BEYOND THE NUMBERS
Debates over issues like health reform’s Medicaid expansion or proposals to turn Medicaid into a block grant often raise important questions about states’ role in Medicaid. Here are two relevant points from our recent paper.
1. Medicaid gives states significant flexibility to design their own programs — whom they cover, what benefits they provide, and how they deliver health care services.
The federal government sets minimum standards, including the categories of people that all states must cover. Beyond that, states set their own rules. As a result, Medicaid eligibility varies substantially from state to state.
Medicaid benefits vary significantly as well. States decide whether to cover services like dental and vision care for adults and the amount, duration, and scope of the services they provide. States also decide whether Medicaid delivers health care services through managed care, fee-for-service, or other delivery systems and how much to pay providers and plans that serve Medicaid beneficiaries.
Many states take advantage of Medicaid’s flexibility to improve beneficiaries’ health while lowering costs, as we explain in this paper. Wisconsin, for example, adopted an initiative to reduce inappropriate emergency room (ER) use among Medicaid beneficiaries. A provider organization mainly serving Medicaid patients identified frequent ER users, educated them on proper ER use, and made primary care appointments for them. In 2012, the organization reduced ER visits by 44 percent among those who kept their scheduled appointments.
2. Health reform’s Medicaid expansion has not only helped millions of low-income people gain health coverage but also produced state savings.
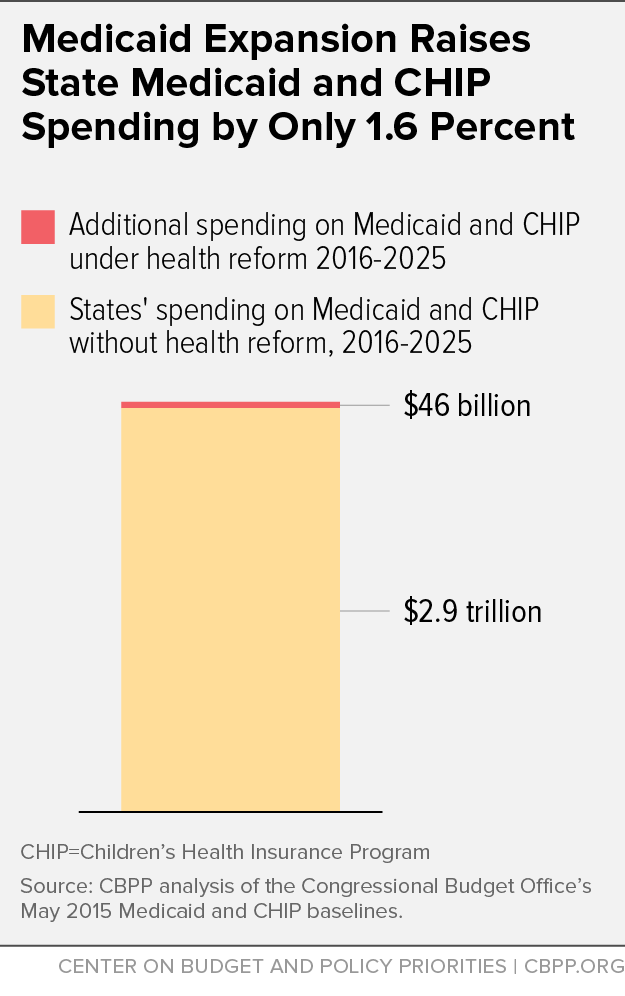
Under health reform, the federal government picks up 100 percent of the expansion’s cost through 2016 and at least 90 percent thereafter. The federal share will average roughly 95 percent from 2016 to 2025, the Congressional Budget Office (CBO) estimates. CBO estimates also show that states will spend just 1.6 percent more on Medicaid and the Children’s Health Insurance Program (CHIP) with the expansion than they would have without health reform, if most states adopt the expansion (see graph).
For many states, the expansion has produced savings. As more low-income uninsured residents gained coverage, demand for entirely state-funded services that serve the uninsured has declined, yielding net savings.
While some critics argue that the federal government will someday renege on its commitment to finance nearly all expansion costs, history shows that’s unlikely. Congress has only modified Medicaid’s overall matching rate three times over the last three and a half decades, and the most recent changes were temporary increases to aid states during the last two economic downturns.
As Medicaid turns 50, learn more about how it improves access to health care, its long-term benefits, and why states should expand Medicaid: www.cbpp.org/medicaid-at-50