BEYOND THE NUMBERS
The share of Americans without health insurance remained at a historic low in 2017 and unchanged from 2016, the Census Bureau’s new Current Population Survey (CPS) data show. The year 2017 marked the fourth full year of the Affordable Care Act’s (ACA) major coverage expansions, but the first of them that didn’t show large coverage gains.
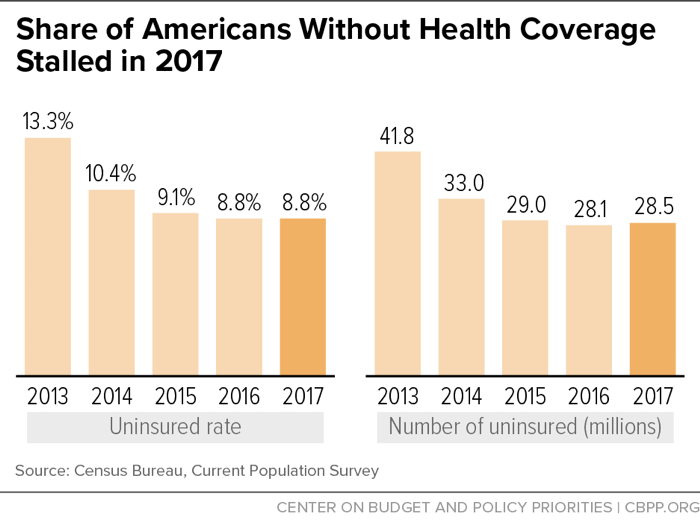
Some 8.8 percent of people lacked insurance in 2017, unchanged from the 2016 rate of 8.8 percent but still down more than one-third from the 2013 rate of 13.3 percent. The number of uninsured rose due to population growth, to 28.5 million people in 2017 from 28.1 million in 2016 (see chart).
Today’s CPS data show that the ACA proved resilient in the face of sabotage efforts by the Trump Administration and congressional Republicans that began in January 2017. These included the Administration’s cancellation of most federal outreach efforts toward the pivotal end of the open enrollment period for 2017 marketplace coverage and public confusion caused by year-long Administration and congressional attempts to repeal the ACA. (Today’s data do not reflect the effects of more recent sabotage efforts, including Administration rules that are designed to expand short-term health insurance plans and association health plans.)
Last year’s sabotage efforts likely prevented additional coverage gains by creating barriers to obtaining available and affordable coverage. Roughly 55 percent of the uninsured are eligible for health insurance coverage with financial assistance under the ACA or other public programs, the Kaiser Family Foundation and the Urban Institute find.
While the uninsured rate remained stable for the overall population, certain vulnerable groups experienced coverage declines in 2017:
- young adults aged 19 to 24, from a 13.1 percent uninsured rate in 2016 to 14.0 percent in 2017; and
- those living in states that haven’t expanded Medicaid coverage to low-income adults, from 11.8 percent to 12.2 percent.
Additional data from the Centers for Disease Control and Prevention (CDC) show that the 2017 uninsured rate remained unchanged at a record low (with data back to 1997), with the number of uninsured falling by more than 19 million since 2010 when the ACA’s first provisions took effect. While the new CPS data are considered the gold standard for national-level health coverage estimates, it’s necessary to use the CDC’s National Health Interview Survey (NHIS) data for longer-term trends due to technical changes in the CPS data over time. Results based on the NHIS, however, are highly consistent with those based on the CPS.
A growing body of research highlights the significant short- and long-term benefits of health coverage for the uninsured. For example, studies show that Medicaid coverage expands access to health care providers and services, improves health, increases preventive care and screenings, and reduces financial hardship. It also improves children’s long-term educational outcomes and earnings as adults.
Similarly, the Commonwealth Fund finds that more than 7 of 10 adults with marketplace coverage used it to visit a provider or fill a prescription — and 61 percent of them said they couldn’t have obtained this care without the marketplace coverage.
Trump Administration efforts to sabotage the ACA and congressional efforts to repeal it are likely responsible in large part for halting the historic progress of recent years in expanding health coverage in 2017. Unfortunately, the sabotage has continued in 2018, further threatening coverage gains. Policymakers should build on the ACA’s gains, enabling more people to get covered, rather than make it harder for them.