off the charts
POLICY INSIGHT
BEYOND THE NUMBERS
BEYOND THE NUMBERS
This is the next in our “Medicaid Works” blog series, which aims to inform the debate over Medicaid’s future by providing the latest facts and figures on this essential and popular part of the nation’s health care system.
Medicaid provides health coverage to low-income families and individuals, including children, parents, pregnant women, seniors, and people with disabilities. Here are ten key facts about how Medicaid helps millions of Americans live healthier, more secure lives:
- Medicaid provided quality health coverage for 97 million low-income Americans over the course of 2015. In any given month, Medicaid served 33 million children, 27 million adults (mostly in low-income working families), 6 million seniors, and 10 million persons with disabilities, according to Congressional Budget Office (CBO) estimates.
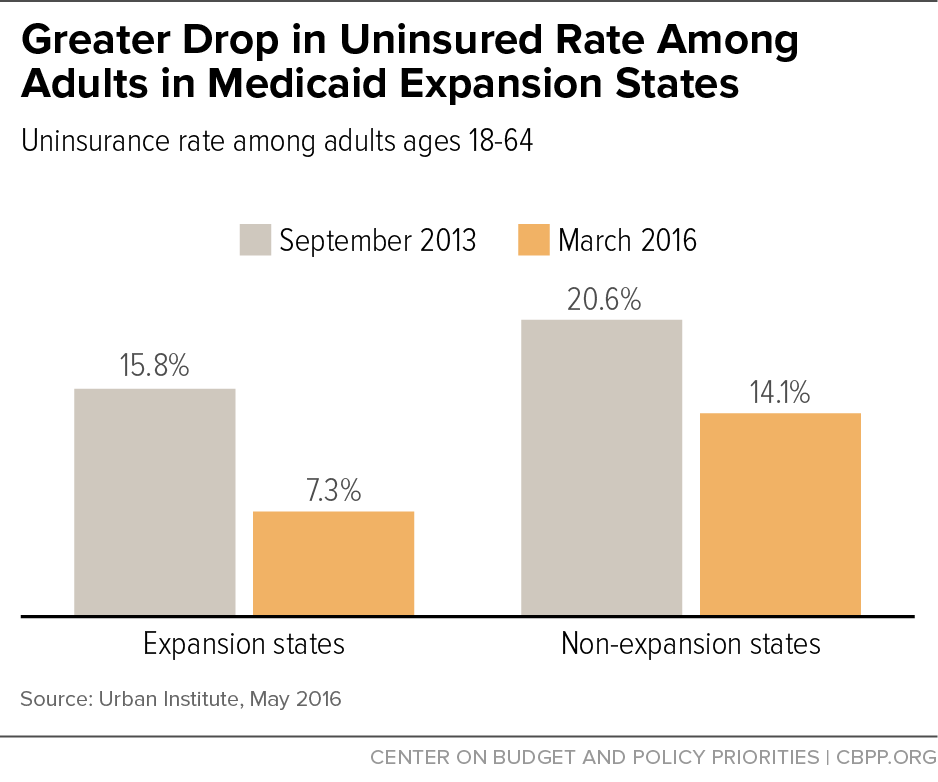
- Medicaid has cut dramatically the number of Americans without health insurance. Since the implementation of health reform’s major coverage expansions in 2014, Medicaid and the new health marketplaces have helped cut the number of uninsured Americans from 45 million to 29 million, the Centers for Disease Control and Prevention estimates. States that expanded Medicaid have had significantly greater reductions in the share of residents who were uninsured than non-expansion states (see chart). By 2020, an estimated 13 million more adults will have enrolled in Medicaid and gained access to affordable health coverage due to health reform.
- Medicaid participation is high. Some 65.6 percent of low-income adults with children who are eligible for Medicaid are enrolled, according to the Urban Institute, a relatively strong participation rate compared to some other programs. And evidence so far among states adopting health reform’s Medicaid expansion shows substantial increases in overall Medicaid enrollment, which indicates robust participation among expansion-eligible individuals. In addition, 88.3 percent of eligible children participate in Medicaid or the Children’s Health Insurance Program (CHIP), according to the Urban Institute.
- Medicaid has improved access to care for millions, including those with chronic conditions. A landmark study of Oregon’s Medicaid program found that beneficiaries were 40 percent less likely to have suffered a decline in their health in the last six months than similar people without health insurance coverage. They were also likelier to use preventive care (such as cholesterol screenings), to have a regular clinic where they could receive primary care, and to receive a diagnosis of and treatment for depression and diabetes.
- Medicaid provides significant financial support to low-income beneficiaries. Medicaid lifted 2.6 million people out of poverty in 2010, equating to a 0.7 percentage-point drop in the poverty rate. The program cut poverty most among adults with disabilities, children, seniors, African Americans, and Hispanics. Research from Oregon’s Medicaid program also shows that beneficiaries were 40 percent less likely to go into medical debt or leave other bills unpaid in order to cover medical expenses, and that Medicaid coverage nearly eliminated catastrophic out-of-pocket medical costs.
- Medicaid produces long-term educational benefits for kids. Children who are eligible for Medicaid do better in school and miss fewer school days due to illness or injury. They‘re also likelier to finish high school, attend college, and graduate from college. Kids who are eligible for Medicaid earn more as adults and experience fewer emergency room visits and hospitalizations, research shows.
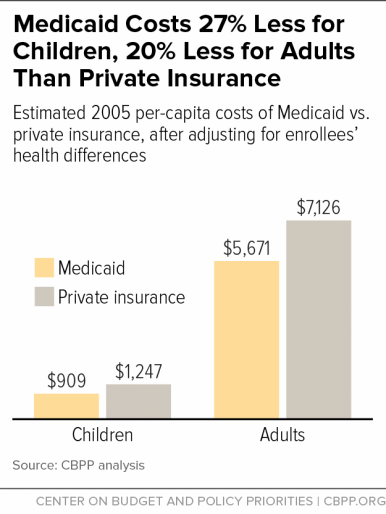
- Medicaid is cost-effective. Medicaid’s costs per beneficiary are substantially lower (see chart) and have been growing more slowly than for private insurance. Medicaid provides more comprehensive benefits than private insurance at significantly lower out-of-pocket cost to beneficiaries, but its lower payment rates to health care providers and lower administrative costs make the program very efficient.
- Medicaid gives states flexibility to design their own programs. The federal government sets minimum standards, including the categories of people that all states must cover. Beyond that, states set their own rules, including whom they cover, what benefits they provide, and how they deliver health care services. As a result, Medicaid eligibility varies substantially from state to state. Moreover, states have taken advantage of Medicaid’s existing flexibility to improve beneficiary health outcomes while lowering costs by changing how health care is delivered.
- Health reform’s Medicaid expansion is saving states money. The federal government will pay the entire cost of health care for newly eligible beneficiaries through 2016, and many states that have expanded Medicaid have found that it has produced net savings for their budgets. States will spend just 1.6 percent more on Medicaid and CHIP with the expansion than they would have without health reform, CBO estimates. Hospitals in expansion states are treating fewer uninsured patients, and the amount of uncompensated care they are providing is declining steeply. Meanwhile, hospitals in the states that haven’t expanded Medicaid continue to provide large amounts of uncompensated care, and the states are missing the opportunity to leverage billions of dollars in new federal funding through the expansion.
- Medicaid expansion supports work. Charges that health reform discourages poor families from working more don’t match reality. In states that have adopted health reform’s Medicaid expansion, poor parents can earn substantially more and retain their Medicaid coverage. In addition, some states have used their program flexibility to further encourage work overall among Medicaid beneficiaries by offering a set of supportive employment services.
Learn more about how Medicaid improves access to health care, its long-term benefits, and why states should expand Medicaid: www.cbpp.org/medicaid-works
Topics:
Policy Basics
Health
Report
States Are Using Flexibility to Create Successful, Innovative Medicaid Programs
June 13, 2016
Report
Medicaid Expansion Producing State Savings and Connecting Vulnerable Groups to Care
June 15, 2016
Stay up to date
Receive the latest news and reports from the Center