BEYOND THE NUMBERS
Repealing the Affordable Care Act (ACA) would undo the historic recent gains in children’s health coverage, a new Urban Institute report finds. Some 4.4 million children would lose coverage by 2019 and the children’s uninsured rate, which has fallen from 7 percent to 4.1 percent under the ACA, would jump to 9.6 percent. And these numbers could grow much higher under other possible changes in federal and state policies.
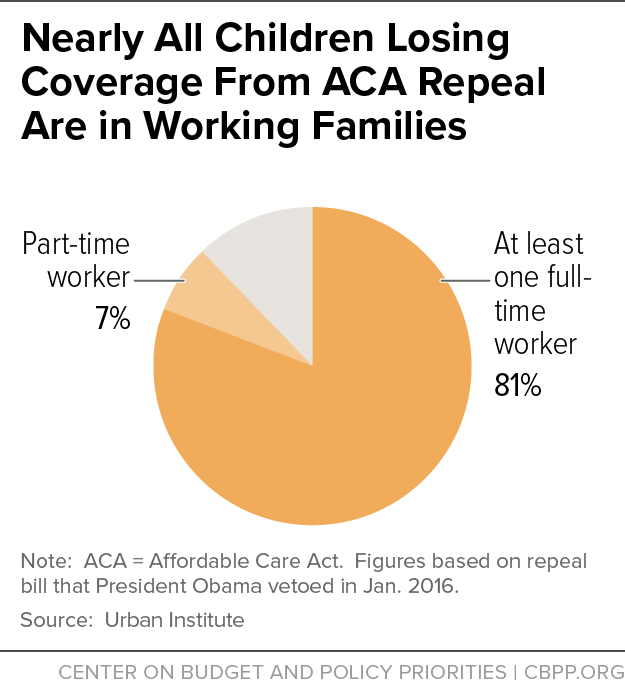
A separate Urban report showed that nearly 30 million people would lose coverage by 2019 from an ACA repeal bill similar to the one President Obama vetoed in January 2016, due to its Medicaid eligibility restrictions, loss of subsidies for marketplace coverage, and the near-collapse of the individual insurance market. This new report shows that 4.4 million of those losing coverage would be ages 18 and under. Roughly 9 in 10 of the children losing coverage would be in families with working parents (see graph).
Almost all children with coverage in the individual market would lose it, largely due to the loss of subsidies that make private insurance more affordable. Many children would also lose Medicaid coverage, even though the repeal bill wouldn’t change children’s Medicaid eligibility, because their parents would lose coverage. Research shows that parents are less likely to enroll their children in coverage if the parents themselves aren’t eligible. The share of parents who are uninsured would more than double under repeal, to nearly 23 percent. Most of the parents losing coverage are in working families.
Even more children would lose coverage if certain other changes take place:
- If federal policymakers don’t extend funding for the Children’s Health Insurance Program (CHIP), which is set to expire in September 2017, states could eliminate their separate CHIP programs. Some 3.7 million children would lose coverage (on top of the 4.4 million noted above), the Urban report estimates.
- If federal policymakers repeal the ACA requirement that states cover all children in families with incomes below 138 percent of the poverty line, plus the ACA’s “maintenance of effort” requirement that states keep their current eligibility limits until 2019, states could roll back Medicaid and CHIP eligibility to 138 percent of poverty for children under age 6 and to 100 percent of poverty for children ages 6 to 18. If all states cut coverage to these minimum levels, 8.9 million children would lose coverage (on top of the 4.4 million noted above). While that’s unlikely, the potential for cuts in children’s coverage would grow if congressional Republicans enact a Medicaid block grant or per capita cap, which would force governors to make large Medicaid cuts in response to large declines in federal funding.
Uninsured children go without needed health care, which not only causes significant stress for families but has serious long-range impacts. Studies show that children who are eligible for Medicaid have better health outcomes and earnings in adulthood, and the benefits grow with each year they’re eligible.