BEYOND THE NUMBERS
When Vice President Pence travels to Kentucky this weekend to make the case for House Republicans’ Affordable Care Act (ACA) repeal bill, he’ll presumably echo President Trump’s claim that the ACA is failing in that state. Kentucky’s an odd choice to make that claim: it’s seen the sharpest drop in the adult uninsured rate of any state under the ACA, from more than 20 percent in 2013 to less than 8 percent in 2016.
Some Republicans, including Kentucky Governor Matt Bevin, have suggested these coverage gains don’t count because a large share of them is due to the ACA’s Medicaid expansion. As Bevin argues, “If you have a Medicaid card, but you can’t find a doctor that will see you, how does that Medicaid card help you? … [A] piece of plastic doesn’t make you healthier.”
Fortunately, Kentucky’s Medicaid expansion has been among the most carefully studied of any state. The research shows that the hundreds of thousands of Kentucky (and Arkansas) residents who’ve gained coverage are indeed finding doctors, getting health care, and becoming healthier.
In a study in the Journal of the American Medical Association, researchers compared changes in access to care, financial security, and health outcomes for low-income adults in Kentucky and Arkansas, which expanded Medicaid, with changes over the same period for low-income adults in Texas, which didn’t. They found that expansion led to:
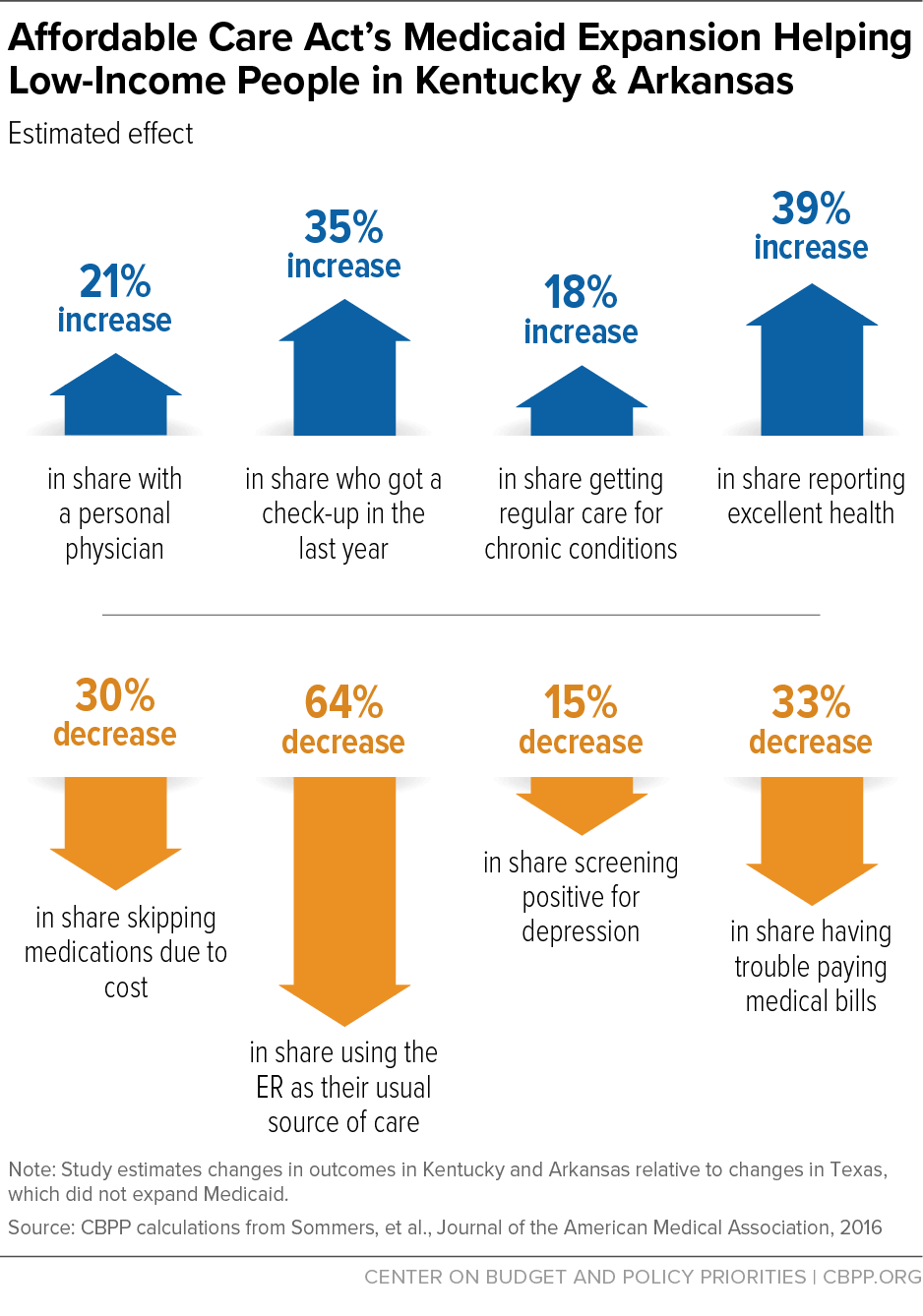
- Improved access to care, including a 21 percent increase in the share of people with a personal physician, a 30 percent drop in the share who had to skip medications due to cost, and a 64 percent drop in the share relying on the emergency room as a usual source of care.
- Improved financial security, including a 33 percent drop in the share of people having trouble paying medical bills.
- Improved health, including a 40 percent increase in the share of people reporting that they’re in excellent health and a 15 percent drop in the share who’ve screened positive for depression.
And gains have risen over time. In particular, improvements in self-reported health were small (and not statistically significant) when measured in 2014, the first year of expansion, but doubled in 2015.
Unfortunately, Kentucky’s Medicaid expansion is doubly at risk. The House Republican ACA repeal bill would effectively end the expansion across the country. And even absent congressional action, Governor Bevin’s proposed Medicaid waiver would, if approved, lead 86,000 Kentuckians to lose coverage after five years, based on the state’s own estimates.