Shortly after the Supreme Court ruled that states can choose whether to adopt the health reform law’s Medicaid expansion to cover low-income parents and other adults, some governors declared that they will forgo the expansion, claiming it would place a heavy financial burden on their states.[1] Claims that states will bear a substantial share of the costs of expanding Medicaid, however, and that the expansion would drain state budgets do not hold up under scrutiny.
The Congressional Budget Office (CBO) estimates that the Medicaid expansion will add very little to what states would have spent on Medicaid without health reform, while providing health coverage to 17 million more low-income adults and children. In addition, the Medicaid expansion will reduce state and local government costs for uncompensated care and other services they provide to the uninsured, which will offset at least some — and in a number of states, possibly all or more than all — of the modest increase in state Medicaid costs. Expanding Medicaid is thus a very favorable financial deal for states.
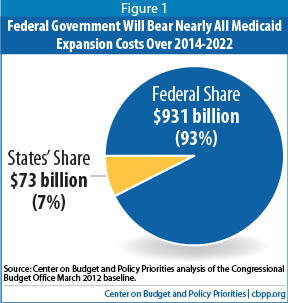
- CBO estimates show that the federal government will bear nearly 93 percent of the costs of the Medicaid expansion over its first nine years (2014-2022). The federal government will pick up 100 percent of the cost of covering people made newly eligible for Medicaid for the first three years (2014-2016) and no less than 90 percent on a permanent basis.
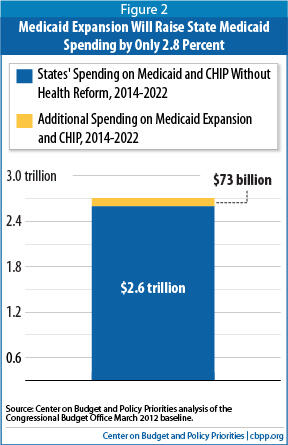
- The additional cost to the states represents a 2.8 percent increase in what they would have spent on Medicaid from 2014 to 2022 in the absence of health reform, the CBO estimates indicate.
- This 2.8 percent figure significantly overstates the net impact on state budgets because it does not reflect the savings that state and local governments will realize in other health care spending for the uninsured. The Urban Institute has estimated that overall state savings in these areas will total between $26 and $52 billion from 2014 through 2019. The Lewin Group estimates state and local government savings of $101 billion in uncompensated care.
Other independent analyses show similar or even more favorable results for states. An Urban Institute analysis finds that state Medicaid expenditures would likely increase by 1.4 percent over what states would otherwise spend on the program from 2014 through 2019, before taking offsetting savings in uncompensated care and other health services into account, while the Lewin Group estimates an increase in state Medicaid expenditures of 1.1 percent over that period. These estimates reflect the increased state costs for Medicaid but not the offsetting savings states will also secure in uncompensated care and other health services.
Critics argue that state budgets will be hit hard by the costs of extending Medicaid to people who are already eligible for the program but unenrolled under current state rules, but will enroll as a result of health reform. States will receive the standard federal Medicaid matching rate for covering these individuals (57 percent, on average), which is well below the 93 percent average federal match noted above for people whom the Affordable Care Act makes newly eligible for Medicaid. But the CBO, Urban Institute, and Lewin Group estimates all account for the cost to states of covering the already-eligible individuals who will enroll. CBO’s 93 percent average federal share of the Medicaid expansion’s costs and the estimate that state Medicaid costs will rise just 2.8 percent on average — and the even lower Urban Institute and Lewin estimates of state costs — reflect this cost.
Moreover, health reform’s other provisions, such as the individual responsibility requirement to have health coverage (sometimes referred to as the “individual mandate”) and the measures to simplify Medicaid enrollment procedures, will remain in place under the Supreme Court decision. These provisions will themselves boost enrollment among those already eligible for Medicaid regardless of whether states take up the expansion. Thus, the additional cost to states of expanding Medicaid to cover more low-income people is smaller than the CBO and other estimates would indicate, because those estimates don’t distinguish the increased costs due to higher enrollment of already-eligible individuals that will occur from the other features of the bill from the increase in cost and enrollment that may result just from the Medicaid expansion.
In short, the Medicaid expansion will cover 17 million low-income people at a very modest cost to states — a cost that will be at least partly offset by savings in uncompensated care and other state-funded services for the uninsured.
A state’s decision not to go ahead with the Medicaid expansion, despite this extremely favorable financing, would have adverse consequences for many poor individuals and families without health insurance.
- In the typical (or median) state today, a working-poor parent loses eligibility for Medicaid when his or her income reaches only 63 percent of the poverty line (about $12,000 for a family of three in 2012). An unemployed parent must have income below 37 percent of the poverty line (about $7,100 in 2012) in the typical state in order to qualify for the program. Only a handful of states provide coverage to any low-income adults without dependent children, regardless of how poor they are.[2]
- Only individuals with incomes between 100 and 400 percent of the federal poverty line will be eligible for premium and cost-sharing subsidies to buy coverage through health reform’s new health insurance exchanges. [3]
- In states forgoing the Medicaid expansion, therefore, working people with incomes above the Medicaid eligibility limit but below the poverty line would have neither Medicaid nor subsidized exchange coverage. Due to the low wages they earn, many working-poor parents would have incomes too high to qualify for Medicaid but too low to qualify for subsidies to buy coverage in the exchanges. Many would likely remain uninsured and go without needed care. According to the Urban Institute, there are 11.5 million uninsured people nationwide with incomes below the poverty line who would be newly eligible for Medicaid under the expansion.[4] They would be at risk of remaining uninsured if their states do not move forward and expand Medicaid.
The Affordable Care Act (ACA) calls for states to expand Medicaid eligibility to 133 percent of the poverty line for all non-elderly citizens and individuals who have lawfully resided in the United States for more than five years, are not age 65 or over, and are not eligible for Medicare. CBO estimates that as enacted, some 17 million more individuals — most of whom are now uninsured — will enroll in Medicaid and the Children’s Health Insurance Program (CHIP) by 2022.
[5] To minimize the financial burden on states of the Medicaid expansion, the ACA calls for the federal government to pay nearly 93 percentof the expansion’s cost over the next nine years, according to CBO.
Specifically, the federal government will, for the first three years (2014-2016), assume 100 percent of the costs of covering those made newly eligible by the health reform law.[6] Federal support will then phase down slightly over the following several years (95 percent in 2017, 94 percent in 2018, and 93 percent in 2019). By 2020 and for all subsequent years, the federal government will pay 90 percent of the costs of covering these individuals.
According to CBO, between 2014 and 2022, the federal government will pay $931 billion of the cost of the Medicaid expansion, while states will pay roughly $73 billion, or 7 percent (see Figure 1).
[7] This $73 billion equals a 2.8percent increase above the $2.6 trillion that states were projected to spend on Medicaid over the same timeframe in the absence of health reform (see Figure 2).
As noted, health reform will likely increase participation among individuals who are currently eligible for Medicaid but not enrolled. States will receive the regular federal Medicaid matching rate for covering these people. CBO’s $73 billion estimate of the net increase in state Medicaid costs due to the expansion includes the cost of covering more currently eligible individuals.
Other analyses support these results. An Urban Institute analysis found that between 2014 and 2019, state Medicaid spending would increase by 1.4 percent over what states would spend without the expansion (and by 2.9 percent if participation among currently- and newly-eligible individuals turns out much higher than expected).[8] The Lewin Group found that between 2014 and 2019, total state Medicaid spending will increase by $17.4 billion, which represents an average increase in spending of 1.1 percent over this period.[9]
Massachusetts Shows That Expanding Coverage Reduces Other Health Care Costs
Massachusetts’ experience with its health reform efforts offers strong evidence that expanding coverage under a comprehensive health reform plan can lead to sizeable reductions in state costs for uncompensated care.
Massachusetts enacted legislation in 2006 to provide nearly universal health care coverage. The legislation combined a Medicaid expansion with subsidies to help low- and moderate-income residents purchase insurance, an employer responsibility requirement, and a requirement for individuals to obtain coverage. All of these also are core elements of the Affordable Care Act.
With the expansion of affordable health insurance options and the institution of an individual mandate, spending on uncompensated care decreased significantly in Massachusetts. As part of its health reform effort, the state replaced its Uncompensated Care Pool (also known as “Free Care”) with the Health Safety Net, which provides financial support to public hospitals and community health centers that serve low-income residents who are uninsured or underinsured or who have significant medical needs. In 2008, the first full year of health reform implementation, Health Safety Net payments were $252 million, or 38 percent, less than the previous year’s Uncompensated Care Pool payments.a
This reduction in uncompensated care costs coincided with a decline in the share of residents who are uninsured. Only 2.7 percent of residents were uninsured in 2009, compared to 5.7 percent in 2007.b
a Massachusetts Division of Health Care Finance and Policy, “2009 Annual Report – Health Safety Net,” December 2009.
b Massachusetts Division of Health Care Finance and Policy, “Access to Health Care in Massachusetts: Results from the 2008 and 2009 Massachusetts Health Insurance Survey,” November 2009.
To assess the fiscal impact on states of the Medicaid expansion, one must look at more than just the effects on Medicaid spending, because expanding Medicaid will reduce state and local costs for health services provided to people who are uninsured now but will be covered by Medicaid as of 2014.
- By sharply reducing the number of people without health insurance, the Medicaid expansion will reduce state and local costs for hospital care for the uninsured. In 2008, state and local governments shouldered $10.6 billion, or nearly 20 percent, of the cost of caring for uninsured people in hospitals, according to Urban Institute research.[10]
- The Medicaid expansion will also push down state costs in providing mental health services to the uninsured. State and local governments provided 44 percent of the funding for state mental health agencies in 2009, amounting to $17 billion.[11]
Thus, a portion of CBO’s estimated $73 billion in additional state Medicaid spending under the new law will be offset by state savings in other areas, as poor uninsured people become eligible for Medicaid and the federal government begins paying most of the costs of providing care to people for whom states have been bearing significant costs until now. Put another way, part of a state’s new costs under the Medicaid expansion will actually substitute for existing state spending on the uninsured.
The savings that states realize from this large reduction in the number of the uninsured should grow over time. Experts at the Urban Institute have noted that in the absence of health reform, state uncompensated care costs would increase as employer-sponsored insurance continued to erode and the ranks of the uninsured continued to grow.[12] By shrinking the number of uninsured people and having the federal government pick up the overwhelming bulk of the tab, the Medicaid expansion will ease cost pressures on states stemming from uncompensated hospital care, mental health care, and other health care services. Urban Institute researcher John Holahan has observed: “There are a number of states that have state-funded programs that will no longer be necessary and virtually every state and localities within those states make payments for uncompensated care to support the uninsured. A lot of that can go away and those savings would offset any new state spending on Medicaid.”[13]
A separate Urban Institute study estimates that under the ACA, states would see a decrease of between $26 billion and $52 billion in uncompensated care costs over the 2014-2019 period.[14] The Lewin Group concluded that there will be reductions in net spending on state and local government safety net programs to provide care to the uninsured of $101 billion between 2014 and 2019.[15]
Health reform also will bring other benefits to states. Its insurance-market reforms should improve access to health insurance for people at all income levels, and the expansion of health-care coverage will help protect residents against preventable illnesses and should result in a healthier workforce.[16]
Some critics of the health-reform law have heavily overstated the cost that various states will face as a result of the law’s Medicaid expansion. They have cited estimates purporting to show very large increases in state Medicaid costs, but those estimates have typically been derived through the use of various highly problematic assumptions, including the following:
- Assumptions of Medicaid participation rates that are inconsistent with decades of experience in means-tested programs. Some estimates assume that 100 percent of the people who will be eligible for Medicaid will sign up. Nomeans-tested public program has ever achieved a 100 percent participation rate. Even Medicare, a universal social insurance program, has a participation rate of only 96 percent, and a variety of other means-tested programs have participation rates of 43 percent to 86 percent.a While a mandate to have health insurance, requirements to establish a simplified and seamless enrollment process, and the publicity and outreach efforts surrounding the expansion should result in increased enrollment, the evidence is overwhelming that the participation rate will not be 100 percent.b
- Assumptions concerning “crowd out” rates among already-insured people that are inconsistent with historical experience and the research in the field. Some estimates adopt unplausible assumptions that all or a very substantial share of insured individuals who become eligible for Medicaid will drop their existing coverage and enroll in Medicaid instead. Estimates of increased Medicaid costs generated for Mississippi, Nebraska, and Indiana have assumed that between 35 and 45 percent of all new Medicaid enrollees in the state will be people who drop private coverage to enroll in Medicaid.c The research indicates, however, that “crowd-out” rates of this magnitude are extremely unlikely. Studies that have looked at whether Medicaid crowds out private health insurance, focusing primarily on state expansions of children’s Medicaid eligibility in the 1990s, show that between 10 percent and 20 percent of new Medicaid enrollees previously had private coverage, rather than much higher percentages.d
- Assumptions of costs per newly enrolled Medicaid beneficiary that the data show to be heavily overstated. An estimate of increased state costs in Mississippi concludes that if the ACA’s Medicaid expansion had been in effect in 2009, it would have cost $4,540 per beneficiary for the adult expansion population and $2,421 per beneficiary for children. Yet estimates that the Urban Institute produced for the Kaiser Commission on Medicaid and the Uninsured find that per-capita costs for the current adult and child populations in Mississippi’s Medicaid program were far lower — $2,612 and $1,798, respectively — in 2009,e and the Urban Institute figures are based on actual data that the state reported. Another estimate, cited to show that the Medicaid expansion would impose high costs on Nebraska, contended that the per-beneficiary cost of covering parents whom the ACA will make newly eligible for Medicaid would have been $4,881 in that state if the expansion had been in effect in 2009. This figure is 74 percent higher than what the Urban Institute found to be the cost of covering parents in Nebraska’s Medicaid program in 2009. Since uninsured people eligible for coverage typically seek insurance when they become ill or develop medical conditions, experts overwhelmingly argue that the average cost per beneficiary of already-eligible people who have not signed up for Medicaid will be lower, not dramatically higher, than the average cost of those the program already serves.
a Dahlia Remler and Sherry Glied, “What Other Programs Can Teach Us: Increasing Participation in Health Insurance Programs,” American Journal of Public Health, January 2003.
b Sherry Glied, Jacob Hartz, and Genessa Giorgi, “Consider It Done? The Likely Efficacy of Mandates for Health Insurance,” Health Affairs, November/December 2007.
c For a more detailed analysis of these estimates and the studies from which they are drawn, see January Angeles, “Some Recent Reports Overstate the Effect on State Budgets of the Medicaid Expansion in the Health Reform Law,” Center on Budget and Policy Priorities, October 21, 2010.
d See, for example, Matthew Broaddus and January Angeles, “Medicaid Expansion in Health Reform Not Likely to Crowd Out Private Insurance,” Center on Budget and Policy Priorities, June 22, 2010; Gestur Davidson, Lynn Blewett, and Kathleen Call, “Public Program Crowd-out of Private Coverage: What Are the Issues,” The Synthesis Project, Robert Wood Johnson Foundation, June 2004; Lisa Dubay, “Expansions in Public Insurance and Crowd Out: What the Evidence Says,” Kaiser Family Foundation, October 1999; and Anna Sommers, Steve Zuckerman, Lisa Dubay, and Genevieve Kenney, “Substitution of SCHIP for Private Coverage: Results from a 2002 Evaluation in Ten States,” Health Affairs 26:529-537, March/April 2007.
e The Urban Institute and Kaiser Commission on Medicaid and the Uninsured estimates are based on data from Medicaid Statistical Information System (MSIS) and CMS-64 reports from the Centers for Medicare and Medicaid Services (CMS), 2010. Data provided were for 2007. Estimates were converted to 2009 dollars using the National Health Expenditure Survey’s estimate of the per capita growth in medical expenditures between 2007 and 2009.
Florida Governor Rick Scott recently declared that his state will not expand Medicaid, initially claiming that it would cost the state $1.9 billion a year. This figure is highly exaggerated and based on several deeply flawed assumptions that ignore how the Medicaid expansion will work after the Supreme Court decision. Even the governor’s office subsequently acknowledged that the $1.9 billion figure is overstated.a
According to the state’s Agency for Health Care Administration (AHCA), whose estimates themselves are overstated, as explained below, the Medicaid expansion will cost the state about $577 million in 2014, with the cost rising to the $1 billion level by 2016, and reaching $1.5 billion per year in 2022.b In contrast, the Urban Institute’s careful estimates find that the state would spend a total of $1.2 to $1.4 billion to expand Medicaid over the entire six-year period from 2014 through 2019.c
The Florida agency’s cost estimate suffers from some of the same methodological flaws as other state estimates that substantially overstate the cost of the Medicaid expansion. For example, it assumes 100 percent participation by uninsured people who are currently eligible or become newly eligible under the expansion — enrollment rates that are unrealistically high and inconsistent with program experience and research. It also assumes that 80 percent of Medicaid-eligible people who currently have employer-sponsored insurance would drop it and enroll in Medicaid, a “crowd out” rate far above what experience and research would predict. As a result, the state estimates that by 2019, nearly 2 million people will enroll in the state’s Medicaid and CHIP programs. In contrast, the Urban Institute estimates that enrollment in these programs is likely to be between about 950,000 under a standard participation scenario, and 1.4 million under a scenario where enrollment is much higher than expected.
Compounding these problems, the Florida agency’s estimate also uses the wrong federal matching rate for children ages 6 to 19 who would move from CHIP to Medicaid and includes $400 million in costs related to the ACA’s increase in Medicaid reimbursement rates for primary care physicians, which as discussed in the text of this analysis, is independent of the Medicaid expansion and should not be considered part of the expansion’s cost. The cost to Florida of expanding Medicaid and covering low-income adults and parents in 2022 is likely to be much closer to the Urban Institute estimates than to what Governor Scott is claiming.
a The St. Augustine Record, “Scott Overstates Cost of Health Care Overhaul,” accessed July 7, 2012 at http://staugustine.com/news/local-news/2012-07-04/scott-overstates-cost-health-care-overhaul#.T_UOtpGrGct.
b Agency for Health Care Administration, “Overview of the Federal Affordable Care Act,” January 4, 2012. Available at https://docs.google.com/presentation/d/1W-_7l8uN4-xmz-x3cyfALeKPwNOZWMdICh_qvffwywg/edit?pli=1#slide=id.p17
c See John Holahan and Irene Headen, “Medicaid Coverage and Spending in Health Reform: National and State-by-State Results for Adults at or Below 133% FPL,” Kaiser Commission on Medicaid and the Uninsured, May 2010.
Critics who claim that the Medicaid expansion is too costly have generally focused not on the cost of covering people who would be newly eligible, for whom the federal government will pick up nearly all of the cost, but on the cost of covering people who are currently eligible but not enrolled and will be funded at the state’s regular matching rate if they sign up. As mentioned previously, however, CBO’s estimate that states will spend only 2.8 percent more on Medicaid with health reform than without it, as well as the lower Urban Institute and Lewin Group estimates, include the cost of covering individuals who are currently eligible but uninsured.
Moreover, a state will have to incur certain costs under health reform even if it does not expand Medicaid. The marginal cost of the Medicaid expansion is much smaller than critics generally claim.
- The ACA’s requirement to purchase insurance, its simplification of Medicaid eligibility procedures, and the significant outreach and education that will be aimed at encouraging individuals to apply for subsidized coverage in the exchanges will increase Medicaid participation among individuals who are currently eligible but are not enrolled even if the state rejects the Medicaid expansion. A state will incur some additional costs for covering some of these individuals regardless of whether it expands Medicaid, and such costs cannot be attributed to the Medicaid expansion.
- The Affordable Care Act also requires states to increase Medicaid payments for certain primary care services in 2013 and 2014, with the cost of the increase funded entirely by the federal government. Although there is no federal requirement to maintain these rates beyond 2014, many states have indicated that they are likely to do so. To the extent that a state chooses to maintain these payment rates for its current Medicaid population, this cost, as well, should not be considered a part of the cost of expanding Medicaid. (If a state adopts the Medicaid expansion, the cost after 2014 of continuing to pay the higher rates for primary care services provided to newly eligible beneficiaries would be covered at the very high federal matching rate for newly eligible beneficiaries, so it would be paid almost entirely by the federal government.)
Contrary to claims made by some of the Medicaid expansion’s critics, the expansion does not impose substantial financial burdens on states. The additional state Medicaid spending that CBO expects to result from the expansion equals 2.8 percent of what states would have spent on Medicaid in the absence of health reform; this estimate includes the cost of covering individuals who are currently eligible but not enrolled. Estimates from other respected independent sources are similar or even lower — and both those estimates and CBO’s reflect state costs before factoring in state savings in areas such as uncompensated care costs and mental health services.
CBO expects that the expansion will result in 17 million more people being covered, which will significantly reduce state costs for uncompensated care and related programs and offset some or potentially all of the increase in state Medicaid costs.
In short, the federal government will pick up the overwhelming share of the costs of the Medicaid expansion, making it an extremely favorable deal both for states, as well as for their low-income uninsured residents.