- Home
- A Technical Assessment Of SNAP And Medic...
A Technical Assessment of SNAP and Medicaid Financial Eligibility Under the Affordable Care Act (ACA)
Beginning in 2014, the number of low-income people eligible for Medicaid will expand dramatically. The Affordable Care Act (ACA) sets a national minimum standard for Medicaid eligibility to cover most individuals with incomes below 133 percent of the poverty line.[2] The Supreme Court ruling leaves it up to states to decide whether or not to expand, but Medicaid will still be a critical pathway to health coverage for millions of low-income Americans in all states.
Health coverage has been out of reach for millions of low-income Americans because they frequently do not receive affordable coverage for themselves or their families through their employers, and private coverage is unaffordable for most low-income families. Even when public health coverage is available, many low-income individuals do not enroll. Making it easy for newly eligible and already eligible individuals to enroll in Medicaid will be crucial to the success of the ACA and its goal of reducing the number of uninsured.
States currently are developing new systems for enrollment into Medicaid that are designed to coordinate with the provision of premium tax credits subsidizing coverage offered through exchanges. As they transition to new systems, it will be important for states to ensure that they maintain coverage for all individuals currently enrolled in Medicaid, who often are in very low-income families with multiple health and educational barriers. There is a risk that some currently-enrolled Medicaid participants (as well as some newly eligible people) could lose or fail to secure coverage due to unintended problems, staffing gaps, confusion, or program errors, particularly if the eligibility process for Medicaid is separated from the process for other assistance programs.
To maximize coverage and reduce unnecessary administrative work for states, the Department of Health and Human Services (HHS) has proposed rules that will establish a simplified and streamlined process for enrollment in all health coverage programs. Eligibility for CHIP, premium tax credits and Medicaid for most non-elderly beneficiaries will be based on Modified Adjusted Gross Income (MAGI). The eligibility process will largely rely on the use of third-party data to verify eligibility factors. However, for many very low-income individuals, third-party data bases may not contain sufficient income information to determine eligibility. This could mean that these individuals would have to provide paper documentation to prove their income eligibility, making it less likely they would successfully enroll in coverage.
Millions of low-income individuals already provide verified information about their incomes to establish their eligibility for the Supplemental Nutrition Assistance Program (SNAP). More than 80 percent of the households eligible for SNAP that don’t contain an elderly member participated in SNAP in 2010. And using CBO’s baseline, more than 35 million non-elderly, non-disabled individuals will be enrolled in SNAP in an average month in 2014 and 2015. CBO’s latest estimates, taking the Supreme Court decision into account, find that 58 million people whose eligibility is based on determination that their income is below 138 percent of the poverty line using the new MAGI rules will participate in Medicaid in a typical month in 2019.[3] With effective outreach and enrollment procedures, and if more states opt for the Medicaid expansion than CBO anticipates, the number could be higher.
Using SNAP information to determine and renew eligibility for Medicaid would make it much more likely that low-income SNAP participants enroll in Medicaid. It also would reduce Medicaid administrative costs for states and the federal government.
HHS’s regulations ensure that states make use of SNAP information for verification of eligibility for insurance affordability programs. The strategic use of these data will help states meet enrollment goals and reduce the burden for individuals and states.
The use of SNAP data for Medicaid determinations can be greatly simplified if states are allowed to deem SNAP participants as financially eligible for Medicaid without requiring states to recalculate their income. This would give states an extremely powerful tool to easily extend Medicaid coverage to newly eligible groups and to ensure that individuals currently enrolled in Medicaid do not lose coverage as states are building and transitioning to new health enrollment technology and business process systems. It would also give states more options in designing the information technology that will support eligibility functions and ensure that many of the lowest income individuals have access to real-time eligibility determinations.
This paper uses data from SNAP to explore how many SNAP recipients are certain to be financially eligible for Medicaid, and what the important differences between SNAP and Medicaid may be.
Our analysis, described in detail below, finds that for about 75 to 80 percent of SNAP households that have members who may be eligible for Medicaid using a MAGI-based determination of income (because the households have at least one member who is under 65 or not receiving SSI) SNAP information is sufficient to determine that household members have incomes below the applicable income standard (see Appendix 1).
Many of the individuals in the remaining 20 to 25 percent of SNAP households will also be financially eligible for Medicaid, but it may take additional information from the household to confirm eligibility, or a more sophisticated “rules-based” automation capacity that, for example, allows for different treatment of income.[4] For example, a SNAP household may include an individual who no longer qualifies for SNAP because the individual has reached the 3-month time limit for unemployed childless adults. Not all of this person’s income is counted when the SNAP eligibility and benefits of the other members of the household are determined. In this case, the state could use SNAP data to recalculate the household’s income to determine its members’ eligibility for Medicaid, but some additional computer programming would be needed to accomplish the different treatment.
Why SNAP Is a Good Source of Information About Low-Income Households
As detailed later in this memo, the overwhelming majority of SNAP participants are in households with incomes below 138 percent of the poverty line. This is because:
- Most SNAP recipients are poor. Of all SNAP households, only 15 percent had gross income above 100 percent of the poverty line in 2010. For households with children, half have gross income below half of the poverty line. In 2010, only 2.5 percent of SNAP households had gross income above 138 percent of the poverty line.
- Almost all the differences between Medicaid and SNAP in terms of income counting go in the direction of SNAP counting more income than MAGI. (See Appendix 2 for a comparison of the rules for counting income.)
SNAP household income data are rigorously verified and are no more than six months old at any point in time, making it a current and reliable source of income information.[5] (See Appendix 3.) Basing financial eligibility for Medicaid on participation in SNAP would make it possible to determine eligibility for these individuals in a way that is consistent with the streamlined system described in HHS guidance and regulations.
Why States Could Benefit From a Simplified Process to Use SNAP Data
HHS eligibility rules require states to use SNAP information in the determination of Medicaid eligibility if the state determines such information is useful.
As is the case today, in 2014 SNAP and Medicaid will use different methodologies for determining income and defining household units. Under the proposed regulation calling for states to use SNAP data in making Medicaid income determinations, we assume that the state would have to re-calculate specific income items for each SNAP unit member in order to apply the Medicaid methodology. A simpler alternative would be for states to use SNAP participation information without recalculating using the Medicaid methodology for some or all very low-income SNAP households.
For example, consider a household of three consisting of an unmarried couple and a child who is the woman’s biological daughter. The man earns $750 per month and the woman earns $250 per month and receives $200 per month in Temporary Assistance for Needy Families (TANF) benefits. The combined monthly income for this three person household would be $1,200, or 80 percent of the poverty line. SNAP would consider all members to be in the same household if they purchase and prepare food together, and all of the income would count in determining income eligibility for the three person household. For Medicaid, financial eligibility of the woman and her child would be based on a unit of two and household income would consist of the woman’s earnings of $250 a month (but not the TANF), which would be well below 138 percent of poverty. The man’s Medicaid unit would include himself and the woman and her daughter if he claims them as dependents on his tax return.[6] If he does not claim them as dependents, his eligibility for Medicaid would be considered separately as a unit of one with his monthly income of $750. In this case the state could dispense with figuring out the tax-filing relationship and excluding the TANF income because the combined monthly SNAP income of $1,200 is below 138 percent of the poverty line for a household of one. Thus, there is no possibility that any member of the household could be financially ineligible for Medicaid. If the state used SNAP participation to confer financial eligibility the Medicaid agency would not need to inquire about the household’s tax filing status and verify the income of each individual.
Such an approach would allow states to simplify their processes and reduce staff burden. It would give states options as they move towards developing or upgrading their eligibility systems, would potentially help them manage the transition to new systems, and would facilitate using SNAP as an outreach vehicle to find and enroll newly eligible individuals. There are a number of ways states could use such an option to simplify their processes.
- New applicants using a health-only online application: It is expected that states will develop eligibility systems and online applications that enable them to verify eligibility factors in “real time” using third-party data sources, including SNAP data. Using the option we propose, these systems could be programmed to determine which households could be found financially eligible for Medicaid based on their participation in SNAP. For example, states could add the list of SNAP recipients who are certain to be financially eligible for Medicaid to their state data hub that their Medicaid eligibility system will look to for automated sources of verification. More applicants could have their eligibility determined in “real time.”
- Initial and ongoing outreach: States will face a formidable challenge in processing applications for large numbers of newly eligible individuals in 2014. In 2013 states could begin educating SNAP participants about the new coverage opportunity. Messages about the Medicaid expansion could be included with SNAP applications, re-certifications and six-month reports. These forms could be modified to allow households to consent to use information provided for SNAP for the purpose of completing Medicaid eligibility determinations.[7] Using SNAP participation as the basis for a finding of financial eligibility for Medicaid would significantly reduce workload for staff. If states needed to limit the option to a subset of SNAP participants, they could send a supplemental form to get additional information to complete the Medicaid eligibility determination. A similar process could be used on an ongoing basis to enroll individuals who apply for SNAP coverage who are not already enrolled in health coverage.
- Annual renewals: Under the Medicaid eligibility rules, states must use data in case files and third-party data sources whenever possible to renew Medicaid eligibility. Using SNAP participation as the basis for an income eligibility finding would significantly increase the number of renewals that could be accomplished without requiring documentation from beneficiaries. States could use SNAP participation at the time of a beneficiary’s scheduled annual Medicaid renewal, or they could use “rolling renewal,” which pushes forward the Medicaid renewal date by 12 months at the time beneficiaries are re-certified for participation in SNAP.
It is likely that some states would find this approach allows them to keep more currently-enrolled individuals connected during the transition to their new eligibility systems and allow for a greater share of applications and renewals for the lowest income families to be done in “real time.” The box on the next page provides examples of how states could use SNAP participation as the basis for a finding of financial eligibility for Medicaid.
Box1: How Different States Could Use the Proposed State Option
There are a number of ways states could use SNAP participation to determine financial eligibility for Medicaid. Consider three types of states:
- States that have completely separate workers and eligibility systems for Medicaid and SNAP and expect to maintain this structure in 2014. (Alabama, Louisiana, Massachusetts, and South Carolina are examples of such states now.) These states could create a bridge between their SNAP and Medicaid systems so that certain people who apply through the health door would automatically meet Medicaid income eligibility requirements with no need to further verify their income. Similarly, information on certain people who apply for SNAP through the human services door and also want to apply for Medicaid could be forwarded to the health agency with a flag that identifies them as income-eligible with no need for additional income verification.
- States with integrated eligibility processes for SNAP and Medicaid for families who apply through the human services office (more than 40 states today) that intend to continue that practice in the future. At least some of these states expect to experience a transition period during which their SNAP eligibility will not be integrated into the new eligibility system they are creating for Medicaid. These states may, for a number of years, have SNAP and Medicaid in two different eligibility systems but may expect the same worker to process eligibility for both so that the separate systems are invisible to the family. Under this approach, the Medicaid system could be designed to have a simple flag that identifies individuals who participate in SNAP (in households that meet certain criteria) so that once the state worker completes the SNAP determination, income eligibility can be assumed (and verified) for Medicaid and the worker doesn’t need to re-enter all of the income data into the Medicaid system or re-calculate the income using MAGI methodology.
- States that have integrated eligibility for SNAP and Medicaid now — so that families can apply for Medicaid when they apply for SNAP — but are moving Medicaid eligibility to a new health insurance agency with an online portal and separate process, with no immediate plans for integration with human services. These states could create a way that SNAP eligibility workers could process income eligibility for Medicaid up to a point by entering the information in the online application (perhaps with special status), and the application could then be forwarded to the health agency. This would be far preferable to just referring SNAP participants to a web address of the health online application or even to a kiosk in the lobby with the online health application.
At renewal, for all states, this approach would allow for a simpler process for households that are up-to-date on their SNAP information. Once a state determines that a household qualifies in this manner, if nothing substantial has changed, Medicaid eligibility can be pushed forward 12 months at each SNAP report or recertification.
Identifying SNAP Households That Are Certain to Be Financially Eligible for Medicaid
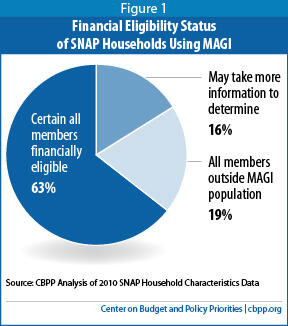
We found that SNAP households fall into three categories:
- About one in five SNAP households (19 percent) have no household members who could be eligible using MAGI rules because all household members were age 65 or older or received SSI (see figure 1).[10] There were 2.9 million such households in 2008 and 3.5 million in 2010.
- Of the other households, which include members whose eligibility will be determined based on MAGI rules:[11]
- 75 to 80 percent are certain to be financially eligible for Medicaid, based on the data used to determine their eligibility for SNAP. There were 7.6 million such households with 18.0 million potentially Medicaid eligible members in 2008, and 11.5 million such households with 25.8 million potentially Medicaid eligible members in 2010.
- 20 to 25 percent of households are very likely to contain Medicaid eligible members, but the state may need more information.[12] There were 2.0 million such households with 7.0 million potentially Medicaid eligible members in 2008, and 3.3 million such households with 11.3 million potentially Medicaid eligible members in 2010.
For a detailed table, see Appendix 1. For a description of the methodology, see Appendix 4.
SNAP Households Certain to Be Financially Eligible Using MAGI
The households we call “certain to be financially eligible” (75 to 80 percent of households with members who may be eligible for Medicaid using MAGI rules) are households where, based on household income and the relationship among the people who live together as reported for SNAP, states can be certain that the household members are financially eligible for Medicaid using MAGI rules. Most differences between SNAP unit and income rules and MAGI are differences that would make someone more likely to be eligible for Medicaid than SNAP. For example, pregnancy is not considered in determining eligibility for SNAP. Considering pregnancy in Medicaid makes the household larger and the income limit higher, if the pregnant woman is income-eligible for SNAP, she will certainly also be income-eligible using MAGI rules.
SNAP participants certain to have income below the applicable Medicaid income standard are households with gross income at or below 138 percent of the federal poverty level in which:
- All members are eligible for SNAP (so the total income of all members is counted), and
- The household falls into either of the following two groups:
- The household consists of individuals who live alone, parents living with their children, or married couples (with or without children), with the result that they will also be considered a household under Medicaid rules — and there are no other members present who may not be in the Medicaid unit; or
- Other members are present in the household, but the total household income is below 138 percent of the poverty level for a household of one, so it would be impossible for any household members, if they were a separate unit, to be ineligible for Medicaid; and
- There is no income from sources that may be more likely to be excluded in SNAP than under MAGI and there are no tax unit members living outside the home with substantial income. Both of these issues are rare and are discussed in more detail below.
SNAP Households That May Require More Information to Determine Financial Eligibility for Medicaid Based on a MAGI Determination
Below we enumerate the types of households in which members might qualify for SNAP but may not have income below Medicaid’s applicable income standard. Most of the people in these types of households actually have very low incomes, and they are very likely to qualify for Medicaid. It is just that states may need additional information if they wanted to be certain that these people’s income falls below the applicable income standard. (See figure 2.)
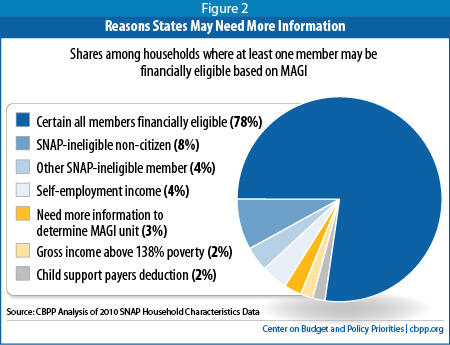
- Households that include ineligible immigrants (nationally, 8 percent of SNAP households with potentially Medicaid eligible members under MAGI rules, although the share varies substantially among the states). In SNAP, for households with ineligible immigrants, states have several options for how they count the income of the ineligible members in determining the eligibility of the other household members (and the options vary depending on whether the immigrant would have been eligible under pre-1996 rules.) Most states count a pro-rated share of the income of the ineligible immigrants toward the eligibility of the other household members (and the household size includes only the eligible members.) The rules in Medicaid will be based on the general household and income rules that apply for each individual seeking coverage. It is possible a state could choose an option in SNAP that would treat these households the same as in Medicaid. A state could also identify certain households where the state is certain that the SNAP household members are financially eligible for Medicaid, or could automate a recalculation based on the different rules. However, because it could be complicated, and because the state would still need to determine eligibility under the different programs’ immigrant eligibility rules, for this analysis we have excluded these households. In the states with large populations of ineligible immigrants it would likely be important to investigate the opportunities for including such households. A description of the treatment in SNAP can be found here: http://www.fns.usda.gov/snap/government/non_citizen_guidance.htm.
- Households that include other SNAP-ineligible members (4 percent of SNAP households with potentially Medicaid eligible members under MAGI rules). Some people are ineligible for SNAP because they are ineligible students, unemployed childless adults who have hit SNAP’s three-month time limit for such individuals, or people who have been disqualified for reasons such as failing to comply with work requirements. SNAP has rules for how income from these individuals is counted toward the income of the eligible household members (7 C.F.R. 273.11(c)). Many of these individuals would be eligible for Medicaid, so the determination of income eligibility would fully consider their income. The SNAP information could still be used to determine eligibility for Medicaid because information on the income of the ineligible members would be available, but the Medicaid agency might want to recalculate income for the Medicaid unit, including the income from household members who are ineligible for SNAP.
-
Households that may be defined differently for Medicaid and SNAP with income above 138 percent of the poverty line for a household of one (3 percent of SNAP households with potentially Medicaid eligible members under MAGI rules). In 2014, SNAP and Medicaid units will be defined differently. For SNAP, the unit (known as a household) is all individuals who live together and purchase and prepare meals together. Certain individuals, such as spouses and parents and their minor children, must be a household together. (See 7 C.F.R. 273.1) Medicaid usually will group spouses, parents, step-parents and children living together and will also take tax filing into consideration. They often will be the same as a SNAP household, but sometimes will not include people who are in the SNAP unit, such as other relatives and unrelated people.
It is possible that a SNAP unit could have gross income below 138 percent of poverty, but when the Medicaid units are split out and household size consequently falls, the Medicaid unit has income that exceeds the Medicaid eligibility threshold. For example, consider an unmarried couple with one unemployed worker with no income and one worker with earnings at 110 percent of the poverty line, resulting in a household of two with income of about $1,350 a month. This couple would be in the same SNAP household if they purchase and prepare food together, but would be considered as separate households for Medicaid unless the employed worker claimed the unemployed worker as a dependent on his or her tax return. The unemployed worker would be eligible for Medicaid, but the worker’s income of $1,350 a month would be 149 percent of poverty for a household of 1, and so would qualify for premium tax credits rather than Medicaid.
These types of household situations are problematic in determining Medicaid eligibility only if the SNAP household’s gross income is above 138 percent of poverty for a household of one. This is because if household income is below 138 percent of poverty for a household of one, it would be impossible for the household to be split in a way that the individuals in the SNAP household would not be income eligible for Medicaid. Thus, we have included such households as certain to be eligible if the gross income of all household members is below 138 percent of the poverty line for a household of one. In only about three percent of SNAP households that may have a Medicaid eligible member, the income of SNAP household members as a group is between 138 percent of the poverty line for a household of one and 138 percent of the poverty line for a household of the relevant size.[13]
- SNAP households with SNAP gross income above 138 percent of poverty (2 percent of SNAP households with potentially Medicaid eligible members under MAGI rules). SNAP households can have gross income over 138 percent of poverty for two reasons: 1) households with elderly and disabled members are not subject to the SNAP program’s 130 percent of poverty gross income limit; and 2) some states have lifted the gross income limit that applies to other households through a state option known as “broad-based categorical eligibility.”[14] Because households must still have net income (after deductions) that is low enough to qualify for a SNAP benefit, there are not a large number of households that have gross income above 138 percent of the poverty line. Individuals in these SNAP households would be less likely to be eligible for Medicaid, so states would need to take a closer look at their income and circumstances.
- Households with self-employment income (4 percent of SNAP households with potentially Medicaid eligible members under MAGI rules). In general, Medicaid rules for determining countable self-employment income are likely to be more generous than SNAP rules, and so a household with self-employment income that qualifies for SNAP will be almost certain to be eligible for Medicaid in 2014. (See 7 C.F.R. 273.11(a) for SNAP’s federal rules.) However, a handful of states have opted to simplify self-employment income determination for SNAP by developing a method to calculate the cost of doing business that uses a flat percentage of gross receipts, a figure based on average costs, or some other method. It is possible in these states that the SNAP methodology counts less income in some cases, and so someone could be eligible for SNAP but not Medicaid. According to FNS, in 2012 the following states used this option: Alabama, Alaska, California, Delaware, Georgia, Idaho, Iowa, Kansas, Maryland, Michigan, Ohio, Oklahoma, Oregon, South Carolina, South Dakota, Utah, Washington and Wyoming.[15] In the analysis, we assumed all states would need more information to determine Medicaid eligibility for SNAP households with self-employment income, which overstates the issue. The median amount of self-employment income counted in SNAP households that have such income was about $400 a month in 2010.
- Households that pay child support for children living outside of the household in states that have opted to exclude this from the gross income determination for SNAP (2 percent of SNAP households with potentially Medicaid eligible members using MAGI rules). In general, SNAP allows households that pay child support to deduct from their income the amount of the child support paid, since this income is not available to purchase food. States have the option to exclude the amount from gross income rather than deduct it so that such households are not made ineligible by the program’s gross income limit. According to FNS, the following states had adopted the state option in 2012: Arizona, California, Colorado, Connecticut, Delaware, Illinois, Iowa, Maine, Massachusetts, Missouri, New Mexico, New York, North Carolina, Rhode Island, South Dakota, and Washington.[16] In these states, for these households, “gross income” will be lower in SNAP and so someone could be eligible for SNAP but not Medicaid (though the state will know the amount of the child support that was excluded and could add it back in). In the analysis, we assumed all states would need more information to determine Medicaid eligibility for SNAP households with members who report paying child support, which overstates the issue. In addition, because of the SNAP option to raise the gross income limit through expanded categorical eligibility, some states may no longer use this option, or could reverse it in the future to conform with MAGI. The median amount of child support paid for households that make such payments was about $200 a month in 2010, according to SNAP administrative data.
-
Households where the SNAP unit may not correspond to the tax filing unit. In certain circumstances, tax units can be made up of people who do not live together. Thus, a SNAP household could include an individual who is not part of the tax unit and, conversely, a household may not include everyone in the tax unit. For reasons that we explain further below, we believe that this is not a significant issue, and that in most cases where this does occur, there is likely to be very minimal impact on Medicaid eligibility of individuals in the SNAP household. We are not able to model this issue using the SNAP data. Below are some scenarios.
- In the first scenario a married couple lives separately but file taxes jointly. One spouse could be in a SNAP household and the spouse living apart is not. The income of the spouse living apart may not be counted at all towards the SNAP household or, if he or she is making payments towards the household, only partially counted. Medicaid would count the spouse living apart towards the size of the Medicaid unit and all of his or her income would also count towards the Medicaid eligibility.
- The second scenario, in which a SNAP household includes an individual who is not part of the tax unit, most often occurs when a child within the SNAP household is being claimed as a tax dependent by a non-custodial parent. In this case, the fact that the child is claimed by someone outside of the SNAP household does not have bearing for the Medicaid eligibility of the child because Medicaid rules require that eligibility of children be based on the income of their custodial parent, regardless of who claims the child for tax purposes. But this may have an impact on Medicaid eligibility of other members of the SNAP household because the household size could change for remaining household members. For example, if there is a single mother living with her child that is claimed as a tax dependent by the non-custodial parent, the household size for the child would be two but the mother’s household size would be one because her child is claimed as a dependent by someone else.
-
The third scenario involves a taxpayer in the SNAP household claiming an individual who does not live with him or her as a tax dependent. The concern might be that an individual outside the SNAP household has additional income that is not being accounted for that would make members of the SNAP household ineligible for Medicaid. We believe that this should not be an area of concern since tax data show that these instances rarely occur. In 98 percent of all tax filings for the 2009 tax year, tax dependent exemptions were claimed for children living in the home.[17]
Even in the other two percent of tax filings, Medicaid and tax rules make it highly unlikely that a tax dependent who lives outside of the SNAP household will have income that will make others in the SNAP household ineligible for Medicaid. The tax rules for tax dependency require the individual to have minimal taxable income,[18] while the rules for when such income would count in Medicaid require that the individual have taxable income that is high enough to require him or her to file taxes. The likelihood of a person outside the home being a tax dependent and having taxable income sufficient to be required to file taxes is very small.
These issues will be rare, but, nevertheless, states could ask if there are any members of the tax unit living outside of the home that are required to file taxes. As in the circumstances described above, in most cases the families will still meet the Medicaid income standard but may need to provide additional information for a determination.
- Other issues we could not model. There may be some other small groups of SNAP recipients that would need to be excluded. For example, households with income from obscure sources that SNAP does not count but would be counted under MAGI; certain individuals in substance abuse treatment centers that receive SNAP as a subsidy to the institution; or recipients of Disaster SNAP. In addition, eligibility for college students is complicated in both SNAP and Medicaid, so they likely would need to be excluded in some circumstances. As states, CMS, and FNS conduct further analysis, they may uncover some additional issues.
Conclusion
Most SNAP participants will qualify for Medicaid in 2014. States in collaboration with CMS and FNS could develop processes and procedures that take advantage of the information states have verified in determining eligibility for SNAP benefits. Not only would this approach give states a new tool to facilitate real-time eligibility, but it could help to minimize disruption in health coverage during transitions as states build new health eligibility and enrollment systems that may not include SNAP until several years in the future.
(Additional detail on our analysis, information about the reliability of SNAP data, and the differences between SNAP and Medicaid can be found in the appendices to this memo.)
End Notes
[1] This paper was originally posted in March 2013, before the Department of Health and Human Services issued guidance that describes a state option very similar to the option envisioned in this paper. The current version contains only minor revisions to the version from March. The HHS guidance can be found here: “Facilitating Medicaid and CHIP Enrollment and Renewal in 2014,” Center for Medicaid & CHIP Services, U.S. Department of Health and Human Services, SHO #13-003, ACA #26, May 17, 2013, http://www.medicaid.gov/Federal-Policy-Guidance/Downloads/SHO-13-003.pdf.
[2] In determining eligibility for Medicaid, income equal to five percent of the poverty line will be disregarded. Thus, the effective minimum income standard for Medicaid will be 138 percent of the poverty line, which is the standard we use in this analysis.
[3] CBO’s baseline for fiscal year 2019 includes about 72 million children and non-elderly adults whose eligibility is not based on disability participating at any time over the year. CBO estimates that about 80 percent, or 58 million such individuals, will participate in an average month. (See “Spending and Enrollment Detail for CBO’s May 2013 Baseline: Medicaid,” at http://www.cbo.gov/sites/default/files/cbofiles/attachments/44172-Baseline2.pdf.) Not all of these individuals will be eligible based on a finding that their MAGI is below 138 percent of the poverty line. Some states may maintain Medicaid eligibility standards above that level for children and possibly for parents.
[4] CBPP estimates that among such SNAP households (those with at least one member who is under 65 or not receiving SSI), some 90 to 95 percent would ultimately be found financially-eligible for Medicaid.
[5] SNAP eligibility determinations are based on current and expected income and circumstances, which is consistent with the “point-in-time” eligibility determinations required for Medicaid. See 7 C.F.R. 273.10 for SNAP “budgeting” rules.
[6] A taxpayer can claim an unrelated individual as a dependent if they lived together for the entire year and the annual gross income of the dependent is below a certain threshold ($3,700 in 2011), and the taxpayer paid more than 50 percent of the dependent’s support.
[7] States can select to either obtain affirmative consent or notify households that information will be shared for the purposes of Medicaid eligibility and allow them the option to not disclose their information.
[8] The SNAP QC Characteristics data files and technical documentation are available at http://hostm142.mathematica-mpr.com/fns/.
[9] We present data for fiscal years 2008 (before the recession) and 2010. SNAP caseloads rose considerably over these years because of the recession, and it is not clear whether the number and characteristics of SNAP recipient households in 2014 and later years will be more like 2008 or 2010.
[10] Because the majority of states deem SSI recipients to be eligible for Medicaid, we did not consider individuals under 65 receiving SSI to be in the population of individuals whose eligibility for Medicaid will be determined based on MAGI methodology.
[11] Under section 435.911 of the Medicaid eligibility rule, all individuals under 65 not enrolled in Medicare whose income is below the state’s applicable income standard using MAGI rules will be considered eligible for Medicaid.
[12] See footnote 3 above.
[13] SNAP QC reviews focus on the people who are in a SNAP household together. The rules for SNAP households require people who purchase and prepare food together to be in the same unit. They also require spouses who live together and parents and their minor children who live together to apply together (“minor” children include individuals who are under 22 years old with their own children). There may be households we cannot identify with people who live together but are not included in the SNAP unit because they do not purchase and prepare food together. Our assumption is that for the most part, if people do not eat together, they probably do not claim each other as dependents or file taxes together and so would also be different MAGI units.
[14] For the list of the states that have higher gross income limits for SNAP, see USDA, Food and Nutrition Service, “Broad-Based Categorical Eligibility Chart” at http://www.fns.usda.gov/snap/rules/Memo/BBCE.pdf.
[15] USDA, Food and Nutrition Service, SNAP State Options Report, 10th edition, August 2012, at http://www.fns.usda.gov/snap/rules/Memo/Support/State_Options/10-State_Options.pdf, p. 13.
[16] Ibid, p. 12.
[17] IRS, Statistics of Income Division, July 2011.Table 2.3 All Returns: Exemptions by Type and Number of Exemptions by Size of Adjusted Gross Income, Tax Year 2009.
[18] The types of things that make someone likely to be a dependent are also likely to mean they do not have significant income. Tax exemptions can be claimed for dependents who are “qualifying children” or “qualifying relatives.” Qualifying relatives must meet an income test, and cannot have annual income exceeding $3,700. Among other requirements, qualifying children generally have to live with the tax payer for most of the year.
More from the Authors

Areas of Expertise
Recent Work:

Areas of Expertise
