BEYOND THE NUMBERS
Despite health reform’s Medicaid expansion to more low-income adults, some states are still paying for uninsured adults’ health care through uncompensated care pools. As we explain in two new papers, Medicaid expansion is a better way to address uncompensated care.
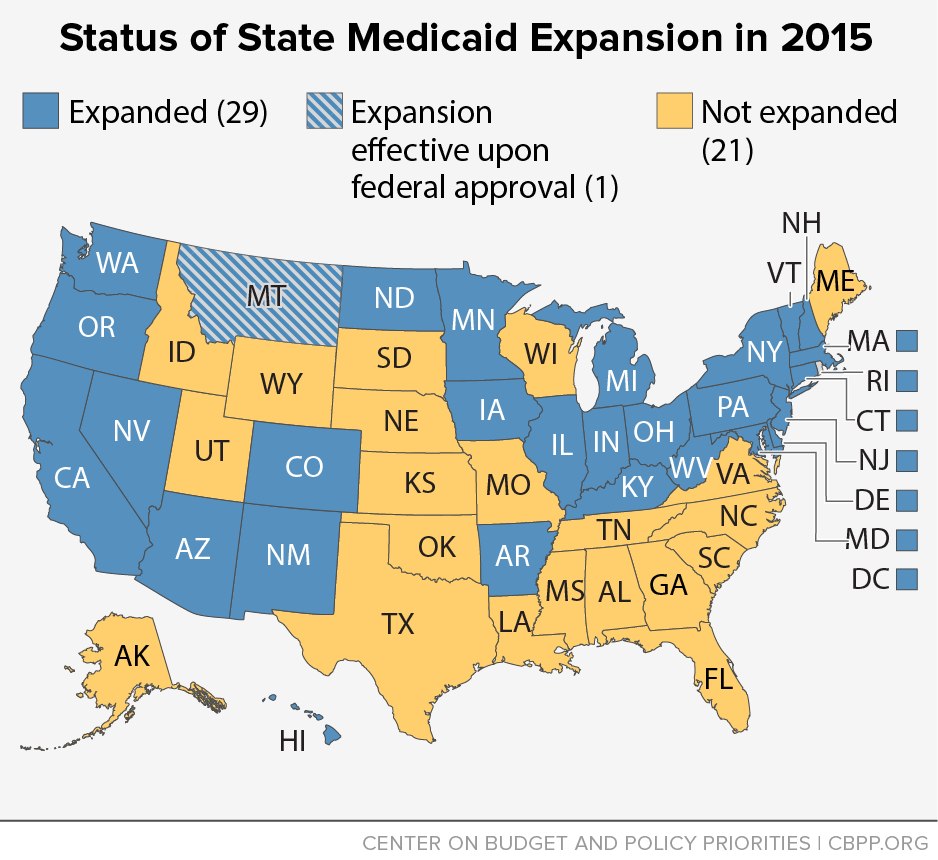
Today’s paper by Jesse Cross-Call shows how Medicaid expansion is cutting the number of uninsured Americans, significantly reducing the uncompensated care that hospitals deliver and saving states money. (See the map below for the states that have expanded Medicaid.) The report explains how Kentucky and Arkansas, for example, have cut the number of uninsured people in half and saved tens of millions of dollars.
The paper also describes how almost immediately after health reform’s major coverage provisions took effect in 2014, hospitals in states that expanded Medicaid reported (1) higher-than-expected revenues and (2) a shift to providing more care to patients with Medicaid coverage and less to uninsured patients. For instance, Community Health Systems, a nation-wide hospital chain, experienced a 72 percent drop in uninsured admissions at its hospitals in 12 states that expanded Medicaid and no change in 17 states that did not.
By contrast, Jessica Schubel and I wrote yesterday about Florida, which hasn’t expanded Medicaid. The Centers for Medicare and Medicaid Services (CMS) won’t extend Florida’s Low-Income Pool, which provides funding to health care providers to help finance uncompensated care, without significant changes. After the current pool expires at the end of June, federal matching funds will no longer be available to finance health care for people who could be covered through Medicaid. CMS also expects Florida and other states with uncompensated care pools to pay providers enough to ensure that Medicaid beneficiaries have adequate access to care.
As Florida’s legislature considers expanding Medicaid, policymakers should recognize the expansion’s positive impact in states like Arkansas and Kentucky — and the benefits of covering the state’s low-income adults through Medicaid.