- Home
- Opportunities For States To Coordinate M...
Opportunities for States to Coordinate Medicaid and SNAP Renewals
Jennifer Wagner and Alicia Huguelet[1]
About three-quarters of households receiving Supplemental Nutrition Assistance Program (SNAP, formerly food stamps) benefits in 2014 had at least one member receiving health coverage through Medicaid or the Children’s Health Insurance Program (CHIP),[2] and even more SNAP households may be eligible for one of those programs. This overlap in eligibility and participation provides opportunities for states to coordinate their policies and processes to improve administration, customer service, and program participation.
One key opportunity exists when families renew their eligibility for SNAP and Medicaid. Eligible households can lose benefits when they don’t complete the renewal process, either because they didn’t submit all required paperwork or because the state didn’t process their paperwork in a timely manner. In these cases, the household remains eligible for assistance and frequently reapplies for benefits within a few months. This process, known as churn, is costly for participants (who go without needed assistance) and for state agencies (which must process new applications).[3]
States can address churn by coordinating Medicaid and SNAP renewals as they modernize their eligibility systems. State and county agencies administering health and human service programs, including Medicaid and SNAP, are implementing new eligibility systems and policies under the Affordable Care Act (ACA). Due to similarities in eligibility for these two programs, many states are better integrating Medicaid and SNAP through data sharing, coordinated policies, and inclusion of both programs in the same eligibility systems as they streamline and modernize their public benefits delivery systems.
Through interviews and site visits with agencies administering these programs, we have identified four major strategies states can use, alone or in combination, to improve integration, streamline operations, and help eligible families keep their benefits at renewal.
We focus on households where the SNAP-Medicaid eligibility overlap is most likely to occur: households without elderly or disabled members, which represent the majority of participants in both programs. The four strategies to coordinate renewals are:
- Using SNAP income data for Medicaid renewals. Data gathered for a SNAP renewal can be used to renew Medicaid even before the Medicaid renewal is due. In addition, when a Medicaid renewal does come due, states can use income information in the SNAP file to complete the Medicaid renewal without requiring additional information from the participant.
- Aligning renewal processes when SNAP and Medicaid are due at the same time. When Medicaid and SNAP renewals are due at the same time, states can align their notices and procedures to maximize coordination and minimize participant confusion.
- Streamlined Enrollment. States can use Streamlined Enrollment to renew Medicaid eligibility for a certain subset of SNAP households automatically, based on the fact that they receive SNAP. (This strategy differs from the first strategy outlined above, in which the state uses income information from SNAP to recalculate a household’s ongoing eligibility for Medicaid.)
- Express Lane Eligibility. States can use Express Lane Eligibility to renew Medicaid for children in households receiving SNAP without requiring additional information.
Although states vary widely in their existing levels of integration between Medicaid and SNAP, the technological sophistication of their eligibility systems, and whether they have expanded Medicaid under the ACA, each state can implement one or more of these strategies to coordinate renewals. In so doing, it can help participants retain their benefits while significantly reducing administrative burdens on state and county eligibility workers as they touch cases less often, deal with fewer inquiries regarding discontinued benefits, and process fewer re-applications.
Why Coordinate Medicaid and SNAP Renewals?
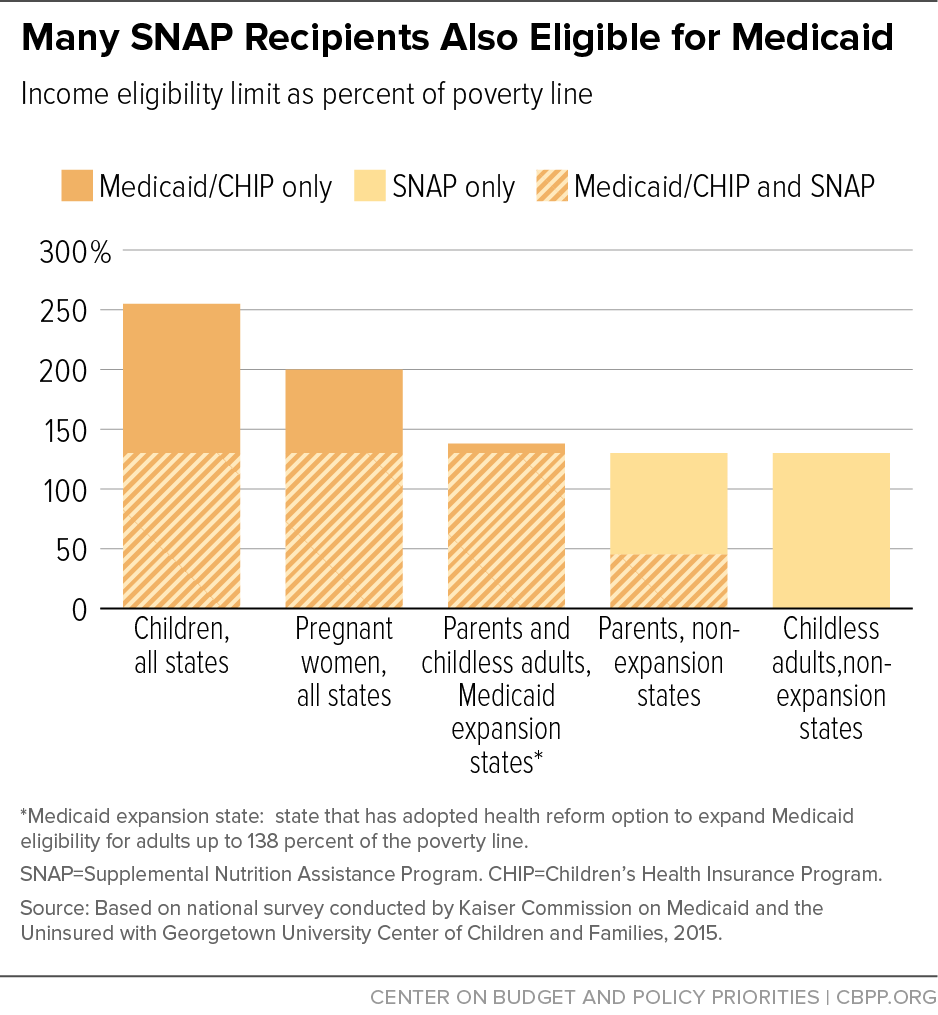
About three-quarters of SNAP households had at least one member receiving Medicaid or CHIP in 2014. To qualify for SNAP, households generally must have gross income below 130 percent of the poverty line. Medicaid eligibility varies among states and types of participant. In states that have expanded Medicaid for adults under the ACA, the minimum eligibility threshold is 138 percent of the poverty line. In most states that haven’t expanded Medicaid, adults without children aren’t eligible at all and parents are eligible at lower income levels. Children in all states are eligible for either Medicaid or CHIP at income levels higher than the SNAP eligibility threshold. (See Figure 1.)
Similarities also exist between SNAP’s and Medicaid’s processes for applying and determining eligibility. Households newly applying for Medicaid and/or SNAP must submit an application with information on who is in the household, their citizenship and immigration status, and what income they receive. State or county eligibility workers verify that information using available data sources as well as documentation the applicant submits, such as pay stubs. After approval, participants must report certain changes in their income or household situation, and states periodically renew eligibility by examining information the participants report as well as available data sources to determine if households remain eligible.
At renewal, the risk exists that financially eligible participants will lose eligibility. Participants may find the renewal process confusing or may not receive the renewal notice, or the state agency may not process documents in a timely manner. In most cases, households that lose benefits at renewal are still low income and quickly come back to the agency to reapply in order to reinstate their benefits. This “churn” in participation means that households go without needed benefits until they reapply and re-establish their eligibility. It also raises administrative costs for state agencies, which must respond to inquiries from households about their lost benefits and process their applications to re-establish eligibility.
Seventeen to 28 percent of SNAP households experienced churn in 2011, according to a recent Urban Institute study in six states.[4] This means that millions of participants lost benefits, only to reapply within a few months. The study notes that while the causes of churn are complex, procedural difficulties during renewal are a significant factor. In the six states, 66 to 90 percent of churn occurred upon renewal. Both state agencies and community organizations identified reducing burdens on participants at renewal — through approaches such as clearer notices and aligned renewals — as a way to reduce churn. Churn raised state administrative costs by an estimated $80 per case, according to the study.
Churn also raises costs for insurers and clinics when they have to re-enroll or re-register a patient. Further, even short gaps in coverage can lead to interruptions in care that can result in a decline in health, greater use of emergency rooms, and/or higher hospitalization rates.[5]
One of the most effective state strategies to reduce churn is coordinate renewals across the programs in which a family participates in order to reduce the number of notices that households receive, the number of forms and documents they must submit, and the number of actions eligibility workers must take to renew coverage. By coordinating the renewal process for the millions of people receiving both Medicaid and SNAP, states can increase the share of eligible participants who successfully renew their eligibility, increasing participation in these critical programs. Minimizing churn can also substantially reduce costs — for both participants and governments.
Medicaid and SNAP Renewal Policies
The ACA significantly changed the policies governing Medicaid eligibility determinations and renewals. (See the Appendix for details on renewal policies for Medicaid and SNAP.) For many Medicaid households, including children, parents, and newly eligible adults, states must now use Modified Adjusted Gross Income (MAGI), which relies on income tax rules to define household size and countable income. For Medicaid participants whose eligibility is calculated using MAGI, cases must be renewed no more frequently than every 12 months.[6] The state agency must first attempt to conduct an ex parte renewal by reviewing electronic data sources to see if it can renew eligibility without requiring information from the participant (see Box 1):
- If the agency confirms that the participant remains eligible using available information, it sends the participant a notice with the information used to make that determination and directs the participant to notify the agency if any information is incorrect. The participant need not return the form if the information is correct.
- If the agency cannot confirm ongoing eligibility using available information, it sends the participant a renewal form pre-populated with available information and with instructions to provide missing information, update information as needed, and return the form with any required supporting documents.
Box 1: Ex Parte Medicaid Renewals
States must conduct ex parte (meaning “by one side”) renewals for certain Medicaid cases. This means that states must attempt to renew a Medicaid participant’s eligibility based on available information, using information in the participant’s case file as well as electronic sources such as Social Security Administration data, quarterly wage data, and information in a SNAP file. The state can only require additional information from the participant if the information indicates the participant is no longer eligible or there is insufficient information to make a determination. The success rate of ex parte renewals completed without requiring information from the participant depends on the state’s data sources and the standards it applies, but the higher the success rate, the lower the possibility for churn. Ex parte renewals are sometimes referred to as “administrative” or “passive” renewals.
Medicaid eligibility doesn’t depend on a participant’s precise income. As long as the electronic information shows income is below the applicable eligibility threshold, the agency may renew Medicaid eligibility without requiring pay stubs or other documentation.[7], [8]
In SNAP, most households have a six- or 12-month certification period[9] and must have some contact with the state agency before that period ends to continue receiving benefits. About 45 days before a household’s eligibility expires, the state sends the household a form explaining that its benefits will end unless it takes action to recertify. Households must complete, sign, and return the renewal form, along with supporting information such as pay stubs, to continue receiving benefits. In addition, most households are required to complete an interview, either in person or over the phone, every 12 months.[10]
Households approved for 12 months often must complete an interim report (also known as a periodic report) halfway through the certification.[11] While the interim report generally includes fewer questions than a full renewal and only requires participants to report changes (such as a change in source of income), participants still must complete, sign, and return the form to continue receiving benefits. In some states, if no changes are reported on the interim report, the state automatically continues eligibility without requiring further documentation or a review of electronic data sources. Other states have a more thorough interim report process, checking electronic data sources for all households — even if they report no changes — before continuing benefits.
SNAP benefits vary based on a household’s income and circumstances. Although the average benefit is about $125 per person per month,[12] a household of three may receive up to $511 per month.[13] State agencies can electronically verify the amount of certain types of household income, such as Social Security and unemployment benefits, but they often can’t electronically verify the amount of earned income since few data sources are current enough to provide recent income. As a result, states often require households with earnings to provide pay stubs to verify their income.
Interactions Between SNAP and Medicaid at Renewal
Prior to the ACA, many states conducted joint renewals for SNAP and Medicaid. They often had households return a single renewal form along with supporting information and evaluated continued eligibility for both programs. States now find it more challenging to conduct joint renewals because the renewal processes differ in key areas:
- In SNAP, households lose eligibility at the end of their certification period unless they reapply and re-establish eligibility. The household must provide information showing that it still meets the eligibility requirements and submit a signed application form.
- In contrast, Medicaid approaches renewals from the perspective that the participant is likely still eligible, and the state agency uses available data to confirm ongoing eligibility or call eligibility into question. Many participants don’t have to return a form to renew their coverage.
Although the ACA widened the differences between Medicaid and SNAP in this area, it also provided an impetus for greater integration. Medicaid regulations now specify SNAP as a data source that states can use for Medicaid eligibility determinations.[14] Further, the ACA’s enhanced funding for integrated technology systems[15] recognizes the overlap between these programs and the significant opportunity to modernize states’ overall benefit delivery systems. As states modify their eligibility systems, they can expand coordination between Medicaid and SNAP.
To reap the benefits of greater coordination, though, states must overcome certain hurdles:
-
Differences in federal rules. SNAP and Medicaid rules differ for determining who is in a household, what income to count, how to use electronic data, and the timing of notices.
-
Complexity of eligibility systems. Although eligibility systems allow for automation of rules across programs, changing the systems requires significant lead time, time-consuming design work, and often vendor involvement.
-
Involvement of multiple agencies. Medicaid and SNAP reside in different agencies in many states, requiring coordination of policy and process between agencies with different priorities.
- Competing priorities. Some states are torn between prioritizing integration across health coverage programs (Medicaid, CHIP, and the marketplaces) and integration across health and human services programs.
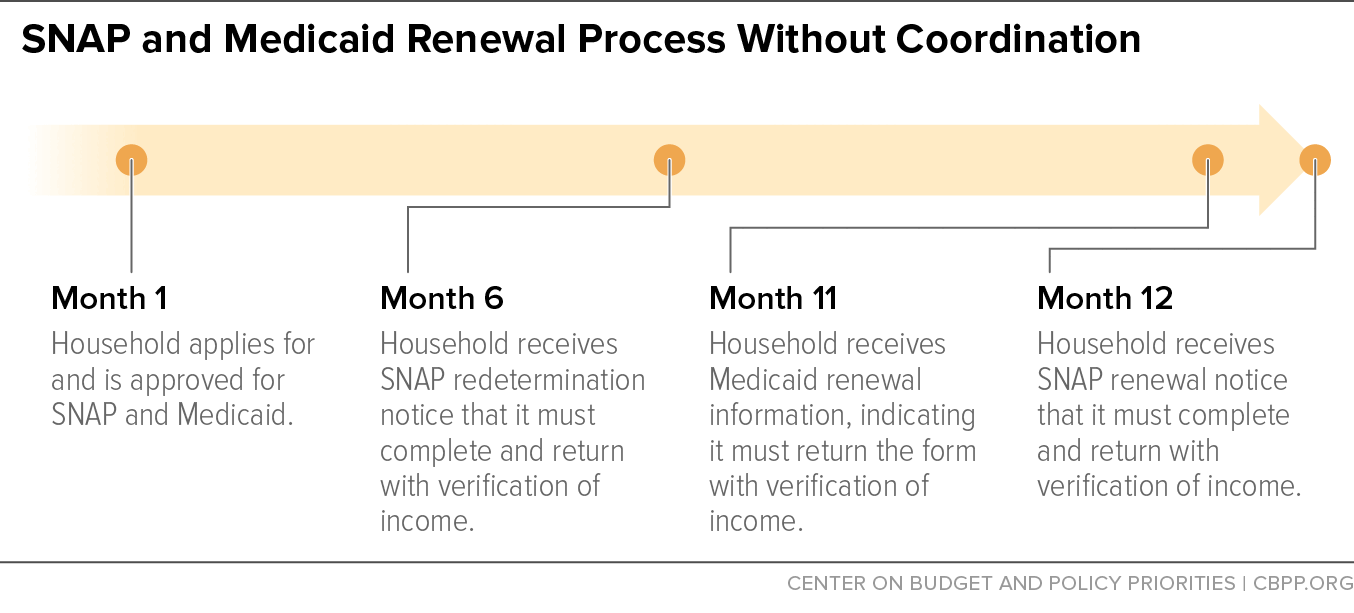
The benefits of coordination for states and families outweigh these challenges, however. Consider the experience of a household enrolled in both SNAP and Medicaid when the renewal processes are not coordinated. As Figure 2 shows, the household receives a redetermination notice from SNAP six months after its case is approved and must return the form along with supporting documents such as pay stubs. A few months later, if the Medicaid agency can’t confirm ongoing eligibility using available data sources, the household must again provide verification of income. Around the same time, the household is due for its next SNAP renewal and must return a form with the same pay stubs it just provided to the Medicaid agency. If the household doesn’t complete all of these required steps or erroneously believes that providing information to one program counts for both programs, it will lose benefits and have to reapply, likely once more having to provide proof of income and other eligibility factors.
The four renewal coordination strategies described below can enable states to improve integration, streamline operations, and reduce costly churn, ultimately helping low-income families retain the support on which they rely.
Strategies to Coordinate Medicaid and SNAP Renewals
We asked a diverse group of state health and human service agencies to complete a web-based survey about how they approach Medicaid and SNAP renewals and followed up with phone interviews and site visits to better understand the technical details of their policies and processes. The states we selected represent the different ways states can administer SNAP and Medicaid. In the areas of system and workforce integration, they ranged from states where both programs are in the same eligibility system and managed by the same staff to states where the programs have completely different eligibility systems and are managed by different agencies and staffs. They also included states that have expanded Medicaid under the ACA as well as those that haven’t, and states operating state-based and federally facilitated marketplaces.
Using this information, we identified four primary strategies that states are using or considering to coordinate Medicaid and SNAP renewals; states may use them alone or in combination. One way to consider the application of these strategies is to look at the different renewal scenarios a household receiving SNAP and Medicaid may encounter. Sometimes the SNAP case is due for renewal but Medicaid isn’t, sometimes both programs are due at the same time, and sometimes only the Medicaid case is due. As summarized in Table 1 and highlighted in the state profiles below, different strategies may be most useful in each scenario, and states may want to target their use based on the scenarios that families will most likely encounter.
1. Using SNAP Income Data for Medicaid Renewals
Medicaid regulations require agencies to use trusted electronic data sources to determine Medicaid eligibility at application and renewal, and they specifically identify SNAP data as a useful source. Because SNAP cases are generally reviewed more frequently and with precise verification of income, income information recorded from SNAP can be used for ex parte Medicaid renewals — either for an early Medicaid renewal in conjunction with a SNAP renewal or for a Medicaid renewal when it’s due.
Conducting Early Medicaid Renewal When SNAP Renewal Due
For most SNAP households, states conduct a recertification or process an interim report every six months. For households receiving SNAP and Medicaid, a SNAP renewal will often be due before a Medicaid renewal since Medicaid cases are certified for 12 months. States may use the information gathered from the SNAP renewal to conduct a Medicaid renewal, even if the Medicaid renewal isn’t yet due.[16], [17] This could be done manually: a caseworker could use information in the SNAP renewal to complete a MAGI Medicaid eligibility determination. It could also be done in an automated fashion: the state could program its eligibility system to do a MAGI Medicaid determination based on the income information gathered for SNAP, appropriately sorting the income by type and recipient and applying MAGI rules.
Box 2: Early Medicaid Renewals Still Allowed Under ACA
Some states have questioned whether the Centers for Medicare & Medicaid Services (CMS) regulation prohibiting renewals more frequently than every 12 months allows states to conduct an early Medicaid renewal in conjunction with a SNAP renewal or change report, if the Medicaid case isn’t due for renewal. (Several states used this practice, sometimes known as “rolling renewal,” prior to the ACA.) While states can’t initiate a renewal more frequently than every 12 months, they must act on changes that become known to them during the 12-month period. If, while reviewing those changes, the agency has sufficient information to renew Medicaid eligibility, it may begin a new 12-month eligibility period. Information submitted to the state as part of a SNAP renewal is considered a change that becomes known to the agency. See 42 C.F.R § 435.916 (d).
Some level of system or workforce integration, however, is required to use income information gathered for SNAP to renew eligibility for Medicaid and grant the household a new 12-month certification period if it remains eligible.
When a SNAP renewal is due but a Medicaid renewal isn’t, states must not take negative action on a Medicaid case if the household’s SNAP case is closed for a procedural reason, such as failure to return the renewal form, provide required verification, or complete a required SNAP interview. In these instances, Medicaid continues and a renewal will be completed at the end of the Medicaid eligibility period. If, however, the information gathered during the SNAP renewal indicates the household is no longer eligible for Medicaid, the state must end Medicaid for household members not protected by continuous eligibility provisions, subject to notice and hearing requirements.[18]
A state can always use this strategy during a full SNAP recertification, but using it during a SNAP interim report is contingent on the state’s process for its interim report. Some states ask the household if any key circumstances have changed, such as a switch from part- to full-time work or a change in hourly wages; if the participant reports no changes, the state renews the household for another six months without checking electronic data sources. Other states consult electronic data sources at the time of the interim report even if the household reports no changes. A state may push forward Medicaid during the SNAP interim report only for households for which they check electronic data sources — states may not renew Medicaid without consulting available data sources.
States that use or are considering an interim report for SNAP can weigh the costs and benefits of checking electronic sources for all participants, even if they report no changes. While not checking data sources allows for significant workload savings, checking data sources on all cases improves payment accuracy and facilitates coordination with Medicaid. States may also elect to push forward Medicaid only for households reporting a change on a SNAP interim report that leads to a check of data sources. This allows the benefit of automation when no changes are reported, but maximizes coordination when the reported change requires a more thorough review.
Using a SNAP renewal to conduct an early Medicaid renewal allows SNAP to stay “ahead” of Medicaid because the Medicaid case is granted a new 12-month certification period and SNAP is reviewed again in six months. This ensures that for most individuals participating in both SNAP and Medicaid, a Medicaid-only renewal never comes due, so they don’t face multiple and potentially conflicting requests for information and notices. To facilitate this process, states must ensure that their SNAP renewal forms include all questions necessary for a Medicaid renewal, such as information about the household’s tax filing status.[19]
State Profile: Using SNAP Income Data for Medical Renewal When SNAP Due, Medicaid Not Due — Utah
Utah workers manually push forward Medicaid when a SNAP renewal is completed.
Utah has an integrated eligibility system and workforce for Medicaid and SNAP cases. When updating information during a SNAP renewal, the state worker manually prompts the system to conduct a Medicaid renewal, even if the Medicaid eligibility period hasn’t ended. Households whose ongoing Medicaid eligibility is approved receive a new 12-month eligibility period. Even though the worker must prompt the system to initiate the Medicaid review, most workers complete this step as it is less burdensome for participants and saves the worker the effort of conducting a separate Medicaid renewal in the future. Workers conduct Medicaid renewals for many of their SNAP cases using this strategy.
Using SNAP Data to Renew Medicaid When SNAP Isn’t Due
SNAP income information is also useful when a Medicaid renewal is due but a SNAP renewal isn’t. Since most SNAP cases are reviewed every six months and SNAP has rigorous verification requirements, the income information on the SNAP file is generally current and reliable. At Medicaid renewal, the eligibility worker or eligibility system can use the SNAP information to re-calculate Medicaid eligibility, thereby completing an ex parte renewal without participant action.
State Profiles: Using SNAP Income Data for Medical Renewal When Medicaid Due, SNAP Not Due — Idaho and Alabama
Idaho’s eligibility system uses SNAP data to perform ex parte Medicaid renewals.
Idaho has an integrated eligibility system and an integrated workforce. The eligibility system automatically checks SNAP data when attempting an ex parte Medicaid renewal. For households enrolled in both programs, the SNAP data is used to determine ongoing eligibility for Medicaid. State officials expect this process to yield a very high match rate, resulting in the majority of dually enrolled households being automatically renewed for Medicaid without requiring action by participants.
Alabama eligibility workers consult SNAP data when performing ex parte Medicaid renewals.
SNAP and Medicaid cases in Alabama involve different eligibility systems and different eligibility workers. Alabama uses SNAP data when determining whether parents remain eligible for Medicaid at renewal. (Children can be automatically renewed using Express Lane Eligibility.) The process requires manual action by the eligibility worker to view the electronic SNAP file and use the income data to determine the parents’ eligibility.
If the state has an integrated eligibility system, the system could directly use the SNAP income information to conduct an ex parte renewal. If the state has separate eligibility systems, SNAP can be “pinged” just like an unemployment or Social Security database, and the income information from SNAP can be used to determine if the household remains eligible for Medicaid. Or, if the Medicaid renewal is being handled manually, a Medicaid worker could review income information or documents in the SNAP system to determine ongoing Medicaid eligibility.
2. Aligning Renewal Processes When SNAP and Medicaid Are Due at the Same Time
Many states synchronized certification periods so that SNAP and Medicaid are due for renewal in the same month, which allowed the state to send a single renewal form to the household that the household could sign and return to continue receiving both Medicaid and SNAP. But the timing and logistics of aligning renewals due at the same time have become more complicated now that states must attempt an ex parte Medicaid renewal before requiring documentation from the participant. States have ways to streamline the process, however. States can ensure that households receive as few notices as possible, and that the notices provide coherent and consistent instructions.
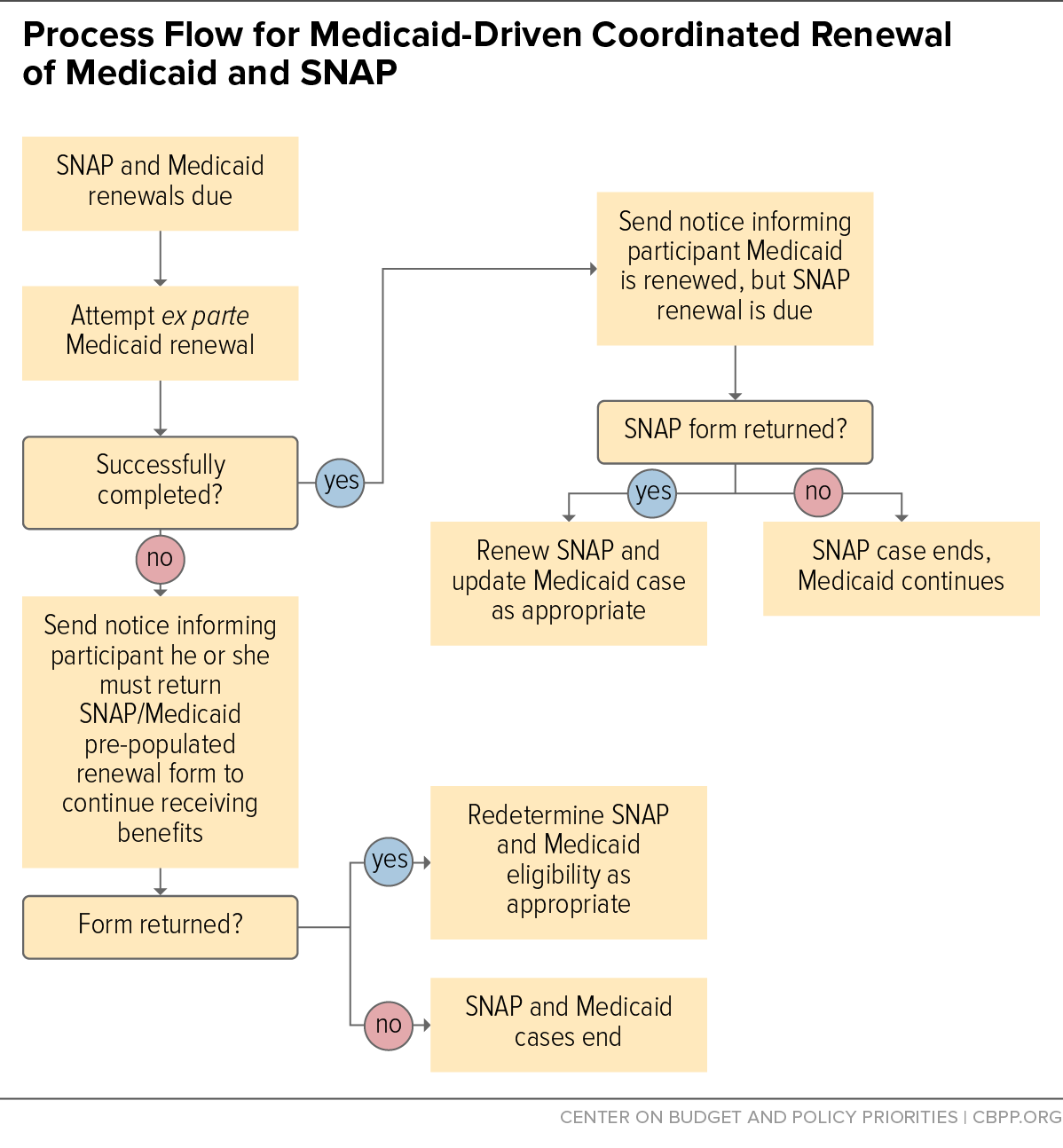
Some states allow one program to drive the renewal process, which determines the directions given for the other program. One option is for the state to attempt the Medicaid ex parte renewal first; if it succeeds, Medicaid can be renewed and the SNAP renewal proceeds as usual. If the SNAP renewal process yields different information than the Medicaid ex parte process, this is considered a change and the state must update the Medicaid case. If the state can’t complete the ex parte Medicaid renewal, it can send the household a unified set of instructions for both the SNAP and Medicaid renewals, which the household must complete and return to continue receiving Medicaid and SNAP. (See Figure 3.)
Alternatively, the state may first attempt the SNAP renewal. If the household provides all required information, the state uses the data to renew both SNAP and Medicaid. If the household doesn’t provide the required information, SNAP benefits end and the caseworker or system attempts to complete an ex parte Medicaid renewal based on available electronic data sources.
Timing is key for these strategies to succeed. When the Medicaid renewal drives the process, the state must complete the ex parte renewal before sending out the SNAP renewal to ensure that the household receives proper instructions. When the SNAP renewal drives the process, the state must leave sufficient time after the SNAP form’s due date for the state to attempt the ex parte Medicaid renewal and send any required notices if the SNAP form isn’t returned.
Aligning the Renewal Process When SNAP and Medicaid Are Due at the Same Time — Utah, Illinois, and Pennsylvania
Utah — Medicaid drives the joint renewal process.
Utah has an integrated eligibility system and integrated workforce and allows the Medicaid ex parte renewal to drive the process. Eligibility workers attempt an ex parte review for Medicaid about two months before the Medicaid certification period ends. If the worker verifies continuing eligibility for Medicaid, the worker sends a notice that the participant is still eligible for Medicaid and a separate renewal notice for SNAP, which the participant must complete and return. If the ex parte process doesn’t verify continuing eligibility for Medicaid, the worker sends a renewal notice for SNAP and Medicaid that the participant must return to continue receiving benefits. Utah conducts early Medicaid renewals in conjunction with SNAP renewals, so the group due for SNAP and Medicaid renewals at the same time is relatively small.
Illinois — Medicaid drives the joint renewal process.
Illinois has an integrated eligibility system and integrated workforce. When the second phase of its eligibility system is implemented in 2016, Medicaid will drive the renewal process. Approximately two months before the end of the certification period for a household receiving Medicaid and SNAP, the system will attempt an automated ex parte review for Medicaid. If the system confirms continuing eligibility for Medicaid, it will send a notice informing the participant that Medicaid has been renewed and instructing the participant to complete and return the enclosed SNAP renewal form. If the ex parte process doesn’t confirm continuing Medicaid eligibility, the system will send a different notice instructing the participant to return the renewal form in order to continue receiving Medicaid and SNAP.
Pennsylvania — SNAP drives the joint renewal process.
Pennsylvania operates with an integrated eligibility system and workforce and allows the SNAP renewal to drive the process. When SNAP and Medicaid are both due for renewal, the state sends out a SNAP renewal form. If the household completes and returns it, the eligibility worker renews both SNAP and Medicaid. If the household doesn’t return the form, the worker ends SNAP benefits and attempts a manual ex parte renewal for Medicaid.
3. Streamlined Enrollment
In 2013, the Centers for Medicare & Medicaid Services (CMS) created a temporary, targeted enrollment option for coordinating SNAP and Medicaid to help states transition to new policies and systems under the ACA.[20] It allows states to rely on participation in SNAP to enroll certain non-elderly, non-disabled SNAP participants in Medicaid automatically.
Several states that expanded Medicaid have used this option, enrolling hundreds of thousands of newly eligible Medicaid participants without requiring them to complete a new application and provide supporting documentations to prove their income. Although the guidance also allows states to use the strategy at renewals, CMS requires that a state make a full MAGI determination within 12 months of using this approach. This effectively prohibits a state from using this methodology on an ongoing basis at renewal.
CMS recently released guidance on a new state plan option that allows states to use a variation on this approach at application or renewal.[21] States first identify participants in SNAP households who are certain to be eligible for Medicaid based on the information already known for SNAP. (About 80 percent of SNAP households with non-elderly, non-disabled members include individuals who are certainly eligible for Medicaid, research shows.[22]) For these participants, receipt of SNAP is considered a determination that their income is below the applicable MAGI-based eligibility level for Medicaid.
Using this state option, states can automatically renew Medicaid cases for certain participants who receive both Medicaid and SNAP (or another program with similar eligibility requirements). The process is similar to Express Lane Eligibility (described below) but, unlike Express Lane Eligibility, can be used for adults.
States can use this strategy when Medicaid is due for renewal even if the state’s systems have only minimal integration, since extensive system interaction isn’t required. For example, a state could program a report from its SNAP system listing all SNAP households meeting the specified criteria; as Medicaid renewals come due, the Medicaid agency could check households against the list and renew Medicaid for those listed as receiving SNAP.
This option also may be helpful for states with large backlogs of overdue Medicaid renewals. It could provide significant relief to state staff, since many Medicaid participants are in households that also receive SNAP.
4. Express Lane Eligibility
Established in the 2009 Children’s Health Insurance Reauthorization Act, Express Lane Eligibility (ELE) allows Medicaid agencies to “borrow” the findings of other low-income programs such as SNAP or TANF in making eligibility determinations for children[23] for Medicaid at application or renewal, even if income calculations differ between the two programs.[24] In other words, the Medicaid eligibility system need not recalculate income eligibility, since the fact that the Medicaid participant is enrolled in SNAP is sufficient to renew Medicaid eligibility. States can use ELE as an outreach tool to enroll participants receiving SNAP into Medicaid, or use it at renewal.
At renewal, states apply this strategy when Medicaid is due regardless of when the SNAP renewal is due. States also can use it to conduct an early Medicaid renewal following a SNAP renewal. It is often effective in systems with minimal integration. The SNAP (and/or TANF) system produces a monthly file of enrollees, and the Medicaid system matches cases due for renewal against that file. If children due for Medicaid renewal also receive SNAP, the state renews their Medicaid eligibility without further action required.
State Profiles: Express Lane Eligibility Medicaid Due — Alabama and South Carolina
Alabama uses enrollment data from SNAP and TANF to automatically renew children’s Medicaid eligibility.
SNAP and Medicaid cases in Alabama involve different eligibility systems and different eligibility workers. The agencies match data from SNAP and TANF with their child-only and family planning Medicaid cases. If the Medicaid participant due for renewal also receives SNAP and/or TANF, the system automatically renews Medicaid eligibility for another 12 months without action by the caseworker.
South Carolina uses enrollment data from SNAP and TANF to automatically renew children’s Medicaid eligibility.
South Carolina has minimal integration between its SNAP and Medicaid systems and eligibility workers. The Medicaid agency receives a file from the SNAP and TANF agency with children currently enrolled in those programs. These children are auto-enrolled for Medicaid benefits. When Medicaid renewals come due, Medicaid participants who also receive SNAP or TANF are automatically renewed without further action by the caseworker.
The specific strateg(ies) a state adopts to better coordinate its SNAP and Medicaid renewal processes will depend primarily on the state’s level of workforce and system integration. Table 1, which shows how the different strategies can apply to different renewal scenarios, lists important features for states to assess when contemplating each of the four strategies.
| TABLE 1 | ||
|---|---|---|
| Features of Coordinated Renewal Strategies | ||
| Scenario | Strategy | Features |
| SNAP Due, Medicaid Not Due |
Use SNAP income data for Medicaid renewal |
|
| Both SNAP and Medicaid Due |
Align renewal processes for SNAP and Medicaid |
|
| Medicaid Due, SNAP Not Due |
Use SNAP income data for Medicaid renewals |
|
|
Streamlined Enrollment |
|
|
|
Express Lane Eligibility |
|
|
Box 3: Adding Other Programs into the Mix
Many families on SNAP and Medicaid also receive assistance from other programs such as the Child Care Assistance Program, Special Supplemental Nutrition Assistance Program for Women, Infants, and Children (WIC), and Low Income Home Energy Assistance Program (LIHEAP). States can use the comprehensive review of income and other information done for SNAP to facilitate applications or renewals for these programs as well. Although other programs may have specific requirements not addressed during a SNAP application or renewal (e.g., work or school schedule for child care), relying on information verified by SNAP can lessen the burden on participants and eligibility workers at application and renewal.
Conclusion: Key Issues to Consider
As states’ policies and eligibility systems continue to evolve, they will benefit from looking carefully at opportunities to coordinate Medicaid and SNAP renewals. Key factors to consider include:
- How the current process works for participants. How many notices do they receive? Are the directions consistent or conflicting? Does the state require them to submit the same documents multiple times?
- Whether states with integrated eligibility systems are maximizing coordination at renewal. What opportunities exist to minimize the number of times a caseworker touches a case?
- How SNAP data can facilitate an ex parte renewal for Medicaid. Can the system pull income information from the SNAP case and use it to determine Medicaid eligibility? Or, can the state use a Medicaid participant’s enrollment in SNAP as the basis for continuing eligibility through Streamlined Enrollment or ELE?
- The costs and benefits of checking electronic data sources at the SNAP interim report for all respondents. On the one hand, states can achieve significant workload savings by processing renewals automatically, without checking electronic sources, for participants who report no changes. On the other hand, this may increase errors and doesn’t allow states to push forward Medicaid renewals at interim SNAP reports.
- How the process works in the county or local office. It is important to talk with participants to see how the current process works, since system or operational challenges can significantly affect policy implementation. What system or process changes might help participants and state or county staff? Where is more training required?
- What data are available to measure churn. How does the state know whether a particular policy or practice is minimizing churn? How can the state measure the impact of changes? Could data be helpful in developing a cost-benefit analysis of proposed changes?
Coordinating Medicaid and SNAP renewals is a critical strategy to reduce churn and improve outcomes for both participants and state agencies. Regardless of their level of system or workforce integration, states have opportunities to simplify the messages to participants, reduce the number of forms they send out, and eliminate unnecessary touches by eligibility workers. As states continue to modernize benefit delivery systems and implement other changes brought about by the ACA, it is an important time to reexamine the coordination of Medicaid and SNAP renewals. This will take time and collaboration across agencies and/or teams, but the potential for improvement makes the effort well worth it. By focusing on opportunities to coordinate at renewal, states can increase retention of eligible participants and significantly reduce duplication of effort.
Acknowledgements
The authors would like to thank January Angeles, Stacy Dean, Shelby Gonzales, Cemeré James, Dottie Rosenbaum, Judy Solomon, and Suzanne Wikle for providing valuable technical and editorial feedback. Thanks also to John Springer and Michele Vaughn who edited the paper and Rob Cady who formatted it.
The Center on Budget and Policy Priorities thanks the following organizations for their support for this paper:
- California HealthCare Foundation (CHCF) based in Oakland, California
- Ford Foundation
- The JPB Foundation
- MAZON: A Jewish Response to Hunger
- Packard Foundation
- W.K. Kellogg Foundation
- Wal-Mart Foundation
| APPENDIX TABLE 1 | ||
|---|---|---|
| Comparison of Medicaid and SNAP Renewal Requirements | ||
| Medicaid | SNAP | |
| Renewal process |
The state agency must use information in the case file and available through data matching (including SNAP):
|
The state agency must notify a household of its expiring certification period and make available a renewal application and a list of required verifications.
|
| Renewal form & signature | The state must not require participants to return a form unless the state is unable to determine continuing eligibility via the ex parte process. | The state must require a signed and dated re-application form as part of the renewal. |
| Interview | The state cannot require an interview as part of the renewal process. | The state must require an interview every 12 months for most participants. |
| Certification period | The state can initiate a renewal only every 12 months, unless there is a change in circumstance that may affect the participant’s eligibility. | The state may choose certification periods of up to 12 months for most households. The majority of states choose a six-month certification period or 12-month certification period with a six-month interim report. |
| Income verification | The state uses electronic verification of income when possible to confirm ongoing eligibility. | The state verifies the exact amount of income through electronic data sources and/or participant documents. |
End Notes
[1] Alicia Huguelet is a senior consultant at Koné Consulting.
[2] CBPP analysis of the Census Bureau’s March 2015 Current Population Survey.
[3] For more information on churn, see Dottie Rosenbaum, “Lessons Churned: Measuring the Impact of Churn in Health and Human Services Programs on Participants and State and Local Agencies,” Center on Budget and Policy Priorities, March 20, 2015, https://www.cbpp.org/research/lessons-churned-measuring-the-impact-of-churn-in-health-and-human-services-programs-on.
[4] Gregory Mills et al., “Understanding the Rates, Causes, and Costs of Churning in the Supplemental Nutrition Assistance Program (SNAP) - Final Report,” prepared by the Urban Institute for the U.S. Department of Agriculture, Food and Nutrition Service, November 2014.
[5] Leighton Ku, Erika Steinmets, and Tyler Bysshe, “Continuity of Medicaid Coverage in an Era of Transition,” George Washington University, November 2015.
[6] 42 CFR §435.916(a).
[7] This approach is commonly referred to as reasonable compatibility. As long as the information attested to by the applicant is reasonably compatible with what the data sources show, the agency should not request further verification. The information is considered reasonably compatible when, for example, the difference doesn’t affect eligibility (i.e., both attested income and data sources show income below the eligibility threshold for the family size).
[8] If, during a renewal, the state determines the household is no longer eligible for the category of assistance it was receiving, the state must consider the household’s eligibility for other insurance affordability programs, including other Medicaid programs or marketplace assistance.
[9] States may issue shorter or longer certification periods for certain populations. For example, SNAP agencies may certify households consisting entirely of elderly and disabled members for 24 months since their income is stable. (Some states have waivers to certify certain elderly households for 36 months.) Households with unemployed childless adults subject to the three-month limit may receive three-month certification periods.
[10] 7 CFR §273.14.
[11] 7 CFR §273.12(a)(5)(iii).
[12] “Chart Book: SNAP Helps Struggling Families Put Food on the Table,” Center on Budget and Policy Priorities, updated January 8, 2015, https://www.cbpp.org/research/food-assistance/chart-book-snap-helps-struggling-families-put-food-on-the-table#part2.
[13] “Quick Guide to SNAP Eligibility and Benefits,” Center on Budget and Policy Priorities, revised November 5, 2015, https://www.cbpp.org/sites/default/files/atoms/files/11-18-08fa.pdf.
[14] 42 CFR §435.948(a)(2).
[15] Under the ACA, the federal government provides enhanced matching funds for states to build or update Medicaid eligibility systems. Further, the federal agencies overseeing Medicaid, SNAP, and Temporary Assistance for Needy Families (TANF) have issued a cost allocation waiver, valid through 2018, encouraging states to maximize these enhanced matching funds for systems shared by other health and human services programs. Many states are taking advantage of this to deploy new or enhanced integrated eligibility systems. See Terri Shaw and Lucy Streett, in collaboration with Shelby Gonzales and Dottie Rosenbaum, “State Innovations in Horizontal Integration: Leveraging Technology for Health and Human Services,” Center on Budget and Policy Priorities, updated March 24, 2015, https://www.cbpp.org/research/state-innovations-in-horizontal-integration-leveraging-technology-for-health-and-human.
[16] States may not, however, conduct an early SNAP renewal in conjunction with a Medicaid renewal due to SNAP’s requirement for a signed renewal form and more precise income verification.
[17] States may also apply this strategy when a Medicaid participant applies for SNAP and when a change is reported for SNAP or Medicaid. The state can conduct an early renewal of Medicaid if it has verified sufficient eligibility factors, including income, in processing the SNAP application or the change report.
[18] Continuous eligibility is a Medicaid option that allows certain participants to receive Medicaid for a full 12 months regardless of changes in the household situation.
[19] Any questions on the SNAP renewal form that are not required for SNAP, such as tax filing status, must be identified as not mandatory for SNAP. If the household doesn’t answer these questions, the agency should not deny the SNAP recertification even if it can’t complete the early Medicaid renewal.
[20] CMS Letter RE: Facilitating Medicaid and CHIP Enrollment and Renewal in 2014, May 17, 2013, http://www.medicaid.gov/Federal-Policy-Guidance/downloads/SHO-13-003.pdf.
[21] CMS Letter RE: Policy Options for Using SNAP to Determine Medicaid Eligibility and an Update on Targeted Enrollment Strategies, August 31, 2015, http://www.medicaid.gov/federal-policy-guidance/downloads/sho-15-001.pdf.
[22] Dottie Rosenbaum, Shelby Gonzales, and Danilo Trisi, “A Technical Assessment of SNAP and Medicaid Financial Eligibility under the Affordable Care Act (ACA),” Center on Budget and Policy Priorities, revised June 6, 2013, https://www.cbpp.org/research/food-assistance/a-technical-assessment-of-snap-and-medicaid-financial-eligibility-under-the.
[23] Before the ACA was implemented, CMS approved a “section 1115” waiver for Massachusetts to expand ELE to include adults. It is unclear if CMS would approve similar new waiver requests in light of post-ACA rule changes. Also, Alabama uses ELE to enroll adults in its family planning program.
[24] Laura Parisi and Jennifer Sullivan, “Express Lane Eligibility: What Is It and How Does It Work?” Families USA Issue Brief, October 2010.
More from the Authors