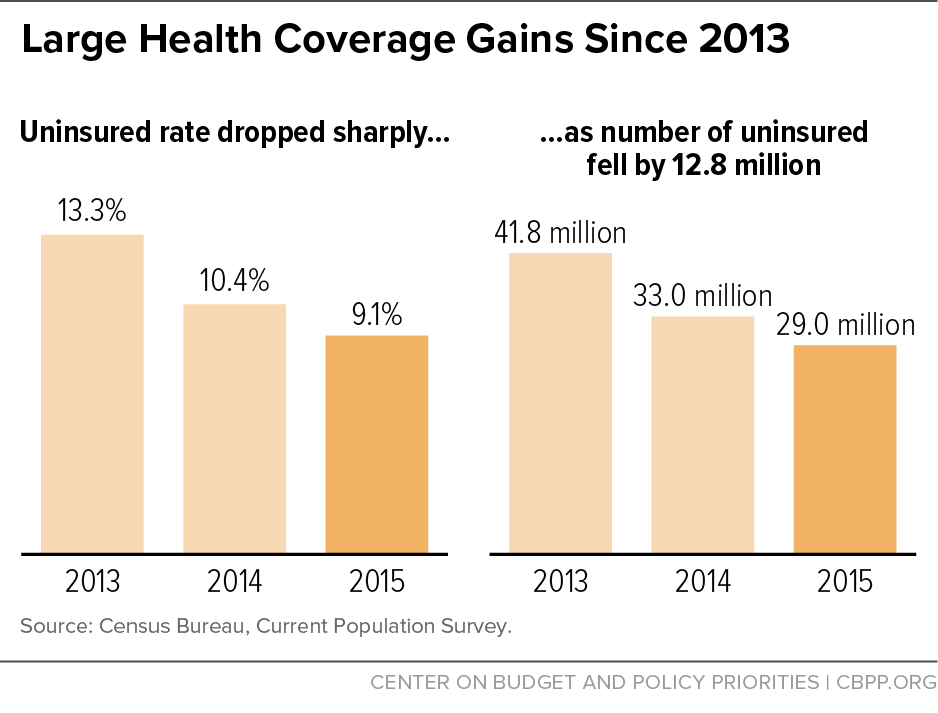
The historic gains in health insurance coverage in 2014 — when the Affordable Care Act’s (ACA) major coverage expansions took effect — continued in 2015, Census Bureau data based on the Current Population Survey (CPS) show.[1] The share of Americans who are uninsured fell from 10.4 percent in 2014 to 9.1 percent in 2015, while the number of people without insurance dropped from 33.0 million to 29.0 million. (See Figure 1.) These improvements follow a 2.9 percentage-point reduction in the uninsured rate and 8.8 million person drop in the number of uninsured in 2014. These are the two largest single-year reductions on record, with data back to 1987.
The new figures capture the continued effect of the ACA’s major coverage expansions and are consistent with the historic coverage gains measured in the Centers for Disease Control and Prevention’s (CDC) National Health Interview Survey (NHIS) and several private surveys. Starting on January 1, 2014, the ACA gave states the option to expand Medicaid to more low-income adults and established subsidies for low- and moderate-income families to buy private coverage through health insurance marketplaces.
The new Census data include estimates from both the CPS and American Community Survey (ACS), which are considered the gold standard for national- and state-level health coverage estimates, respectively. Because the Census Bureau revised the CPS health coverage questions in 2013, only the 2013 through 2015 CPS coverage estimates can be compared directly. But the ACS questions have not changed, so the ACS can be used for comparisons back to 2009. This analysis bases single-year historical comparisons on CPS data and longer-term comparisons on a combination of adjusted CPS data, ACS data, and data from the NHIS.
The new CPS figures also show:
- Private coverage and public coverage rates grew together in 2015 for the second consecutive year and only the second time since 2000. The share of Americans with private coverage rose from 66.0 percent in 2014 to 67.2 percent in 2015, likely reflecting increased enrollment in subsidized marketplace coverage and continued progress in covering young adults, as well as the improving economy. The share with public coverage rose from 36.5 percent in 2014 to 37.1 percent in 2015, reflecting primarily growth in the share of the population enrolled in Medicare, as another cohort of baby boomers aged into Medicare eligibility.
- The uninsured rate fell among virtually every demographic category that the CPS data cover, including categories by gender, family income, working status, and race/ethnicity.[2] Coverage gains were greatest among the groups historically least likely to have coverage. Among adults under age 26, for example, the uninsured rate dropped from 17.1 percent in 2014 to 14.5 percent in 2015; among Latinos, it fell from 19.9 percent to 16.2 percent; among part-time workers, it fell from 18.1 percent to 15.8 percent. People in families under 300 percent of the poverty line and people with only a high school education also experienced large gains (see Appendix Table 1).
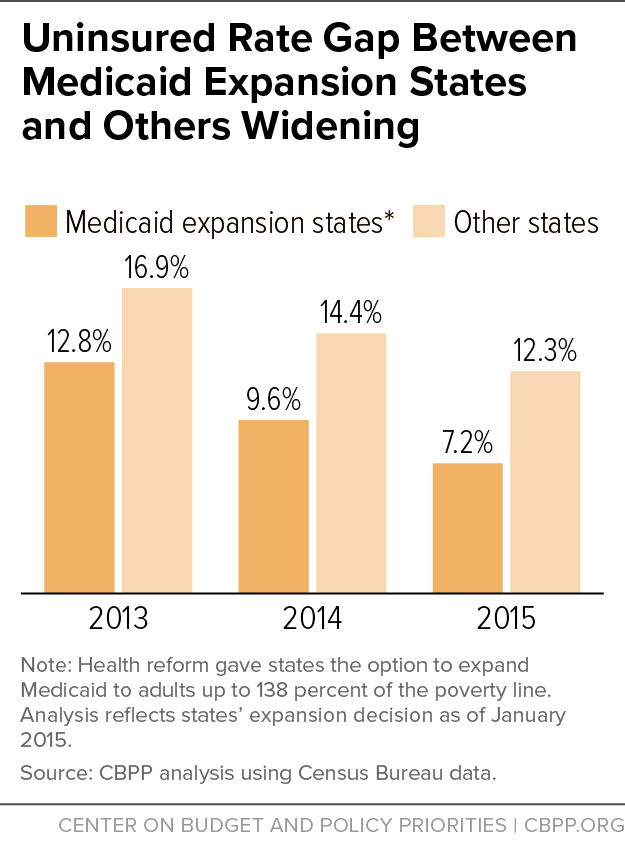
The ACS data show that the uninsured rate in 2015 was 7.2 percent in states that had expanded Medicaid and 12.3 percent in non-expansion states. While states adopting the expansion had lower average uninsured rates than other states before the expansion took effect in January 2014, the coverage gap between expansion and non-expansion states has widened since then, growing from 4.1 percentage points in 2013 to 4.8 percentage points in 2014 and to 5.1 percentage points in 2015. If the uninsured rate had fallen in non-expansion states at the same rate as in expansion states, an additional 3.7 million uninsured Americans would have gained coverage since 2013.
In addition, an array of public and private surveys and data show that the number of Americans without insurance has continued falling in 2016. The number of uninsured fell from nearly 45 million in 2013 to 36.0 million in 2014, 28.6 million in 2015, and 27.3 million in the first quarter of 2016, according to the CDC’s National Health Interview Survey.[3] At 8.6 percent, the CDC’s estimated uninsured rate for the first quarter of 2016 was the lowest since the CDC began collecting these data in 1997, and more than two-fifths below the peak in 2010. Similarly, results from the Urban Institute’s Health Reform Monitoring Survey show the uninsured rate falling from 10.3 percent in March 2015 to 9.9 percent in March 2016.[4]
Although the CPS is the most widely used source of health coverage information, changes in its health coverage questions in 2013 — the result of a multi-year Census initiative to improve the reliability and accuracy of the survey’s health coverage estimates — mean results from 2013 and subsequent years can be compared to one another but not to data for prior years. The CPS estimates remain of substantial value, however, because of the high quality of the CPS’s survey design and the CPS’s wealth of additional information on income and demographics.
For comparisons with earlier years though, the ACS is the preferred data source. This paper uses both ACS and CPS data as appropriate — the ACS data and a modified version of several different CPS-based historical series for comparisons to years before 2013, and the CPS data for comparing coverage rates for 2013 and years after, as well as 2015 coverage rates across population groups.
Analysts had long maintained that the CPS estimate of the number of uninsured is too high for what the survey purportedly measures — the number uninsured for the entire calendar year. The revised CPS survey questions, which ask separately about coverage at the time of the interview and coverage transitions over the course of the previous year, are designed to generate more reliable estimates. These changes have strengthened the CPS’ ability to accurately measure the effects of recent changes in health care coverage sources, such as the availability of subsidies to purchase marketplace coverage under the Affordable Care Act. The Census Bureau believes that the 2013 CPS data on health coverage provide an improved baseline to accurately measure the effects of the 2014 ACA coverage expansions.
The 2015 health coverage gains build upon the historic progress in 2014, as well as much smaller but steady gains since 2010. The ACS data show that the uninsured rate declined for the fifth consecutive year in 2015, from 15.5 percent in 2010 to 9.1 percent in 2015. (The ACS estimates of the overall uninsured rate are modestly higher than the CPS estimates, as they reflect whether an individual was uninsured at the time of the interview while the CPS estimates reflect whether an individual was uninsured for the entire year.)
The improvement prior to 2014 likely reflects, in substantial part, ACA provisions permitting young adults to get coverage through their parents’ health insurance up to age 26 and barring states from scaling back Medicaid or CHIP eligibility or making it harder for eligible individuals (including children) to enroll, as well as continued progress in a number of states in reaching more eligible children through Medicaid and CHIP.
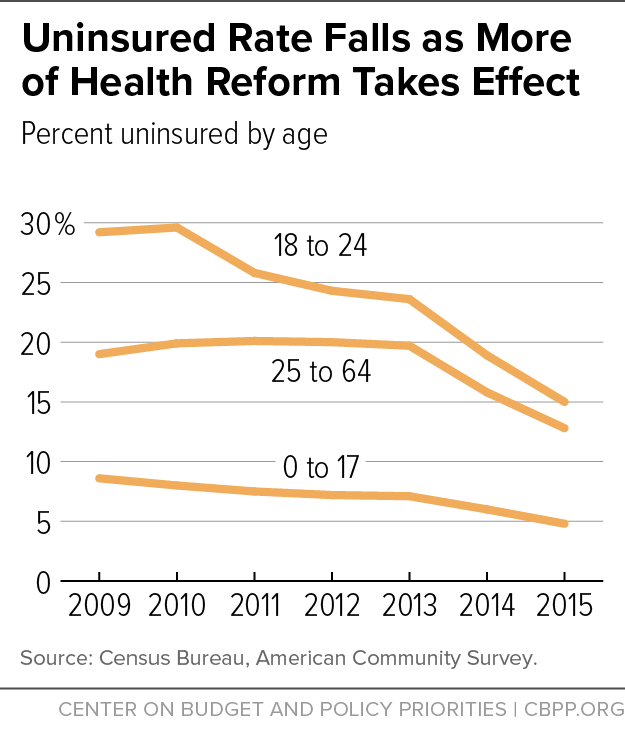
Among adults under age 26, the uninsured rate fell from 29.6 percent in 2010 to 23.6 percent in 2013, 18.9 percent in 2014, and 15.0 percent in 2015, the ACS data show. Among children, the uninsured rate fell from 8.6 percent in 2009 to 7.1 percent in 2013, 6.0 percent in 2014, and 4.8 percent in 2015.
The nation has also made major progress in extending coverage to other non-elderly adults. Some 12.8 percent of adults aged 26-64 were uninsured in 2015, down from 15.8 percent in 2014 and 19.7 percent in 2013, according to the ACS. Coverage rates for this group stagnated between 2010 and 2013; the coverage gains starting in 2014 reflect the ACA’s major coverage expansions.
For all three age groups — children through age 17, people aged 18 to 24, and adults aged 25 to 64 — the 2015 uninsured rate is a historic low. (See Figure 2.)
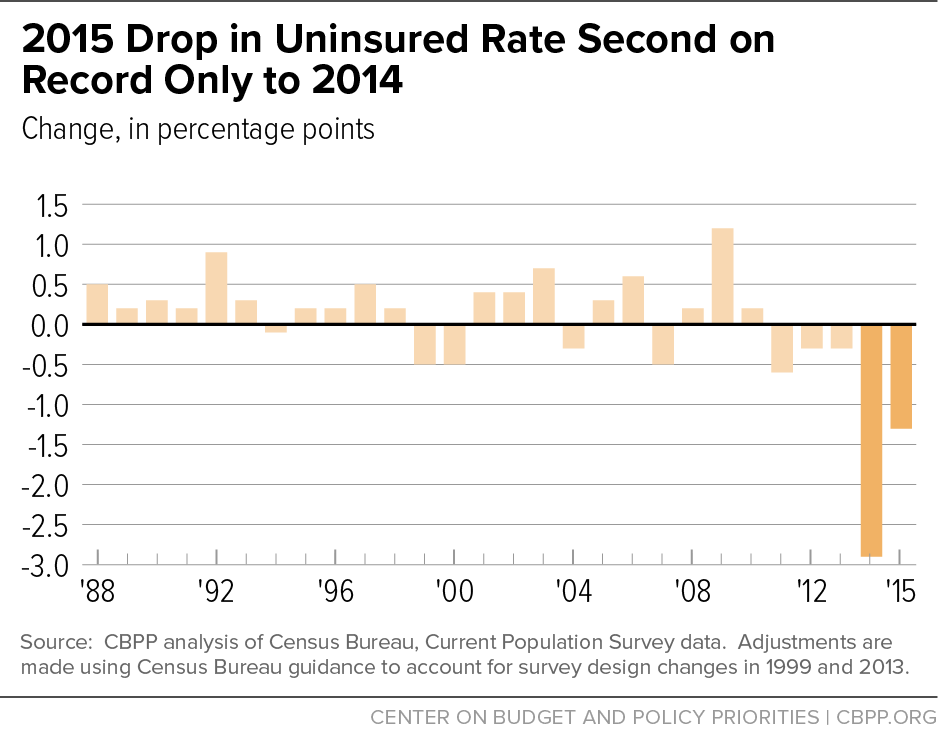
Although the adoption of new CPS questions for 2013 means that the uninsured rates for 2013 and beyond cannot be directly compared with the rates for previous years, the changes in the uninsured rate in 2014 and 2015 can be compared with other single-year changes within earlier CPS historical series (each of which contains consistent, comparable data) dating back to 1987, when the CPS health insurance data were first collected.[5] Under this analysis, the decline in the uninsured rate of 2.9 percentage points (or more than one-fifth) in 2014 is by far the largest single-year reduction on record and is several times greater than any previous single-year decline. The 2015 decline of 1.3 percentage points is the second largest single-year decline on record. (See Figure 3.)
Data from other government and private surveys that did not change their survey methods also confirm that the 2015 uninsured rate was lower than in any other year for which these surveys collected data.
- Under the CDC’s National Health Interview Survey, which has used the same questions since 1997, 2015’s uninsured rate of 9.1 percent is the lowest on record and is one-fifth below the previous low (11.5 percent in 2014).[6]
- Similarly, the ACS and Gallup’s Well-Being Index[7] show the 2015 uninsured rate to be lower than in any year since those surveys first were conducted in 2008.
The share of Americans with private coverage grew from 66.0 percent in 2014 to 67.2 percent in 2015, according to CPS data. This builds off of the 2014 increase, which was the first such increase since 2000. The percentage of Americans with private coverage fell by more than one-seventh between 2000 and 2013.[8]
The growth in private coverage was driven almost entirely by an increase in coverage that individuals purchased themselves, as the share of Americans with private coverage who didn’t receive it through their employer rose from 14.6 percent in 2014 to 16.3 percent in 2015, an increase of 5.9 million people. The overwhelming share of this increase is likely due to enrollment in health reform’s insurance marketplaces. The large majority of those enrolled in marketplace coverage received premium subsidies and cost-sharing assistance to help make marketplace coverage affordable for low- and moderate-income people.[9]
Some 55.7 percent of Americans had employer-sponsored coverage in 2015, statistically unchanged from 2014. The share of workers with employer-sponsored coverage remained stable as well. This counters claims that health reform would lead to substantial reductions in employer-based coverage.[10]
The share of Americans covered by programs like Medicare, Medicaid, and CHIP rose from 36.5 percent in 2014 to 37.1 percent in 2015, according to CPS data. Enrollment in public health programs has grown each year since 2009, according to ACS data first collected in 2008,[11] but the annual increase has been more than one-fourth greater since health reform’s Medicaid expansion took effect.
Since 2013, the share of adults below the poverty line enrolled in Medicaid has increased from 36.5 percent to 40.5 percent.[12] This is primarily due to state take-up of the ACA’s Medicaid expansion. Medicaid and CHIP also continue to play a significant coverage role for children: 76.7 percent of poor children were enrolled in Medicaid or CHIP in 2015.
For the fourth consecutive year, Medicare enrollment rose significantly in 2015 (by 1.3 million people), as the share of the population aged 65 or older reached another historic high.
Some 12.3 percent of people in the 23 states that did not implement the ACA’s Medicaid expansion were uninsured in 2015, compared to 7.2 percent of people in the 28 states (including the District of Columbia) that had expanded Medicaid by January 1, 2015.[13] The uninsured rate fell in both groups of states but fell more in expansion states, widening the gap between the two groups of states to 5.1 percentage points in 2015. (See Figure 4.) The CDC, Urban Institute, and Gallup also have all found evidence of this growing divide.
Certain Groups Remain Disproportionately Uninsured
Despite broad coverage gains throughout the population in 2015, certain groups remain uninsured at disproportionately high rates, the CPS data show.
- 26- to 34-year-olds. Some 16.3 percent of 26- to 34-year-olds were uninsured in 2015, a decline of 1.9 percentage points from 2014 but still the highest among all age cohorts. Adults under age 26 were the age cohort with the highest uninsured rate until 2013, but they have also benefited from the ACA provision allowing children to remain on their parents’ plans until age 26.
- Hispanics. Some 16.2 percent of Hispanics were uninsured in 2015, compared to 11.1 percent of African Americans, 7.5 percent of Asian Americans, and 6.7 percent of non-Hispanic whites. This disparity continued to narrow somewhat in 2015.
- Residents of the South and West. Some 12.0 percent of those living in the South and 8.5 percent of those living in the West were uninsured in 2015, well above the comparable figures for the Northeast (6.1 percent) and Midwest (6.9 percent). Since 2013, however, the uninsured rate has declined in the West more than one and a half times more than in the South.
- Unemployed or underemployed. Some 15.8 percent of both those who were unemployed for at least one week in 2015, and those who worked less than full time, were uninsured, well above the 9.9 percent uninsured rate for people who had a full-time job throughout the year. This disparity has narrowed somewhat since 2013 as more of the unemployed or underemployed gained access to affordable coverage through the ACA’s insurance marketplaces and Medicaid.
- People in low-income households. The uninsured rate was more than twice as high among people in households with incomes below $50,000 (13.5 percent) as among people in households with incomes of $50,000 or more (6.5 percent). Nevertheless, this disparity, as well, narrowed further in 2015 due to the Medicaid expansion and marketplace subsidies, both of which are targeted to people with low or modest incomes. The uninsured rate among households with incomes below $50,000 declined from 19.9 percent in 2013 and 15.2 percent in 2014.
The CDC issued preliminary data from its National Health Interview Survey earlier this year showing that the ranks of the uninsured fell in the first quarter of 2016 by another 0.7 million people (or 0.5 percentage points).[14] The CDC estimates that the uninsured rate fell from 9.1 percent in 2015 to 8.6 percent in the first quarter of 2016 — the lowest since the CDC began collecting these data in 1997 and more than two-fifths below the peak of 16.0 percent in 2010.
These CDC figures are consistent with two independent private surveys showing coverage gains for adults in 2016. (One study examined non-elderly adults; the second examined all adults.) All three surveys also indicate that the Medicaid expansion and subsidized marketplace coverage are driving these large reductions in the ranks of the uninsured.
- Data from the Urban Institute’s Health Reform Monitoring Survey show the uninsured rate among adults aged 18-64 fell from 17.6 percent in the third quarter of 2013 to 10.5 percent by the third quarter of 2015, and to 9.9 percent in the first quarter of 2016, translating into a decline in the number of uninsured non-elderly adults of 15.5 million since 2013.[15]
- Results from the Gallup-Healthways Well-Being Index show that the uninsured rate among adults (including those aged 65 and above) fell from 18.0 percent in the third quarter of 2013 to 11.9 percent in the fourth quarter of 2015 to 11.0 percent in the second quarter of 2016, the lowest level since Gallup and Healthways began tracking this information in 2008.[16]
| APPENDIX TABLE 1 |
|---|
| |
2014 (%) |
2015 (%) |
Percentage Point Change |
Percent Change |
|---|
| TOTAL |
10.4 |
9.1 |
-1.3 |
-12.5 |
| RACE/ETHNICITY |
|
|
|
|
| White, not Hispanic |
7.6 |
6.7 |
-0.9 |
-11.7 |
| Black |
11.8 |
11.1 |
-0.7 |
-5.6 |
| Hispanic |
19.9 |
16.2 |
-3.7 |
-18.5 |
| Asian |
9.3 |
7.5 |
-1.8 |
-19.5 |
| AGE |
|
|
|
|
| Under 19 |
6.2 |
5.3 |
-0.9 |
-14.8 |
| 19 to 25 |
17.1 |
14.5 |
-2.6 |
-15.1 |
| 26 to 64 |
13.8 |
12.2 |
-1.6 |
-11.4 |
| 65 and older |
1.4 |
1.1 |
-0.3 |
-19.6 |
| WORK EXPERIENCE |
|
|
|
|
| Full-time, year-round |
11.2 |
9.9 |
-1.3 |
-11.6 |
| Less than full-time, year-round |
18.1 |
15.8 |
-2.3 |
-12.5 |
| Did not work at least one week |
17.7 |
15.8 |
-2.0 |
-11.1 |
| POVERTY STATUS |
|
|
|
|
| Below 100% of poverty line (FPL) |
19.3 |
17.4 |
-1.9 |
-10.0 |
| 100%-199% FPL |
15.1 |
13.6 |
-1.5 |
-9.8 |
| 200%-299% FPL |
11.7 |
9.8 |
-1.9 |
-15.9 |
| 300%+FPL |
5.7 |
5.2 |
-0.5 |
-8.9 |
| HOUSEHOLD INCOME |
|
|
|
|
| Less than $50,000 |
15.2 |
13.5 |
-1.7 |
-11.2 |
| $50,000+ |
7.4 |
6.5 |
-0.9 |
-12.6 |
| REGION |
|
|
|
|
| Northeast |
7.8 |
6.1 |
-1.7 |
-21.8 |
| Midwest |
8.2 |
6.9 |
-1.3 |
-15.5 |
| South |
13.0 |
12.0 |
-0.9 |
-7.2 |
| West |
10.4 |
8.5 |
-1.8 |
-17.8 |
| EDUCATION |
|
|
|
|
| No high school diploma |
30.4 |
27.6 |
-2.8 |
-9.2 |
| High school, no Bachelor’s degree |
15.5 |
13.3 |
-2.2 |
-14.4 |
| Bachelor’s degree, or higher |
7.2 |
6.2 |
-1.0 |
-13.6 |