BEYOND THE NUMBERS
Another 3,815 Arkansans Lost Medicaid in November Due to Rigid Work Requirement
Some 3,815 Arkansas Medicaid beneficiaries lost coverage on November 1 for not reporting at least 80 hours of work or work-related activities for three months, the state reports. That brings to 12,277 the number of beneficiaries who have lost coverage since the state implemented its rigid work requirement in June. They won’t be able to get Medicaid coverage for the rest of 2018 even if they report 80 hours of work or work-related activities in future months or become exempt from the requirement due to illness or other reasons.
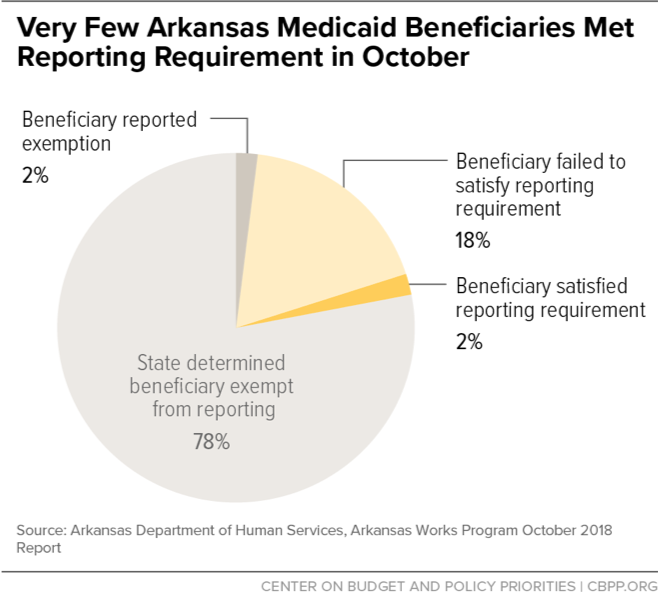
More Arkansans almost certainly will lose their Medicaid in the months ahead. Over 12,000 beneficiaries (18 percent of those subject to the work requirement) didn’t report sufficient work hours in October (see chart). Another 80 percent were exempt or were requesting an exemption. Just 2 percent satisfied the reporting requirement — a share that hasn’t risen since the state implemented the requirement in June. Meanwhile, over 6,000 beneficiaries have two months of non-compliance and will lose coverage if they have one more.
The large coverage losses have generated concern from the nonpartisan Medicaid and CHIP Payment and Access Commission (MACPAC), which advises Congress on Medicaid and Children’s Health Insurance Program (CHIP) policy. In a letter to Health and Human Services Secretary Alex Azar, MACPAC stated that the “low level of reporting is a strong warning signal that the current process may not be structured in a way that provides individuals an opportunity to succeed, with high stakes for beneficiaries who fail.” MACPAC requested that the Secretary pause Arkansas’ disenrollments until the state and federal government can improve awareness and compliance and finalize robust monitoring and evaluation methods.
MACPAC and others also expressed concern that Arkansas doesn’t have an approved plan in place to evaluate the waiver’s success in meeting its stated goals — nor has it issued a request for proposals for an evaluator. The Centers for Medicare and Medicaid Services sent the state a letter on November 1 raising concerns with its draft evaluation design.
Further, Arkansas isn’t protecting vulnerable beneficiaries with disabilities. It hasn’t adequately explained beneficiaries’ rights under the Americans with Disabilities Act and it lacks a comprehensive system for providing reasonable modifications to protect people with disabilities, such as modifying the hourly requirement or providing support to help people meet the reporting requirement. Due to the lack of protections and the design of the work requirement itself, individuals with disabilities are losing coverage and may face serious harm as a result.
The 12,000 beneficiaries who have lost coverage thus far will be eligible to re-enroll this month for coverage effective January 1, and their three-month “clock” will restart then. Considering that many didn’t know they were subject to a work requirement, however, it’s unlikely that a large number of beneficiaries will understand that they are again eligible and will re-enroll for January coverage.
Moreover, the number of beneficiaries subject to the work requirement will rise in January as Arkansas begins phasing in beneficiaries aged 19 to 29. Between January and April, Arkansas will subject about 45,000 more beneficiaries to the work requirement, putting their Medicaid coverage at risk if they, too, can’t navigate the state’s complex rules and reporting requirements.