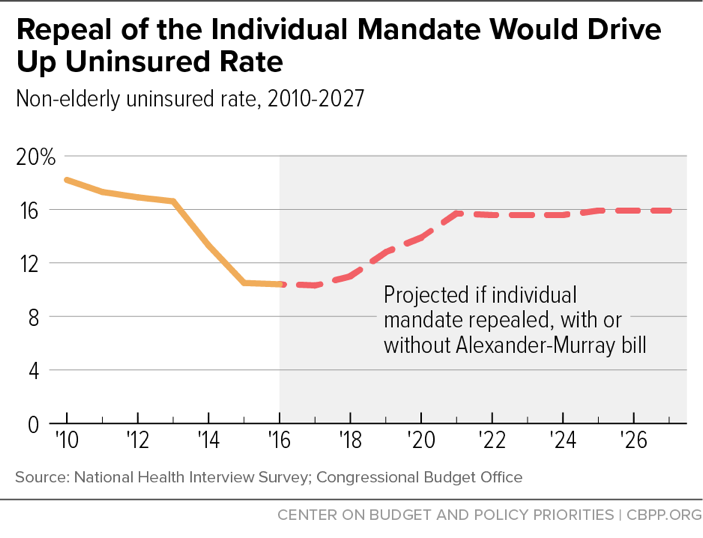
Alexander-Murray Legislation Can’t Undo the Severe Harm Resulting From Individual Mandate Repeal
End Notes
[1] See Jordain Carney, “Key GOP senator: ObamaCare payments likely to be included in funding bill,” The Hill, November 15, 2017, http://thehill.com/homenews/senate/360495-key-gop-senator-obamacare-payments-likely-to-be-included-in-funding-bill. While Senate Republican leaders have suggested that they might be willing to pass the Alexander-Murray bill after the tax bill, some House Republicans have continued to voice strong opposition. See Holly Rosenkrantz, “‘Terrible’ to Add Obamacare Fix in Spending Deal: Freedom Caucus,” Bloomberg, November 15, 2017.
[2] Robert Greenstein, “Alexander-Murray Agreement an Important Step Toward Bipartisanship on Health Care,” Center on Budget and Policy Priorities, October 18, 2017, https://www.cbpp.org/press/statements/greenstein-alexander-murray-agreement-an-important-step-toward-bipartisanship-on.
[3] Congressional Budget Office, “Repealing the Individual Health Insurance Mandate: An Updated Estimate,” November 2017, https://www.cbo.gov/system/files/115th-congress-2017-2018/reports/53300-individualmandate.pdf.
[4] “Senator Murray: Tacking Bipartisan Alexander-Murray Health Bill to Partisan Republican Tax Reform ‘Like Trying to Put Out a Fire with Penicillin,’” November 15, 2017, https://www.murray.senate.gov/public/index.cfm/newsreleases?ID=41D56DEB-C7E8-404A-82C7-924A4FF3CC75.
[5] Aviva Aron-Dine, “Senate Tax Bill Would Add 13 Million to Uninsured to Pay for Tax Cuts of Nearly $100,000 Per Year for the Top 0.1 Percent,” Center on Budget and Policy Priorities, November 15, 2017, https://www.cbpp.org/blog/senate-tax-bill-would-add-13-million-to-uninsured-to-pay-for-tax-cuts-of-nearly-100000-per-year.
[6] See, for example, Terrence Dopp, “Obamacare Mandate’s End Will Make Repeal Try Easier: Republicans,” Bloomberg, November 15, 2017.
[7] Silver plans are those with actuarial values of about 70 percent; these plans serve as the “benchmark” plans for setting premium tax credits.
[8] Even the minority of states that instructed insurers to increase premiums for all plans for 2018 to account for non-payment of CSRs may switch to instructing them to raise premiums for silver plans only for 2019. For a survey of state approaches, see Sabrina Corlette, Kevin Lucia, and Maanasa Kona, “States Step Up to Protect Consumers in Wake of Cuts to ACA Cost-Sharing Reduction Payments,” Georgetown Center on Health Insurance Reforms, October 31, 2017, https://ccf.georgetown.edu/2017/10/31/states-step-up-to-protect-consumers-in-wake-of-cuts-to-aca-cost-sharing-reduction-payments/. In many states, insurers only raised premiums for silver plans sold through the ACA marketplaces, meaning that lower-premium silver plans are available off marketplace.
[9] Ashley Semanskee, Gary Claxton, and Larry Levitt, “How Premiums Are Changing In 2018,” Kaiser Family Foundation, November 14, 2017, https://www.kff.org/health-reform/issue-brief/how-premiums-are-changing-in-2018/. Kaiser previously projected a 19 percent increase in silver plan premiums from non-payment of CSRs. Larry Levitt, Cynthia Cox, and Gary Claxton, “The Effect of Ending the Affordable Care Act’s Cost-Sharing Reduction Payments,” Kaiser Family Foundation, April 25, 2017, https://www.kff.org/health-reform/issue-brief/the-effects-of-ending-the-affordable-care-acts-cost-sharing-reduction-payments/.
[10] Centers for Medicare & Medicaid Services, “Health Insurance Marketplaces 2017 Open Enrollment Period Final Open Enrollment Report,” March 15, 2017, https://www.cms.gov/Newsroom/MediaReleaseDatabase/Fact-sheets/2017-Fact-Sheet-items/2017-03-15.html. Increases in sticker price premiums generally affect only unsubsidized individual market consumers, since premium tax credits adjust to shield subsidized consumers from premium increases.
[11] For many subsidized consumers, the increases in silver plan premiums resulting from the Administration’s decision not to pay CSRs will actually make gold and bronze plans more affordable than they otherwise would be. See Aviva Aron-Dine and Tara Straw, “The Outlook for Marketplace Open Enrollment,” Center on Budget and Policy Priorities, October 31, 2017, https://www.cbpp.org/research/health/the-outlook-for-marketplace-open-enrollment.
[12] For example, CareFirst, a major insurer in Maryland, Virginia, and Washington D.C., requested additional rate increases of 15 percent due to concerns about the individual mandate (see https://www.vox.com/2017/5/8/15563448/trump-insurance-premiums-2018), and Pennsylvania’s insurance commissioner reported in June that insurers would request additional rate increases averaging 14.5 percent if concerns about mandate non-enforcement or repeal were not addressed ( see http://www.media.pa.gov/Pages/Insurance-Details.aspx?newsid=248).
[13] Larry Levitt, “Insurers adjusted reasonably well to termination of cost-sharing payments and some people are actually paying lower premiums. Why is the individual mandate different? (thread),” Twitter, November 15, 2017, https://twitter.com/larry_levitt/status/930782635693084672.
[14] Interviews took place in December 2016 and January 2017. Sabrina Corlette et al., “Uncertain Future for Affordable Care Act Leads Insurers to Rethink Participation, Prices,” Urban Institute, January 2017, https://www.urban.org/sites/default/files/publication/87816/2001126-uncertain-future-for-affordable-care-act-leads-insurers-to-rethink-participation-prices_1.pdf.
[15] Congressional Budget Office, “Cost Estimate: Bipartisan Health Care Stabilization Act of 2017,” October 25, 2017, https://www.cbo.gov/system/files/115th-congress-2017-2018/costestimate/bipartisanhealthcarestabilizationactof2017_0.pdf
[16] In fact, CBO projected small coverage increases over time if CSRs are not paid. That’s because, as noted above, not paying CSRs makes coverage more affordable for some subsidized consumers. Congressional Budget Office, “The Effects of Terminating Payments for Cost-Sharing Reductions,” August 2017, https://www.cbo.gov/system/files/115th-congress-2017-2018/reports/53009-costsharingreductions.pdf.
[17] For a more complete discussion of these issues, see Aviva Aron-Dine, “Republicans Considering Increasing Number of Uninsured by Millions, Raising Premiums to Help Pay for Tax Cuts,” Center on Budget and Policy Priorities, updated November 9, 2017, https://www.cbpp.org/research/health/republicans-considering-increasing-number-of-uninsured-by-millions-raising-premiums.
[18] See Sarah Kliff, “The Newest GOP Health Idea? Auto-Enroll the Uninsured,” Vox, April 19, 2017, https://www.vox.com/policy-and-politics/2017/4/19/15363976/auto-enroll-uninsured-health-care-plan, and James C. Capretta, “Republicans are wrong about the individual mandate,” American Enterprise Institute, November 6, 2017, https://www.aei.org/publication/republicans-are-wrong-about-the-individual-mandate/.
[19] See Paul N. Van de Water, “Automatic Enrollment in Health Insurance Would Be Complex and Difficult to Administer,” Center on Budget and Policy Priorities, June 16, 2017, https://www.cbpp.org/research/health/automatic-enrollment-in-health-insurance-would-be-complex-and-difficult-to, and Sarah Lueck, “Commentary: House GOP Proposed Penalty for Non-Coverage Fails on Several Fronts,” Center on Budget and Policy Priorities, March 8, 2017, https://www.cbpp.org/health/commentary-house-gop-proposed-penalty-for-non-coverage-fails-on-several-fronts.