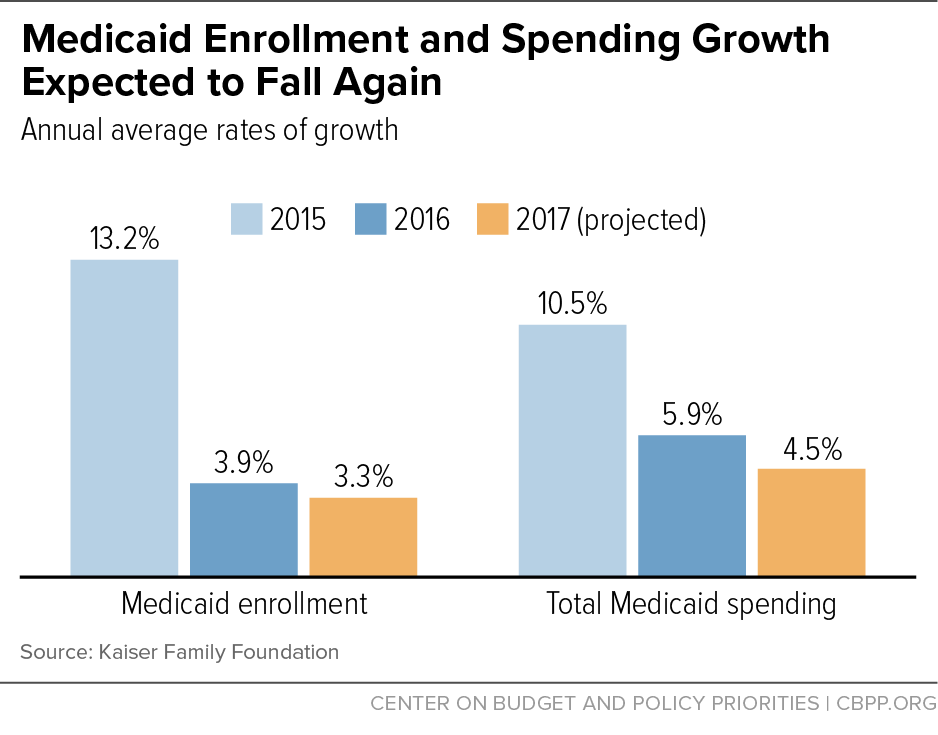BEYOND THE NUMBERS
Medicaid enrollment and spending growth is expected to slow again in state fiscal year 2017 as the initial effects of health reform’s Medicaid expansion taper off, the new Kaiser Family Foundation annual survey of state Medicaid directors finds. While expansion states expect to spend slightly more of their own money on Medicaid next year due to the expansion, states knew that would be the case before they adopted the expansion. Moreover, as we’ve noted, the expansion will continue producing net savings for many states in coming years.
The growth in combined state and federal Medicaid spending fell from 10.5 to 5.9 percent between state fiscal years 2015 and 2016 and states expect it to fall further in 2017, to 4.5 percent, the survey shows. States expect enrollment growth, which slowed dramatically in 2016, to continue slowing next year as well (see graph).
The 31 expansion states (plus the District of Columbia) expect their share of Medicaid costs to grow by 5.9 percent in state fiscal year 2017, compared to 4 percent in states that haven’t expanded. Next year will be the first year that states cover a modest share of the cost of covering people enrolled in the expansion. Under health reform, the federal government pays the entire cost of covering the newly eligible through calendar year 2016 and at least 90 percent thereafter.
The Kaiser report rebuts claims that Medicaid enrollment in expansion states is rising unsustainably. After an initial but expected large boost when the expansion took effect, enrollment will rise only 2.6 percent next year, expansion states project. That’s a key reason why they expect their overall (state and federal) Medicaid spending growth to slow for a third straight year.
Other reports show that some expansion states expect budget savings from expanding that will more than offset their share of expansion costs. For example, as more people gain health coverage, expansion states are spending less on health programs outside their Medicaid programs that are entirely state-funded, such as mental health and behavioral health programs. Expansion states are also collecting more revenue from existing taxes on health providers and plans.
Holdout states should strongly consider the positive effects of expansion, including larger gains in health coverage and net budget savings.