast, DI program growth is attributable largely to demographic changes.[49]
From an American perspective, the Dutch had ample room both to cut benefits and to restrict eligibility. On the one hand, wage replacement rates of 80 percent in the pre-reform period provided greater margin for cutting benefits. On the other, the Netherlands’ expansive definition of disability provided leeway to restrict the DI caseload to those with substantial losses of earnings capacity. Even in the post-reform period, eligibility standards are among the least stringent among a group of ten EU countries and the United States.
In the United States, by contrast, the average DI wage replacement rate is just 50-55 percent.[50] As for eligibility, according to the OECD, the United States is among the handful of countries with “the most stringent eligibility criteria for a full disability benefit, including the most rigid reference to all jobs available in the labor market.”[51]
Unlike the Netherlands, the United States lacks the space to reduce benefits or tighten eligibility without harming beneficiaries, the great majority of whom cannot return to work.
The Dutch caseload includes a large fraction of beneficiaries for whom efforts at rehabilitation and return to work are more likely to be successful. Since prior to reform the Dutch awarded benefits to workers with as little as a 15 percent loss of earnings capacity, Dutch DI caseloads were a fertile area for rehabilitation. Even in the post-reform period, the Dutch DI rolls include individuals with as little as 35 percent loss in earnings capacity.
With a stricter definition of disability and a more impaired caseload, the United States has a considerably smaller fraction of DI-eligible workers for whom rehabilitation can reasonably be expected to result in return to work.
The Gatekeeper Protocol imposes detailed and costly regulation on employers. It requires employers to hold a sick worker’s job open for two years while paying sickness benefits of at least 70 percent of prior wages. Employers must also implement and finance rehabilitation, cover certain forms of medical care, make workplace accommodations, find a new job for workers for whom they can no longer offer comparable employment, and prepare detailed reports of all such efforts.
Heavy employer regulation is not an add-on but the centerpiece of the Dutch redesign of DI. This approach was possible in the Netherlands because of strong trade unions, a shared commitment to social partnership, precedents for enrolling employers in efforts to achieve social goals, and a tradition of compromise. In the United States, by contrast, such heavy regulation of employers would be at odds with prevailing norms and practice. Even in the Netherlands, it is coming under increasing challenge.
This shift of sickness and disability costs to individual employers has serious, unwanted side effects. These include: (1) increased employer aversion to hiring workers with health problems, (2) increased temporary employment, (3) disproportionate rates of sickness and disability among those with temporary contracts, and (4) increased use of employment agencies as a way to dodge the sickness and disability costs of direct hires.
The 70 percent Dutch tax on earnings by workers with partial disabilities compares unfavorably to the 50 percent tax under the SSI section 1619 program and a zero loss for the first $1,090 of earnings per month under SSDI. Additional U.S. work incentives — e.g., the Trial Work Period, Extended Period of Eligibility, and the Ticket to Work[52] — have no counterparts in the Dutch DI program.
All said, Dutch efforts to reduce DI expenditures were multifaceted, determined, and impressive. The Dutch drove expenditures down by reducing benefits and restricting eligibility, shifting sickness financing to employers, extending sickness benefit duration, experience rating a portion of DI contributions for individual employers, and requiring employers to rehabilitate and accommodate their own employees. The results include not only large DI cost reductions but also negative side effects. In the wake of Dutch DI restructuring, people with disabilities have greater difficulty finding work, and temporary employment is more widespread. While the Dutch are no longer an international outlier on DI spending, they are still at the upper end of the continuum. Dutch employers’ objections to the costs that have been shifted to them are increasingly sharp. With these outcomes, it is difficult to see the Netherlands as a model for DI cost cutting in the United States.
These mixed results do not, however, call into question the usefulness of early intervention. Given the disappointing results of U.S. efforts to rehabilitate people with disabilities after they join the DI rolls, new approaches to early intervention merit more focused investigation, consideration, and support. What is needed is homegrown analysis of how to target such supports cost-effectively in a context in which the DI-eligible population is a small subset of all persons with disabilities. Such targeting constitutes a major challenge. The Netherlands provides a thought-provoking experience but not a blueprint for U.S. action.
I gratefully acknowledge useful feedback on early drafts of this paper from Paul Van de Water and Kathy Ruffing of the Center on Budget and Policy Priorities, Ilene Zeitzer of Disability Policy Solutions, Anneke van der Giezen of the Dutch Ministry of Social Affairs and Employment, and John Francis of JMF Research Associates. In addition, Philip de Jong of APE and Carla van Deursen of the Dutch Social Insurance Institute provided useful information in personal correspondence. Patrick Watson edited the paper with a high level of attention and care. Any errors are, of course, entirely my own responsibility.
Elaine Fultz is an independent consultant. She has served as a professional staff member of the House Committee on Ways and Means, Subcommittee on Social Security, and as an official of the International Labor Organization, Social Security Department.
| TABLE 1 |
|---|
| Year |
Government Action |
|---|
| 1982-85 |
Reduction in real pension benefit levels through:
- abolition of tax exemptions,
- reduction of earnings base used for benefit calculation
- reduction in wage replacement rate, from 80 percent to 70 percent.
Consideration of labor market opportunities barred in benefit decisions. |
| 1992 |
Penalty for firms whose employees are awarded disability benefits. Bonus for hiring partly disabled workers (both subsequently repealed). Residual functional capacity (RFC) definition broadened to include earnings from any job commensurate with worker’s RFC. Eligibility of those under age 45 reviewed under stricter standard. |
| 1993 |
Lower replacement rate for long-term disabled. |
| 1996 |
Employers made responsible for providing first year of sickness benefits. |
| 1998 |
Introduction of experience rating on employer disability contributions. |
| 2002 |
Regulation of employer efforts to rehabilitate employees, through Gatekeeper Improvement Act. |
| 2003 |
Incentives for hiring of workers with disabilities
- Government pays any sick pay for five years,
- Employers exempted from experience rating on these employees.
Employers must hire private reintegration firm to find jobs for disabled workers for whom they have no commensurate work. |
| 2004 |
Employer responsibility for sickness benefits is increased from one to two years; employers must guarantee worker’s job for this period; and DI eligibility rules are made more stringent.[53] |
| 2006 |
Disability pension scheme split into two parts, one for permanently and totally disabled with a 75 percent replacement rate, and a second for all others. In the latter, those with full non-permanent disabilities receive a 70 percent replacement rate, and partially disabled receive 70 percent of difference between previous and current wage. If the earnings of a partially disabled beneficiary are less than half of residual earning capacity, eventually the benefit is reduced. This is achieved by substituting the minimum wage for the previous wage in the benefit formula. |
A worker who applies for a disability pension is interviewed by a doctor at the Social Insurance Institute. Through personal discussion, the doctor explores the impact of the individual’s physical or mental impairments on his/her work capacities, daily routine, and even hobbies. The doctor may perform a physical examination or consult with the family doctor or treating physician but is not required to do so.
Claimants are found fully disabled if their impairments are terminal or require that they be institutionalized, or if the individual is in steep decline. In addition, claimants may be classified as fully disabled based on labor qualifications if their “theoretical loss of income” is greater than 80 percent.
To determine theoretical loss of income, a labor expert at the Social Insurance Institute decides which professions a claimant can still perform. This involves reliance on a large database in which all the jobs in the Netherlands are described. If there are at least three suitable professions, the Social Insurance Institute takes the middle job and computes the difference between the old and new income. If the loss is more than 80 percent, the person is declared fully disabled. If the loss is less than 35 percent, the claimant is not eligible for a disability pension. Those with a loss between 35 and 80 percent will receive a partial pension whose amount reflects their remaining capacity.
Example: Before he got sick, Ronald earned €2,700 per month as a coach. The labor expert identified several jobs that Ronald can still perform taking into account his health and education: a commercial salesperson (€1,800 per month), a warehouse worker (€1,700), and a call-entry worker (€1,600). The middle wage is €1,700, which is 63 percent of his previous wage. Therefore, Ronald’s degree of disability is 37 percent.
Source: “Work and Income According to the Labor Capacity Act,” Dutch Social Insurance Institute (WIA), May 11, 2015, and personal correspondence with Carla van Deursen, senior advisor, UWV, May 18, 2015.