American Indians and Alaska Natives (AI/ANs) have a unique legal relationship with the federal government that provides them with specific rights, protections, and services, including the right to health care. Despite the assurance of health care, AI/ANs face persistent health disparities, including a high uninsurance rate, barriers to accessing care, and significant physical and mental health needs. Like many other groups, AI/ANs have benefited greatly from the Affordable Care Act’s (ACA) coverage expansions.
This progress is at risk under the Senate’s Better Care Reconciliation Act (BCRA). The bill would make significant changes to both Medicaid and the marketplace, reversing recent coverage gains for AI/ANs. Specifically, the bill would:
- Effectively end the Medicaid expansion, which has allowed 31 states and the District of Columbia to provide coverage to 11 million low-income adults, including more than 290,000 AI/ANs. Starting in 2021, states would have to pay increasingly large amounts to cover their expansion enrollees, forcing most states to end their expansions. The Medicaid expansion has improved access to care for thousands of AI/ANs, especially in states with large AI/AN populations including Alaska, Arizona, and New Mexico. It has also provided much-needed revenue to Indian Health Service (IHS) and Tribally operated facilities, allowing them to expand services and hire and retain more staff. Ending Medicaid expansion would jeopardize coverage for these newly insured low-income AI/AN adults, and reduce revenue for IHS and Tribally operated facilities, forcing them to revert to pre-ACA service levels.
- Radically restructure Medicaid’s federal financing. The Senate bill would fundamentally change Medicaid’s financing, ending the current federal-state financing partnership and converting virtually the entire Medicaid program to a per capita cap or block grant starting in 2020, putting coverage at risk for nearly 70 million people.[1] This change would force states to make cuts in eligibility and benefits that would grow deeper over time. While payments for services provided to AI/ANs would be outside the per capita cap, AI/ANs would not be immune to eligibility, benefit, and provider rate cuts resulting from the per capita cap.
- Eliminate subsidies that help AI/ANs with out-of-pocket costs. The Senate bill would eliminate cost-sharing reduction subsidies that reduce deductibles, copayments, and coinsurance for lower-income consumers. These subsidies are currently available to AI/ANs with incomes less than 300 percent of poverty, and ensure that they incur no cost-sharing when receiving essential health benefits from non-Indian health providers. Eliminating these subsidies would drive up out-of-pocket costs, making coverage even more unaffordable.
- Cut tax credits and increase premiums. The Senate bill would make an across-the-board cut to premium tax credits by linking them to less generous health coverage, and it would entirely eliminate them for people with incomes between 350 percent and 400 percent of the poverty line. The Senate bill also changes the current tax credit schedule, generally reducing premium tax credits for older people while increasing them for younger people — which is on top of allowing insurers to charge older people up to five times as much as younger people. These changes would make coverage unaffordable for many AI/ANs who rely on marketplace coverage.
The provision of health care to AI/ANs is a unique system with special rules, and in most cases, multiple sources of coverage. IHS, an agency within the Department of Health and Human Services (HHS), is the primary health care provider to nearly 2.2 million non-elderly individuals who self-identify as AI/AN.[2] In addition to being eligible for IHS-funded health care, AI/ANs may also have other sources of insurance, such as Medicaid and private coverage, which in 2015 covered 42 percent and 44 percent of AI/ANs, respectively.[3]
The Role of IHS and Tribes
IHS-funded health care is provided to AI/ANs through a network of hospitals, clinics, and health stations operated by IHS, Tribes or Tribal organizations, and urban Indian health programs (UIHP). Health services provided at IHS and Tribally operated facilities are generally limited to members of federally recognized Tribes and their descendants who live on or near federal reservations. Eligibility for UIHPs is broader than that for IHS and Tribal facilities, and includes service to state-recognized Tribes and Indians from Tribes whose federal recognition has been terminated. AI/ANs don’t have copayments or other out-of-pocket costs for services they receive at any of these facilities.
IHS and Tribally operated facilities mostly provide primary care services; their ancillary and specialty care is quite limited. If facilities are unable to provide needed care, they contract with private providers under the Purchased/Referred Care (PRC) program to provide services.[4] Funding for the PRC is limited — $914 million in fiscal year 2016 — resulting in facilities having to ration care to the most critical cases in order to stretch their PRC dollars throughout the year.[5] In fiscal year 2016, the PRC program denied 80,000 services needed by eligible AI/ANs.[6] In addition, available funds aren’t equally distributed among facilities, resulting in further unmet health care needs and insufficient access to care.
Unlike Medicaid, IHS funding is limited as it’s a discretionary program that requires Congress to appropriate funding each fiscal year. As expected, most of IHS’ budget goes to the provision of direct health care services, but the lack of funding for its facilities has dire consequences, including death, for thousands of AI/ANs.
No region has been harder hit than the Great Plains, where facilities in Nebraska and South Dakota closed temporarily due to the IHS facilities’ poor conditions: there wasn’t enough funding to ensure emergency departments had defibrillators in each room, repair surgical sanitization equipment so that hospital staff didn’t have to wash surgical equipment by hand, or fix a dishware sanitation machine that had been broken for three years so patients didn’t have to eat off of disposable dishware.a
The lack of funding also has hindered IHS’ ability to hire and retain high-quality physicians and other providers. In South Dakota, a high schooler died from a blood clot in her lung after being misdiagnosed with a cough and anxiety. In Nebraska, a man died of kidney failure after not being hospitalized when a test showed his kidneys were shutting down.b
Despite these serious and life-threatening problems, President Trump’s budget would cut $56 million from IHS’ budget in 2018, including $76 million — or 14 percent — from IHS’ facility budget that would help IHS make needed repairs.
a Regina Garcia Cano, “AP NewsBreak: Documents detail serious issues found by federal inspectors at two hospitals in South Dakota that provide care to Native Americans,” U.S. News & World Report, January 28, 2016, https://www.usnews.com/news/us/articles/2016-01-28/ap-newsbreak-reports-detail-issues-at-reservation-hospitals and Letter to Mary Smith from Ranking Member Frank Pallone, House of Representatives, Energy and Commerce Committee, August 4, 2016, https://democrats-energycommerce.house.gov/sites/democrats.energycommerce.house.gov/files/documents/IHS%20Smith%20IHS%20Hospitals%20Letter%202016%208%204.pdf
b Dan Forsch and Christopher Weaver, “’People are Dying Here’: Federal Hospitals Fail Tribes,” The Wall Street Journal, July 7, 2017, https://www.wsj.com/articles/people-are-dying-here-federal-hospitals-fail-native-americans-1499436974.
Medicaid is an important source of affordable coverage for AI/ANs, a population with significant physical and mental health disparities. Compared to non-Hispanic whites, AI/AN adults are twice as likely as to be overweight, obese, diagnosed with diabetes, and experience feelings of sadness, hopelessness, and worthlessness.[7] Medicaid provides access to a broader array of services and providers than AI/ANs can access through IHS-funded health care, helping them meet their physical and mental health needs.
Medicaid coverage is particularly important for AI/AN children, who — like their parents — face significant health disparities. For example, compared to non-Hispanic white children, AI/AN children are 60 percent more likely to have asthma, twice as likely to die from sudden infant death syndrome, and 70 percent more likely to die from accidental deaths before age 1.[8] Under Medicaid’s mandatory Early Periodic Screening, Diagnostic and Treatment (EPSDT) benefit, AI/AN children are guaranteed access to a strong set of comprehensive and preventive health services, such as screenings, hearing, vision, dental, mental health, and developmental services, which help identify and treat emerging conditions.
Medicaid also provides specific beneficiary protections unique to AI/ANs. For example, AI/ANs are exempt from Medicaid cost-sharing, including premiums. In addition, states are prohibited from counting certain types of property as resources in determining Medicaid eligibility, and cannot mandatorily enroll AI/ANs in Medicaid managed care plans. The AI/ANs who opt to enroll in Medicaid managed care receive special protections. Medicaid managed care plans are required to have a sufficient number of Indian health providers participating in their networks, and they must allow AI/ANs to go outside the plans’ networks to seek care from an Indian health provider.
In addition to being a critical source of coverage, Medicaid is a key source of financing for IHS and other Indian health providers. Because IHS is the payer of last resort behind Medicaid and other forms of insurance, IHS and Tribally operated facilities can bill Medicaid, at an enhanced match, for covered services that they provide to Medicaid-enrolled AI/ANs. The federal government covers 100 percent of these costs as long as the services are “received through” an IHS or Tribally operated facility, reflecting the federal trust responsibility to provide health care to AI/ANs as well as a policy that states shouldn’t have to use state dollars to pay for health care provided by a federal facility. This special financing rule allows IHS to collect additional revenue, enhancing its capacity to provide services, retain and hire staff, and stretch its limited PRC dollars further. In fiscal year 2016, IHS collected $1.2 billion in revenue from other forms of insurance (e.g., Medicaid, Medicare, and Veteran Affairs, etc.), with the largest share — $880 million — coming from Medicaid.[9]
Expanding Services That Qualify for 100 Percent Federal Funding
In 2016, the Centers for Medicare & Medicaid Services (CMS) issued guidance expanding the scope of services that qualify for the 100 percent Medicaid match to include any service that’s covered by the Medicaid state plan that the IHS or Tribal facility is authorized to provide. This means that transportation services, related travel expenses, home- and community-based services, and other long-term services and supports now qualify for the 100 percent match. Non-IHS/Tribal providers can also claim for the enhanced match if they’re a Medicaid provider, an IHS/Tribal provider has requested the service they’re providing, and there’s a written care coordination agreement in place.
The intended purpose of this policy change is to “help states, the IHS, and Tribes improve delivery systems for AI/ANs by increasing access to care, strengthening continuity of care, and improving population health.”a Not only does it improve health and access to care, it also helps reduce state costs, freeing up state dollars for other health initiatives such as Medicaid expansion. Alaska and South Dakota have shown interest in implementing this policy:
- The new policy has allowed Alaska to increase access to its rural AI/AN beneficiaries as it’s now able to claim for 100 percent of the costs associated with transportation and related travel expenses. This is critical for Alaska in light of the significant distances between providers and Tribal members living in remote areas of the state.
- In 2016, South Dakota outlined a proposal that not only expanded services to AI/ANs, such as telehealth, but also included a pathway to finance Medicaid expansion using the savings generated from the additional services eligible for the enhanced match. The state is continuing its progress on telehealth initiatives, but has yet to move forward with Medicaid expansion.
a Centers for Medicare & Medicaid Services, “SHO #16-002: Federal Funding for Services ‘Received Through’ an IHS/Tribal Facility and Furnished to Medicaid-Eligible American Indians and Alaska Natives,” February 26, 2016, https://www.medicaid.gov/federal-policy-guidance/downloads/SHO022616.pdf.
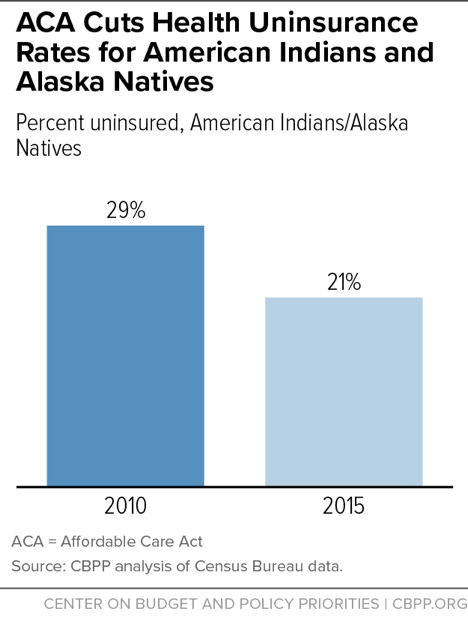
Despite guaranteed access to health care through the IHS, AI/ANs have historically had higher rates of uninsurance than the general population. In 2010, before the enactment of the ACA, the uninsured rate for AI/ANs was 29 percent, compared to 16 percent for the general population.[10] The ACA’s expansion of Medicaid and subsidized marketplace coverage have provided coverage to over 200,000 AI/ANs, reducing the AI/AN uninsured rate by more than a quarter, from 29 percent in 2010 to 21 percent in 2015.[11] (See Figure 1.)
Before the ACA, Medicaid only covered parents with very low incomes, and typically didn’t cover adults without children regardless of their income. The ACA changed this by expanding Medicaid to all adults with incomes below 138 percent of poverty in states taking the option. This includes a number of states, such as Alaska, Arizona, and New Mexico, with large AI/AN populations. In these three states alone, over 53,000 AI/ANs have gained coverage through Medicaid expansion. (See Table 1.)
Medicaid expansion not only provides coverage of essential services for AI/ANs, it provides them with access to providers beyond those who are available through an IHS or Tribal facility. Moreover, improved access to care means improved health outcomes. Studies show that expansion has improved access to care, health outcomes, and financial security for low-income adults.[12]
Medicaid expansion, coupled with CMS’ updated Tribal financing policy, provides an opportunity for increased Medicaid revenues for IHS and Tribally operated facilities. In the states that have expanded Medicaid, the share of beneficiaries served by IHS and Tribal facilities as well as the expanded scope of services eligible for the enhanced match will most likely grow, increasing these facilities’ revenue. This in turn will help them retain and potentially hire more staff, expand the scope of services they can provide “in-house,” or purchase new medical equipment to improve the delivery of care in rural areas, such as increased telehealth capacity.
Medicaid expansion has also helped extend the availability of PRC funds. In fact, HHS cited Medicaid expansion as an important source of funding that “ensures [PRC] programs can purchase preventive care beyond emergency care services, such as mammograms or colonoscopies.”[13] This means that IHS funds can go further to help those who remain uninsured. Before Montana expanded Medicaid in 2015, IHS and Tribal facilities generally could only refer their patients for specialty care in emergency “life or limb” situations due to the high number of uninsured patients and limited PRC funding. After the state expanded, however, these facilities reported that they were able to stretch their PRC funding, and have authorized non-emergency specialty care that AI/ANs previously had to forgo.[14]
The marketplace serves as another important source of coverage for AI/ANs. As with other marketplace enrollees, AI/ANs with incomes between 100 and 400 percent of the poverty line who are not eligible for other coverage may receive premium tax credits. The ACA also allows Tribes to make coverage even more affordable to AI/AN marketplace enrollees by paying an individual’s monthly premiums through a Tribal Sponsorship program. This not only helps increase access to care for the individual, but also helps Tribes and IHS extend the availability of PRC funding.
In addition to premium tax credits, AI/ANs with incomes below 300 percent of the poverty line are also eligible for additional cost-sharing reduction subsidies regardless of the metal-level Qualified Health Plan (QHP) they purchase. This is a special consumer protection afforded to AI/ANs as these subsidies are only available to people in the general population with incomes below 250 percent of poverty who enroll in silver-level coverage.
The additional subsidies AI/ANs receive ensure that they pay no cost-sharing when receiving essential health benefits from a non-Indian health care provider. Moreover, because these subsidies are available to AI/ANs regardless of a QHP’s metal level, AI/ANs can enroll in bronze-level QHPs, which have the lowest premiums of all the metal levels, making their overall coverage costs (premiums plus out-of-pocket costs) even more affordable. When coupled with a Tribal Sponsorship program, some marketplace AI/AN enrollees may have to pay nothing or very little for their coverage.
Senate Bill Jeopardizes Medicaid and Marketplace Coverage for American Indians and Alaska Natives
The Senate bill’s significant changes to Medicaid and the marketplace would put AI/ANs at risk. According to the Congressional Budget Office, the bill would cut Medicaid by $772 billion over the next ten years, causing 15 million beneficiaries to lose coverage.[15] It would effectively end the Medicaid expansion and fundamentally change how the program is financed.[16] AI/ANs enrolled in marketplace coverage would face equally significant changes to the affordability of their coverage because the bill would cut premium tax credits and eliminate cost-sharing reduction subsidies entirely. Taken together, these changes would reverse recent health care improvements in Indian country.
Starting in 2021, the Senate bill would reduce the Medicaid matching rate for Medicaid expansion enrollees. This means that states would have to pay increasingly large amounts to cover their expansion enrollees, forcing most states to end their expansions. This would be devastating for the over 290,000 AI/ANs who have gained coverage, such as those in Alaska, Arizona, and Ohio.
Ending expansion is particularly harmful to AI/AN adolescents transitioning into young adulthood, such as those being treated for mental illness. In 2014, suicide was the leading cause of death for AI/AN girls between the ages of 10 and 14, and AI/AN boys were twice as likely as non-Hispanic whites to commit suicide.[17] In fact, suicide is the second-leading cause of death for AI/ANs between the ages of 10 and 34.[18] Thanks to the ACA’s Medicaid expansion, these young adults will continue to have a source of coverage once they turn 19 years old and no longer qualify for Medicaid as children, ensuring that they will continue to get the care they need and live productive lives in their communities with greater financial stability.[19] Ending the Medicaid expansion would leave young adults few options for coverage.
AI/AN parents and children are also at risk for losing coverage. The ACA expanded coverage for millions of parents who weren’t previously eligible. By effectively ending the Medicaid expansion, the BCRA would force many of these parents back into the ranks of the uninsured, harming both AI/AN children and parents alike, as studies show that children are more likely to have health insurance if their parents are covered.[20] AI/AN children are particularly at risk as they already have higher-than-average uninsured rates (11 percent versus 6 percent for the general population), and can’t afford for those with coverage to fall off.[21]
While improving AI/ANs’ access to care and financial security, the Medicaid expansion has also helped IHS and Tribes extend valuable PRC dollars to help provide needed care to its members. Ending expansion would result in IHS and Tribal facilities receiving less Medicaid funding because fewer AI/ANs would be covered by Medicaid.
The Senate bill would end Medicaid as we know it, ending the current federal-state financing partnership and converting virtually the entire Medicaid program to a per capita cap in 2020, shifting significant costs and risks to states. Under the Senate bill’s per capita cap proposal, states would receive a fixed amount for beneficiaries in the following eligibility groups: children, seniors, people with disabilities, non-expansion adults, and expansion adults. The per-beneficiary amounts would be set below projected Medicaid spending and would grow each year at a lower rate than expected health care costs. States would ultimately receive less federal funding than needed to maintain coverage at current levels, forcing states to raise taxes or cut other parts of their budget, or as is far more likely, make increasingly deep cuts to Medicaid eligibility, benefits, and provider payments.[22]
While payments for services provided for AI/ANs at IHS or Tribal facilities wouldn’t be subject to the per capita cap, AI/ANs would still feel its effects because of how capped funding works.[23] No one, including AI/ANs, could or would be protected from the large and growing Medicaid eligibility, benefit, or provider rate cuts states would have to make to their entire programs in response to the federal funding shortfalls under a per capita cap.[24] Because of the likely benefit cuts, IHS and Tribal facilities would also receive reduced Medicaid revenue as fewer Medicaid-covered services would be eligible for the enhanced federal match.
Under the Senate bill, states would be forced to make hard decisions on potential cuts to their Medicaid programs, with optional eligibility pathways and benefits, such as home- and community-based services (HCBS), as the most likely targets for cuts. HCBS allow seniors and people with disabilities to stay in their homes rather than move to a nursing home to get the long-term services and supports they need. Unlike nursing home services, which states must cover, most HCBS are optional Medicaid benefits that states can cut when they face funding shortfalls, making them likely targets because states spend more on optional HCBS than on any other optional benefit.[25] The Senate bill would cause states to cap enrollment, impose waiting lists, or eliminate their HCBS programs altogether.
Such HCBS cuts would be particularly harmful to AI/ANs as older AI/ANs are among the fastest aging population — between 2000 and 2010, the number of AI/AN adults 65 years or older increased by nearly 41 percent, and is projected to rise by an additional 350 percent by 2050.[26] These demographic changes demonstrate a clear need for long-term services and supports in Indian country. HCBS are particularly important to elder AI/ANs as they allow them to remain in their communities near their families and other Tribal members as well as receive culturally appropriate care in their homes. Studies show that elder AI/ANs who receive HCBS lead an improved and prolonged life compared to those that move into nursing homes.[27] In Alaska, for example, the Tanana Chiefs Conference uses Medicaid to implement its Community Health Outreach Program, a program that relies on Medicaid to provide chore services, personal care assistance, respite for caregivers, specialized medical equipment, home modifications, and care coordination to elders and people with disabilities living in the Tanana Chiefs Conference rural area.[28] The Senate bill puts this program, along with others across the country, at risk.
In addition to the Medicaid changes, the Senate bill would drastically cut premium tax credits and cost-sharing reduction subsidies currently available to AI/ANs. The biggest marketplace change affecting AI/ANs is the elimination of the cost-sharing reduction subsidies. Eliminating these subsidies would make coverage unaffordable for nearly 30,000 AI/ANs, jeopardizing their coverage. (See Table 2.)
In addition to eliminating the cost-sharing reduction subsidies, the Senate bill would also cut premium tax credits across the board by linking them to less generous health coverage. It would also change the current tax credit schedule, reducing the premium tax credits for older people while increasing them for younger people. This change, when coupled with the ability for insurers to charge older people up to five times more than younger people, would be especially harmful to AI/ANs, who are aging more quickly than the general population. The Senate bill would also eliminate tax credits entirely for people with incomes between 350 and 400 percent of the poverty line.[29] These premium tax credit changes would make it harder for AI/ANs purchasing their coverage in the marketplace to afford their monthly premiums.
The Senate bill would jeopardize AI/ANs’ recent coverage gains by slashing Medicaid and making marketplace coverage unaffordable. Although payments for services provided to AI/ANs fall outside the proposed per capita cap, capping federal Medicaid funding would still harm them, as states would have to cut eligibility, benefits, and provider rates that affect their entire Medicaid programs. The elimination of cost-sharing reductions and cuts to premium tax credits would put coverage out of reach for many moderate-income AI/ANs. Moreover, these changes would not only affect coverage for AI/ANs, but would cut needed revenue from IHS and Tribal facilities, forcing them to return to rationing care due to high numbers of uninsured AI/ANs and limited funding.
| APPENDIX TABLE 1 |
|---|
| |
Estimated Number Losing Medicaid Expansion Coverage |
Number Losing Cost-Sharing Reduction Subsidies |
|---|
| Alabama |
|
- |
|
|
358 |
|
| Alaska |
|
5,400 |
|
|
762 |
|
| Arizona |
|
12,900 |
|
|
1,073 |
|
| Arkansas |
|
N/A |
|
|
499 |
|
| California |
|
88,900 |
|
|
N/A |
|
| Colorado |
|
16,300 |
|
|
N/A |
|
| Connecticut |
|
N/A |
|
|
N/A |
|
| Delaware |
|
N/A |
|
|
- |
|
| District of Columbia |
|
N/A |
|
|
N/A |
|
| Florida |
|
- |
|
|
992 |
|
| Georgia |
|
- |
|
|
326 |
|
| Hawaii |
|
N/A |
|
|
N/A |
|
| Idaho |
|
- |
|
|
N/A |
|
| Illinois |
|
5,200† |
|
|
334 |
|
| Indiana |
|
N/A |
|
|
163 |
|
| Iowa |
|
N/A |
|
|
77 |
|
| Kansas |
|
- |
|
|
840 |
|
| Kentucky |
|
4,100 |
|
|
N/A |
|
| Louisiana |
|
N/A |
|
|
266 |
|
| Maine |
|
- |
|
|
199 |
|
| Maryland |
|
N/A |
|
|
N/A |
|
| Massachusetts |
|
N/A |
|
|
N/A |
|
| Michigan |
|
13,500 |
|
|
1,009 |
|
| Minnesota |
|
8,800 |
|
|
N/A |
|
| Mississippi |
|
- |
|
|
62 |
|
| Missouri |
|
- |
|
|
770 |
|
| Montana |
|
11,228 |
|
|
1,013 |
|
| Nebraska |
|
- |
|
|
393 |
|
| Nevada |
|
5,000† |
|
|
370 |
|
| New Hampshire |
|
N/A |
|
|
N/A |
|
| New Jersey |
|
N/A |
|
|
52 |
|
| New Mexico |
|
45,600 |
|
|
903 |
|
| New York |
|
3,100 |
|
|
N/A |
|
| North Carolina |
|
- |
|
|
665 |
|
| North Dakota |
|
3,900† |
|
|
984 |
|
| Ohio |
|
13,600 |
|
|
122 |
|
| Oklahoma |
|
- |
|
|
9,319 |
|
| Oregon |
|
24,100 |
|
|
683 |
|
| Pennsylvania |
|
9,700 |
|
|
168 |
|
| Rhode Island |
|
N/A |
|
|
N/A |
|
| South Carolina |
|
- |
|
|
216 |
|
| South Dakota |
|
- |
|
|
755 |
|
| Tennessee |
|
- |
|
|
309 |
|
| Texas |
|
- |
|
|
3,125 |
|
| Utah |
|
- |
|
|
845 |
|
| Vermont |
|
N/A |
|
|
N/A |
|
| Virginia |
|
- |
|
|
297 |
|
| Washington |
|
30,700 |
|
|
N/A |
|
| West Virginia |
|
N/A |
|
|
N/A |
|
| Wisconsin |
|
- |
|
|
1,134 |
|
| Wyoming |
|
- |
|
|
191 |
|
| APPENDIX TABLE 2 |
|---|
| |
Percent Change in Uninsurance from Coverage Under Affordable Care Act |
|---|
| Alabama |
|
14.2% |
|
| Alaska |
|
59.6% |
|
| Arizona |
|
37.8% |
|
| Arkansas |
|
N/A |
|
| California |
|
209.9% |
|
| Colorado |
|
158.9% |
|
| Connecticut |
|
N/A |
|
| Delaware |
|
N/A |
|
| District of Columbia |
|
N/A |
|
| Florida |
|
62.3% |
|
| Georgia |
|
8.7% |
|
| Hawaii |
|
N/A |
|
| Idaho |
|
55.8% |
|
| Illinois |
|
127.0% |
|
| Indiana |
|
N/A |
|
| Iowa |
|
N/A |
|
| Kansas |
|
27.4% |
|
| Kentucky |
|
N/A |
|
| Louisiana |
|
N/A |
|
| Maine |
|
N/A |
|
| Maryland |
|
N/A |
|
| Massachusetts |
|
N/A |
|
| Michigan |
|
181.3% |
|
| Minnesota |
|
64.9% |
|
| Mississippi |
|
16.3% |
|
| Missouri |
|
36.2% |
|
| Montana |
|
93.0% |
|
| Nebraska |
|
30.6% |
|
| Nevada |
|
113.3% |
|
| New Hampshire |
|
N/A |
|
| New Jersey |
|
119.7% |
|
| New Mexico |
|
231.9% |
|
| New York |
|
72.6% |
|
| North Carolina |
|
35.1% |
|
| North Dakota |
|
97.8% |
|
| Ohio |
|
194.0% |
|
| Oklahoma |
|
20.4% |
|
| Oregon |
|
236.6% |
|
| Pennsylvania |
|
N/A |
|
| Rhode Island |
|
N/A |
|
| South Carolina |
|
62.2% |
|
| South Dakota |
|
2.0% |
|
| Tennessee |
|
26.7% |
|
| Texas |
|
23.0% |
|
| Utah |
|
31.8% |
|
| Vermont |
|
N/A |
|
| Virginia |
|
39.9% |
|
| Washington |
|
174.8% |
|
| West Virginia |
|
N/A |
|
| Wisconsin |
|
52.8% |
|
| Wyoming |
|
10.7% |
|
| Total |
|
72.5% |
|