State and federal policymakers have tried for several decades to make it easier for people to demonstrate their Medicaid eligibility by streamlining enrollment processes and limiting unnecessary requests for documents to verify eligibility. Kentucky's new Medicaid waiver and the extension of Indiana's current waiver mark a sharp reversal of these efforts: both erect multiple new barriers that can trip up eligible but unaware enrollees and lead them to lose coverage or even not apply in the first place if they think they aren't eligible. The waivers will likely significantly increase the number of people who experience gaps in health coverage or lose it altogether despite being eligible.[1]
Efforts to streamline the eligibility process reflect an understanding that burdensome paperwork requirements often keep eligible people from enrolling or staying enrolled, and that there are ways to eliminate these barriers while still ensuring that only eligible people get covered.[2] Strategies are grounded in state experience reducing enrollment "churn," when eligible people go on and off Medicaid or lose eligibility altogether at the time of coverage renewal, when they move, when their incomes and family circumstances change, or for other reasons.
Churn has a number of adverse effects. It leads to higher use of the emergency room, including for conditions like asthma and diabetes that can be managed in an outpatient setting when people have consistent access to treatment.[3] That's not surprising because low-income families have trouble paying for medication and other services out of pocket when they don't have coverage. Gaps in coverage make it less likely that people establish relationships with health care providers, which also can undermine the quality of care they receive.[4]
Churn also increases administrative costs, both for state Medicaid agencies and for managed care organizations (MCOs), which pass these cost increases on to state and federal governments. Churn also makes it much harder for MCOs to effectively manage and coordinate care and harder for states to measure the quality of care Medicaid beneficiaries receive, because quality measures generally require enrollment in at least 11 of 12 months of the measurement period.[5]
Kentucky's new Medicaid waiver and the extension of Indiana's current waiver will both disenroll people from coverage for non-compliance with multiple program rules or new work requirements, locking them out for up to six months. In Indiana, large numbers of beneficiaries have already lost coverage when they didn't pay the premiums required under the waiver, and more will lose coverage due to the revised waiver's new work requirement and penalty for not renewing coverage on time.[6] The cumulative impact of these "lockouts" in both states — and in others that may receive similar waivers — will be to reduce the number of months many beneficiaries stay continuously enrolled. Many more enrollees will cycle on and off coverage and others will likely lose coverage altogether, with serious adverse consequences for access to care and health outcomes.
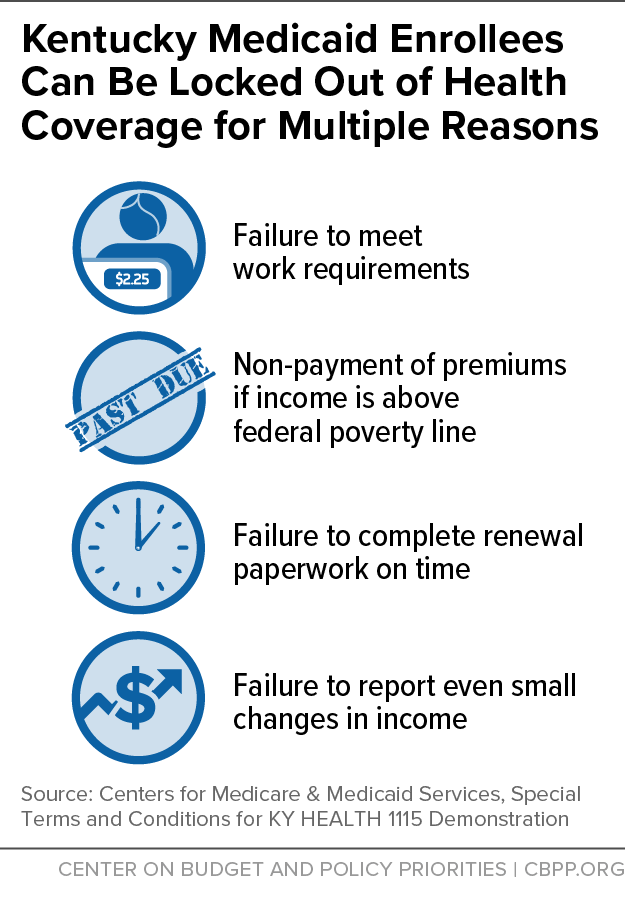
Kentucky and Indiana Waivers Lock People Out of Coverage for Multiple Reasons
Hundreds of thousands of Medicaid beneficiaries in Indiana and Kentucky will soon be at risk of getting "locked out" of coverage, if they:
- Don't work or engage in work-related activities. In Kentucky, most adults who aren't pregnant, primary caretakers of a dependent child, or full-time students will have to work or engage in other specified activities for at least 80 hours a month starting in July 2018, unless they are deemed "medically frail" or can provide medical documentation showing they are unable to work. Beneficiaries who don't comply in any month are suspended unless they make up the hours they were short or participate in a health or financial literacy course the following month. The suspension lasts until the month following a month in which the beneficiary works 80 hours, shows good cause for not complying or that he or she is exempt from the requirement, or completes a health or financial literacy course.[7]
Indiana's requirement, which starts in 2019, requires five to 20 hours per week of work or work-related activities depending on how long a beneficiary has been enrolled in Medicaid. Indiana will review compliance for all beneficiaries each December, and beneficiaries who haven't met the requirements for eight of 12 months will have their eligibility suspended in the following calendar year. The suspension will last until the beneficiary works the appropriate number of hours for one month. If that doesn't occur by the beneficiary's next scheduled redetermination date, eligibility will be terminated.
- Don't pay monthly premiums. Beneficiaries with incomes between 100 and 138 percent of the poverty line must pay premiums in both Indiana and Kentucky.[8] If they fall 60 days behind on their premiums, they lose coverage for six months.
- Fail to submit renewal paperwork on time. Beneficiaries who don't complete their annual renewals of eligibility on time will lose coverage for six months in Kentucky and three months in Indiana. In both states, the lockout will start 90 days after the date coverage is terminated for not renewing on time. During the 90-day period beneficiaries can re-enroll, but it's not clear whether coverage would be retroactive to the date of termination.
- Fail to report changes in income, employment, or work-related activities. Beneficiaries in Kentucky who don't report changes affecting their eligibility will lose coverage for up to six months.
The decision to allow states to require Medicaid beneficiaries to work or engage in work-related activities at the risk of losing their coverage has received most of the attention around approval of the Indiana and Kentucky waivers, and that attention is well founded, because many people will likely lose coverage because they don't meet the paperwork requirements necessary for compliance or can't show they are exempt.[9] But other provisions will add to the impact and increase the risk of losing coverage for all beneficiaries in Kentucky and Indiana. While parents of minor children, students, and some people with disabilities are exempt from work requirements, most of these beneficiaries aren't exempt from the other requirements that could cause them to lose coverage.
Kentucky's and Indiana's programs are operating under waiver authority in Section 1115 of the Social Security Act, which allows states to request approval from the Department of Health and Human Services (HHS) to implement demonstration projects that are "likely to assist in promoting the objectives of [Medicaid]." To carry out these projects, states may waive certain provisions of the Social Security Act, but such waivers are only allowed to the extent necessary to implement the demonstration project and test new or experimental policies.[10] As Medicaid's core mission is to provide comprehensive health coverage to low-income people so they can get the health care services they need,[11] changes that cause large numbers of people to lose coverage and experience harm from being uninsured are not a proper use of waiver authority.
The Centers for Medicare & Medicaid Services (CMS) approved both states' waivers despite the likelihood that they will cause such harm. Kentucky's waiver will cause a 15 percent drop in adult Medicaid enrollment by its fifth year, according to the state's own projections.
Moreover, the changes Kentucky and Indiana are making under the guise of experimentation — including making participation in work or work-related activities a requirement for Medicaid eligibility — are based on false hypotheses. CMS has attempted to justify Medicaid work requirements by citing research showing that people with jobs have better health and higher incomes than people without jobs. But that research doesn't show whether employment causes improved health or rather, as is likely for many people, the causal relationship is in the other direction — namely, that healthy people are likelier to have jobs than those in poor health.[12]
In its Indiana approval letter, CMS claims with no evidence that changes such as paying premiums and renewing coverage on time will "increase the likelihood that beneficiaries will transition to commercial health insurance since the demonstration seeks to provide members the tools to successfully utilize commercial market health insurance." CMS provided a similar rationale for allowing Kentucky to lock people out of coverage for not reporting changes that affect their eligibility.
Most people already comply with program rules, and whether they transition to commercial coverage has nothing to do with their on-time renewal of Medicaid, but with their income and the availability of employer coverage in their jobs. Moreover, people with employer coverage don't have to report income changes to their insurer and renewal of coverage is often automatic unless an employee wants to make a change. Kentucky's and Indiana's changes won't increase the number of people with employer coverage but will make it more likely that many eligible people who rely on Medicaid will become uninsured due to unnecessary and burdensome paperwork.[13] As one Kentuckian put it, "Part of it feels like they're trying to catch you, by burying people in paperwork and making it a huge inconvenience."[14]
Medicaid and Children's Health Insurance Program premiums reduce coverage for both children and adults by deterring enrollment, increasing disenrollment, and shortening people's time on the program, several decades of research show. The impact is greatest on people with incomes below the poverty line, who are also likelier to remain uninsured if they lose public coverage.[15]
An evaluation conducted for Indiana of its first three-year waiver confirms that research, showing that 55 percent of people eligible to make a premium payment during their enrollment didn't do so. The large majority of these individuals had incomes below the poverty line, which means they were moved to less comprehensive coverage when they failed to pay. But nearly 60,000 individuals with incomes above the poverty line were either disenrolled from coverage because they didn't pay their premiums or never enrolled because they didn't make their first payment.[16] Beneficiaries, providers, and advocates didn't understand that the lockout for non-payment applied only to people with incomes above the poverty line, according to focus group research. One participant said, "You have to sit out for six months and pray you don't get sick for six months."[17]
Premiums, and the complexity of the waiver provisions, may also be deterring people from even applying. A former chef living in Indianapolis who is now homeless said, "I haven't signed up for my Medicaid because it's so confusing, and because I don't have a way to pay for it." Because he didn't sign up, he has been unable to get treatment for high blood pressure, insomnia, and the flu.[18]
Despite the research and Indiana's own evaluation, both Kentucky and Indiana will charge premiums and lock beneficiaries with incomes above the poverty line out of coverage for six months if they fail to pay. Both states will also delay coverage for new enrollees until they pay their premiums: those with incomes above the poverty line will never be enrolled if they don't pay, while those with incomes below the poverty line will be enrolled in a plan with co-payments after 60 days. The lockouts for those with incomes above the poverty line who fail to pay and the delays in coverage for all beneficiaries will leave many people with gaps in coverage.
About 60 percent of Medicaid beneficiaries affected by these waivers are already working.[19] Many low-wage workers don't have an offer of affordable employer coverage, and Medicaid is their sole option for health coverage. Large shares of those who aren't working are ill, have a disability, or are caring for a child or other family members. Most of these beneficiaries already renew their coverage on time and report changes in their income that would make them ineligible for coverage. Threatening to cut off their health for not reporting changes or renewing coverage won't make it more likely that they "transition to commercial health insurance," as CMS claims.
However, some people do miss the renewal deadline. In rejecting an earlier Indiana proposal to lock people out for failing to renew their coverage, CMS recognized that many low-income individuals face challenges in completing the renewal process such as language access and problems getting mail. CMS also found that mental illness or homelessness can make completing the renewal process difficult and that coverage gaps could cause harm. For these and other reasons, CMS previously found that penalizing people for not completing their renewals didn't promote Medicaid's objectives.[20]
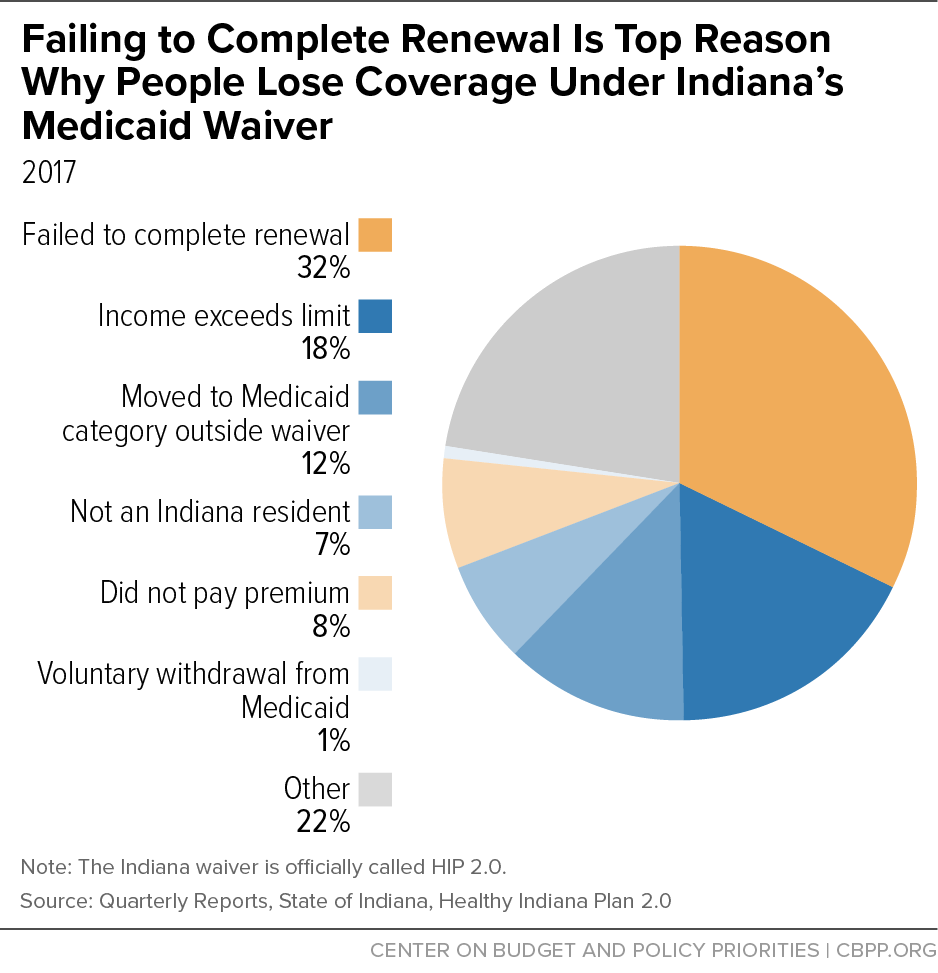
The number of people likely to lose coverage due to this provision, while a small share of the total number of beneficiaries, is significant when the consequences of losing coverage are considered. Moreover, those who lose coverage are likely to be especially vulnerable, as CMS' earlier denial of Indiana's proposal noted. Quarterly reports on Indiana's waiver show that failing to complete the renewal process is the most frequent reason for case closures. Over the last four quarters (from November 1, 2016 through October 31, 2017) an average of about 13,000 cases were closed for this reason each quarter, although some of these beneficiaries may have had their eligibility reinstated within 90 days of the date of termination.[21] (See Figure 1.)
The risks to continuous coverage will be even greater in Kentucky, because the state also plans to lock people out of coverage for up to six months for failing to report changes in circumstances that affect eligibility, defined as failures that "led to additional month(s) of Medicaid eligibility during which the member was not otherwise eligible."[22]
Medicaid beneficiaries in all states must report changes in circumstances that affect their eligibility, but Kentucky is the first state allowed to cut people off for six months for failing to report such changes.[23] The complexity and multiple new requirements in Kentucky's waiver mean that enrollees will need to have a detailed understanding of the new rules to know when to report changes to avoid losing coverage. (See Figure 2.) Moreover, reporting changes may be difficult for some enrollees. Among non-elderly adult Medicaid enrollees in Kentucky, 19 percent lack any access to the Internet, and 42 percent don't have broadband access, recent research shows.[24]
Prior to the approval of Kentucky's waiver, eligibility for adults depended primarily on their income and household size and continued residence in the state. Beneficiaries only had to know that they should report changes if their income changed enough to put them over the 138-percent-of-poverty eligibility level, if they moved out of Kentucky, or if they gained or lost a family member through marriage, birth, or other circumstances.
Under the waiver, beneficiaries must understand the complex rules regarding work, including exemptions, hours of work, and requirements to pay premiums, because all these factors can affect eligibility for one or more months. For example, consider the requirement to pay premiums. Beneficiaries with incomes below the poverty line can forgo paying a premium and enroll in a plan with co-payments, but those with incomes above the poverty line must pay premiums to stay enrolled. A beneficiary earning $990 a month in the co-payment plan whose income rose to just $1,010, putting her above the poverty line, would have to pay a premium. If she didn't know the impact of this minor change and failed to report it — which wouldn't be surprising as her income would remain well below 138 percent of the poverty line — she could lose her coverage for six months.
Others would be at similar risk. For example, a low-income parent who works part time could lose her exemption from the work requirement if her child moves out of the home. Despite remaining eligible based on her income, she could be locked out of coverage for up to six months if she delayed reporting her child's move, as she would be failing to report that she was now subject to the work requirement. The same could be true for people no longer caring for family members with disabilities.
Many Medicaid beneficiaries' monthly income fluctuates from month to month. If a beneficiary gets extra shifts, for example, his income may rise over the income eligibility level for one month. Failing to report that change could lead to ineligibility for six months. Similarly, beneficiaries could be at risk for failing to report changes in work hours. Beneficiaries who work 120 hours a month are deemed to satisfy the work requirement without reporting their hours, while those who work less than that are subject to monthly reporting. Presumably, failing to report a change in hours that makes them subject to monthly reporting — even if they are working 80 hours a month — could put them at risk of losing coverage for six months.
Medicaid waivers should implement demonstration projects that are experimental in nature and promote Medicaid's objective of providing coverage to low-income and vulnerable people who wouldn't otherwise have a pathway to coverage and care. Waivers should not limit participation or purport to test policies already shown to limit coverage and access to care or those certain to do so. In approving waivers that experiment with low-income people's health coverage, CMS should uphold the Hippocratic oath and "do no harm." Unfortunately, Kentucky's and Indiana's waivers fail that test.