- Home
- Lessons Churned: Measuring The Impact Of...
Lessons Churned: Measuring the Impact of Churn in Health and Human Services Programs on Participants and State and Local Agencies
Public benefit programs for low-income individuals and families typically require households to apply, establish eligibility, and then, at subsequent regular intervals, to re-establish eligibility. While periodically reviewing eligibility is important for ensuring that benefits are properly targeted to individuals and families that remain eligible for assistance, the redetermination process can result in eligible households temporarily losing eligibility, experiencing a short period without benefits, and then reapplying — a phenomenon sometimes called “churn.”
Churn entails costs for recipients — in lost benefits, short-term hardship, and effort reapplying — and also for state agencies, because processing a new application usually involves more resources, such as staff time, than re-determining continuing eligibility. In recent years, state agencies and other policymakers and advocates have begun to pay closer attention to churn in state-administered public assistance programs such as Medicaid, the Supplemental Nutrition Assistance Program (SNAP), and Child Care assistance. Reducing churn is seen as a win-win: it can both increase program efficiency for state agencies and help ensure that eligible people retain benefits that can improve their well-being. Some states have begun to assess churn through data-driven approaches, but there is not yet a standard way to measure churn. Recent developments, such as changes brought about by the implementation of the Affordable Care Act (ACA) and the recent reauthorization of the Child Care and Development Block Grant (CCDBG), which both include components designed to improve continuity of care, present new opportunities for reducing churn.
Box 1: Work Support Strategies
This report was written in coordination with the Work Support Strategies Project. Work Support Strategies (WSS) is a multiyear, multi-state initiative to help low-income families get and keep the package of work supports for which they are eligible. WSS has been working directly with Colorado, Idaho, Illinois, North Carolina, Rhode Island, and South Carolina since 2011. Through grants and expert technical assistance, WSS helps states reform and align the systems delivering work support programs intended to increase families’ well-being and stability — particularly SNAP, Medicaid and the Children’s Health Insurance Program (CHIP), and child care assistance through the Child Care and Development Block Grant. Through WSS states seek to streamline and integrate service delivery, use 21st Century technology, and apply innovative business processes to improve administrative efficiency and reduce burden on states and working families.
The Center on Budget and Policy Priorities coordinates the Technical Assistance for the project. Our work in this effort helped to inform this paper.
For more information about WSS, see: http://www.clasp.org/issues/work-support-strategies
This paper presents preliminary lessons learned about churn derived from the states participating in the Work Support Strategies project (WSS, see box) and other states, and highlights recent research. It first defines churn and outlines its consequences, then explores approaches to measuring churn, and finally looks at possible approaches to reducing churn. State policy officials and others may find this information useful as they develop policies and processes in health and human services programs to monitor and reduce churn.
What Is “Churn”?
In the context of public benefit programs, “churn,” which brings to mind swirling agitation, is used to describe unnecessary or unproductive cycling of families and individuals off and back on benefit coverage.
Public benefit programs require periodic reassessment of families’ eligibility for benefits in order to maintain program integrity and to target federal and state budgetary resources to families with the greatest need for assistance. Ideally, such renewals would be based only on financial eligibility (i.e., families would lose coverage at renewal only because of changes in household income and other household characteristics that made them ineligible.) However, since much of the information needed to determine eligibility is available only from household members, eligibility determinations require interactions between state agencies and families, and so opportunities for procedural problems arise – when either families or the state do not take a required action during the window in which it must occur.
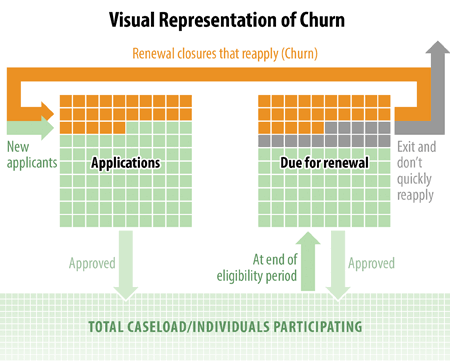
Figure 1 presents a simplified visual representation of a state’s caseload for a month and how churn might affect the flow of cases. In any given month, most program participants are in the middle of an eligibility period (shown as the green box at the bottom). Each month states process new applications (to the left) and approve eligibility for applicants who meet the program’s eligibility rules. After some number of months of eligibility, usually six months or a year, cases come up for “renewal,” a periodic reassessment of their eligibility (to the right in the figure).[1] During a window of time (usually about six weeks) states and families must take certain actions to enable the state to reassess eligibility. Many cases successfully renew, but some do not because they are ineligible, because they choose not to reapply, or because, although they wish to continue to receive benefits, they experience a procedural problem in the process. “Churning” occurs when eligible families exit the program only to reapply for benefits within a short period of time (as shown in orange in figure 1.)[2]
Churn is problematic for participants: their families lose benefits that are crucial to making ends meet for a period of time, despite remaining eligible for help. For states, it can mean avoidable “re-work,” for example, re-processing eligibility (or other tasks).[3]
For purposes of this paper, we emphasize “churn” that occurs at the time households are expected to “renew” eligibility, which researchers have found is the principle time that churn occurs. A recent study of churn in SNAP found, in the six states studied, that between 68 percent and 90 percent of the program exits that triggered a churn spell occurred at recertification.[4]
Because the income, expenses, and other circumstances of low-income families are often volatile, some movement off and on benefits, or among health coverage options, is inevitable and to be expected. (See box 3.) People start jobs and then lose them, or reunite with a partner and then separate again. It is not uncommon for low-income individuals to anticipate that their circumstances will improve and they will not need help from a government program anymore, and then realize they cannot make ends meet and reapply for help. This type of churn may be unavoidable.
However, it also is common for families that have not experienced a change, but rather remain continuously eligible, to experience a short break in participation because of a procedural issue in the renewal process. It is quite unusual for states or counties to purposefully create procedural barriers for families in order to deter participation. More often the procedural requirements are not well understood, are difficult for families to comply with, or are the result of over-burdened state processes that cannot respond in a timely fashion when families do comply.
Typically state agencies and families must take a number of steps, in proper sequence and within a specified window of time, to maintain benefits or coverage at the time of a scheduled renewal. The renewal process varies depending on the state and program, and also is changing in significant ways, especially for health coverage under the ACA and child care under its recent reauthorization (see box 4).[5] For illustrative purposes, consider the renewal process that is typical for SNAP:
- In the month before the last month of the eligibility period the state contacts the family by a mailed notice to initiate the renewal process and communicate about what the family needs to do to maintain eligibility.
- The family must take the required action to reapply, including providing information about its recent income and other circumstances and any required documentation or verification.
- The state must schedule and conduct (and the family must participate in) an interview at least once a year for most families.
- The state worker must assess the information the family submits, determine if it is complete and adequate (and request additional information if it is not). The family must address any outstanding issues.
- The state worker must take the necessary steps in the state’s eligibility computer system(s) to extend eligibility for an additional period of time and issue a notice to inform the family.
Box 2: How Different Program Rules May Affect Churn
The three public benefit programs we focus on in this paper — SNAP, Medicaid, and child care — have many common features, but also some differences that may affect churn and churn measurement. State agencies also administer other programs, such as cash assistance under the Temporary Assistance for Needy Families (TANF) program, energy assistance, and, in some states, General Assistance (GA). States may wish to include these other programs in their churn measurement efforts.
- Program structure: SNAP and Medicaid are funded as open-ended entitlements, meaning that funding is available for all families or individuals who meet federal and state program rules. In child care, by contrast, funding (and, as a result, participation) is capped in almost every state. This can affect whether benefits are available to reopen cases when a case closes for a procedural reason, which may affect churn. In addition, Medicaid and the Children’s Health Insurance Program (CHIP) operate as part of a range of health coverage programs that are available to individuals, so changes among health programs also are relevant for churn (see box 3). For SNAP and child care subsidies there generally is no alternative coverage option available.
- Federal renewal rules: States conduct eligibility renewal within federal rules in all three programs.
- SNAP: Under SNAP rules, states initiate the recertification process by notifying the household of the recertification requirement and providing an application and a list of required verifications. SNAP certification periods are for a fixed number of months and then expire unless there is a new, approved application. States must interview households (by phone or in person) at least once every 12 months. All applications must include a signature (which may be electronic or by telephone). In addition, families must tell the state if their income exceeds 130 percent of the federal poverty level (the program’s federal gross income limit) and, if the state assigns a 12-month certification period, the family must file a “simplified report” after six months to report key changes in circumstances.
- Medicaid: States first evaluate information available in casefiles and through electronic data matches. If such information is sufficient to determine Medicaid eligibility, the agency extends eligibility and sends a notice informing the family of continued eligibility and the basis of the decision. (The individual does not need to take any action unless there are inaccuracies in information used to determine eligibility.) If available electronic data or information in casefiles is not sufficient, the agency must give families the opportunity to renew eligibility in person, online, by telephone, or by mail. The agency must send forms that are pre-populated with available information and provide the individual with reasonable time to correct any inaccuracies and provide any additional required information. Medicaid renewals are required annually, but eligibility periods are not fixed. If an individual contacts the state within 90 days of losing coverage and is still eligible the state must re-establish coverage without requiring a full application. Consumers are required to report changes in their circumstances and states are required to act on changes that may impact eligibility. A signature is not required with each Medicaid renewal.
- Child care: Under the Child Care Development Block Grant (CCDBG), states have significant flexibility in structuring eligibility redeterminations and what they require from families procedurally. The recently enacted CCDBG reauthorization requires children to be eligible for subsidies for a minimum of 12 months, regardless of income changes and temporary changes in employment, as long as family income remains under the federal income standard. It also requires states to ensure that their redetermination procedures do not require parents to unduly disrupt employment in order to comply.
- Non-financial eligibility requirements: Of the three programs, SNAP has more non-financial rules; for example, individuals without children may be subject to a three-month time limit when they are not working. In addition, states may sanction individuals for not complying with Employment and Training requirements. In child care, states may close cases when families do not pay a copayment.
The federal rules regarding renewal are different in each program, and because states have latitude on the details of their processes, certain procedures will differ by state or local office (for example, how often renewals are required, what business can be conducted online or by telephone, or what specific verification is required.) Some of the steps outlined above can be collapsed, for example, if the family submits all required verification at step 2, or the state can obtain all necessary information through automated data matches, then the back-and-forth between the state and family at later steps can be avoided. However, if either the state or the family does not take one of the required steps in a timely manner, then benefits likely will be denied, suspended, or delayed until the process is completed, which sometimes involves repeating earlier steps.
When assessing churn, a common approach is to begin with a conversation about whether the state or the family is to “blame” for incomplete renewals that precipitate a churn spell. In some instances blame could, in theory, be assigned. If, for example, the family returns the renewal information but the state does not act on it, then churn would be the state’s fault. Or, if the family receives and understands the renewal requirements but chooses to not reapply in a timely manner, then churn would be the family’s fault. Assigning fault within a state’s process, however, does not result in an improved renewal process. Often, it is unclear why renewals do not move past a certain point in the process. For example, states’ renewal notices may be confusing, steps in the process may appear redundant and unnecessary, families may have moved and never received the notice, or they may have called a call center to report they moved, but have not been able to get through to a call center agent.
It would be advantageous for both states and low-income households for states to identify those points in the process where renewals appear to result in procedural denials and work to eliminate any obvious barriers that exist or to improve the process design so that more renewals for eligible families are successful. This will reduce churn, especially the instances where the household reapplies very soon (i.e., less than a month) after losing benefits, and it is very likely that the household never lost eligibility. The goal could be to make the renewal process more navigable so there are virtually no procedural denials of eligible families, which would benefit both states and families.
This paper focuses on this issue of households that cycle off and on benefits because of avoidable “procedural” issues, as opposed to including households that lose and regain eligibility because of a change in circumstances that only temporarily eliminates the household’s need for help.
Box 3: A New Kind of Churn Among Health Coverage Programs
This paper focuses on the “churn” that low-income individuals experience on and off of programs because of procedural issues. However, because the Affordable Care Act (ACA) created health coverage options for higher-income consumers through state and federal marketplaces, there now also is the risk of churn among health programs as a consumer’s income changes over time.
In Medicaid, once individuals are found eligible, they must generally report changes in their circumstances that may affect their eligibility during the year and states must act on these changes. That’s especially hard for Medicaid beneficiaries and state agencies because peoples’ incomes often fluctuate over the course of a year, sometimes even month to month. Thus, beneficiaries may have to switch back and forth between Medicaid and subsidized marketplace coverage, and they may experience coverage gaps if the paperwork proves overly burdensome and too difficult to complete.
Moving beneficiaries back and forth repeatedly between Medicaid and the marketplace is costly for state Medicaid agencies, for marketplaces, and for health plans, and it may cause disruptions in care for beneficiaries.
The Costs of Churn
Families that lose benefits or have their benefits delayed for several days or weeks because of a procedural issue during the renewal process face tangible effects. They may not have food for at the start of the next month. People commonly find that their case has closed at the supermarket check-out counter. They similarly may not have coverage for a medical visit, or may be turned away from their child care provider and not be able to go to work that day. These events can trigger a cascade of acute problems, even if benefits can be restored retroactively, as is sometimes the case in SNAP and often the case in Medicaid and child care.[6] For health care and child care, where continuity of care is important, churn can contribute to poorer outcomes, for example, if individuals cannot receive needed medical care or fill a prescription, or if a child loses access to a high-quality child care provider.
Continuity of benefits is a matter of urgency not only for families; it also is important for states that are facing increased demand for services and strained budgets. Churn can waste caseworker and agency time. Consider a state that has 200,000 participating cases in a typical month. If the state must reestablish eligibility for each family about once a year, and one-quarter of those families do not renew on time (yet remain eligible and subsequently reapply for benefits), then the state might need to process about 50,000 additional new applications a year because of churn. Further, this simplified example assumes that renewals are coordinated across programs. If the state must do a separate SNAP and Medicaid renewal each year, or separate SNAP, Medicaid, and Child Care renewals, then the number of applications that might be avoided by reducing churn could increase several times over.
In addition, states and families alike may experience costs from the duplicative work that may need to occur to re-establish eligibility, especially if the family had made it partway through the renewal process before the case closed. State and county local offices as well as call centers feel the effects of churn when families, which can be experiencing stress and agitation, come to the office or call to find out why their case closed.
A USDA six-state study of SNAP churn found that in 2011 states spent about an additional $80 to process eligibility for each household that churned. Households missed out on between $2 million in SNAP benefits in Idaho, the state with the smallest amount of foregone benefits studied, and $108 million in Florida, the state with the most.[7]
Finally, the unexpected loss of benefits caused by churn also imposes hardship and costs on community groups and businesses. For example, emergency food providers and other charities may be called on to step in when benefits end unexpectedly, child care providers may have trouble meeting payroll when families’ subsidies are not paid on time, and community health facilities and hospital emergency services may unnecessarily experience a higher volume of patients.
Measuring Churn
Individual eligibility workers, call center staff, and community organizations that help families apply for benefits report that churn is a common problem. But aggregating those individual stories to determine how common churn is statewide, or in a particular county or local office, can be challenging because it requires tracking information about households over several months. Untangling the root cause of churn can be even more difficult because it requires a nuanced exploration of why families may not have acted as needed to retain their benefits, or whether and why the state failed to act on time to ensure that benefits continue.
Nevertheless, understanding and reducing churn can help states manage their workload. Some share of human services work is outside the state agency’s control – for example, when more families become eligible because of income loss during an economic downturn. But if states can project applications that come from churn and work to reduce these types of applications, their workloads could become more efficient.
Churn exists within the flow of a state’s entire certification process, and involves numerous policies and procedures that occur at application, renewal, and at points in-between. It is about measuring something that did not happen; for example, a renewal form or verification that a family did not return on time, or an action to continue benefits that a state eligibility worker did not complete. Many states have programmed their computers to automatically close cases unless these types of actions trigger the case to continue, and so churn often is invisible to state policymakers - the reapplication from a case that churns is difficult to distinguish from a new application from someone who has not participated before.
As a result, churn can be complicated to measure and requires connecting the dots across several pieces of the process. To say that a state has a “churn rate” of 25 percent will not usually mean much intuitively and raises numerous questions. Thus, when measuring churn it is important to explain what the measure means.
In this section we explore how states and other researchers have captured the magnitude of churn with three different measures. We present a “theoretical example” for an imaginary state where we try to present consistent numbers across the three measures to facilitate comparison. (Though not for a specific state, these theoretical examples are based on the magnitude of churn in some of the states that have measured it.) We also include an actual instance of where the measure has been used, and discuss the advantages and considerations for each approach. Finally, we discuss some other measures that are relevant in assessing procedural issues in program administration. (Appendix 1, a table, summarizes the three measures detailed here. In Appendix 2, we discuss some of the more technical measurement issues that are common across the three measures.)
Churn Measure 1: Renewal Churn Rate
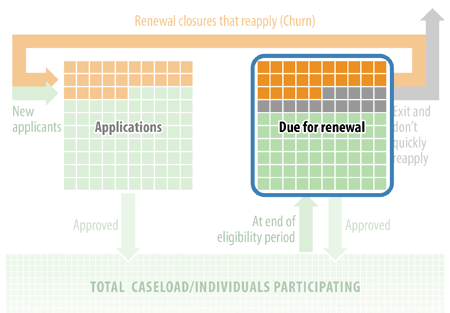
Measure: The share of participants who are due to have their eligibility re-determined in a given month who experience an interruption in benefits, but return to the program within a short period of time. This measure is highlighted in Figure 2.
Theoretical example: In July, 10,000 of a state’s cases are up for renewal. Sixty percent, or 6,000, successfully complete the renewal process on time and receive benefits (or continue health coverage) for August. However, 4,000 are not renewed on time and have their cases closed. About two-thirds of those 4,000 cases, or 2,600, reapply (or, in some Medicaid cases, are reinstated[8]) within the following 90 days. Those 2,600 are 26 percent of all cases that were due for renewal in July. See Figure 3.
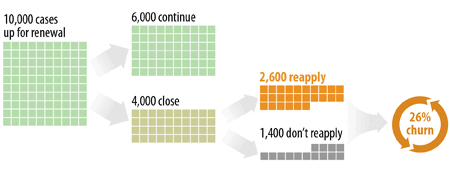
So the Renewal Churn Rate would be:
Number of cases that close in a month
but return within 90 days
Number of cases due for
renewal that month
Actual Example: Of Idaho’s monthly SNAP re-evaluations, about a third do not continue benefits for procedural reasons.[9] (The others are either approved, or denied because they are found to be ineligible.) Of these cases about half reapply within 90 days (mostly within a month). This could be expressed as a churn rate of 16 percent of all households up for redetermination.
Advantages: This measure is the most direct measure of churn that is caused by procedural problems at redetermination, and as a result it may be the most useful for diagnosing the root causes of churn and for measuring the effectiveness of possible revisions to the renewal process that a state may wish to test.
Considerations: This measure cannot be finalized until several months after the redetermination month when information about reapplication can be known. It is somewhat difficult (and wordy) to express renewal churn as one number. Ideally it is composed of two concepts: the share that are closed and the share of those that reapply. In the theoretical example above, if the state were able, through redesigned procedures, to reduce the share of cases that close from 40 percent to 10 percent, then the renewal churn rate would drop from 26 percent to about 7 percent, even if a large majority (65 percent) of those who do close still reapply.[10] In addition, this measure does not capture churn that occurs outside of the renewal process (i.e., from cases that close in the middle of an eligibility period.)
In addition, a very important drawback is that this measure does not capture the effect of policies that reduce the incidence of renewal. So, a state that moves to longer eligibility periods or that eliminates many Medicaid renewals because it coordinates Medicaid eligibility reviews at the time of a SNAP renewal may still have a high churn rate for those households that still do come up for renewal. But far fewer households will need to participate in the renewal process and so reductions in the magnitude of overall churn will not be evident in this measure. As a result, to be most useful this measure needs to be considered alongside other measures, or at a minimum, in conjunction with other information about changes in the number of cases experiencing the renewal process.
Churn Measure 2: Applications from Churn
Measure: The share of new applications from households that participated in the recent past (the highlighted portion of figure 4).
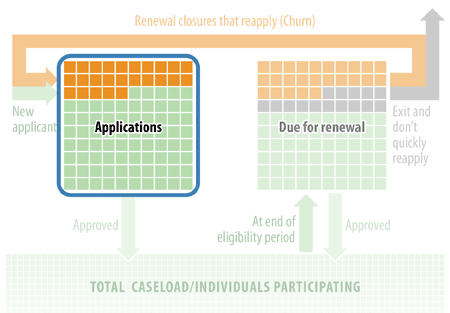
Theoretical example: In September, the state receives a total of 9,600 “new” applications (i.e., not including timely renewal applications). Of these, 2,600 are from cases that closed at renewal within the previous 90 days (i.e., the corollary to the cases counted in “renewal churn” under the previous measure.) The state also receives 1,000 applications from cases that closed within the previous 90 days, but not at a renewal. (These cases may have reported changes that made them ineligible or asked to have their case closed.)[11] Those 3,600 applications are 37 percent of all new applications in September. (See Figure 5.)
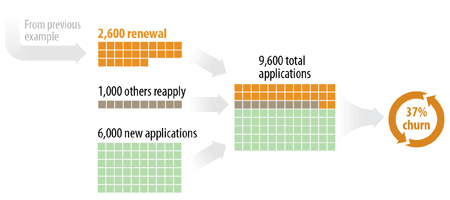
So the Applications from Churn Rate would be:
Applications from cases that participated
within the previous 90 days
All new applications
Actual Example: In California, 22 percent of SNAP applications are from cases that closed in the previous 90 days. California’s state officials sometimes help people visualize this measure by saying, “Picture a local office waiting room filled with 100 people who are there to apply for benefits; 22 of them recently participated but lost benefits.”[12]
Advantages: This measure captures the impact of churn on states’ workload in a tangible way. States can visualize that if they do a better job keeping eligible households connected to benefits then they will have fewer reapplications. Since this measure can be done monthly looking back at the previous three months, it can be produced more quickly than the other measures, and so it may be better for monitoring performance. Unlike the “renewal churn rate” this measure will capture policies that reduce the frequency of renewals and can also capture the churners whose exit did not occur at renewal.
Considerations: This measure looks at a more indirect consequence of churn (the reapplication) and not the root cause (the closure), so it may not be as helpful for diagnosing the problem as the renewal churn rate, or other data that focuses on procedural issues in the renewal process (see below).
Churn Measure 3: Annual Churn Rate
Measure: The share of cases that experience at least one spell of “churn” in a year (i.e., the case closes but the family reapplies within a short period of time.)
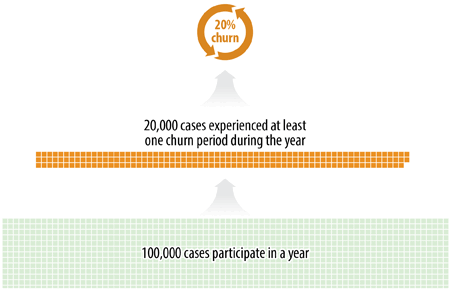
Theoretical example: The state has 100,000 cases that participated in the program at any time during the year. Of these cases, 20,000 experienced at least one spell of churn over the year — that is, the case closed but they returned to the program within 90 days. Those 20,000 cases are 20 percent of the 100,000 cases that participated during the year. (See Figure 6.)
So the Annual Churn Rate would be:
Number of cases that experience a churn spell during the year
All cases that participated during the year
Example: USDA-sponsored research conducted by the Urban Institute recently found that in the six states studied, between 17 and 28 percent of participating households “churned” during 2011. Such households exited the program (as measured by a break in SNAP benefits) but returned within four months.
Advantages: This measure can be derived from state administrative data about households’ monthly benefits (rather than based on monthly application information). It represents the impact on program caseloads broadly, so it would capture the effects of longer eligibility periods or other policies that reduce the frequency of recertification risk points.
Considerations: This measure looks back at what happened in a prior year. It would be difficult for states to produce on a monthly basis, and thus, is less timely for monitoring program performance. With this measure it also may be more difficult for states to capture cases that experience a delay in benefits but retroactively receive the full amount of benefits or coverage. The measure may be less intuitive, so may not be as useful for state staff in seeing the impacts of churn on workloads or helping to diagnose the causes of churn and develop policies to address it.
Box 4: Is Zero Churn a Realistic Goal?
Some kinds of churn are inevitable. For example:
- It is natural, and unavoidable, for some people to make a choice to not reapply and then change their minds.
- Also, families’ circumstances change so they become ineligible, but then another change may, within a short period of time, change their circumstances again so that they requalify. (This type of churn can be reduced by changing eligibility or reporting rules.)
As a result, if the churn measures a state uses includes these types of situations, it is unlikely churn will be eliminated entirely.
It is reasonable, however, to expect churn that is triggered by procedural problems to be close to zero. Unfortunately, the information about the eligibility of families who do not participate often is not available to states, and so establishing churn measures and tracking state progress over time can help states and other stakeholders determine if changes the state is making are working and procedural churn is declining as a result, even if it cannot be reduced to zero.
All three of these measures are useful, and multiple measures can help states and others to gain a fuller picture of churn. Some states’ systems may not be able to easily “pull” each of these measures, so it may require creative approaches or building the capacity into the data reporting functions of the updated eligibility systems that now are under development in many states. There also are numerous technical measurement issues involved (see Appendix 2). While it is important to strive for methodologically rigorous data, if the goal is to reduce churn, then the precise measure may matter less than tracking it in a consistent way over time so that state officials and other stakeholders can engage in meaningful conversations about what issues are contributing to churn and to track progress in reducing it.
Measures of Procedural Problems
Measuring churn using one or more of the options described above can allow states to understand their overall magnitude of churn. Additional work will be necessary to determine the root causes of churn, and where in the process procedural hurdles occur. Figure 7 presents a simplified version of the typical flow in a process with multiple steps that may present procedural hurdles. At each step there is a risk that either the family or the state will fail to take actions, contributing to churn. Isolating the problems and quantifying their size will help states develop improvements in their processes and systems that they can test to address churn.
States may, for example, be able to quickly determine that a large share of cases that are sent a renewal form never take any action at all, and that such cases represent a large share of the cases that close at renewal. That would point to solutions that address mail and notice problems. Alternatively, some states close a large share of cases because people miss interviews or there are not sufficient interview times available to accommodate every case for which an interview is required before the computer automatically closes the case. In other states, a large number of closures are due to a “failure to provide required verification,” which could suggest that reducing the paperwork required of households, making it easier to submit documents, or improving the mailroom workflow could be promising approaches. In many states multiple parts of the process will need attention.
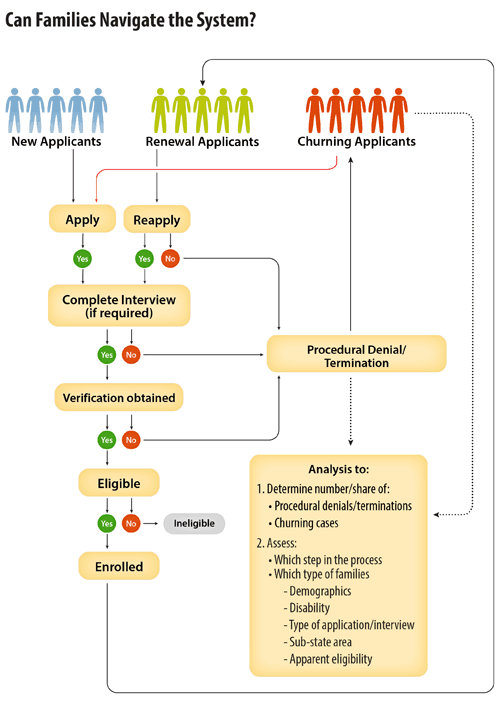
Below are some examples of data that states may already be collecting, or could collect to help them determine where procedural problems occur and start to identify possible solutions.
Procedural Reasons. Some states’ eligibility systems allow them to distinguish between “procedural” and “eligibility” reasons for denial or case closure. Examples of procedural reasons for denial that occur at renewal include “failure to provide required verification,” and “missed interview.” An eligibility reason might be that “income exceeds program limit.” A common reason for a procedural closure at renewal is that the state never receives a re-application or contact from the household, so the state closes the case.[13]
The quality of state administrative data on procedural reasons varies substantially. When the data is reliable it can be highly useful in identifying places in the state’s process that are the most difficult for families to navigate, and therefore may be fruitful for improvements. However, many states report that their data on procedural reasons are not coded consistently or are missing for too many case closures, which limits their usefulness. In addition, many state computer systems automatically close cases at the end of a certification period in SNAP or child care when the eligibility worker does not finalize the eligibility determination, and these types of closures may not include a reason.[14] Such autoclosures may occur because the client did not take a necessary action (for example, return verification or reapply), but sometimes cases autoclose when clients do their part but the state loses paperwork or does not complete its work on a renewal on time. New applications and the number of cases and related renewals increased rapidly as a result of the recent recession, and some states fell behind. Similar problems have occurred recently in some states with problematic implementation of new systems and backlogs from health reform’s rollout.
Other workload data. Many states have the capacity to access useful workload data that can provide insights into churn. For example, some states have call centers to respond to families’ inquiries or to conduct parts of the certification process, such as taking applications or conducting interviews. Some states have mail processing centers, which may track returned mail, or have software that helps with lobby management. Most states also have online applications. These types of task-based processes may provide two sources of interesting data.
-
First, technology involved in the task may be able to provide data about the types of people who are experiencing churn or the types of problems and questions people have. That task in the workload process may represent the “front line” or “first responder” to churn; for example, families may reach out to a call center when they discover their benefits or health coverage has lapsed, or go online to check their benefits or visit a local office. States may have the capacity to gather information from these types of interactions with clients that would be useful in diagnosing churn.
Similarly, if families are confused about a notice they may reach out to the call center to ask questions about what the notice means. As a result, high call center volume, long wait times, or a high number of dropped calls at a call center may signal a procedural problem elsewhere in the process that the state can investigate further.
- Second, these tasks could themselves be contributing to churn, or have elements of churn within their processes that contribute to higher workloads. For example, when people can’t get through to the call center, they may start calling more or on multiple lines in an effort to get through; a backlog of people in the waiting room of a local office may hinder staff’s ability to triage easy transactions and result in even more crowded waiting rooms.
Client, community, and staff input. Perhaps the single best source of data on the causes of churn is the customers themselves and their experiences navigating the process. States could conduct client surveys or focus groups to gather input on which stages of the process present barriers, what people understand and don’t understand about local office requirements and options for families, and what their experiences are in their interactions with the state agency. Even without a sophisticated survey or resources for research, state staff can survey people in the lobby or ask staff or community partners who work directly with clients to gather feedback. People who interview applicants in person or over the telephone will, in many ways, have a perfect sample of churners to probe about what happened. If states collect such information from even a relatively small number of people who churn, it could shed light on problematic parts of the process.
States also could conduct focus groups or interviews with other knowledgeable individuals. Community groups, which work directly with low-income families and often help them to apply or reapply for benefits, may have insights about common problem areas and which changes might have the largest impact. In addition, the eligibility workers and supervisors who process eligibility may also be an invaluable resource to state and local officials who want to understand which parts of the process are most problematic and the merits of possible changes to address the problems.
Approaches to Reducing Churn
As states have begun to measure churn, they also are testing strategies to address it. Because churn is entwined with a state or county’s certification process, not all approaches will be relevant in every state or county.
For example, early in its Work Supports Strategy project, Idaho developed churn measures that revealed that 60 percent of families receiving SNAP whose cases were closed for failure to complete the reevaluation process reapplied within 90 days and, as a result, one-third of application volume could be eliminated by improving the re-evaluation process.[15]
Promising approaches fall into three categories: reducing renewal risk points, addressing the specific churn risk points when there is a need for renewal, and prioritizing measuring and testing progress.
Reducing Renewal Risk Points
This first category of solutions is a high level structural issue — how often are renewals required — rather than a detailed look at a step in the renewal process. The purpose of regular renewals is to periodically reconfirm eligibility (and for some programs to ensure that benefit or subsidy levels are correct). Yet with each required renewal there is a risk that families will encounter a procedural barrier and that eligible families will lose benefits as a result. These risk points can be minimized, however, if states adopt policies to require paperwork, or other actions, from families less often. Examples of policy or procedural changes states and counties have used to reduce renewal frequency include:
-
Using the longest eligibility periods appropriate for family circumstances. States renew Medicaid and CHIP eligibility only once a year, as federal rules require, and federal rules have changed to require a minimum eligibility period of 12 months for child care. Many states still review SNAP eligibility every six months, though longer certification periods are allowed with interim reports. Using annual (or longer) eligibility periods across all programs can save time for state workers and keep families enrolled. States are allowed to recertify eligibility of elderly and disabled households for SNAP every 24 months. USDA’s research finds that when a household with an elderly or disabled member is required to recertify, its odds of experiencing a spell of churn are higher than the typical SNAP household (so such households may be more vulnerable to procedural hurdles), but because such households tend to have stable income, many states assign longer certification periods, lowering their rates of churn over the course of a year.[16]
Use of longer eligibility periods may make most sense for households with stable circumstances and when combined with efforts to educate families about any program requirements to report changes in income and other family circumstances during an eligibility period (and to facilitate families’ submission of such reports, as discussed below).
-
Push forward or renew Medicaid or child care eligibility based on SNAP information. The fact that most SNAP families must provide updated information every six months under “simplified” reporting creates an opportunity to limit the frequency of renewals in other programs.[17] States can either push forward the other program’s redetermination date by 12 months at the time of the successful SNAP recertification or report, or, when the other program’s renewal comes due they can look first to the most recent SNAP income and household information to confirm eligibility. If eligibility can be confirmed then the household can be sent a notice informing them of their continued eligibility for Medicaid or child care based on the information they reported for SNAP on income, earnings, and other factors.
With this approach, it is important to note, however, that Medicaid, CHIP, or child care may not be terminated if the SNAP recertification fails to be completed. In such an instance the family would keep its health or child care coverage through the original renewal period and at that point there would be an opportunity to renew health or child care coverage, (and in states with integrated eligibility processes, to screen and enroll the family in SNAP if they are eligible.)
A variation on this approach would renew or extend eligibility at any time a family contacts the state (rather than just at renewal). So, for example, if a family calls to report a change, the call center worker could apply that change to Medicaid and child care under those program’s reporting rules and, if the family remained eligible, the end dates on the eligibility period for Medicaid and child care could be reset for 12 months in the future. States could similarly use information that families report to the state through their online account to extend eligibility periods.
Idaho has implemented this approach for Medicaid and child care. When processing information the family submits for SNAP at recertification, on a report, or an interim change report, the state also reprocesses Medicaid and child care eligibility under those programs’ rules and sets a new 12-month eligibility period. As a result, Idaho has reduced the number of Medicaid redeterminations for families that also receive SNAP.
- Align renewals. When eligibility periods are not aligned families may need to renew benefits in different months for each program (and for health coverage, sometimes multiple times if individual within the family are on different renewal schedules.) This can result in duplicative work for states and can be confusing for families, who may believe that the state human service office already is taking into account the information they’ve submitted for other programs that the same agency administers. Consider a family of three with one adult and two children. If eligibility periods are not aligned and this family participates in Medicaid, SNAP, and child care, it could be asked to complete seven renewals in a year, even if it experiences no changes in its income or circumstances (three different eligibility periods for each family member for Medicaid, one SNAP recertification and one SNAP simplified report, plus one child care redetermination for each child). But that number could be reduced to two if the state aligns certification periods. North Carolina piloted aligned eligibility periods for SNAP and Medicaid in 2012 and found that though 85 percent of participants did not have aligned periods before the pilot, for the majority it was feasible to get the periods into alignment at the time of a SNAP recertification.[18]
- Use administrative renewals. As discussed in box 2, states are required to attempt to administratively renew all Medicaid cases based on trusted data sources before requiring information from families. This practice can reduce families’ paperwork requirements. Other programs could use elements of this approach in designing a less burdensome renewal process for families.
Addressing Specific Procedural Causes of Churn
In addition to minimizing the frequency of procedural requirements, states can lower the procedural burdens for households to maintain eligibility when renewals do occur. As discussed above, the specific causes in any state or county will depend on the local practices and policies, so it will be important to understand the individual state, county, or local office processes and identify where in the process people drop out. For example, do a large share of families not file a renewal form in the first place? Or do they file the form, but not complete an interview, or fail to return a telephone call seeking clarification? Or is required verification never received, or received and not acted on in time? State and federal policymakers sometimes assume that most procedural problems are caused by families’ lack of compliance with requirements. While this undoubtedly occurs, it also is important to ascertain whether families received notice of requirements, understood those requirements, and were able to complete them. In addition, especially with recent caseload growth and ACA implementation, some state or local offices have backlogs that can result in procedural problems.
The types of changes states can consider to address the specific causes of churn fall into two categories: improving communication with their customers and streamlining their processes to provide better customer service.
Improving communications. Some families who receive public benefits have low literacy levels and/or limited English proficiency. States, with the support of federal agencies and nonprofit groups, are exploring how they can improve communications with such families.[19]
-
Forms and notices. In the past, the state notices that eligibility systems issue to inform people of the need to renew benefits, as well as approval and denial notices, have been legalistic and formatted in a way that makes the information difficult to comprehend. Notices can be especially confusing for families if they receive multiple notices for different programs because of unaligned eligibility periods.
Some states have begun projects to simplify and clarify notices, paying attention to the reading level of the content, making them more effective visually, and pre-populating forms with the information already known to the state.[20] Innovative states have incorporated “user-experience” expertise to improve their communications. Involving community partners and plain-language experts also can help identify problematic notices or wording.
- Other forms of communication. Many states are making greater use of online accounts, which can help some participants, and the community groups that may assist them, check the status of their benefits and troubleshoot procedural problems. Similarly, call centers that can answer questions and provide accurate information can help improve communication if they are adequately staffed to minimize wait times. Some states also are starting to experiment with email notices and text messages (see below), which for some families, can be more convenient than the mail, though these communications channels are not available to all families.
Revising business processes. Many states are revising their processes to be more efficient. In the past, health and human services agencies used a caseworker-based approach for delivering benefits, where families would have an ongoing relationship with a dedicated social worker who would assess their income and circumstances and determine eligibility. Many states have found this model could not be sustained for all families in the face of rising caseloads and financial constraints, and was contributing to poor customer service. Many states now are pursuing a “task-based” model in which individual staff focus on completing specific steps in the certification process and bottlenecks are identified and removed so that families can be served more quickly. These new task-based approaches give states and local offices the flexibility to direct staff resources to the tasks that are backed up in order to address procedural bottlenecks. Many states are now setting a standard of “same-day service” wherever possible because, in addition to providing excellent customer service, such an approach enables states to “touch” cases fewer times.
Ways states can modify their business processes to help reduce churn include:
- Resources for call centers, renewal units, and documentation processing. A strategic investment in resources for specific areas of the renewal process, such as additional staff or investments in improved technology, may help to reduce churn. For example, an investment in call center staff could help to streamline a piece of the process, for example, making it easier for families to apply over the telephone, or for staff to conduct an eligibility interview or report changes, and also may help families quickly answer questions. It is vital that call center staff be adequately trained in program rules so that they can properly carry out their critical, and growing, role in the eligibility process.
- More options for families. In the past, the renewal process has been envisioned as one where states lay out the steps in order (i.e., receive notice of need to renew, reapply, participate in an interview, submit verification) and families need to follow the steps in proper sequence. States are becoming more aware that giving families options for how they can comply with requirements may help reduce procedural problems. For example, some states allow families to call for an interview within a window of time so that the interview can take place when it is convenient for the family. The ability to upload documents to a portal can make it easier for some families to provide verification, either themselves or through a partner agency. Multiple avenues for submitting renewal applications and reporting changes (i.e., online, by phone, or by mail) also can help families comply with paperwork requirements.
-
Addressing frequent moves and returned mail. Historically, states have notified families of renewal requirements through mailed notices and required families to take the next step by submitting an application or renewal form. But the recent study of SNAP churn, which interviewed clients and state staff, identified “lack of receipt and response to mail notifications [as] a key issue in churn.” For example, if a household has moved or the mail delivery in its building is not reliable, families may never receive the notice or know that they need to reapply. And on the state side, some states report that their eligibility systems sometimes produce inaccurate mailing labels, for example, by deleting “apartment number” from the address, which results in returned mail.
Some states are experimenting with using text messages or emails to send reminder notices. San Francisco County in California recently piloted optional text reminders to SNAP recipients who are at risk of case closure and found that almost 40 percent responded to the reminders immediately by calling a call center.[21] Reminder notices could also be included in other forms of communication, such as at the grocery store through EBT receipts or through child care or health care providers.
- Limit paperwork for verification. As discussed elsewhere, under the ACA states are moving toward making greater use of electronic verification in Medicaid in lieu of requiring paperwork from families. These electronic data sources also hold promise for reducing paperwork burdens on families for other programs, though they also can increase paperwork and churn if the matches are not current and reliable. In addition, electronic case files can store permanent verification items, such as proof of age and citizenship, and allow verification to be shared across programs, which, where permitted, can limit the need for households to present the same documents multiple times.
- Quickly re-establish eligibility after a break. States must reinstate Medicaid coverage when a family returns within 90 days of a termination. Because it often is much less burdensome for states and families to reopen an existing case than it is to start the application process anew, states may wish to consider using the flexibility offered in child care to reopen recently closed cases (or denied applications). For SNAP, USDA similarly allows states to apply for waivers to reopen SNAP cases that they have closed in the middle of a certification period.
Measuring and Tracking Progress
Historically, understanding, measuring, and reducing churn has not been central to the measurement of human services programs’ performance. States, federal agencies, and client advocates have been more focused on two other important measures of access: timeliness of initial application processing and participation or coverage rates among those who are eligible.
Yet, measuring, tracking, and taking steps to reduce churn can improve both coverage rates and administrative efficiency. For example, Louisiana state officials found in the early 2000s that 22 percent of their CHIP and Medicaid cases up for renewal were being closed for procedural reasons. In response, the state took a number of specific steps to simplify the renewal process, including using administrative renewals, increasing telephone follow-ups, and allowing off-cycle renewals (that is, pushing forward Medicaid eligibility periods by 12 months any time the state had contact with the family.) Four years later, closure rates at renewal were down to 8 percent; by 2008, they had fallen to only 1 percent.
Despite recent progress, there is no agreed-upon methodology for measuring churn, nor a large body of evidence on what works to reduce it. Below are suggestions for where state officials and others interested in reducing churn may wish to start.
- Prioritize measuring and reducing churn and set related goals. The first step is to begin to measure churn and set goals for reducing it. California state and county officials, as well as an alliance of advocates, for example, are working together to reduce churn in SNAP. The state publishes quarterly data on churn (for the state and each county) as part of an online data dashboard.[22] The state has used the dashboard to spark conversations among counties, advocates, and other stakeholders about strategies for lowering churn.
-
Even before statewide and sub-state measures can be finalized, however, states and local offices can take steps to begin to investigate churn. One such step would be for states to determine which of the churn measures discussed in this paper they can draw from their data systems and setting a timeline for when that data will be available.
- Some counties or local offices may be able to measure churn before the state can do so systematically because they may have application and renewal information for cases in their area more easily available.
- In addition, looking at monthly county or local office data on the number of closures and/or applications may be useful. Areas with high (or low) closures and/or applications in relation to the size of their caseload may have higher (or lower) churn rates than other areas of the state.
Once states or local offices have a baseline, they can start to determine what the right goals might be. For example, is it possible to set a goal of reducing churn by 50 percent? Or if information on procedural issues is available, is it possible to come close to eliminating churn from certain types of procedural problems? If a state finds that some counties or local offices have much higher churn than others (when measured the same way) it might make sense to set a goal for all offices by performing at the level seen in the best-performing offices.
-
Identify areas of focus. In addition to building churn-specific measures, states can begin to investigate other churn-related information. For example:
- Exploring the reasons identified for case closure;
- Developing process maps using data that identifies where in the renewal process cases drop out;
- Understanding how their state’s eligibility systems and eligibility workers treat cases at renewal (for example, under what circumstances cases are “pended” versus “autoclosed,” and when the state requires a new application as opposed to reopening an existing case.)
- Getting input. States can gather input from stakeholders, such as county and local office staff, as well as from customers through surveys, focus groups, and conversations with community groups that help with application processes. Such efforts need not be highly sophisticated; some states and local offices have found that interviewing people waiting in the local office lobby about their experiences can yield useful information about churn.
Conclusion
Reducing churn in public benefit programs can be a daunting task. It is one, however, that states increasingly are paying attention to, as it has the potential to improve both coverage rates and administrative efficiency. This paper has laid out some options for measuring churn, outlined some of the related technical issues, and offered options states can take to use administrative data and other information to begin to address churn. For some states, the first step may be to start a conversation among agencies, advocates, and program participants about the importance of churn.
Appendix 1: Three Measures of Churn
| Renewal Churn Rate | Applications from Churn | Annual Churn Rate | |
| Definition | The share of cases up for renewal that experience an interruption in benefits but return to the program within a short period of time. | The share of new applications that are from households that participated in the recent past. | The share of cases that experienced at least one spell of churn in a year. |
| Advantages | Most direct measure of churn caused by procedural problems at renewal, so useful for diagnosis and measuring progress. |
|
|
| Disadvantages |
| Describes a more indirect consequence of churn (the reapplication) and not the root cause (the closure), so may not be as helpful for diagnosis. |
|
Appendix 2: Technical Measurement Issues Related to Churn
The paper’s section on measuring churn lays out three measures in a simplified format. All are useful, and multiple measures can help states and others to gain a fuller picture of churn. This appendix delves into some of the issues and choices that states face in measuring churn. In some cases states will want to make decisions about these issues based on what makes the most sense for developing policy and procedures to address churn. In other instances, states may decide the perfect answer is not easily available, but that having an imperfect measure based on more readily available data is still worthwhile. If the state’s goal is to reduce churn, the precise measure may matter less than tracking it in a consistent way over time so that state officials and other stakeholders can engage in meaningful conversations about what issues are contributing to churn and track state progress in reducing it.
Unit of measurement. Should states measure churn for units (or cases) or for individual program participants? Most analyses of churn have measured churn among cases because the unit of state workload usually is a case, which often includes multiple individuals. Especially for measures that come directly from states’ eligibility systems it is likely that closures and applications will be measured in “cases.” For health coverage, however, individuals within the same unit may not all be eligible for the same program, so tracking churn among individuals may make more sense for uncovering churn among health coverage programs (i.e., Medicaid, CHIP, and federal subsidies under the ACA).
Length of the break in participation (30, 60, 90 days, or longer). Most states that have tracked churn report that the overwhelming majority of cases that return to the program do so within the first month. USDA’s study of SNAP found that 62 to 79 percent of churners were off SNAP for one month or less (the study counted a return to SNAP as churn if it was within four months).[23] California similarly has found that the return to SNAP occurs within 30 days for about 60 percent of cases that churn within 90 days. (As discussed below, some measures of churn may understate the share that experience a very short break in participation because of measurement issues in identifying short spells off the program.) It is more likely that cases that have a longer spell of non-participation experienced two changes, and may have been ineligible, or needed help less for some period of time; those that return very quickly are more likely to have been eligible in the interim. Thus, if a state wants to consider reapplications after 60 days (or longer) to be churn, it would make sense to break it into 30-day increments so that the information about the very quick reapplications also is available.
Defining program “exits” and “re-entries.” A critical issue for measuring churn is identifying when a family experiences a break in benefits or coverage, which is defined by a program exit and subsequent re-entry within a short period of time. In some situations, states are able to restore benefits (or coverage) retroactively, or reinstate benefits (sometimes without a new application). Short delays can be difficult to identify in some state systems because the household may later be coded as having received benefits for the month (perhaps at a slightly reduced level), or being covered for a period of time when they did not actually have coverage.
Even a relatively short delay, however, can present a serious hardship for families and may be just as costly for states in terms of unnecessary re-work. A family that may have exhausted its SNAP benefits by the third week of the month and was depending on its electronic benefit card being reloaded for the next month may be left without food if those benefits unexpectedly do not arrive on time. Similarly, a family that loses child care subsidy even for a short period of time may lose its slot with the child care provider, who often has a wait list and must keep slots filled with “paying” clients in order to make payroll. For states, these short delays may actually trigger a great deal of work in responding to inquiries from the family and the provider and taking care of the retrospective coverage or reinstatement. They may result in crowded local offices and clogged phone lines as families in distress hustle to re-establish eligibility. As a result, it would be preferable for states to be able to capture these types of short delays or breaks and count them as churn.
In measuring churn it is important to understand both the state or county’s eligibility procedures and policies for pending cases and reinstating benefits or coverage, as well as, from the technical side, the way cases with short breaks are coded in the state’s eligibility system. To quantify the effects of churn on the states’ workload, it is desirable to capture information in real time, rather than retrospectively, and to collect as much information about individual contacts between the state and the family as possible. For example:
- Some measures of churn will use state issuance or coverage data to examine whether participants received benefits during each month. But these measures may miss short breaks in participation that later are “fixed.” In such instances, the state may wish to develop other ways to gather information about these shorter churn spells.
- Not all programs (or all reasons for case closure) require an application to reopen benefits. In Medicaid, for example, states must reinstate existing cases without a new application when a family returns within 90 days of a termination.[24] If only new applications are counted, then the cases that are relatively quickly reopened or that receive retrospective coverage may be missed. States may want to develop measures that also identify other contacts with the state agency to inquire about reopening or reinstating benefits, such as in-person visits to a health and human services or child care office, or by telephone.
SNAP mid-year reports. In addition to a full recertification, household reports are an important component of the SNAP redetermination process in some states. SNAP rules allow states to assign longer certification periods to households if the state requires an interim report during the eligibility period. Specifically, for most households (and all families with children) states may use up to 12-month certification periods with a “simplified report” at the six-month mark (which is shorter than a full application, but requires updated information on (and often verification of) a few eligibility items, including income, household members, and residence). For households with only elderly or disabled members (and no earned income) states may use two-year certification periods with a contact at the one-year mark. These periodic reports are less burdensome than a full SNAP recertification, but they nevertheless may present families with procedural barriers that cause them to lose SNAP eligibility.
As a result, states may wish to measure churn that occurs at the time a simplified report is due for SNAP. If the state’s process for reports is similar to a full recertification, it may want to treat the two the same. In Idaho’s SNAP churn measures cited above and in the USDA study of SNAP churn, the researchers included both SNAP recertifications and simplified reports. If the state’s processes for the two are different, it may make sense to track churn separately. Information about the differences might shed light on where procedurals barriers exist in one process but not the other.
Which case closures to count. States may decide to look at churn among cases that close at renewal, or more narrowly, at those that the state determined closed at renewal for a procedural reason (see below), or more broadly, at churn that results from any case closure (for example, after a change report or a data match triggers a closure in the middle of an eligibility period). Casting a wider net may provide more information and uncover more of the effects of churn, but a narrower analysis may be useful for isolating the effects of specific policy changes the state may be considering to reduce procedural barriers. While it would be preferable to make the decision based on the goal of the analysis, in many states this decision may depend on the type and quality of available data (i.e., the way a state’s automated system tracks case closures).
Which “returns” to count. A final question is how to measure the end of a churn spell: whether to count only approved applications (or case reopenings) as returns, because families that are found to be financially ineligible are not viewed as problematic, or whether to count the application (or contact with the agency seeking to reopen benefits) as a return, without regard to whether the case actually was reopened. If the state counts only cases that receive benefits, it will miss two things:
- First, the contact or application may represent a fuller measure of the workload consequences of churn; and
- Second, if the number of reapplications or contacts without a reopening is much larger than the number of reopenings, the reason may be that those families are experiencing another procedural barrier (or still experiencing the same barrier that initiated the churn spell). A state that measures only cases that successfully navigate the application process may miss out on important information about where families are experiencing procedural hurdles.
Resources
Gina Adams (Urban Institute) and Hannah Matthews (Center for Law and Social Policy), Confronting the Child Care Eligibility Maze: Simplifying and Aligning with Other Work Supports,
December 2013, http://www.urban.org/publications/412971.html.
Alliance to Reform CalFresh, “Zero Churn Toolkit: Providing Food and Stability to Families in Need,” http://www.transformcalfresh.org/zerochurn.html.
Tricia Brooks, Georgetown Center for Children and Families, “Data Reporting to Assess Enrollment and Retention in Medicaid and SCHIP,” January 2009, http://ccf.georgetown.edu/wp-content/uploads/2012/03/Data-reporting.pdf.
Tricia Brooks, Georgetown Center for Children and Families, “The Louisiana Experience: Successful Steps to Improve Retention in Medicaid and SCHIP,” February 2009, http://ccf.georgetown.edu/ccf-resources/louisiana-experience-successful-steps-improve-retention-medicaid-schip/.
Center on Law and Social Policy, Reauthorization and Implementation Resources for the Child Care and Development Block Grant Act of 2014, www.clasp.org/ccdbg.
Mary Harrington, Christopher Trenholm, and Andrew Snyder, “New Denial and Disenrollment Coding Strategies to Drive State Enrollment Performance,” Maximizing Enrollment, Issue Brief, October 2012, http://www.mathematica-mpr.com/~/media/publications/PDFs/health/coding_strategies_state_enrollment.pdf.
Kate Lewandowski, “Churn Toolkit: Stabilizing Coverage for Children and Families,” Community Catalyst, 2014, http://www.communitycatalyst.org/resources/publications/churn-toolkit.
Gregory Mills, Tracy Vericker, Heather Koball, Kye Lippold, Laura Wheaton, and Sam Elkin, “Understanding the Rates, Causes, and Costs of Churning in the Supplemental Nutrition
Assistance Program (SNAP): Final Report,” Urban Institute, for the U.S. Department of Agriculture, Food and Nutrition Service, November 2014, http://www.fns.usda.gov/understanding-rates-causes-and-costs-churning-supplemental-nutrition-assistance-program-snap.
Dorothy Rosenbaum and Stacy Dean, “Improving the Delivery of Key Work Supports: Policy and Practice Opportunities at a Critical Moment,” Center on Budget and Policy Priorities, February 2011, https://www.cbpp.org/cms/?fa=view&id=3408.
Southern Institute on Children and Families, “Medicaid and CHIP Retention: A Key Strategy to Reducing the Uninsured,” March 2009,
http://www.thesoutherninstitute.org/docs/publications/MedicaidCHIPRetention.pdf.
Kendall Swenson, “Child Care Subsidy Duration and Caseload Dynamics: A Multi-State Examination,” U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation, October 2014, http://aspe.hhs.gov/hsp/14/childcaresubsidy/rpt_childcaresubsidy.pdf.
Christopher Trenholm, Mary Narrington, Andrew Snyder, and Alice M. Weiss, “Using Data to Drive State Improvement in Enrollment and Retention Performance,” Maximizing Enrollment, Issue Brief, November 2011, http://www.maxenroll.org/resource/using-data-drive-state-improvement-enrollment-and-retention-performance.
Acknowledgements
The author wishes to express gratitude to the many people who assisted with this report. Shelby Gonzales and Hannah Matthews provided important guidance with respect to the report’s content in their respective areas of expertise: health coverage and child care. Stacy Dean and Alicia Koné contributed to the overall direction of the report. Julia Isaacs, Cemeré James, Shane Leach, Kim McCoy Wade, Greg Mills, and Linda Patterson offered valuable technical and editorial feedback. Thanks also to Michele Vaughn, who edited the report, and Rob Cady and Edward Bremner who created the figures. Finally, special thanks to the many state and local health and human services officials and staff, in WSS states and in other states, who have graciously hosted local office visits, shared their experiences, and taken the time to answer many questions. Any errors are the author’s alone.
The Center on Budget and Policy Priorities is grateful to the following funders for their generous ongoing support of the Center’s work on improving work supports and coordinated benefit delivery:
- California Health Care Foundation
- Center on Law and Social Policy
- Charles Stewart Mott Foundation
- Ford Foundation
- The JPB Foundation
- MAZON: A Jewish Response to Hunger
- Packard Foundation
- W.K. Kellogg Foundation
- Wal-Mart Foundation
- Anonymous donors
End notes:
[1] The eligibility redetermination process has different names in different programs (and sometimes different states use different words). In SNAP regulations it is called “recertification.” Child care programs typically use the term “redetermination.” Medicaid uses both “redetermination” and “renewal.”
[2] To simplify presentation, figure 1 omits cases that exit in the middle of an eligibility period, though such cases also may contribute to churn. Within federal rules, states determine what types of changes in income and other circumstances families must inform the state of, so not all families participate for the full eligibility period.
[3] It is important to note that child care, unlike SNAP and Medicaid, is not an entitlement. As a result, it is not certain that families that lose child care subsidies because of a procedural reason will be reinstated when they reapply. They may instead be put on a wait list.
[4] Gregory Mills, Tracy Vericker, Heather Koball, Kye Lippold, Laura Wheaton, Sam Elkin, “Understanding the Rates, Causes, and Costs of Churning in the Supplemental Nutrition Assistance Program (SNAP): Final Report,” Urban Institute, for the U.S. Department of Agriculture, Food and Nutrition Service, November 2014, http://www.fns.usda.gov/understanding-rates-causes-and-costs-churning-supplemental-nutrition-assistance-program-snap.
[5] For health coverage this paper focuses on coverage for adults and children under Medicaid and the Children’s Health Insurance Program (CHIP) (as opposed to Medicaid for elderly or disabled individuals). In part because of concern about churn, under the Affordable Care Act (ACA), states are moving away from burdensome renewal processes in Medicaid and CHIP and relying more on reliable administrative data sources and other technology such as online and email tools to renew families’ health coverage when possible. CCDBG’s reauthorization, which was enacted in late 2014, includes several provisions to address continuity of child care over time.
[6] The USDA Urban Institute study (Mills, et. al.) included focus groups with participants and interviews with community providers that flesh out some of the consequences of churn in SNAP.
[7] Mills, et. al., Chapter 6. The study counted a return to SNAP as churn if it occurred within four months.
[8] See Appendix 2.
[9] Idaho includes cases that do not reapply as a reason for procedural closure.
[10] The math for this: 10 percent closing X 65 percent of those reapplying = 6.5 percent, compared to 40 percent closing X 65 percent of those reapplying = 26 percent.
[11] Because we are focusing at churn from procedural problems at renewal, we have not focused on this type of closure, but if the state is measuring the share of new applications that come from recent participants, they will be a part of the story.
[12] California distinguishes between “total” applications from churn, which is the share of applications that come from any household that participated recently, and “recertification” churn, which is the share of applications that come from cases whose case recently closed at recertification. Recertification churn represents about 80 percent of churn from households that reapply within 30 days, and about a third of churn from households that reapply over the 30- to 90-day period. See http://www.cdsscounties.ca.gov/foodstamps/ for California’s churn data.
[13] In SNAP, because of fixed certification periods, cases that do not reapply at the end of a certification period are not generally counted as a closure, but rather as an expired certification period. They should be counted in the churn rate, however, if they reapply within a short timeframe.
[14] States are required to provide Medicaid beneficiaries a renewal notice and give them at least 30 days to respond prior to terminating coverage. They also must consider the consumer for eligibility in other categories of Medicaid and other insurance affordability programs.
[15] Monica Rohacek, “Early Lessons from the Work Support Strategies Initiative, Idaho,” The Urban Institute, March 2013, http://www.urban.org/UploadedPDF/412791-Early-Lessons-from-the-Work-Support-Strategies-Initiative-Idaho.pdf.
[16] Mills, et. al., Chapter 5.
[17] See box 2 and Appendix 2 for a discussion of SNAP “simplified” reporting. The changes from the recently-enacted Child Care and Development Block Grant reauthorization are new. The approaches outlined here appear to be allowable, but specific guidance interpreting the new law is forthcoming.
[18] Pamela Loprest and Lindsay Giesen, “Early Lessons from the Work Support Strategies Initiative: North Carolina,” Urban Institute, March 2013, and Public Consulting Group, “North Carolina Department of Health and Human Services Aligned Certification Periods Pilot Study Final Report,” 2012, http://www.urban.org/UploadedPDF/412793-Early-Lessons-from-the-Work-Support-Strategies-Initiative-North-Carolina.pdf.
[19] See the National Standards for Culturally and Linguistically Appropriate Services in Health and Health Care at https://www.thinkculturalhealth.hhs.gov/Content/clas.asp. While specifically targeted to health providers, this resource provides useful information on culturally and linguistically appropriate service delivery that can be applied more broadly.
[20] USDA, “Best Practices in Developing Effective Supplemental Nutrition Assistance Program Client Notices,” May 2014, http://www.fns.usda.gov/sites/default/files/SNAP%20-%20Best%20Practices%20in%20Developing%20Effective%20SNAP%20Client%20Notices.pdf
[21] Alliance to Transform CalFresh, “Zero Churn Toolkit: Providing Food and Stability to Families in Need,” http://www.transformcalfresh.org/zerochurn.html. The information on the text messages is in a webinar from September 30, 2014.
[22] California’s CalFresh (SNAP) data dashboard, which in addition to information on churn includes information on SNAP/Medicaid overlap, timeliness, error rates, and other measures and demographic information, is available at http://www.cdsscounties.ca.gov/foodstamps/.
[23] If the study had instead used a three-month break in participation to define churn, then 70 percent to 83 percent of churners in the six states returned to SNAP within one month or less.) See Mills, et. al., Table 4.
[24] In SNAP states can receive a waiver from USDA to reinstate eligibility after a break in benefits during a certification period, including at the time a simplified report is due, but a new application is required after a certification period expires. In child care, states have flexibility to reopen cases.
More from the Authors
