BEYOND THE NUMBERS
Why Re-Enrolling in Federal Marketplace Makes Sense
As of December 5, only about 720,000 customers had returned to the federally run health insurance marketplace to re-enroll or switch plans for 2015, the New York Times reports. Our recent paper explains why people who bought private health insurance last year through the marketplace could pay more than they should next year unless they return to the marketplace to renew coverage. Next Monday is the deadline for enrolling in coverage to start January 1.
As our paper points out:
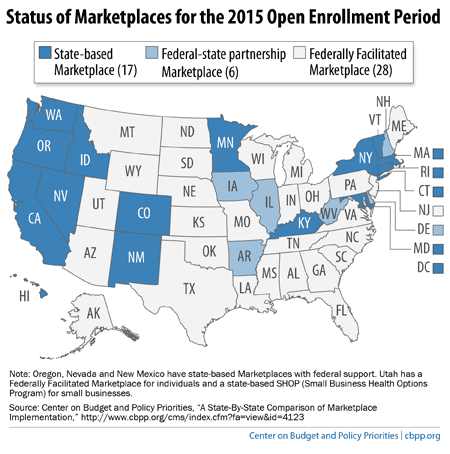
People in 34 states who enrolled in health coverage for 2014 through the Federally Facilitated Marketplace (FFM) will be automatically re-enrolled in the same plan in 2015 unless they choose a new plan through the FFM during the open enrollment season, which began November 15 (see map). While auto-renewal is an important backstop to avoid loss of coverage, it could leave many people paying more for health care than the Affordable Care Act envisions — and more than they will pay if they go back to the Marketplace.
Unless people provide updated information and have their eligibility re-determined, most who received subsidies for marketplace coverage in 2014 will automatically receive the same dollar level of subsidies in 2015. (These subsidies consist of advance payments of premium tax credits, which are paid to insurers on enrollees’ behalf to help cover the enrollees’ premiums.) But since many factors that affect the level of people’s subsidies change from year to year, a high percentage of people who auto-renew will receive advance premium credits that turn out to be too low or too high.
To avert such problems, consumers need to return to the FFM (rather than auto-renewing) to receive an updated eligibility determination. That is the only way to ensure they receive the correct level of benefits.