Are Medicaid expenditures growing “out of control”? This paper reports new data showing that Medicaid expenditures did not grow at all in fiscal year 2006 and are expected to grow only modestly in 2007.
There are good reasons to be concerned about projected increases in Medicaid expenditures over the long term, since health care costs continue to rise throughout the U.S. health care system and the U.S. population is aging. The underlying problem, however, is not that Medicaid has unusually high or increasing costs, but that the provision of health care in the United States has become very expensive and that health care costs in the private and public sectors alike have been rising at a rapid clip and are expected to continue doing so for the indefinite future. In recent years, costs per beneficiary have actually been rising at a slower pace in Medicaid than in other health care coverage, including both private health insurance and Medicare. This analysis examines new data on Medicaid expenditure growth, especially in fiscal year 2006, which ended on September 30.
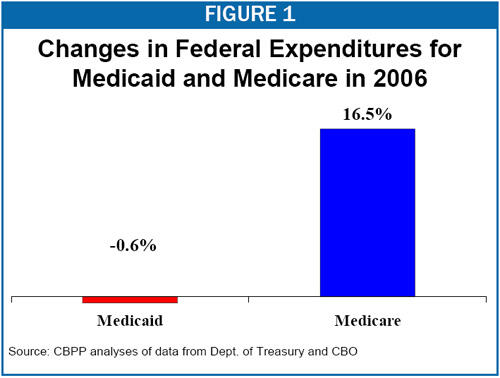
New data from the Treasury Department show that federal outlays for Medicaid were lower in fiscal year 2006 than in 2005 even in nominal dollars (i.e., even without adjusting for inflation). Federal Medicaid expenditures were $180.6 billion in 2006, as compared to $181.7 billion in 2007. Federal Medicaid costs declined by 0.6 percent in 2006 and came in well below expectations. (In March, the Congressional Budget Office projected a 4.5 percent increase in federal Medicaid expenditures in 2006.)
In contrast, federal Medicare expenditures rose 16.5 percent in 2006 (see Figure 1).[1] It should be noted, however, that a one-time factor pushed Medicaid expenditures down and Medicare expenditures up in 2006 — the implementation of the Medicare prescription drug benefit in January 2006, which shifted some costs from Medicaid to Medicare.
-
Starting in January, costs for prescription drugs for people enrolled in both Medicaid and Medicare — the “dual eligibles” — shifted from Medicaid to Medicare. This reduced the amounts that Medicaid spends while increasing what Medicare pays. If we adjust the expenditure estimates for 2006 to net out the effects of this shift, then total federal Medicaid expenditures are seen to have risen by 3.3 percent between fiscal years 2005 and 2006.[2] This is a more accurate measure of the underlying growth of health care costs in Medicaid. Compared to typical growth rates in costs for health care programs or private health insurance, however, this 3.3 percent growth rate is still quite low.
-
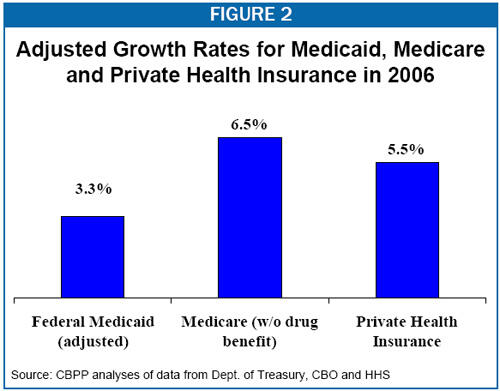
Similarly, the apparent rate of Medicare cost growth in 2006 was exaggerated by the introduction of the Medicare drug benefit in 2006, which produced a one-time surge in cost growth in 2006. If the rise in Medicare drug benefit costs is excluded, the growth in other Medicare expenditures — which better reflects increases in underlying Medicare costs — was 6.5 percent.[3]
Private health insurance expenditures are estimated to grow about 5.5 percent in calendar year 2006.[4] As shown in Figure 2, after adjustments to remove the one-time downward effect on Medicaid costs of the new prescription drug benefit, Medicaid expenditures are seen to have grown in 2006 at about half the rate that costs grew for Medicare and private health insurance.[5]
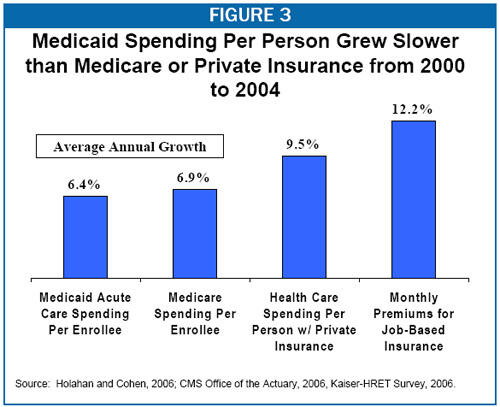
The relatively low growth of Medicaid expenditures in 2006 is not a new phenomenon. Between 2000 and 2004, Medicaid expenditures per beneficiary grew more slowly than expenditures per beneficiary in Medicare or private health insurance, as Figure 3 shows. (Aggregate Medicaid expenditures rose more quickly between 2000 and 2004 than in 2005 or 2006 because Medicaid enrollment was climbing during the economic downturn and the ensuing, initially weak recovery. In comparison, enrollment in Medicare changed little during that period, and private health coverage declined as employer-based insurance eroded.)
Because states pay a substantial fraction of Medicaid costs, they have strong incentives to hold Medicaid costs down. An analysis by economists at the Urban Institute estimated that it costs Medicaid about 30 percent less to cover an adult than it would cost if the same person were covered by private health insurance.[6] In part, this is because Medicaid’s payment rates to health care providers are typically lower than those paid by Medicare or private health insurers. In addition, state Medicaid programs typically use an array of cost containment approaches, including managed care, disease management, utilization review, prospective payment systems and the substitution of generic prescription drugs for brand name drugs. Many of these cost containment initiatives were pioneered as reforms in state Medicaid programs and have been adopted more aggressively in Medicaid than in Medicare or the private sector.[7]
Medicaid expenditures rose slowly in fiscal year 2006 in part because the number of enrollees apparently grew slowly in 2006. A survey of Medicaid directors conducted for the Kaiser Commission on Medicaid and the Uninsured suggests that national Medicaid enrollment grew only 1.6 percent in state fiscal year 2006 (which usually ran from July 1, 2005 to June 30, 2006), about one-fourth as much as the average growth rate in enrollment of 6.9 percent per year from 2000 to 2004.[8] This is consistent with recent Census data showing that there was no appreciable growth in Medicaid enrollment last year.[9]
Enrollment may have grown slowly because the number of low-income people financially eligible for Medicaid did not increase. After several years of economic growth, the number of people with incomes below the poverty line stopped rising in 2005. Medicaid enrollment also may have slowed because of eligibility reductions instituted by a handful of states — including Missouri, Tennessee, Mississippi, Florida and Ohio — and the accumulated impact of actions in a broader number of states where certain procedures that tend to impede Medicaid enrollment were instituted, such as shortening enrollment periods or increasing paperwork requirements.[10]
The effects of the slowing of Medicaid enrollment growth can be seen in the latest data on the number of Americans who are uninsured. Because employer-sponsored health insurance coverage continued to erode while Medicaid enrollment grew only slightly, the number of Americans who are uninsured rose to an all-time high in 2005.[11]
Other factors also may have contributed to the slow growth in Medicaid costs in 2006, although the detailed expenditure and enrollment data needed to analyze these factors are not yet available:
-
In recent years, states implemented a wide array of cost containment initiatives to reduce Medicaid costs per enrollee, such as disease management programs, expanded use of managed care and new drug cost containment policies. [12] Some of these policies may have generated savings that materialized more fully in 2006.
-
The Federal Medical Assistance Percentage — the federal Medicaid matching rate — fell in 29 states in 2006, while rising in 9 states. This held down federal costs and shifted a slightly higher share of costs to states. The Federal Funds Information for States estimates that this reduced federal outlays by about $0.5 billion in 2006.[13]
-
Federal expenditures also may have been held down as a consequence of greater federal scrutiny of states’ Medicaid financing mechanisms (e.g., intergovernmental transfers). This may have shifted some costs to states or to health care providers.
It should be noted that the Deficit Reduction Act, enacted in February 2006, had virtually no effect on Medicaid expenditures in 2006, since few of its provisions were in effect during the 2006 fiscal year.
As with federal Medicaid expenditures, there was no growth in state Medicaid expenditures in 2006, excluding the “clawback” payments that states began making to the federal Medicare program in conjunction with the shift of certain prescription drug costs from Medicaid to Medicare. (The “clawback” payments are not considered Medicaid expenditures.) Considered together with rising revenues in most states, this meant that Medicaid became slightly more affordable in most states.[14] (If the state clawback payments are added to state Medicaid expenditures, combined state expenditures for these purposes rose by 3.3 percent in 2006, as discussed in the box on page 4. This is considerably less than the rate of growth in state revenues; state tax collections in the July 2005 to June 2006 period averaged 8.5 percent higher than in the prior year.[15])
The Treasury data cited above contain information only on federal outlays and not the amounts spent by states, which constitute almost half of total Medicaid expenditures. The preliminary estimates cited here of state Medicaid expenditures and total (i.e., state plus federal) Medicaid expenditures are based on the expenditure estimates that states reported to the federal government in August 2005 and August 2006, one month before the end of each federal fiscal year.[16]
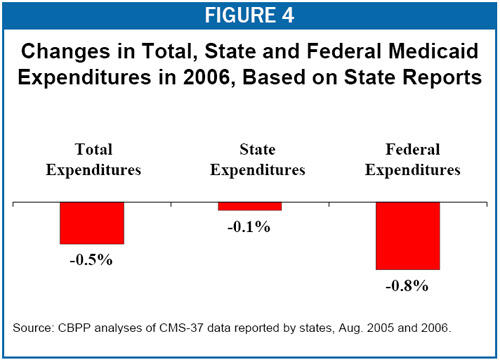
Total Medicaid expenditures were 0.5 percent lower in federal fiscal year 2006 than in 2005, while state-level expenditures in 2006 were 0.1 percent lower, as Figure 4 indicates. Using this data source, federal Medicaid expenditures fell by 0.8 percent in 2006.[17] (One reason for the slight discrepancy between the percentage decline in federal expenditures and the percentage decline in state expenditures is that the federal Medicaid matching rate fell in 29 states in 2006, shifting a small portion of total costs from the federal government to states.)[18]
The figures reported here for state Medicaid expenditures do not include an estimated $4.8 billion in “clawback payments” that states were required to pay to the federal government in fiscal year 2006.* The Medicare prescription drug legislation required that in 2006, states pay the federal government 90 percent of the amount they would otherwise have spent providing prescription drugs to “dual eligibles” under Medicaid, in order to help defray the federal government’s costs for the new Medicare drug benefit. Although state clawback payments are not counted as Medicaid expenditures, states often link them to Medicaid in state budgets. If state clawback payments are added to state Medicaid expenditures, combined state expenditures rose by 3.3 percent in 2006.
* This is based on the estimate of $6.6 billion owed by states in calendar year 2006, adjusted to reflect the fact that only nine months of calendar year 2006 coincide with federal fiscal year 2006.
While Medicare expenditure growth nationally was slightly negative in 2006, the patterns vary by state. Estimated total Medicaid expenditures fell in 22 states in 2006, while rising in 29 states. These variations are due to differences in economic conditions and Medicaid policies across the states.
Medicaid expenditures are likely to climb at a slightly faster pace in 2007. Recent projections of Medicaid growth in 2007 issued by the Congressional Budget Office, the Office of Management and Budget, the Kaiser Commission on Medicaid and the Uninsured, and the National Association of State Budget Officers range from 4.2 percent to 7.4 percent growth. These projections center around 5 percent growth in 2007.
Federal and state Medicaid expenditure growth was low in 2006, and growth rates are expected to remain relatively modest in 2007, compared to the growth rates of earlier years. In addition, the severe state budget pressures of 2001–2004 have eased for the time being because of higher state revenues as well as reduced Medicaid growth. Economists have noted that overall health care cost growth has eased at least temporarily.”[19]
At some point, however, health care costs are expected to start rising again at a more rapid rate than the rate at which the economy is growing. There consequently are good reasons to be concerned about projected long-term growth in Medicaid expenditures.
It is important to remember, nonetheless, that the growth rate in Medicaid expenditures has been comparable to — and of late, more moderate than — the growth rates for expenditures for Medicare and private-sector health care coverage. The underlying fiscal and economic problem is not that Medicaid expenditures uniquely will rise a great deal; it is that health care costs in the U.S. health care system as a whole are rising rapidly and are expected to continue doing so indefinitely, and that the U.S. population is aging and older people have higher health care costs than younger people do.
Most Americans expect to receive quality medical care and long-term care and look forward to having access to medical advances that will prolong life and improve health. These medical advances generally add to costs. Addressing the twin phenomena of escalating health care costs and high health care expectations is a problem that cannot be solved primarily through Medicaid. It ultimately will have to be addressed as part of a broader national effort to reform the overall U.S. health care system.[20]