BEYOND THE NUMBERS
For the third straight year, states that have expanded their Medicaid programs as part of health reform expect their state Medicaid spending to grow more slowly than states that haven’t expanded, a new Kaiser Family Foundation survey finds. It also finds that expansion has produced savings in many states and that covering new enrollees has cost less than expected.

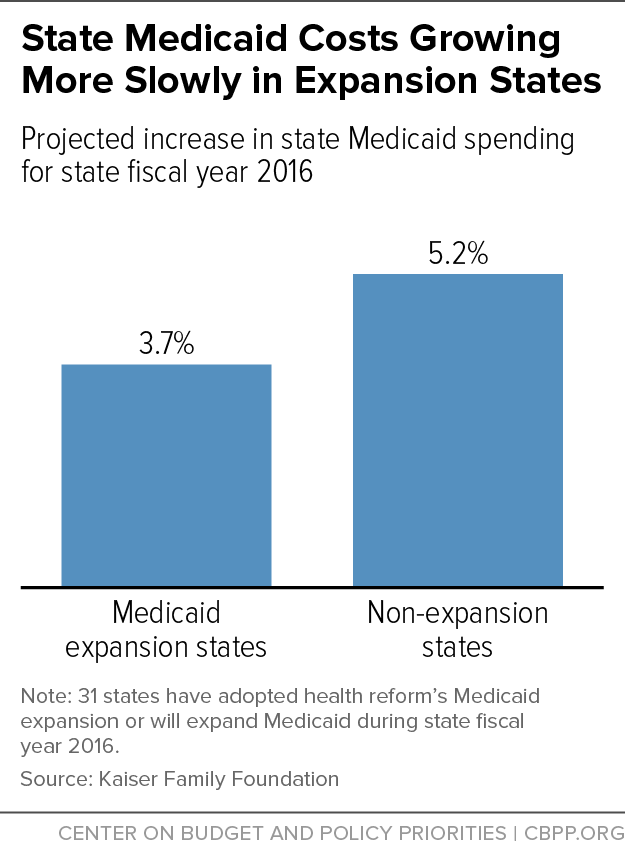
The 31 states (including the District of Columbia) that have expanded Medicaid or will expand it this state fiscal year (2016) expect their Medicaid spending to grow by 3.7 percent this year, compared to 5.2 percent for non-expansion states (see chart).
Expansion states have had lower spending growth, even as millions of people have gained coverage, for two reasons. First, the federal government is covering the entire cost of the expansion through 2016 (and at least 90 percent thereafter). Second, expansion states have moved beneficiaries who had received limited services through targeted Medicaid programs that were financed at the regular federal matching rate into the new expansion eligibility group, with its more generous federal match.
In addition to savings within state Medicaid budgets, expansion has produced other state savings as well as higher revenues, as we’ve shown. The Kaiser report provides further evidence, noting that expansion has allowed some states to reduce state-only spending on uncompensated care, behavioral health programs, and corrections-related health care. Some states also collected more revenue through existing taxes on health providers and health plans because more people have health coverage.
As a result, expansion has produced net budgetary savings in many states.
Most expansion states also report that the expansion’s per-enrollee cost has been lower than expected — contrary to critics’ claims that state costs will skyrocket when states start contributing a modest share of the cost of this expansion in 2017.