The Medicare Part D Low-Income Drug Subsidy (LIS), Medicare Savings Programs (MSPs), and Food Stamps[1] can play important roles in improving the health and well-being of low-income seniors and people with disabilities. Together, these programs can provide several thousand dollars a year in benefits and can significantly increase a low-income Medicare beneficiary’s ability to make ends meet.
Unfortunately, all three programs suffer from very low participation rates among Medicare beneficiaries who are low-income, but not so poor that they qualify for Supplemental Security Income (SSI) and Medicaid. Many low-income Medicare beneficiaries do not know that they can qualify and receive substantial benefits from these programs. For others, the complexity of the eligibility rules and difficulties in enrolling, the differences between program requirements, or the stigma associated with seeking help all serve as barriers.[2]
The Medicare Improvements for Patients and Providers Act (MIPPA[3]), which was enacted in July 2008, included provisions that can help low-income seniors who apply for the LIS connect with the state MSP programs, under which Medicaid pays for Medicare premiums and, for some beneficiaries, Medicare deductibles and copayments. Beginning in January 2010:
- The Social Security Administration (SSA) will begin forwarding, electronically, information from LIS eligibility determinations to state agencies; and
- State agencies will treat the LIS application as an MSP application, as though the applicant had initiated an application directly with the state agency.
This process will help to ensure that low-income seniors who apply for the LIS will have an opportunity to receive MSP benefits as well. The process also presents an outstanding opportunity to enroll eligible seniors for food stamps. Many of the elderly Medicare beneficiaries whose applications will be forwarded to the states also are eligible for food stamps. The benefits of the three programs can be packaged, and can amount to a significant benefit for low-income seniors.
Over the next several months state agencies will be putting in place the procedures for following up, as necessary, with Medicare LIS applicants to determine their eligibility for MSP. With minimal additional effort on the part of both state agencies and low-income Medicare beneficiaries, these individuals and their families can also find out if they are eligible to sign up for food stamps.
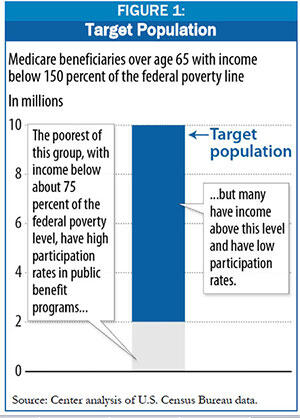
According to the Census Bureau, about one in four Medicare beneficiaries (about 10 million individuals) is over age 65 and has income below 150 percent of the federal poverty line.[4] The poorest of this group, those with income below about 75 percent of the federal poverty level and limited assets, generally can qualify for Supplemental Security Income (SSI) and in most states, Medicaid. But a large share, about three-quarters (8 million individuals), have income above this level, but still below 150 percent of the federal poverty line. (See figure 1.) Many of these seniors will not qualify for Medicaid but still may have significant difficulty affording their basic needs, such as housing and utilities, groceries, medications, and other out-of-pocket medical costs.
USDA finds that one in five low-income households with seniors report “food insecurity,” which means that members of the household “do not have consistent access to enough food for active, healthy lives for all household members during the year.” Similarly, Feeding America, (the food bank network previously known as America’s Second Harvest) reports that one in five adults who pick up food at a food pantry are over age 65, and about half of these seniors have income between 75 percent of poverty and 150 percent of poverty.[5] Yet low-income seniors often do not participate in the public benefit programs that are available to help them meet their basic needs.
The three programs — LIS, MSP, and food stamps — all are designed to provide benefits to low-income seniors to help them maintain overall health and avoid hardship. While the overlap in eligibility rules is not perfect, many low-income Medicare beneficiaries who qualify for one of these programs will qualify for all three. Below are descriptions of the three programs and their eligibility rules. For more detailed information, see Table 1 at the end.
- Medicare Savings Programs (MSPs) — State-operated programs, under which Medicaid pays the Part B premium ($96.40 a month in 2009) for Medicare beneficiaries with income up to 135 percent of the federal poverty line. Beneficiaries with income up to 100 percent of poverty also have no cost-sharing obligations for Medicare Part A or Part B.[6] Assets cannot exceed $4,000 for single individuals and $6,000 for couples. These asset limits will be raised to match the LIS asset limits on January 1, 2010. In addition, states have flexibility to increase both income and asset limits in their MSPs. While Medicaid also pays these costs for fully dual-eligible individuals (i.e., those that qualify for the state’s full Medicaid program), MSP generally refers to those who are below the specified income thresholds but do not qualify for full Medicaid. MSP costs are shared by states and the federal government.[7]
- Part D Low-Income Subsidy (LIS) — A federally funded program that pays the Part D prescription drug plan monthly premiums and limits copayments and other out-of-pocket costs for low-income Medicare beneficiaries with income up to 135 percent of poverty and assets below $6,600 for single beneficiaries and about $9,910 for couples.[8] A partial subsidy for premiums and copayments is available for those with incomes up to 150 percent of poverty (and with somewhat higher assets.) [9] Full dual-eligible Medicaid participants, MSP participants, and SSI beneficiaries with Medicare are “deemed” eligible for the full Part D LIS subsidy, meaning they may receive prescription drug coverage with minimal out-of-pocket obligations. According to SSA, the average annual value of the Part D benefit for a Medicare beneficiary who receives the full subsidy is $3,900 in 2009.
- Food Stamps — Provides monthly benefits on a debit-like card that can be used to purchase food in grocery stores and supermarkets. For households with elderly or disabled members, eligibility is limited to households with “net” income, after the program’s deductions are taken into account, at or below poverty. (There is no limit on the gross income that a household with seniors may have. [10]) A household’s assets must be below $3,000, though about 30 states have taken advantage of state flexibility to lift the asset test.[11] As discussed below, households with substantial medical or housing expenses can qualify for higher benefits. USDA estimates that more than 4 million Social Security recipients are eligible for food stamps but do not receive them. By contrast, USDA estimates that virtually all food stamp eligible seniors who receive SSI participate. The federal government funds all of the benefit costs. Administrative costs are shared with the states. The state agency that administers eligibility for food stamps is almost always the same agency that determines eligibility for MSPs.
Very low-income elderly — those with annual incomes below about 75 percent of the poverty line (which is $7,060 for an individual and $8,898 for a couple in 2009) — are fairly well connected to the safety net; they are generally eligible for cash assistance under the Supplemental Security Income Program (SSI), on its own or in combination with their Social Security check, and health coverage under Medicaid. The majority of these very low-income individuals do participate in food stamps and in the LIS and MSP.
But low-income elderly with incomes above this level — including many such people who live below the poverty line — generally do not qualify for SSI or full Medicaid, and although they are eligible for LIS, MSP, and food stamps, they are very often not enrolled.
- MSPs — Although the Medicare Savings Programs have existed for more than 20 years, researchers find that only about 33 percent of eligible QMBs (those with income below poverty) and about 13 percent of eligible SLMBs (those with income between 101 percent and 120 percent of poverty) have signed up for the benefits.[12]
- LIS — According to data from the Centers for Medicare and Medicaid Services, only about 40 percent of low-income Medicare beneficiaries who qualify for the Part D Low-Income Subsidy and are not automatically enrolled because of their participation in Medicaid or SSI receive the subsidy.[13]
- Food stamps — According to USDA estimates, food stamps serves only about 32 percent of eligible households with elderly members. [14]
Low-income Social Security and Medicare beneficiaries who are not receiving SSI or Medicaid are the very people who apply for the LIS benefit through SSA and whose applications will be forwarded to states for MSP eligibility.
Under the new MIPPA provision, beginning in January 2010 the Social Security Administration (SSA) will send electronic files to states each weekday with information on the LIS applicants for whom an eligibility determination has been made. (As part of the LIS application the applicant may ask SSA not to share the application with states.) If current trends continue, according to SSA data, they will forward an average of about 60,000 to 70,000 applications a month to the states. (See Appendix A, which shows for each state the number of LIS decisions SSA has made over a recent nine month period.[15]).
The electronic file from SSA will contain information from the LIS application, including the name, address, social security number, and phone number of the applicant (and his or her spouse, if any) and income and asset information from the LIS application process. (See Appendix B for a sample version of the revised LIS application).
Under the new law, states will treat the LIS application as an application for MSP benefits.[16] Most states will need to develop procedures for completing the application process. This would likely include contacting the applicant either by mail or telephone to gather any additional information that is needed to make an MSP eligibility determination. [17] The process and the types of information that will be needed will differ by state. States may want to amend their MSP eligibility rules and procedures to minimize the burden of this follow-up on state agency staff and applicants. For example, some states require a face-to-face interview for MSP eligibility. States could substitute a telephone interview, or conduct no interview if the application received from SSA is complete for MSP purposes. Also, some states require additional paper documentation from applicants to establish MSP eligibility. These requirements could be simplified or eliminated.
As part of this follow-up process states also can screen for food stamp eligibility and sign up eligible seniors. This can be done by sending a separate food stamp application to the household or integrating the necessary food stamp eligibility questions into the MSP application. Similarly, if states are contacting the households over the telephone, they could initiate a food stamp application that way. [18] In most states the population of low-income seniors who will be eligible for food stamps will be a subset of the LIS population.[19]
The major instances where additional information may be needed to determine food stamp eligibility include:
- Household composition. States will need information on other household members, if any, who purchase and prepare meals with the Medicare beneficiary (and spouse). Approximately two-thirds of low-income Medicare beneficiaries live alone or with only a spouse, but about one-third live with other individuals, who very likely would need to be included in the food stamp unit.
- Information on deductible expenses. As discussed in more detail below, the amount of food stamp benefits for which a Medicare beneficiary can qualify will depend on the household income and the amount of shelter, out-of-pocket medical, and dependent care expenses. Households with high expenses in these areas can qualify for higher food stamp benefits. The information could be collected on an application or by telephone, and states have wide latitude on what documentation is required. If a household has applied for food stamps but not provided this information its application proceeds without the benefit of the deductions.
- Differences in income and asset rules. Depending upon how states have set their MSP eligibility rules, food stamp rules may require states count slightly different types of income and assets. For the most part these types of income and assets are uncommon and should not pose a significant barrier to coordinating with MSP procedures for most households. For example, beginning in January 2010 LIS will no longer count in-kind support and maintenance (i.e., support from a family member or church) as income, but some states may count it in MSP, and food stamps may or may not count it depending on the circumstances. In addition, food stamps may require more recent household income information, and verification is likely to be required for some types of income, particularly any earnings. (For many types of unearned income, however, states can verify through data matches.)
In addition, there are likely to be some procedural differences, notably:
- States will need a food stamp application with name, address, and signature to establish a filing date. The application could be the same as any materials that are mailed to gather MSP or LIS information, or could be a separate form.
- Food stamps requires an interview, though the interview can (and in many cases would normally) be conducted over the telephone, rather than face-to-face.
Under federal law, Social Security Administration (SSA) offices are required to inform Social Security and SSI applicants and recipients of the availability of the Food Stamp Program and provide an application that can be forwarded to states. (7 U.S.C. 2020(j)) The law provides federal reimbursement to SSA for carrying out these responsibilities. According to USDA budget documents, SSA is expected to receive about $11 million this year.
States and advocates may also wish to engage SSA as a partner in packaging together the various low-income benefit programs. Many seniors have a high regard for the Social Security Administration and some may be more receptive to information that the SSA provides compared to a state human services agency.
For many low-income Medicare beneficiaries, Social Security benefits bring them close to or modestly above the poverty line. When such households do not have high expenses — for example, because they live in public housing and have no out-of-pocket medical costs — the food stamp benefit for which they qualify can be relatively low, perhaps only $16 a month.
If, however, such a household has high shelter expenses (including property taxes and utilities), out-of-pocket medical expenses, or dependent care expenses, its monthly food stamp benefit will be significantly higher. The typical Social Security recipient who does not receive SSI but does participate in food stamps qualifies for about $80 a month in benefits in 2009. (See box below.) A typical household with members who are elderly or disabled and with very high deductions can receive closer to $150 a month or more in food stamps. Outreach messages may be more useful if they explain that households with high expenses will qualify for larger food stamp benefits.
Research has found a variety of reasons that seniors are not enrolled in benefits for which they qualify. A primary reason is lack of knowledge about 1) the existence of the benefits, 2) the eligibility rules, and 3) the amount of benefits that are available. In addition, the complicated and uncoordinated application rules and processes can be daunting for low-income seniors to navigate, and result in a situation where individuals who apply for one benefit will not necessarily receive all benefits for which they qualify.
Consider the estimated benefits in 2009 for a typical Social Security recipient who lives alone. Using food stamp administrative data for such households that do participate in food stamps, the median income for such a household is about $800 a month (or about $10,000 a year).
Typical food stamp benefit: $80 a month, $960 a year[20]
MSP Part B premium value: $96.40 a month, $1,157 a year
LIS average value: $3,900 a year
For this single elderly individual, an $80 monthly food stamp benefit would raise monthly income by almost 10 percent. [21] Food stamp benefits can only be spent on food, but the availability of this resource can free up other income that the senior may have to meet other basic needs.
In addition, such a household very likely would also qualify for MSP, which would raise the household’s income by a minimum of another $96.40 a month for just the payment of the Part B premium. (The household would also no longer have any out-of-pocket deductible or co-insurance costs for Medicare Part A or Part B.) Finally, SSA estimates that the average value of the LIS is $3,900 a year.
Thus, when the typical food stamp benefit is considered along with the benefits of the LIS and MSP the total package can increase a low-income senior’s income by 50 percent or more.
Studies of effective efforts to enroll seniors in the Food Stamp Program and other public benefit programs have found that the most effective strategies include personal assistance from a trusted source, for example, one-on-one counseling and application assistance from a local organization. [22] Efforts to eliminate eligibility barriers, such as asset tests, simplifying application rules, and reducing documentation requirements have also been successful.
While other measures help and should be incorporated into a unified enrollment process, providing comprehensive application assistance is one of the most effective strategies for increasing enrollment among seniors.[23] This kind of intensive enrollment assistance can be expensive, limiting its availability. Still many organizations provide one-on-one application assistance for various programs, such as food banks that help people apply for food stamp benefits and senior centers that help their clients get enrolled in Part D or LIS. In addition, federal grants support State Health Insurance Programs (SHIPs), which provide free counseling and assistance to people with Medicare and their families. It may be possible and cost-effective for these organizations to assist low-income seniors to enroll in multiple benefit programs. Individuals who feel that just one benefit is not worth the trouble of going through the process might be more willing to engage if they understand that one process, mediated by a trusted individual, can help them to obtain a valuable package of benefits. This personal assistance reaches more individuals for each benefit program, as the people seeking food will get help with medical expenses and those at the senior center will also get food assistance.
While this kind of coordinated enrollment assistance and outreach effort may be more cost effective than having separate enrollment assistance for each program, it does require a commitment from all players. Many organizations feel that they do not understand the programs well enough to offer assistance. Outreach workers in these organizations will need training and support as they become proficient in new programs with different rules. Aligning other aspects of program administration, such as documentation and interview requirements, can help enrollment assistance efforts to be expanded more quickly and successfully.
The new LIS/MSP data sharing presents a unique opportunity to couple states’ efforts with the application assistance efforts of community partners to reach low income elderly people with the benefits they need to live a healthy life.
In addition to the new opportunity that will begin in January 2010, states can use existing information about participation in MSP, LIS, food stamps, and other programs to assess how well they are doing in ensuring that beneficiaries participate in all the programs for which they qualify. Administrative data matches can help states and local organizations target their outreach efforts.
For example, states may create a list of Medicare beneficiaries who participate in LIS and/or MSP and conduct targeted outreach for food stamps. The reverse is true as well: some food stamp participants may also qualify for MSP or LIS and not currently be enrolled.
In 2008 New York City identified families who participated in the state’s Medicaid program who appeared eligible for food stamps but did not participate. They mailed letters to these households explaining that they may be eligible for food stamps, accompanied by a brochure explaining the program and providing information on the application process. The City concluded that the effort resulted in 51,000 new food stamp participants.
Low-income Medicare beneficiaries can qualify for substantial benefits through three important programs: the Low-Income Drug Subsidy, the Medicare Savings Programs, and the Food Stamp Program. The three programs have very similar eligibility rules, but all suffer from low participation rates among low-income seniors who are not connected to other benefits like SSI and Medicaid, despite the fact that such benefits can significantly reduce hardship and improve health among low-income seniors.
SSA and state Medicaid agencies will launch a new process beginning in January 2010, when SSA begins forwarding LIS applications to states for MSP eligibility determinations. State agencies can increase the value of this effort by connecting seniors to the full range of public benefits for which they qualify. Because food stamp benefits are funded by the federal government and are, in almost every state, administered by the same agency (indeed, often by the same state worker) as MSP, it would be highly efficient to use the new process as a tool for signing up eligible Medicare beneficiaries for food stamps.
|
Table 1:
Comparison of MSP, LIS, and Food Stamps
|
| |
Medicare Savings Programs |
Medicare part D Low Income Subsidy |
Food Stamps |
|
Eligibility rules
|
|
|
|
|
Income
|
QMB: <100% poverty, covers all Medicare premiums and cost-sharing
SLMB: 101-120% poverty, covers just Part B premiums
QI: 121-135% poverty, covers just Part B premiums
States have flexibility to adjust countable income.
|
Full Dual Medicaid/ Medicare participants: Deemed elig.
MSP: Deemed eligible
Other full subsidy: <135% pov.
Other partial subsidy: under 150% poverty
All beneficiaries face some out of pocket costs, which increase as income increases.
|
No gross income limit for households with elderly or disabled members, but net income (after deductions) must be below 100% poverty.
|
|
Asset Limits
|
All categories:
$4,000 indiv./$6,000 couple
MIPPA raises the MSP asset limits to match the full LIS levels beginning in Jan. 2010.
States have flexibility to increase or waive asset test.
|
Full Dual Medicaid/ Medicare participants: Deemed eligible for full subsidy
MSP: Deemed eligible for full subsidy.
Other full subsidy 2009: $6,600/$9,910
Other partial subsidy 2009: $11,010/$22,010
(Burial expenses up to $1,500/$3,000 do not count)
|
$3,000
State flexibility to lift asset test, which about 30 states have done.
|
|
Typical Annual Benefits[24]
|
QMB: Medicare premiums and cost-sharing (In 2009: $1,157 annual Part B premium; $1,068 hospital deductible; $133.50/day copay for SNF services; 20% co-insurance on most Part B services; $5,000+ in Part A premiums when required)
SLMB and QI: Medicare Part B premiums only, $1,157 in 2009
|
Full subsidy:
No premium, no deductible, Copays limited, No copay after $4,050 out of pocket.
Partial subsidy: sliding scale premium and lower copays.
Average = $3,900 for full LIS. (SSA 2009 estimate)
|
In 2009 the average benefit of current recipients in households with elderly or disabled members is about $80 to $100 a month, or about $1,000 a year. Many with high shelter or medical costs receive higher benefits. Those without high expenses may receive the minimum benefit of $16 a month, or about $200 a year.
|
|
Agencies Determining Eligibility
|
State Medicaid Office
|
SSA (though State Medicaid Offices also authorized.)
|
State Local Welfare Office (usually the same as State Medicaid Office)
|
|
Funding
|
Shared federal/state based on Federal Medical Assistance Percentages (FMAP), except QIs which are 100% federally funded, but overall funding and state allotments are capped.
|
100% federally-funded
|
Benefits 100% federal,
50% match admin.
|
|
Estimated participation rate
|
33% QMB
13% SLMB
|
About 40% of those not automatically enrolled (i.e. non-dual eligibles).
|
Seniors 32%, but SSI seniors very high, so non-SSI seniors even lower.
|
|
Appendix A:
SSA Completed Decisions by State
Date from October 2008 to June 26, 2009
|
| |
Decisions Made |
Eligible |
Not Eligible |
Approximate Total Monthly Applicants Forwarded to States |
| National Total |
568,654 |
312,071 |
256,583 |
63,184 |
| Alabama |
12,402 |
7,560 |
4,842 |
1,378 |
| Alaska |
521 |
289 |
232 |
58 |
| Arizona |
8,105 |
4,369 |
3,736 |
901 |
| Arkansas |
7,913 |
4,804 |
3,109 |
879 |
| California |
49,881 |
25,251 |
24,630 |
5,542 |
| Colorado |
6,248 |
3,841 |
2,408 |
694 |
| Connecticut |
4,959 |
2,125 |
2,834 |
551 |
| DC |
791 |
484 |
307 |
88 |
| Delaware |
2,872 |
786 |
2,086 |
319 |
| Florida |
40,326 |
22,492 |
17,834 |
4,481 |
| Georgia |
20,881 |
12,074 |
8,807 |
2,320 |
| Hawaii |
1,890 |
1,114 |
776 |
210 |
| Idaho |
2,249 |
1,239 |
1,010 |
250 |
| Illinois |
28,678 |
10,231 |
18,447 |
3,186 |
| Indiana |
12,946 |
6,953 |
5,993 |
1,438 |
| Iowa |
4,025 |
1,946 |
2,079 |
447 |
| Kansas |
4,588 |
2,522 |
2,066 |
510 |
| Kentucky |
11,900 |
7,078 |
4,822 |
1,322 |
| Louisiana |
9,253 |
5,175 |
4,078 |
1,028 |
| Maine |
1,623 |
807 |
816 |
180 |
| Maryland |
8,536 |
4,914 |
3,622 |
948 |
| Massachusetts |
10,812 |
4,788 |
6,024 |
1,201 |
| Michigan |
18,448 |
10,316 |
8,132 |
2,050 |
| Minnesota |
5,813 |
3,073 |
2,740 |
646 |
| Mississippi |
8,246 |
4,650 |
3,596 |
916 |
| Missouri |
12,231 |
6,821 |
5,410 |
1,359 |
| Montana |
2,416 |
1,242 |
1,174 |
268 |
| Nebraska |
2,662 |
1,283 |
1,379 |
296 |
| Nevada |
3,962 |
2,443 |
1,519 |
440 |
| New Hampshire |
2,329 |
1,259 |
1,070 |
259 |
| New Jersey |
11,255 |
6,334 |
4,921 |
1,251 |
| New Mexico |
3,954 |
2,322 |
1,632 |
439 |
| New York |
39,145 |
21,484 |
17,661 |
4,349 |
| North Carolina |
21,889 |
12,384 |
9,505 |
2,432 |
| North Dakota |
1,307 |
648 |
659 |
145 |
| Ohio |
19,460 |
10,806 |
8,654 |
2,162 |
| Oklahoma |
6,970 |
4,159 |
2,811 |
774 |
| Oregon |
5,304 |
2,967 |
2,337 |
589 |
| Pennsylvania |
29,262 |
17,706 |
11,556 |
3,251 |
| Rhode Island |
2,361 |
1,272 |
1,089 |
262 |
| South Carolina |
12,180 |
7,110 |
5,070 |
1,353 |
| South Dakota |
1,049 |
543 |
506 |
117 |
| Tennessee |
15,227 |
8,415 |
6,812 |
1,692 |
| Texas |
48,285 |
30,342 |
17,943 |
5,365 |
| Utah |
2,490 |
1,400 |
1,090 |
277 |
| Vermont |
1,031 |
519 |
512 |
115 |
| Virginia |
13,772 |
7,858 |
5,864 |
1,525 |
| Washington |
8,447 |
4,849 |
3,598 |
939 |
| West Virginia |
5,567 |
3,302 |
2,265 |
619 |
| Wisconsin |
6,230 |
3,399 |
2,831 |
692 |
| Wyoming |
726 |
381 |
345 |
81 |
| No Zip Available |
5,286 |
1,942 |
3,344 |
587 |
| Source: Social Security Administration |