Taking Away Medicaid for Not Meeting Work Requirements Harms People Experiencing Homelessness
Medicaid expansion under the Affordable Care Act (ACA) significantly increased health coverage for people experiencing homelessness, a group whose mortality rates are several times higher than the general population. Before the ACA, most adults experiencing homelessness did not qualify for Medicaid unless they could prove they qualified for coverage based on a disability, were pregnant, or over 65. People experiencing homelessness are more likely to have a disability than the general population but have a harder time proving it, in part because lack of access to health care can mean they have limited medical evidence of their conditions. But under the ACA, adults in expansion states with incomes up to 138 percent of the poverty line can enroll regardless of disability. This means coverage is now available for far more people experiencing homelessness, giving them access to both routine and urgently needed health care.
Now, however, the Trump Administration is allowing states to take away Medicaid coverage from people who don’t document that they work a specified number of hours each month. Homelessness can cause health problems, worsen existing conditions, and make it harder for people to engage in care, so the consequences of losing Medicaid coverage are especially severe.
The Administration is allowing states to impose work requirements on adult Medicaid enrollees other than those who are 65 or older, pregnant, or qualify for Medicaid because they receive disability benefits through the Supplemental Security Income program. In Arkansas, the first state to implement such a policy, over 18,000 Medicaid beneficiaries lost coverage in 2018 due to the new requirements. While a federal court has since halted Arkansas’ policy, the Administration is continuing to approve similar policies in other states. Most of these policies require enrollees to document that they work or engage in other work activities (e.g., job training or volunteer work) for at least 80 hours per month, unless they prove that they qualify for limited exemptions.
People Experiencing Homelessness Face Significant Obstacles to Work
While data vary, a survey of officials in 25 cities found that as few as 18 percent of adults experiencing homelessness were employed. People experiencing homelessness face significant barriers to work, including physical and behavioral health conditions, lack of work experience or inconsistent work history, and histories of incarceration.
Homelessness itself is also a barrier to employment. Limited access to showers and washing machines makes it difficult to meet personal hygiene requirements and dress codes. People who sleep outdoors or in a shelter often endure chronic sleep deprivation and stress related to lack of a safe, comfortable place to rest. Shelter hours are not always flexible, sometimes forcing people to choose between getting in line in the afternoon for a bed or working during the day. Workers in evening or night shifts might have to forgo sleeping in a bed because shelters aren’t open during the day or are too noisy for sleep. People experiencing homelessness also often lack reliable mailing addresses or access to a phone, computer needed to apply for jobs, or transportation to work. Even those who do manage to work, including those in unstable jobs that may not provide enough hours each month to meet a work requirement, are still at risk of losing coverage.
Many Experiencing Homelessness Will Lose Coverage Despite Exemptions
The Administration’s policy does not require — or even encourage — states to exempt people experiencing homelessness from work requirements. And while over 40 percent of adults living in a shelter have a disability, the Administration’s “medically frail” exemption is narrow and will leave out many with significant physical or behavioral health conditions.
The Administration has approved work requirements that provide no exemptions for people experiencing homelessness, such as in Ohio and South Carolina. Some other states included exemptions that would fall far short of protecting all vulnerable people from losing coverage. For instance, Wisconsin plans to exempt people experiencing “chronic homelessness,” which typically refers to homelessness that lasts for at least a year or occurs at least four times in the last three years, but the vast majority of people living in shelters stay for six months or less.
Regardless of how exemptions are defined, those who qualify may have trouble proving they do. Red tape and paperwork requirements have been shown to reduce enrollment in Medicaid across the board and could prove even more challenging for people experiencing homelessness, for many of the same reasons that they struggle to find and maintain employment. For example, people lacking a reliable address will likely miss important notices from the state explaining exemptions and paperwork requirements. These barriers are even greater for the 1 in 4 adults experiencing homelessness who also have a serious mental illness.
Losing Coverage Will Worsen Health Outcomes
As noted, people experiencing homelessness have higher rates of many physical and behavioral health conditions than the general population, and homelessness can make it harder to treat those conditions. For people with such serious health needs, coverage interruptions can lead to increased use of emergency departments, admission to hospitals and mental health facilities, and higher health care costs, research shows.
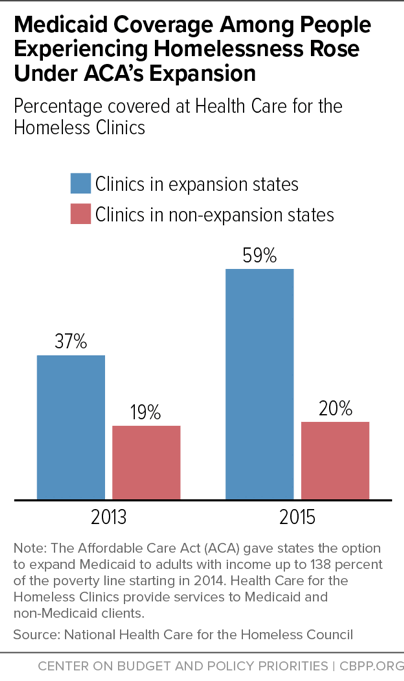
Medicaid expansion increased access to health care for people experiencing homelessness, including primary care, mental health services, substance use treatment, supported employment, and transportation to medical appointments. After expansion took effect, Health Care for the Homeless clinics (which provide primary care and substance use treatment to people experiencing or at risk of homelessness) saw large gains in Medicaid coverage among patients in expansion states, while clinics in non-expansion states did not (see chart). Losing Medicaid coverage threatens crucial supports that can help avoid poor outcomes for people experiencing homelessness. That’s why groups like the National Alliance to End Homelessness (in partnership with Families USA) and the National Health Care for the Homeless Council oppose Medicaid work requirements.
Losing Coverage Will Exacerbate Homelessness
People experiencing homelessness, especially those with chronic physical or behavioral health conditions, often need services to help find a home and remain housed. Health services through Medicaid — including behavioral health case management and housing support services — can meet this need. For example, behavioral health case management models such as Assertive Community Treatment teams can connect people to key housing and other community resources that help them gain housing and address their physical and behavioral health care needs. Medicaid can also pay for supportive housing services, which help people with histories of homelessness or institutionalization maintain housing. Communities are increasingly using Medicaid services in integrated housing and health programs that work to improve housing stability and health outcomes and lower health care costs for people who frequently use expensive emergency services. Losing Medicaid coverage will reduce access to these key supports, worsening homelessness and the health problems that come with it.
Medicaid can also play a key role in preventing homelessness, which often results from unforeseen medical expenses. States that expanded Medicaid saw sharp reductions in evictions after expansion took effect, compared to states that did not. Conversely, work requirements — rather than leading to better financial and health outcomes, as the Administration argues — may set off a vicious cycle where loss of Medicaid coverage leads to other harmful outcomes, such as homelessness.