In recent years, a number of states have increased cost-sharing for low-income Medicaid beneficiaries as one approach to Medicaid cost-containment. While copayments have been most commonly applied to prescription drugs, they also have been assessed for other services, such as physician visits, hospital admission, or outpatient clinic use.
Prior research has found that when low-income patients are required to pay more for health care services or for prescription drugs, they use fewer services or medications.[2] In some cases, their health could deteriorate, with the result that they may subsequently require more expensive emergency room or inpatient hospital care. While private insurance often requires copayments, the low-income patients covered by Medicaid are more likely to experience adverse consequences from copayments because they have a more difficult time affording higher copayments for medications or doctor visits. Low-income patients are also more likely to have fragile health.
This paper presents findings from an analysis of data about changes in the use of medical services and prescription drugs that occurred after “nominal” copayments were instituted in Utah’s Medicaid program in the 2001-2002 period, based on data collected by the Utah Department of Health (UDOH). [3] Our analyses take advantage of the natural experiment that occurred after copayments were imposed on Medicaid beneficiaries. We conclude that:
- $220 copayments for inpatient hospital care reduced hospital admissions;
- $2 copayments for physician services led Medicaid patients to see doctors less often, and increasing copayments to $3 caused further reductions;
- $2 copayments for prescription drugs reduced patients’ use of prescription drugs; and
- $2 or $3 copayments for outpatient hospital clinic visits lowered the number of such visits.
Some of our conclusions conflict with those reached by state officials. A UDOH report concluded that Medicaid beneficiaries in that state did not use less health care after copayments were imposed.[4] This finding has been cited as evidence that copayments do not adverse affect Medicaid beneficiaries. Our review indicates that portions of the state’s analyses were technically flawed. This paper presents revised analyses that reassess the impact of the copayments in Utah.
Our reanalysis finds that the copayments decreased health care utilization for Utah’s Medicaid beneficiaries. Such a finding is more consistent with other information from Utah, as well as being more consistent with prior research. For example, UDOH also reported findings from a survey of Medicaid enrollees in which one-ninth of enrollees reported not seeing a doctor because they could not afford the physician copayments. When Utah submitted its application for a Section 1115 waiver that authorized increased copayments for parents, the state assumed that copayments would reduce health care use and expenditures and that these savings would finance other parts of the state’s waiver project. [5]
An underlying goal of Utah’s Medicaid waiver was to foster use of preventive and primary care in the hope that this would reduce the need for hospitalization. Our analysis suggests that the Medicaid copayments interfered with the use of physician services and medications. While hospitalization rates fell, it appears that this occurred because patients could not afford the copayments. There is no evidence that hospitalizations fell because patients received more primary or preventive care.
UDOH’s survey of beneficiaries’ experiences with nominal copayments provides other useful insights into the effect of cost-sharing on low-income Medicaid beneficiaries. While some did not have problems with the copayments, many others did. Some 42 percent of those surveyed responded that, “[The copayments for doctor visits and prescription drugs] seem small, but are actually a huge problem,” and 39 percent reported “They cause serious financial difficulties for me.”
While $2 or $3 copayments may seem modest, they can create barriers to the use of health services for a number of low-income patients. This analysis does not examine whether the reduction in health care utilization affects the use of “essential” health services or harms patients’ health, but prior studies have found that copayments reduce the use of “essential” as well as “less essential” services and that the use of fewer essential services contributes to subsequent health problems or to higher medical expenses if patients become sicker and require more intensive medical care. [6]
In 2001 and 2002, the state of Utah began imposing copayments in its Medicaid program for low-income parents, as well as for low-income senior citizens and people with disabilities. The state subsequently increased copayments for certain groups. [7] Before this time, Utah did not require copayments. (Under federal Medicaid law, copayments cannot generally be assessed for children, pregnant women and those in institutions, such as nursing homes.)
The copayments were imposed upon very poor beneficiaries. In Utah the maximum income eligibility limit for parents in Medicaid is about 54 percent of the poverty line ($8,500 for a family of three). For seniors and people with disabilities, the income limit is $6,800 for a single person and $10,200 for a couple.
- Beginning in July 2002, low-income parents were required to pay a $2 copayment for prescription drugs under the state’s waiver program.
- In November 2001, Medicaid began charging $2 copayments for physician visits by parents, seniors and people with disabilities. Pregnant women were exempt. In February 2003, the copayment was raised to $3.
- In November 2001, the state began charging $2 copayments for outpatient hospital visits by parents, seniors and people with disabilities. In July 2002, this was increased to $3 for parents.
- In February 2002, the state imposed a $220 coinsurance payment for each inpatient hospitalization.
Projected savings from some of these copayments were used to help finance Utah’s Primary Care Network waiver. At the request of the state legislature, UDOH conducted a study of the effect of these policy changes, and a report was released in December 2003. The study used time-series analyses of changes in the number of fee-for-service Medicaid claims from January 2001 through mid-2003 to assess changes in service use, a survey of Medicaid enrollees affected by cost-sharing (324 people responded out of 600 surveys mailed) and several focus groups. The UDOH study was the most comprehensive analysis of some of the effects of Medicaid copayments in Medicaid that we have seen a state agency conduct.
UDOH reported the results of five time-series analyses that used econometric models to examine trends in health care use before and after the copayments were instituted.[8] Two of the five analyses found that significant reductions in utilization occurred after copayments were imposed:
- The $2 copayments for drugs led to a statistically significant reduction in the level of medication use by low-income parents, as measured by the number of fee-for-service claims. The findings of this analysis indicate that the copayments reduced prescription drug utilization by about 8 percent.
- The $2 copayments for outpatient hospital care led to a significant reduction in outpatient visits for low-income senior citizens and people with disabilities.
UDOH’s survey of Medicaid beneficiaries provided corroborating evidence for these findings: for example, 13 percent said they did not get a prescription because they could not afford the copayment.
But UDOH found no statistically significant effects of copayments in three of its analyses, one for physician visits, one for inpatient hospital use and another for outpatient hospital use among low-income parents. On the basis of these findings, the state concluded that in “most cases,” copayments did not significantly affect utilization.[9]
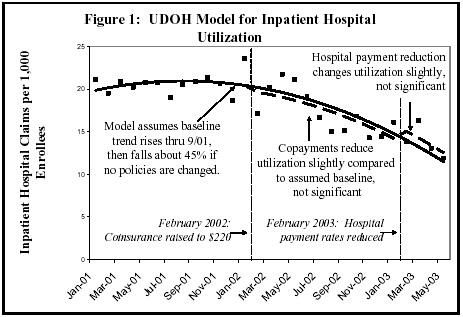
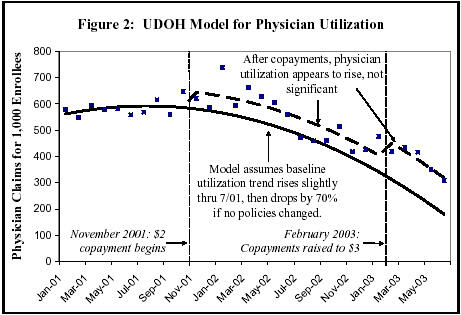
Our review finds, however, that these analyses were based on models with significant technical flaws. Figures 1 and 2 present key components of the UDOH models for inpatient hospital utilization and physician visits. (More technical data about the UDOH models, as well as our revised analyses that are designed to address the problems in these models, are presented in the appendix to this paper.) In Figures 1 and 2, the dots represent the actual observed levels of physician or hospital claims per 1,000 patients in each month, while the solid lines show the baseline trends estimated by the models — that is, the trends the models estimate would have occurred if there had been no policy changes. The dashed lines show the estimated trends after the copayments were instituted and thus how copayments changed utilization, relative to the estimated baseline.
As Figures 1 and 2 illustrate, the models that UDOH used produce highly unusual baseline estimates. The baselines that UDOH generated estimate that, even without any copayments or other policy changes, utilization of physician and inpatient hospital services would decline a remarkable 45 percent to 70 percent between late 2001 (just before the copayments were instituted) and mid-2003. The models that UDOH employed make use of a quadratic (i.e., squared) function in generating their baseline. Use of such a function is unusual in this type of model, and it is the inclusion of a quadratic function that produces the curious estimate that, in the absence of any policy changes, utilization would fall dramatically and at an accelerating pace.
Because the reliance on a quadratic function produces this highly unusual estimate of a sharp drop in utilization, the drop in utilization that actually followed the introduction of copayments is interpreted as being almost entirely unrelated to the copayments. Because of the assumption that utilization would have fallen steeply anyway, the copayments are interpreted as having had only a minimal effect on utilization.
- Figure 1 shows that inpatient hospital utilization was rising slightly before coinsurance was imposed. Yet the model used produces the assumption that utilization would have fallen by 45 percent between August 2001 and May 2003 without any policy changes.
- Figure 2 shows that utilization for physician visits also was rising slightly before the copayments were instituted. But under the UDOH model, utilization was estimated to plummet by 70 percent between August 2001 and June 2003 without any policy changes. To give a sense of the implausible nature of these assumptions, if the assumed baseline trends are extended for a longer period, physician utilization would be expected to reach zero and then become negative by November 2003.
In a commentary on these models and the UDOH analyses that were based on them, Dr. Henry Aaron, a distinguished economist and expert in health economics at the Brookings Institution, concluded that the Utah Department of Health’s “study methodology was invalid.” Aaron wrote, “It is not legitimate to choose some particular functional form (quadratic, for example) without providing a basis for that selection. The quadratic form guarantees that a trend will eventually either rise or fall with accelerating speed. Without some external justification, this procedure is, well, unjustified; even worse, it is unjustifiable.” [10]
The UDOH report speculates that utilization might have fallen if Medicaid patients became healthier in 2002 and 2003, perhaps because new enrollees could be healthier than those already on Medicaid. But an expected reduction in utilization of this magnitude strains credulity. First, Utah’s Medicaid eligibility criteria for adults did not change in this period, so there is no reason to think their health status improved dramatically. Second, earlier research has found that newly enrolled Medicaid beneficiaries actually have higher utilization than ongoing beneficiaries because people often enroll in Medicaid when they are experiencing a bout of illness or when they need care. [11]
UDOH’s conclusion that baseline utilization was falling steeply is an artifact of the particular design of the econometric models that UDOH used. Such steep reductions in baseline utilization run counter to other contemporaneous health care utilization trends in the United States. We reviewed similar utilization data for the 2001 to 2003 period from Medicare (national data), Washington state’s Medicaid program and a large private health insurer. All these insurers experienced increasing rates of physician utilization and slightly rising or stable rates of hospital utilization during this time period.[12]
Since the UDOH models incorrectly ascribe the reduction in utilization that occurred in 2002 and 2003 to a falling baseline, the UDOH models minimize the apparent impact of the copayment increases. For example, in Figure 1, the reduction attributable to the $220 coinsurance for hospital care is minimized because baseline utilization is assumed to fall so sharply. [13] And as Figure 2 indicates, the UDOH model paradoxically indicates that copayments appear to increase utilization and cause people to see the doctor more often (although these increases are not statistically significant).[14]
The findings produced by the UDOH models also contradict other information presented by UDOH. For example, in its survey of Medicaid enrollees, 11 percent reported that they avoided making a doctor’s office visit because they could not afford the physician copayments; this is contrary to the apparent findings cited above that copayments appear to increase physician visits. (Also of note, when the state originally applied for its Section 1115 waiver, its budget assumed that there would be reductions in health care utilization and expenditures as a result of cost-sharing. These savings were assumed to help pay for other aspects of the state’s waiver proposal.)
UDOH’s analyses of utilization trends for outpatient hospital use for traditional and non-traditional beneficiaries used a similar methodological approach with a curvilinear baseline trend. One model (for traditional beneficiaries) found that copayments reduced use of outpatient clinics, while the other (for non-traditional beneficiaries) did not. Both of these models are problematic and are discussed in more depth in the appendix. The UDOH model for prescription drug utilization used a different approach. It did not use a curvilinear baseline trend and found that copayments were associated with a reduction in the use of medications; that model is more in line with accepted modeling practices for this type of analysis and yields results more consistent with other evidence and with economic theory.
In the first part of 2001, before Utah assessed copayments, inpatient hospital and physician utilization rates were rising slightly. [15] Rather than assuming that baseline utilization was going to plummet deeply, a more credible expectation is that utilization would have either have continued to rise or flattened out if copayments had not been imposed. (Technical information about these models is included in the appendix.)
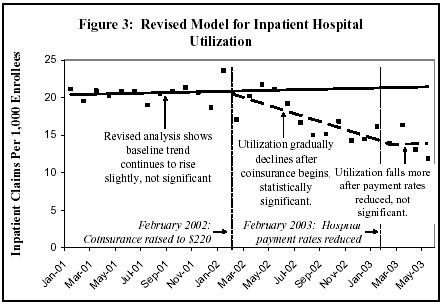
Figure 3 presents our revised analysis of trends in inpatient hospital utilization. This model uses a baseline (the solid line) that continues to rise slightly throughout the entire 2001 to mid-2003 period, although the rise is not statistically significant. Compared to this more plausible baseline, it is clear that the imposition of copayments in February 2002 (showed by the dashed line) led to a gradual reduction in the number of inpatient hospital visits. The reduction due to copayments is statistically significant. (Like the UDOH model, this analysis also examines the effect of a reduction in hospital payment rates instituted in February 2003 and finds it is not statistically significant.)
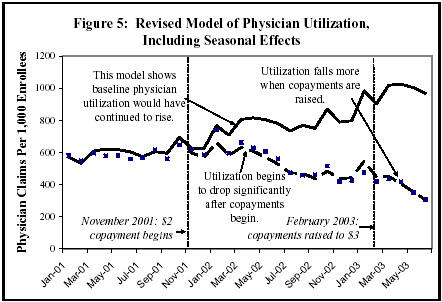
We present two alternative models of the effects of copayments on physician utilization in Figures 4 and 5. While the two alternatives differ in the levels of sophistication and assumptions about the baseline trend, both models indicate that the copayments significantly reduced the number of physician visits made by low-income Medicaid patients.
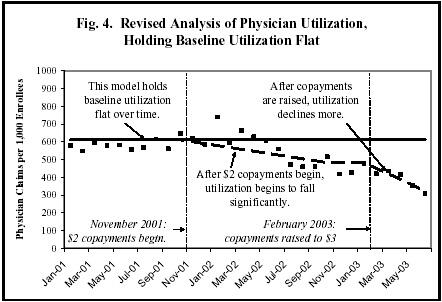
Figure 4 presents the simpler model, in which it is assumed that baseline utilization —the level of physician visits if copayments were not imposed — would have been flat throughout the 2001 to mid-2003 period. In this model, it is clear that the imposition of $2 copayments in November 2001 led to a gradual reduction in the number of physician visits and the increase of copayments to $3 led to a further reduction.
Figure 5 presents a more sophisticated model that includes seasonal trends and a lag effect. This model indicates that physician utilization would have generally increased in 2002 and 2003, although it dips upward and downward at certain seasonal points. The model shows that the $2 and $3 copayments are associated with a significant reduction in physician visits.
While the two models vary in certain assumptions about the nature of the baseline trend, each shows that the copayments led to significant reductions in physician visits.
We also examined the effect of the copayments on outpatient hospital use and found that the copayments led to reduced utilization (see appendix for more discussion). We did not reanalyze the effects of copayments on prescription drug utilization; UDOH’s model did not include a quadratic term for the baseline and was in line with accepted approaches.
Copayments in Medicaid and SCHIP
Copayments have become more common in Medicaid. The Government Accountability Office (formerly known as the General Accounting Office) reported that 34 states increased cost-sharing levels in Medicaid or SCHIP between 2001 and 2003. [16]
Under federal law, copayments in Medicaid must be “nominal” and certain groups, such as children, pregnant women and those in institutions, are exempt. The Centers for Medicare and Medicaid Services have sometimes allowed states to increase copayments beyond nominal levels under Section 1115 waivers, although recent federal court rulings have found that two of these waivers violate requirements in the Medicaid statute that set forth the circumstances under which cost-sharing rules may be waived. [17]
The surveys of beneficiaries that UDOH conducted provide additional insights about how cost-sharing affects beneficiaries. While some could afford the copayments, many could not. Two-fifths (43 percent) of those surveyed agreed with the statement that, “[The copayments for doctor visits and prescription drugs] seem small, but are actually a huge problem,” and 39 percent agreed “They cause serious financial difficulties for me.” All of the Medicaid patients who were required to make copayments in Utah have incomes below the poverty line, and finding additional funds to pay for health care can be a challenge for such people. Surveys show that families living below the poverty line often experience substantial hardships, such as having difficulties paying their rent or utility bills, skipping meals and being unable to see doctors or dentists when needed. [18] The burdens of copayments tend to be the most severe for those with chronic or serious health problems, since they need more health care and therefore have to spend more for copayments. [19]
Supporters of copayments sometimes claim that copayments just create a financial incentive for patients to avoid “unnecessary” medical care, implicitly suggesting that patients continue to get “necessary” care. Studies have repeatedly shown, however, that when copayments rise, some necessary and appropriate medical care is deterred and some patients become sicker and subsequently require more intensive or costly medical care. [20] Most patients do not have the clinical understanding to differentiate reliably between more essential and less essential care and low-income patients may have sufficiently severe budgetary constraints that they sometimes cannot afford copayments for medical care that they believe are necessary.
The classic RAND health insurance experiment found that poor adults and children who are subject to cost-sharing received less in the way of “essential” care and became less healthy than those receiving free care. [21] That study also established that low-income people are more strongly harmed by cost-sharing than those with middle-class incomes. When California’s Medicaid program raised physician copayments in the 1970s, researchers found that while physician utilization fell by 6 percent, use of inpatient services climbed by 17 percent, leading to an apparent (but not statistically significant) increase in total expenditures. [22] A recent Canadian study found that when copayments for prescription drugs were imposed, low-income patients used far fewer medications, but experienced increases in emergency room use and were more likely to experience adverse consequences, such as admission to a hospital or nursing home or death. [23]
Studies of cost-sharing in the private sector have also found that cost-sharing reduces health care utilization and expenditures but may have harmful repercussions on the health of patients or lead to higher treatment costs. One recent study examined the effects of higher copayments for prescription drugs in a number of private health plans and found that higher copayments could have adverse health effects even among middle-class patients. [24] For example, there was a substantial reduction in the use of diabetes medications among diabetic patients when copayments were raised. Another study examined the use of copayments for substance abuse treatment and found that higher copayments produced savings in the initial round of treatment but increased the risk that patients relapse and receive further rounds of treatment, which drives costs up. [25]
The findings of our analyses of copayments in Utah indicate that even “nominal” copayments in the range of $2 or $3 can significantly reduce patients’ use of medical care or prescription drugs when they are applied to poor Medicaid patients. Medicaid patients may be particularly vulnerable to cost-sharing because they are both poorer and, in general, less healthy than middle-class privately-insured patients. [26] In some cases, states have considered or adopted copayments that are much larger than those used in Utah; it is reasonable to believe that the risks are greater when copayments exceed “nominal” levels.
While states have used copayments as a tool to contain Medicaid expenditures, they should be aware that these policies can have adverse consequences. States should be cautious in applying cost-sharing to beneficiaries with low incomes. In addition, states should consider how to minimize harm for those who have chronic health conditions or are in the poorest health, since the burdens of copayments fall most heavily on those who most need health care or medications.
In a commentary on the UDOH analysis and the reanalysis presented here, Dr. Henry Aaron of the Brookings Institution discussed the ways that researchers could evaluate whether copayments affect health care utilization. He concluded that the analysis conducted by the Utah Department of Health failed to meet basic criteria:
The gold standard is the randomized experiment. The only thing that differs between two groups is the experimental intervention. In this case [i.e., the case of the copayments instituted in Utah], one would have had to randomly assign Medicaid enrollees to two groups, one of which faced the new rules and one of which did not. Then, one would compare the use of services between the two groups. The difference would be the effect of the intervention. This approach was not taken and probably couldn't be taken.
A second approach is to identify two similar groups that differ only in that one is in Medicaid and one is not. Each group has a trend of usage. Each is subject (presumably) to the same influences. So the two trends should be similar. If they are not, then, by definition, the two groups are not similar. Then, the rules change for the Medicaid group. If the two trends now diverge, then the divergence could be ascribed to the new rules. This approach is problematic for a whole host of reasons, but it is often the best that can be used and the econometric literature has been vastly expanded by attempts to cope with the problems.
A third approach, which the Utah investigators used, is to take one group, determine the factors accounting for the trend in usage — all of them! — so that one can be confident that these factors accurately forecast usage. Then, if a new policy is introduced and actual usage diverges from predicted usage, one can attribute the divergence to the new policy. This approach requires that one prove conclusively that the factors that allegedly account for trends in usage actually do so. This is a very difficult standard to meet. But there are various ways to try to do so. I do not see from the materials presented any evidence that any of these methods has, in fact, been used [by UDOH].
What are these methods? First, it is not legitimate to choose some particular functional form (quadratic, for example) without providing a basis for that selection. The quadratic form guarantees that a trend will eventually either rise or fall with accelerating speed. Without some external justification, this procedure is, well, unjustified; even worse, it is unjustifiable. The fact that an actual trend falls (or, in the opposite situation, rises) less or more rapidly than an unjustified quadratic relationship proves absolutely nothing. That is [the] fundamental point [of the Center on Budget and Policy Priorities’ reanalysis]. And it is right. The fact that a quadratic equation “fits” is neither here nor there. This is not a matter of statistics, but analytical logic and common sense. What are the factors that make behavioral sense that would cause service use or enrollment to rise or to fall? Do the coefficients make sense? [27]
The UDOH analysis and our reanalysis rely on an examination of changes in trends in health care utilization before and after copayments are imposed. This approach can be called an interrupted time-series analysis, in which the “interruption” is the introduction of copayments. In principle, it would be useful to have other data that also measure other factors that might affect utilization, such as the age, health status or income of Medicaid beneficiaries, but these data were not available for this analysis.
Our analysis and UDOH’s agree on one central point: the utilization of health care services for Utah’s Medicaid beneficiaries began to drop in late 2001 and continued to drop through mid-2003. Where we disagree is in explaining what caused the reduction in utilization. The UDOH analysis suggests that this was because of underlying factors unrelated to the introduction of copayments, while our analysis indicates that there was a “structural shift” in the trends that is related to the introduction of copayments. We do not have the type of data (e.g., a randomized experiment) that allow us to prove rigorously that copayments caused the reduction in utilization, but the combination of the findings from our econometric analysis, from UDOH’s surveys of Medicaid beneficiaries and from prior research studies, plus the lack of contemporaneous reductions in health care utilization in other populations form a strong and consistent case that copayments (and not other underlying factors) led to reductions in utilization in Utah.
The results of statistical analyses are shaped by both the underlying data observations and by how the models are designed and specified. Although we analyze the same data that UDOH examined, our conclusions differ because our statistical models differ. Our review indicates that the UDOH models about physician, inpatient and outpatient hospital utilization had two major shortcomings:
- The models used by UDOH assumed that baseline utilization trends were curvilinear in nature and added a quadratic term for time to the equation (months since January 2001 squared). This resulted in a brief rise in utilization, then a steep and accelerating decline. The inclusion of a quadratic term was unjustifiable, insofar as it inherently assumes that trends will continuously accelerate downward (or upward). While it is common to see time-series models that assume that the baseline has a linear shape, is affected by seasonal trends or is affected by prior levels (i.e., that there are lag effects), it is most unusual to see a quadratic term in this type of model. As noted earlier, these model specifications estimated steep reductions in baseline utilization, so steep that utilization would have soon become negative.
- The UDOH models also assumed the effects of copayments for physician, inpatient and outpatient services are felt at once and are constant once the policies are in effect. That is, the effect in the first month is assumed to be the same as the effect in the twelfth month. The problem, however, is that most people do not go to the doctor or hospital every month, so they may not be not aware that copayments have increased when they first seek medical care. Thus, the consequences are not neither instantaneous nor constant in effect. A more plausible theory is that awareness of such copayments — and behavioral responses — gradually become stronger over time. In contrast, the effects of copayments for prescription drugs are probably more immediate, since a substantial share of prescriptions filled are treatments for chronic illnesses. Since chronic users fill their prescriptions every month, they quickly become aware of the copayments and adjust their purchasing decisions.
Our approach made two improvements to the UDOH models:
- Our revised models were specified so that the underlying baseline trends did not assume a dramatic plunge in utilization. In our inpatient and outpatient hospital utilization models, we specified models with simple linear terms. In our physician models, we specified two alternative models, one with a flat time trend and one with seasonal and lag effects.
- In our revised models, we specified the effect of inpatient hospital, physician and outpatient hospital copayments as gradually rising in the first 12 months of implementation and then stabilizing. [28] This corresponds to the concept that effects are gradually felt, as patients become increasingly aware of copayments and make behavioral adjustments over time rather than all at once.
We would have preferred data from a longer time span, including more months before copayments were required, to measure baseline trends more precisely. Since UDOH said that such data were not available, we analyzed the same data used in the UDOH report.
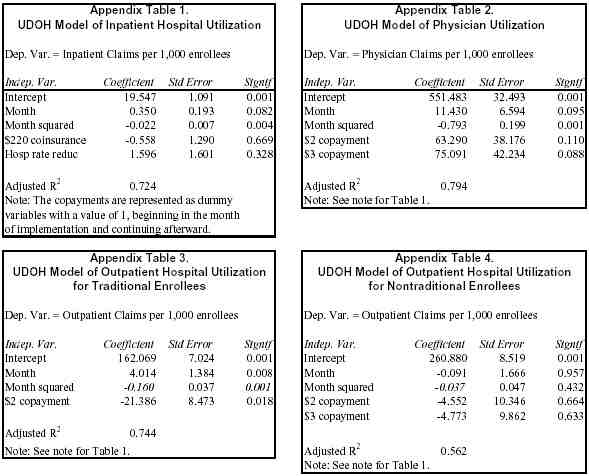
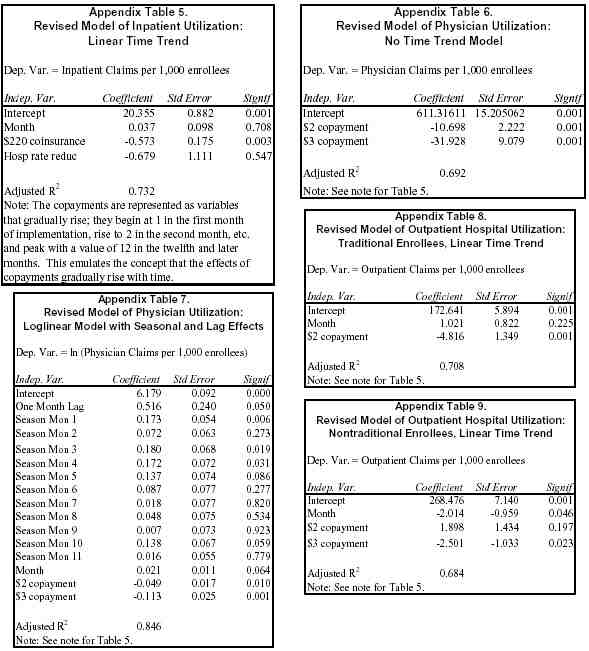
Appendix Tables 1 through 9 present the regression results for both the UDOH models and our models. To compare the models, the results are presented using regular standard errors and adjusted R2 measures. [29] The adjusted R2 measures how well each model fits the variation in the data; a higher R2 value indicates a better statistical fit. For the inpatient models, the UDOH adjusted R2 is .724, and our adjusted R2 is .732. For the physician model, the UDOH adjusted R2 is .794, while our seasonal model has an adjusted R2 of .846.
The main body of this paper compares the results of models for inpatient hospital and physician utilization. For the sake of brevity, we have kept most discussion of the outpatient hospital models to this appendix. UDOH’s model of outpatient utilization for traditional enrollees (elderly and disabled Medicaid beneficiaries) found that the $2 copayment was associated with a reduction in utilization (Appendix Table 3), as does ours (Appendix Table 8). UDOH’s model of outpatient utilization for nontraditional enrollees (low-income parents) failed to identify significant effects of $2 or $3 copayments (Appendix Table 4), but our model found that the $3 copayment significantly reduced outpatient utilization, although we did not find a significant effect for the $2 copayments. For the non-traditional enrollees, the adjusted R2 for UDOH’s model is .562, while it is .684 for our model.