CBO Finds Health Reform's Medicaid Expansion Is an Even Better Deal for States
End Notes
[1] Congressional Budget Office, “Updated Estimates of the Effects of the Insurance Coverage Provisions of the Affordable Care Act: April 2014,” April 2014, http://cbo.gov/sites/default/files/cbofiles/attachments/45231-ACA_Estimates.pdf.
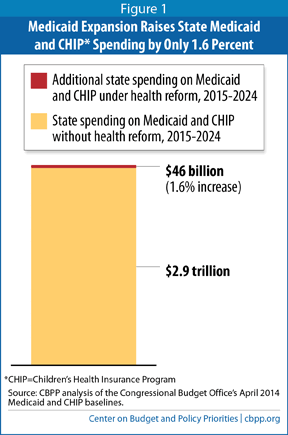
[2] In its February 2014 health reform baseline, CBO estimated that the Medicaid expansion and other health reform coverage provisions would raise state expenditures for Medicaid and CHIP by $70 billion over the next ten years (2015-2024). CBO’s new projection of a $46 billion increase is 34 percent less than its previous projection. Congressional Budget Office, “Insurance Coverage Provisions of the Affordable Care Act — CBO’s February 2014 Baseline,” February 2014, http://cbo.gov/sites/default/files/cbofiles/attachments/43900-2014-02-ACAtables.pdf.
[3] January Angeles, “How Health Reform’s Medicaid Expansion Will Impact State Budgets,” Center on Budget and Policy Priorities, revised July 25, 2012, https://www.cbpp.org/cms/index.cfm?fa=view&id=3801.
[4] Matthew Buettgens, Stan Dorn, and Caitlin Carroll, “Consider Savings as Well as Costs: State Governments Would Spend at Least $90 Billion Less with the ACA than Without It from 2014 to 2019,” Urban Institute, July 2011, http://www.urban.org/UploadedPDF/412361-consider-savings.pdf.
[5] Lewin Group, “Patient Protection and Affordable Care Act (PPACA): Long Term Costs for Governments, Employers, Families and Providers,” Staff Working Paper # 11, June 8, 2010, http://www.lewin.com/~/media/Lewin/Site_Sections/Publications/LewinGroupAnalysis-PatientProtectionandAffordableCareAct2010.pdf.