BEYOND THE NUMBERS
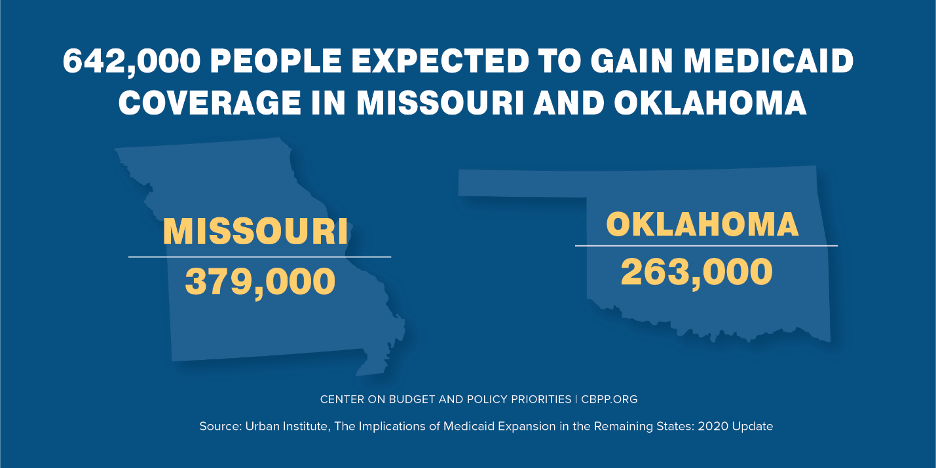
Missouri and Oklahoma policymakers should follow the lead of other states and quickly implement their Medicaid expansions under the Affordable Care Act (ACA), which their voters approved this summer. By moving quickly, policymakers will not only provide coverage to more than 600,000 people in the two states (see figure), but they also will leverage Medicaid’s critical role in addressing COVID-19 and the deep recession.
The 35 states and Washington, D.C. that have implemented expansion (coverage in Nebraska begins on October 1) have much lower uninsured rates than non-expansion states. Expansion has also helped states make progress in addressing racial and ethnic disparities in coverage and care, and beneficiaries report improved health outcomes, among other benefits.
The pandemic and recession make access to Medicaid more critical than ever. With unemployment above 10 percent, many people are losing their job-based health coverage. Some 40 percent of people losing job-based coverage in non-expansion states will become uninsured, compared to 23 percent in expansion states, largely because fewer will qualify for Medicaid, Urban Institute researchers project.
And Medicaid helps not just jobless people. It covers an estimated 5 million workers in essential or front-line industries — working in jobs that may require them to show up regardless of stay-at-home orders or other restrictions. These workers are more than twice as likely to have Medicaid coverage and 42 percent less likely to be uninsured if they live in an expansion state. We estimate that 34,000 uninsured essential workers in Missouri and 22,000 in Oklahoma could gain Medicaid coverage through expansion.
The ballot initiatives that Missouri and Oklahoma voters approved both say that expansion coverage will begin by July 1, 2021, but policymakers can implement it before then. Other states have implemented their expansion quickly. Alaska, for example, began coverage in September 2015, a month and a half after Governor Bill Walker announced that he would adopt the expansion. Louisiana began its coverage on July 1, 2016, after Governor John Bel Edwards announced the move in January of that year.
To begin expansion coverage, states must submit three state plan amendments (SPAs) to the federal Centers for Medicare & Medicaid Services (CMS): one expanding eligibility, one outlining the expansion group’s benefit package, and one describing the procedures for determining the appropriate federal match rate for covering the costs associated with expansion enrollees. Oklahoma has already submitted its SPAs to CMS, though it indicated that it plans to wait to begin coverage on July 1, 2021, the deadline in the ballot initiative.
A state can ask CMS to approve its SPAs retroactive to the start of the quarter when it submitted them, so Oklahoma could have begun accepting applications for expansion coverage now and the people it enrolls could get coverage retroactive to July 1, 2020.
Missouri and Oklahoma should also use strategies from other states to quickly get people covered while limiting the burden on eligibility staff. These include enrolling eligible people in Medicaid based on their enrollment in other federal programs like SNAP (food stamps), as Louisiana and Virginia did; moving people with limited Medicaid coverage for family planning services into expansion coverage; and enrolling parents in expansion coverage based on their children’s Medicaid eligibility.
Unfortunately, Missouri and Oklahoma policymakers suggested that they’re in no hurry to implement expansion, citing worries about its cost and the need to find a funding source for the state’s share of costs. (Under the ACA, the federal government pays 90 percent of expansion costs and states pay 10 percent.) State cost concerns are common but unfounded. For example, a New England Journal of Medicine analysis of state budget data concludes that expansion states saw “no significant changes in spending from state revenues associated with Medicaid expansion” compared to non-expansion states.
Oklahoma estimated its expansion costs at about $150 million a year. Earlier this year, Governor Kevin Stitt vetoed a bill that would raise that amount largely by raising assessments on the state’s hospitals. And Missouri’s cost projections, produced by Washington University researchers, range from a cost of $200 million over five years to savings of $1 billion due to offsetting budget savings that expansion will produce.
With Medicaid coverage more important than ever, Missouri and Oklahoma should move quickly to implement their voter-approved expansion initiatives.
