Medicaid is central to the health care system’s response to the current public health and economic crises. Millions more people will likely enroll in Medicaid in coming months because of the recession, the large majority of whom would otherwise become uninsured. For example, Urban Institute researchers estimate Medicaid enrollment will increase by 8 to 14 million people (16 to 29 percent) if unemployment climbs to 15 percent, consistent with estimates from the Congressional Budget Office (CBO) and other forecasters. Medicaid programs are also incurring other additional costs because of COVID-19, including new investments to protect enrollees and help physicians, hospitals, and other health care providers respond to the crisis.
The growing need for Medicaid coverage and services coincides with an unprecedented state budget crisis. Based on current economic forecasts, state budget shortfalls will total about $650 billion over the next several years, even larger than during the Great Recession. During past budget crises, states restricted Medicaid eligibility, including for seniors, people with disabilities, and pregnant women; made it harder for eligible people to get and stay covered; eliminated or cut key benefits; and cut payments to physicians, hospitals, nursing homes, and other providers. Under current circumstances, such cuts would not only worsen low-income people’s access to care, health, and financial security, but also would undermine the response to COVID-19.
To protect health coverage, policymakers need to substantially increase the federal government’s share of total Medicaid costs (the federal medical assistance percentage, or FMAP). The Families First Coronavirus Response Act took a useful first step, modestly raising the FMAP for the duration of the official public health emergency and incorporating maintenance-of-effort (MOE) protections that keep states from imposing new eligibility restrictions or terminating coverage while receiving the extra federal funds. But the Families First provision is inadequate in three respects:
- It provides far less funding than states need. Its 6.2 percentage-point FMAP increase is much less than federal policymakers provided during the Great Recession and too small to significantly discourage Medicaid cuts or encourage investments to address COVID-19. Together, the Families First FMAP funding and other flexible state fiscal relief in the subsequent Coronavirus Aid, Relief, and Economic Security (CARES) Act will fill only a small fraction of projected state shortfalls.
- It will end too soon. The downturn will likely continue well beyond the official public health emergency, with CBO now projecting that unemployment will still stand at 9.5 percent at the end of 2021. That means states will likely still face large budget shortfalls — and intense pressure to cut Medicaid — when the Families First funding and coverage protections end.
- It does not apply to enrollees covered through the Affordable Care Act (ACA) Medicaid expansion. That’s a serious problem because states that have expanded Medicaid will see much larger enrollment increases during the downturn and will likely incur higher costs related to COVID-19.
In its next COVID-19 response bill, Congress should include additional FMAP increases that, as the bipartisan National Governors Association has urged: (1) automatically adjust to meet need based on the depth of the downturn; (2) continue until the labor market (and thus state budgets) have truly recovered; and (3) apply to costs incurred for people covered through Medicaid expansion. Additional FMAP increases should also incorporate strong MOE protections for beneficiaries. The FMAP proposal in the Take Responsibility for Workers and Families Act (H.R. 6379), which House leaders introduced on March 23, meets all these principles; Congress should quickly adopt this or a similar policy.
Additional FMAP increases are needed even if Congress also provides other forms of state fiscal relief, as it should. Unlike other federal aid to states, FMAP increases protect health coverage by reducing states’ cost per dollar of Medicaid spending, incorporating MOE protections, and automatically providing more funding when Medicaid enrollment or costs increase more than expected. So while Congress can address state budget shortfalls using a variety of mechanisms, a substantial portion of the needed assistance should come in the form of additional FMAP increases.
Strong and effective state Medicaid programs are crucial to addressing COVID-19. But Medicaid programs are under strain, incurring additional costs due to the economic and public health crises.
As people lose their jobs or experience income declines in coming months, Medicaid will grow to meet need, preventing millions of people from becoming uninsured. Sharp spikes in uninsured rates would be harmful at any time — creating financial hardship, keeping people from accessing needed care, and costing lives. But under current circumstances, rising uninsured rates would also undermine the public health response to the virus, since uninsured people with COVID-19 symptoms may be afraid to seek testing or treatment that they worry they cannot afford, delaying detection of new cases.[1]
State policymakers on a bipartisan basis have urged Congress to provide additional FMAP increases, on top of the modest increase in the Families First Act.
- National Governors Association. “As noted in our previous supplemental request letter, governors continue to seek a temporary increase in Federal Medical Assistance Percentages (FMAP) from 6.2 percent to 12 percent, to help address the needs of Americans who have lost their jobs and employer-sponsored health insurance due to COVID-19. This increase should apply to states and territories that expanded Medicaid. The temporary 6.2 percent FMAP increase in the Families First Coronavirus Response Act (Pub. L. 116-127), is half of the average 12 percent FMAP increase states received from the 2009 Recovery Act. Governors request that the 12 percent FMAP be retroactive to Jan. 1, 2020, and remain until Sept. 30, 2021, regardless of unemployment conditions. After Sept. 30, 2021, the 12 percent FMAP increase should not be reduced until the national unemployment rate falls below 5 percent. Governors also request additional FMAP increases be determined based on the increase in a state’s unemployment rate” [emphasis added].a
- National Association of State Medicaid Directors. “The 6.2 percentage point FMAP increase in the Families First Coronavirus Response Act (FFCRA) is a helpful step for bringing fiscal relief to states. . . . However, states will experience unprecedented increases in enrollment applications as newly unemployed individuals turn to Medicaid for health insurance. States have never experienced as sudden shock in unemployment in such a short timeframe as they are experiencing today. . . . An additional FMAP enhancement is necessary to provide states with the fiscal support necessary to meet these increased demands on the Medicaid program. . . . These enhancements should extend beyond the COVID-19 national emergency, as the program’s heightened needs will not be directly tied to COVID-19.”b
- American Public Human Services Association (association representing state and local health and human services agencies). “Increase the Federal Medical Assistance Percentage (FMAP) up to at least 12% and extend the increase beyond the public health emergency to absorb increased demand for services during the economic recovery . . . and phase out the increase gradually over time based on economic conditions.”c
CBO projects that the unemployment rate will peak at 16 percent in the third quarter of this year, while Goldman Sachs projects it will reach 15 percent.[2] Urban Institute researchers project that an unemployment rate of 15 percent would result in an additional 8 to 14 million people enrolling in Medicaid, a 16 to 29 percent increase.[3] Over 40 percent of the additional enrollees are expected to be children.
Individual states are already seeing large increases in Medicaid applications or enrollment, even though Medicaid applications typically lag behind applications for unemployment benefits (which started surging in mid-March). Arizona, Hawaii, Nevada, Ohio, Utah, and Washington have reported spikes in applications or enrollment in late March or early April.[4]
A large body of research finds that most people who enroll in Medicaid, even when the economy is stronger, would otherwise have been uninsured.[5] This is likely even more true during a deep recession, when fewer people have coverage available through an employer.
While Medicare is the primary source of acute care coverage for seniors, Medicaid still covers many of those at greatest risk from COVID-19. As of 2019, it provided health coverage to about 10 million adults aged 50 to 64, and it covers millions of younger people with underlying health conditions that increase their risk from COVID-19.
Medicaid also covers Medicare premiums and cost sharing, nursing home care, and/or home- and community-based services (HCBS), such as home health aides and personal care assistants, for millions of seniors. HCBS are especially important during the current public health crisis since they help seniors and people with disabilities remain in their homes, where they are generally safer from the virus than in nursing homes. But providing these services is also unusually challenging under current circumstances, with health care workers struggling to keep themselves, their clients, and their families safe.[6]
Many state Medicaid programs are proposing or implementing new policies to respond to COVID-19 and maintain access to physical and behavioral health care during the public health crisis. While some of these policies are low cost, others are expensive to implement. States are:[7]
- Expanding or strengthening HCBS for seniors and people with disabilities, for example by temporarily expanding services and supplies such as home-delivered meals and adaptive technology (19 states); expanding settings where HCBS may be provided, such as hotels, schools, churches, and temporary shelters (34 states); increasing payment rates (19 states); providing retainer payments to help keep HCBS providers from reducing services (30 states); waiving service limits and prior authorizations (27 states); and paying family caregivers (25 states).
- Making it easier to enroll in coverage during the public health crisis, for example by accepting self-attestation for all eligibility criteria (11 states); allowing people living temporarily out of state due to the public health emergency to retain state residency (8 states); adopting a simplified/streamlined application (3 states); and expanding presumptive eligibility (which lets providers and other qualified entities temporarily enroll people who appear eligible for Medicaid) to seniors and people with disabilities (5 states).
- Making coverage and care more affordable, for example by eliminating copayments and other cost-sharing charges (14 states) as well as premiums (13 states).
- Making it easier for people to get their prescription drugs, for example by allowing early refills (34 states); increasing the maximum supply or quantity limit of certain drugs (34 states); and making changes to preferred drug lists (12 states).
- Allowing beneficiaries to skip unnecessary trips to the doctor, for example by suspending (42 states) or extending (36 states) prior authorizations for health care services and items through the end of the public health emergency.
- Expanding telehealth capacity for physical and behavioral health care, for example by conducting virtual HCBS evaluations and person-centered planning meetings (35 states); paying some telehealth services at the same rate as face-to-face visits (39 states); waiving or reducing copayments for telehealth services (20 states); and giving providers more flexibility to provide telehealth services (all states, including the District of Columbia).
- Expanding or strengthening their health workforce, for example by increasing payment rates and supplemental payments to certain providers (11 states); making it easier for out-of-state providers to enroll in their Medicaid programs (48 states); and allowing providers to offer health care services in alternative settings, including unlicensed facilities (40 states).
Without additional, longer-lasting federal assistance, many states will likely cut Medicaid or shortchange needed investments to respond to COVID-19, leading people to lose coverage or access to critical services during the public health and economic crises.
Forecasters now project that the current downturn will be deeper than the Great Recession, and the labor market will likely take several years to recover. CBO, for example, projects that unemployment will reach 16 percent in the third quarter of this year, average 10 percent in 2021, and remain at 9.5 percent at the end of 2021.[8] Goldman Sachs projects that the unemployment rate will reach 15 percent later this year and remain elevated into 2022.[9]
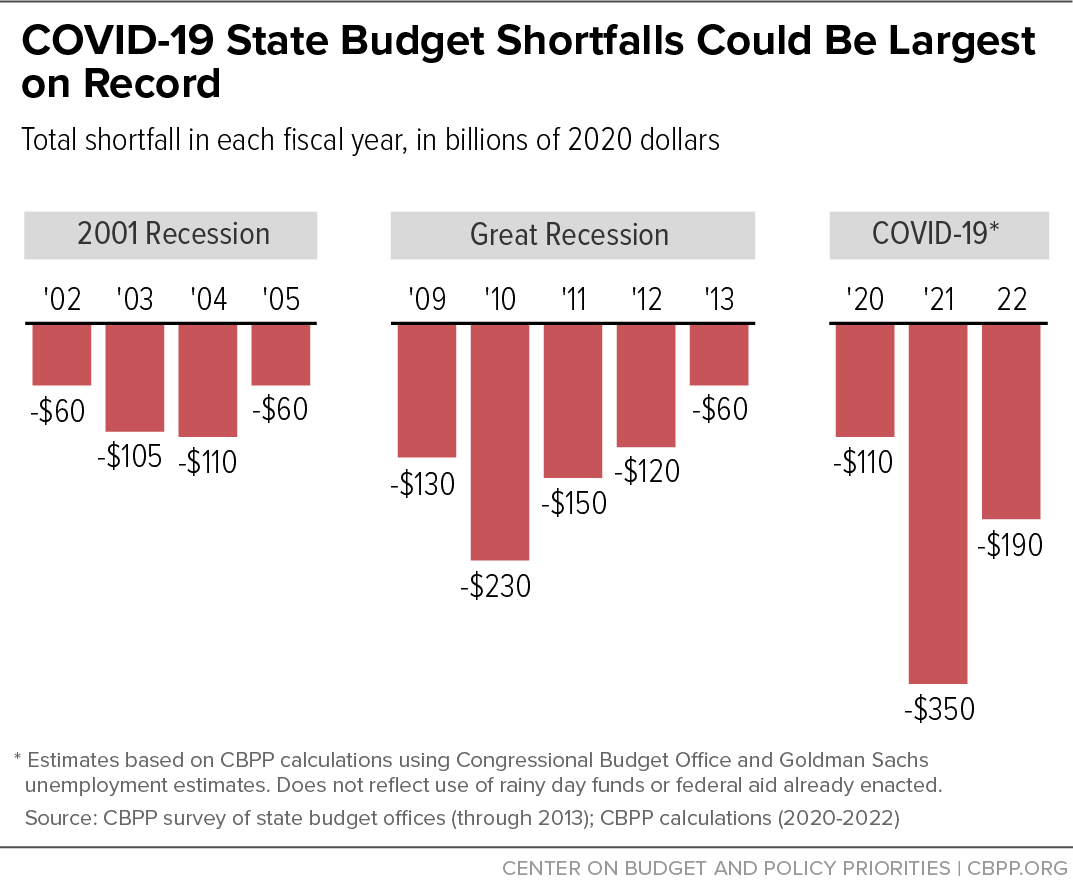
A downturn this severe will create massive budget challenges for states. Based on the historical relationship between unemployment and state revenues and safety net program costs, a 1-percentage-point increase in the national unemployment rate corresponds to a roughly $45 billion deterioration in state budgets.[10] That means states would expect to see shortfalls of about $650 billion through state fiscal year 2022, based on the CBO and Goldman Sachs forecasts — a budget crisis even worse than they faced during the Great Recession and much worse than following the 2001 recession.[11] (See Figure 1.)
Moreover, these estimates are based on the relationship between unemployment and state budgets during prior recessions. They do not include the additional costs states will incur to respond to COVID-19, and they may understate the drop in sales tax revenues states will see in this recession due to social distancing.
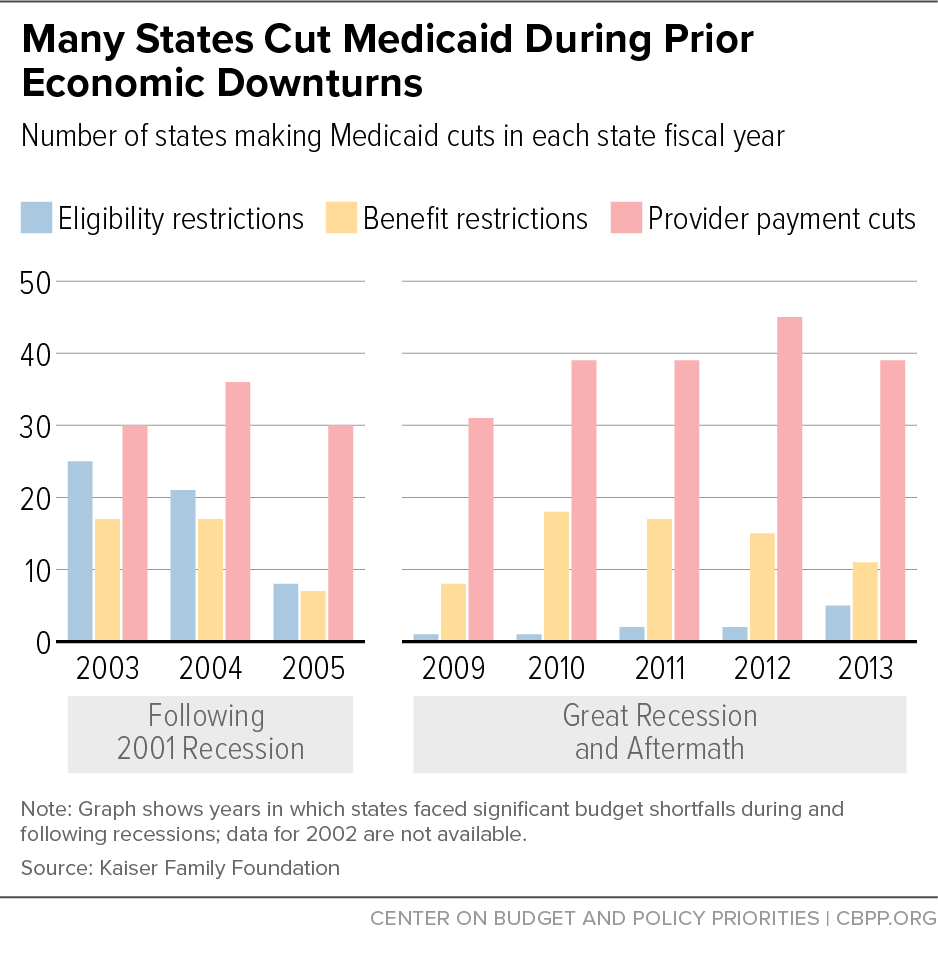
During past downturns, states have responded to shortfalls in part through harmful Medicaid cuts. Even states that usually are strongly committed to maintaining and expanding health coverage have cut Medicaid when they faced severe budget pressures. Notably, however, states made many fewer Medicaid eligibility cuts during the Great Recession than in the much smaller 2001 downturn, largely due to timely, significant FMAP increases that included MOE protections. (See Figure 2.)[12]
Following the 2001 downturn, the federal government did not provide additional Medicaid funding or other state fiscal relief until almost two years into the state budget crunch; even then, the assistance was modest. As Figure 1 shows, state budget shortfalls in the early 2000s were far smaller than those now projected for the next few years. Still, states made significant Medicaid cuts, including:[13]
- Eliminating coverage for “optional” enrollees states were not required to cover under federal law. For example, Colorado and Texas restricted eligibility for pregnant women; Connecticut, Kansas, Kentucky, Massachusetts, Missouri, Nebraska, New Jersey, North Carolina, North Dakota, South Carolina, and Texas restricted eligibility for parents; Florida, Kentucky, Louisiana, Massachusetts, North Dakota, Oklahoma, Oregon, and Wisconsin restricted eligibility for seniors and people with disabilities; and Alabama, Alaska, Colorado, Florida, Maryland, Montana, Tennessee, and Utah restricted eligibility for children covered through Medicaid or the Children’s Health Insurance Program (CHIP).[14]
- Imposing additional premiums and cost sharing. For example, Arkansas, Kentucky, Maryland, Massachusetts, Oregon, Rhode Island, Texas, Vermont, and Wisconsin imposed or increased premiums for adults or children covered through Medicaid or CHIP. Many states also imposed new or higher copayments. Extensive research has shown that premiums significantly reduce low-income people’s participation in health coverage, while cost sharing deters use of needed care.[15]
- Making it harder for eligible people to get or stay covered. For example, Arizona, California, Connecticut, Indiana, Nebraska, Texas, and Washington shifted from reassessing eligibility for either adults or children every 12 months to every six months. The Centers for Medicare & Medicaid Services later concluded that with more frequent redeterminations, “many eligible beneficiaries lose coverage at renewal for procedural reasons, only to reapply and to regain eligibility, soon after losing coverage.”[16]
- Dropping coverage for “optional” benefits they were not required to cover under federal law. For example, 16 states eliminated or restricted dental coverage for adults; states also eliminated or restricted vision coverage and made cuts to HCBS.[17]
- Cutting payments to providers. Nearly all states cut or froze Medicaid payment rates for at least some providers: physicians, hospitals, and/or nursing homes.
While the Great Recession led to much deeper state budget shortfalls than the 2001 recession, few states made cuts to eligibility levels — the direct result of additional federal Medicaid funding and the beneficiary protections that came with it. The 2009 Recovery Act increased state FMAPs by about 10 percentage points, on average, from October 1, 2008 through December 31, 2010 (with a peak increase of 11 percentage points), and relief was subsequently extended through June 30, 2011. The accompanying MOE protections prevented states from introducing more restrictive eligibility requirements.
Without the additional funds, “[most states] could not have continued to support the substantial Medicaid enrollment growth they have experienced,” the Government Accountability Office (GAO) found, adding that the funds “were integral to maintaining current eligibility levels, benefits, and services and to avoiding further program reductions.”[18] Similarly, Kaiser Family Foundation researchers found that Recovery Act funding and MOE protections largely prevented states from adopting the types of eligibility restrictions they introduced during the previous downturn and mitigated other cuts.[19] For example, 36 states said the additional federal funding helped them avoid or limit benefit cuts for fiscal year 2009 (and 37 states for 2010), while 38 states said it helped them avoid or limit cuts to provider payments for 2009 (35 states for 2010).[20] And a study by the American Association of Retired Persons (AARP) concluded that the Recovery Act FMAP increase helped protect HCBS from cuts in many states, although growth in HCBS still slowed during the state budget crisis, according to the Kaiser study.[21]
But the additional Medicaid funding, coupled with other state assistance, fell well short of filling state budget gaps, and, as Figure 2 shows, states still adopted cuts that the MOE allowed.[22] Many states, for example, eliminated or reduced coverage for “optional” benefits or services, such as adult dental coverage. States also cut costs by making it harder for people to enroll, such as by laying off or freezing hiring of eligibility workers, which led to backlogs as the number of people urgently needing coverage rose. And the large majority of states froze or cut provider reimbursement rates.
Large budget shortfalls are already emerging and beginning to drive budget decisions in many states.[23] A number of governors have instructed state agencies to plan for large, across-the-board cuts, including Medicaid cuts. States have also imposed broad hiring freezes, which could lead to delays in processing applications for Medicaid and other needed assistance.[24]
The Families First FMAP provision gives Medicaid some protection from budget cuts by modestly reducing the state cost of each dollar of Medicaid spending and (through its MOE protections) preventing states from introducing new eligibility restrictions or terminating people’s coverage while the higher FMAP is in place. But without more federal help, states will likely address their budget shortfalls by making it harder for eligible people to enroll, eliminating or restricting optional Medicaid services, or cutting provider payments.
Some of these cuts may be especially problematic for responding to COVID-19:
- Cuts to eligibility staff, call centers, or offices that create application backlogs and delay access to coverage could delay testing and treatment for COVID-19, impeding efforts to monitor the spread of the virus and quarantine those infected.
- HCBS will likely be a particular target for cuts since they are the largest category of optional services in Medicaid. As noted above, seniors and people with disabilities are particularly vulnerable to COVID-19 and are likely safer in their homes than in nursing homes. Cuts to HCBS could force some into nursing homes and leave others without needed care.
- Cuts to Medicaid provider payment rates could compound the financial challenges already facing physicians, hospitals, behavioral health providers, home health workers, and others.[25]
Meanwhile, if the Families First FMAP increase, and with it the MOE protections, end as scheduled at the end of the public health emergency — with unemployment still elevated and state budgets still in crisis — then states would likely also cut eligibility, as they did in the early 2000s.
The next COVID-19 response legislation should include additional, longer-lasting FMAP increases, which are needed to protect coverage even if Congress also provides other forms of state fiscal relief, as it should.
The Families First FMAP increase will provide states with about $40 billion in funding for each full year it is in effect, and the CARES Act provided only about $30 billion in flexible funding to help states offset declining revenues and increased demand for Medicaid and other safety net programs.[26] The CARES Act provided another $110 billion to states, but subsequent guidance from Treasury barred states from using the funds to cover their revenue shortfalls. For comparison, states face about $650 billion in projected shortfalls through the end of their 2022 fiscal year, as discussed above.
The Families First FMAP increase is inadequate in several respects:
- It is too small. The 6.2 percentage-point increase has only a modest impact on states’ cost per dollar of Medicaid spending, and thus only a modest impact on their incentives to maintain Medicaid. During the Great Recession, Congress ultimately increased the average state FMAP by almost twice as much.
- It is slated to end too soon, at the end of the quarter in which the Secretary of Health and Human Services declares the end of the official public health emergency. While the COVID-19 public health crisis seems likely to persist for some time, the economic crisis — and with it, the state budget crisis — will likely last longer, with forecasters projecting high unemployment through 2021 and beyond. If the FMAP increase ends prematurely, the MOE protections will end with it, and so if states still face large budget shortfalls, they will likely cut Medicaid eligibility.
- It does not apply to ACA expansion enrollees. This omission is problematic, because states that expanded Medicaid will offer coverage to far more newly unemployed or newly poor adults than non-expansion states, and so they will likely experience much greater enrollment growth. From 2014 to 2018, Medicaid covered about 36 percent of unemployed adults in expansion states, compared to just 16 percent in non-expansion states.[27] In addition, expansion covers millions of older adults and people with underlying health conditions, and so expansion states will likely also incur greater COVID-19 treatment costs. While the federal government covers 90 percent of expansion costs, enrollment growth and COVID-19 treatment costs will still increase state expenditures.
Policymakers should adopt additional FMAP increases that: (1) continue until the economy has truly recovered; (2) automatically scale up or down based on the extent of the downturn; and (3) apply to people covered through Medicaid expansion — principles endorsed by the bipartisan National Governors Association. (See box.) Equally important, additional FMAP increases should continue strong MOE protections along the lines of those in Families First, which are critical to preventing Medicaid eligibility cuts.[28]
The Take Responsibility for Workers and Families Act (H.R. 6379) includes an FMAP proposal that meets these criteria. Specifically, a state’s FMAP — including for expansion enrollees — would increase by 4.8 percentage points for each 1 percentage point of excess unemployment relative to a threshold based on the state’s past unemployment rates.[29] This policy would be permanent law, and so a state would continue to receive additional federal funding until its unemployment rate returned to normal; states would also receive additional funding in future downturns. The bill’s MOE protections would prevent states from adopting new eligibility restrictions and require them to provide enrollees with 12 months of continuous coverage during downturns.
If Congress adopted this policy, it would automatically cover about two-thirds of the state budget shortfalls that result from the downturn. If the downturn proved deeper or longer than expected, states would get more help; if it proved shallower or shorter, they’d get less. This design would also automatically give more help to states hit especially hard by the recession, whether because their economies are especially dependent on affected industries or because they implement longer or more extensive social distancing to keep their residents safe.
The federal government could also deliver state aid that’s responsive to economic conditions through a grant program. But it should deliver at least a significant portion of state aid through the FMAP in order to protect health coverage. Unlike other forms of state fiscal relief, FMAP increases:
- Protect coverage by reducing states’ costs per dollar of Medicaid spending. That is especially important to protect HCBS and other optional benefits, which are likely targets for cuts, as discussed above.
- Protect coverage through MOE requirements, which prevent states from cutting eligibility.
- Incentivize Medicaid investments to respond to the crisis. By lowering state costs, additional FMAP increases would encourage more states to use Medicaid flexibilities to provide needed services, support health providers, and make it easier to enroll in coverage during the public health crisis.
- Automatically adjust based on states’ costs. Unlike other forms of state aid, FMAP increases (even without triggers linked to unemployment rates) will provide more funding if a deeper-than-expected recession causes more people to enroll in Medicaid or if states incur higher-than-expected treatment costs related to COVID-19.