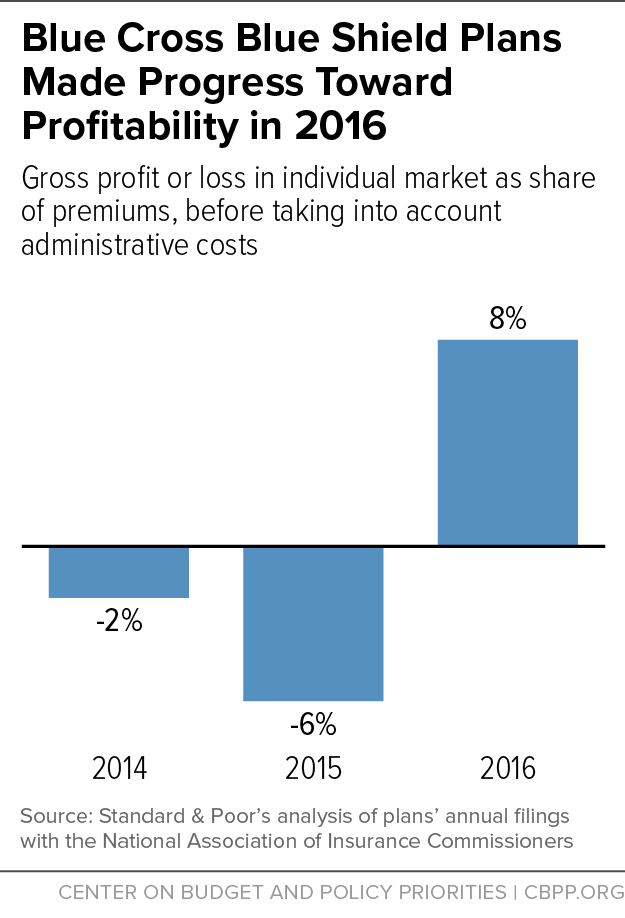ACA Marketplaces Poised for Greater Price Stability and Competition, But Also Vulnerable to Sabotage
End Notes
[1] S&P Global Ratings, “The U.S. Individual Market Showed Progress in 2016, But Still Needs Time to Mature,” April 7, 2017, https://www.globalcreditportal.com/ratingsdirect/renderArticle.do?articleId=1828594&SctArtId=421970&from=CM&nsl_code=LIME&sourceObjectId=10047007&sourceRevId=5&fee_ind=N&exp_date=20270408-00:16:31.
[2] Sarah Lueck, “How the Trump Administration Might Sabotage ACA Insurance Markets,” Center on Budget and Policy Priorities, April 4, 2017, https://www.cbpp.org/health/commentary-how-the-trump-administration-might-sabotage-aca-insurance-markets.
[3] Office of the Assistant Secretary for Planning and Evaluation, “Health Insurance Coverage for Americans with Pre-existing Conditions: the Impact of the Affordable Care Act,” Department of Health and Human Services, January 5, 2017, https://aspe.hhs.gov/system/files/pdf/255396/Pre-ExistingConditions.pdf.
[4] See, for example, McKinsey Center for U.S. Health Reform, “2014 Individual Market Post-3R Financial Performance,” February 5, 2016, http://healthcare.mckinsey.com/sites/default/files/infographics/2016%20Post-3R%20Infographic.pdf.
[5] While many insurers raised premiums for given plans by more than 2 percent, average ACA individual market premiums increased by only 2 percent after consumers shopped and selected new coverage. For these data and data on per-enrollee claims costs, see Centers for Medicare & Medicaid Services, “Changes in Individual Market Costs from 2014-2015: Near-Zero Growth Suggests an Improving Risk Pool,” August 11, 2016, https://www.cms.gov/cciio/resources/forms-reports-and-other-resources/downloads/final-risk-pool-analysis-8_11_16.pdf. For a more extended discussion of insurers’ initial pricing challenges in the ACA individual market, see Council of Economic Advisers, “Understanding Recent Developments in the Individual Market,” January 2017, https://obamawhitehouse.archives.gov/sites/default/files/page/files/201701_individual_health_insurance_market_cea_issue_brief.pdf.
[6] The 8 percent average captures only marketplace premiums (not premiums for individual market plans subject to ACA rules but offered outside the ACA marketplaces), and it includes only states using the HealthCare.gov eligibility and enrollment platform. Premium data for the full individual market for 2016 are not yet available, but the 2015 experience suggests the HealthCare.gov marketplace average provides a reasonable proxy. Assistant Secretary for Planning and Evaluation, “Health Insurance Premiums After Shopping, Switching, and Tax Credits, 2015-2016,” Department of Health and Human Services, April 12, 2016, https://aspe.hhs.gov/system/files/pdf/198636/MarketplaceRate.pdf.
[7] For example, certain states saw 2016 increases in “benchmark” premiums (premiums for the second-lowest cost silver plan, which are used to determine premium tax credits) that were well above the national average, including Alaska, Montana, North Carolina, New Mexico, Oklahoma, Oregon, South Dakota, and Tennessee. Kelsey Avery et al., “Health Plan Choice and Premiums in the 2016 Health Insurance Marketplace,” Department of Health and Human Services Assistant Secretary for Planning and Evaluation, October 30, 2015, https://aspe.hhs.gov/system/files/pdf/135461/2016%20Marketplace%20Premium%20Landscape%20Issue%20Brief%2010-30-15%20FINAL.pdf.
[8] See, for example, McKinsey Center for U.S. Health Reform, “2016 Exchange Market Remains in Flux: Plan Type Trends,” January 4, 2016, http://healthcare.mckinsey.com/sites/default/files/2016%20Plan%20Type%20Trends%20Infographic%20v29.pdf and materials from the Centers for Medicare & Medicaid Services conference on marketplace innovation, available at https://www.cms.gov/CCIIO/Resources/Forms-Reports-and-Other-Resources/.
[9] The S&P report excludes Anthem (the major for-profit Blues plan) and California Blue Cross Blue Shield (because it uses a different reporting template than other Blues plans).
[10] Council of Economic Advisers, “Understanding Recent Developments in the Individual Market,” and Sean P. Keehan et al., “National Health Expenditure Projections, 2016-25: Price Increases, Aging Push Sector to 20 Percent of Economy,” Health Affairs, February 2017, http://content.healthaffairs.org/content/early/2017/02/14/hlthaff.2016.1627.full.
[11] Assistant Secretary for Planning and Evaluation, “Health Plan Choice and Premiums in the 2017 Health Insurance Marketplace,” October 24, 2016, https://aspe.hhs.gov/system/files/pdf/212721/2017MarketplaceLandscapeBrief.pdf, Appendix C.
[12] Data for 2015 and 2016 are available from Assistant Secretary for Planning and Evaluation, “Health Insurance Premiums After Shopping, Switching, and Tax Credits, 2015-2016,” Department of Health and Human Services, April 12, 2016, https://aspe.hhs.gov/system/files/pdf/198636/MarketplaceRate.pdf; data for 2017 are available from Centers for Medicare & Medicaid Services, “Health Insurance Marketplaces 2017 Open Enrollment Period Final Open Enrollment Report,” March 15, 2017, https://www.cms.gov/Newsroom/MediaReleaseDatabase/Fact-sheets/2017-Fact-Sheet-items/2017-03-15.html.
[13] Bob Herman, “Florida Blue Increases Obamacare Profits,” Axios, April 3, 2017, https://www.axios.com/florida-blue-increases-profits-under-obamacare-2338273526.html.
[14] Bob Herman, “How Some Blues Made the ACA Work While Others Failed,” Modern Healthcare, October 15, 2016, http://www.modernhealthcare.com/article/20161015/MAGAZINE/310159989 and Tom Dennis, “Tim Huckle Interview: Obamacare and North Dakota Nice,” Grand Forks Herald, November 27, 2016, http://www.grandforksherald.com/opinion/op-ed-columns/4167359-tim-huckle-interview-obamacare-and-north-dakota-nice.
[15] JoNel Aleccia, ‘“It’s Not Like Other States’: High-Cost Alaska Sits in the Eye of Health Reform Storm,” Kaiser Health News, April 5, 2017, http://khn.org/news/its-not-like-other-states-high-cost-alaska-sits-in-the-eye-of-health-reform-storm/. Note that Alaska’s state-sponsored reinsurance program had not yet taken effect in 2016.
[16] Jayne O’Donnell, “Obamacare was profitable for some insurers despite public comments,” USA Today, December 4, 2016, https://www.usatoday.com/story/news/politics/2016/12/04/obamacare-profitable-some-insurers-despite-public-comments/94732188/.
[17] Kristen Schorsch, “Blue Cross Parent Stops the Bleeding, But at What Cost?” Modern Healthcare, March 14, 2017, http://www.modernhealthcare.com/article/20170314/NEWS/170319958.
[18] Center on Budget and Policy Priorities, “Sabotage Watch: Tracking Efforts to Undermine the ACA,” updated April 14, 2017, https://www.cbpp.org/sabotage-watch-tracking-efforts-to-undermine-the-aca.
[19] Kaiser Family Foundation, “Estimates: Average ACA Marketplace Premiums for Silver Plans Would Need to Increase by 19% to Compensate for Lack of Funding for Cost-Sharing Subsidies,” April 6, 2017, http://kff.org/health-reform/press-release/estimates-average-aca-marketplace-premiums-for-silver-plans-would-need-to-increase-by-19-to-compensate-for-lack-of-funding-for-cost-sharing-subsidies/?utm_campaign=KFF-2017-April-Web-Briefing-ACA-Cost-Sharing-Subsidies&utm_source=hs_email&utm_medium=email&utm_content=50113735&_hsenc=p2ANqtz--ETCChd1Smzc8fbJmgZgEqu8F8u2CUK4nJ8yTyQF5B-ssWnZ6Qcz2Ma3spizILL25hgmJKrdgz3x17hs1A4s3NHbgvkw&_hsmi=50113735.
[20] Bob Bryan, “One of the Nation’s Biggest Health Insurers Is Ditching Iowa’s Obamacare Exchanges,” Business Insider, April 6, 2017, http://www.businessinsider.com/aetna-leaving-iowa-obamacare-exchange-marketplace-2017-4 and Tony Leys, “Wellmark to Halt Sales of Individual Health Insurance Policies,” Des Moines Register, April 3, 2017, http://www.desmoinesregister.com/story/news/health/2017/04/03/wellmark-halt-sales-individual-health-insurance-policies/99994906/.
[21] Letter to President Trump from America’s Health Insurance Plans, Blue Cross Blue Shield Association, American Academy of Family Physicians, American Medical Association, American Hospital Association, Federation of American Hospitals, American Benefits Council, and the Chamber of Commerce, April 12, 2017, https://ahip.org/wp-content/uploads/2017/04/Joint-CSR-Letter-to-President-Trump-04.12.2017.pdf.
[22] Sarah Kliff, “Insurance Regulators Are Panicked About Obamacare’s Future,” Vox, April 10, 2017, http://www.vox.com/policy-and-politics/2017/4/10/15247724/obamacare-future-marketplaces and Letter to Secretary Price from Insurance Commissioner Mike Kreidler and the Association of Washington Healthcare Plans, April 8, 2017, https://www.insurance.wa.gov/current-issues-reform/affordable-care-act/documents/Kreidler-AWHP-letter-HHSSec-TomPrice.pdf.