- Home
- Health Reform Is A Good Deal For States
Health Reform Is a Good Deal for States
Contrary to claims that the health reform law’s Medicaid expansion will place an unaffordable burden on states, the federal government will shoulder nearly all of the cost of the expansion, which will cover 16 million low-income children and adults while raising state Medicaid spending by just 1.25 percent compared to what states were projected to spend without health reform. And health reform as a whole, by greatly expanding health coverage, will result in some reduction in states’ costs for providing care to the uninsured.
Federal Government Will Assume Vast Majority of Medicaid Expansion Costs
Currently, Medicaid covers many low-income individuals but leaves many others out. It generally doesn’t cover childless adults unless they are pregnant, over age 65, or have serious disabilities. It also leaves out many low-income parents. In the median state, working parents can’t receive Medicaid if they earn more than 64 percent of the poverty line, about $14,000 for a family of four.
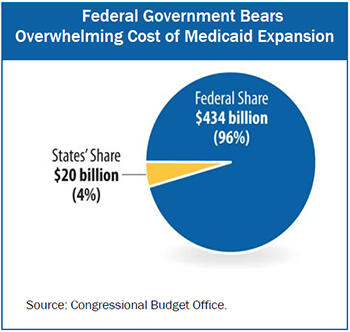
To minimize the financial burden on states, the federal government will pay 96 percent of the cost of expanding Medicaid over the next ten years (see Figure 1). This is much higher than the federal government’s normal share of Medicaid costs (57 percent, on average.
The Medicaid expansion will cost states $20 billion over the next decade, increasing their overall Medicaid spending by 1.25 percent compared to what they were projected to spend in the absence of health reform. This includes the cost of covering individuals who already are eligible for Medicaid, currently are uninsured, and are expected to enroll when the expansion is implemented.
A recent study conducted by the Urban Institute for the Kaiser Commission on Medicaid and the Uninsured has similar findings. According to the study, the federal government will finance 95 percent of the cost of the Medicaid expansion over the next 10 years. While Medicaid enrollment will increase by 27.4 percent, state costs will only increase by 1.4 percent relative to what they would have spent. [1]
Health Reform Will Reduce States’ Costs for Providing Care to Uninsured
The health reform law as a whole will cut the number of uninsured Americans by 32 million, according to the Congressional Budget Office. By dramatically shrinking the ranks of the uninsured, the law will lighten the burden on states of providing health care to their uninsured residents.
State and local governments spend more than $10 billion a year to care for the uninsured in hospitals, and provide around $15 billion a year in funding to mental health agencies that serve many of the uninsured. Those costs will drop considerably under health reform, offsetting part of the increase in state Medicaid spending. (In the first full year of Massachusetts’ health reform initiative, state spending to care for uninsured residents fell by 38 percent.) Urban Institute researcher John Holahan notes that states’ savings from no longer having to finance as much of the cost of providing uncompensated care to the uninsured may fully offset the small increase in Medicaid costs resulting from the Medicaid expansion. [2]
Health reform will also bring other, broader benefits to states. Not only will millions of uninsured low- and middle-income residents gain coverage, but market reforms will improve access to health insurance for people at all income levels. In addition, the infusion of federal funds for the Medicaid expansion and the subsidies for people to purchase private coverage should help protect newly insured state residents from preventable illnesses and result in a healthier workforce.
Critics Exaggerate Costs of Medicaid Expansion
Some states that have complained about the cost of the Medicaid expansion have overstated the likely increase in Medicaid enrollment under health reform.
For example, a study that Indiana commissioned estimated that Medicaid enrollment would jump by 495,000. But Census data show the state has only 264,000 uninsured people who could newly qualify for Medicaid under the new law.
Florida’s Agency for Health Care Administration also released an inflated estimate of the cost of expanding Medicaid. It assumed that 100 percent of eligible people would enroll in Medicaid, even though no other means-tested program has ever achieved anything close to 100 percent participation, and the Congressional Budget Office estimates that the participation rate will remain significantly below 100 percent.
In short, the Medicaid expansion will enable states to cover millions of low-income residents who haven’t been able to afford coverage, and the federal government will pick up 96 percent of the tab over the coming decade, making this a good deal for states.
End Notes
[1] John Holahan and Irene Headen, “Medicaid Coverage and Spending in Health Reform: National and State-by-State Results for Adults at or Below 133% FPL,” Kaiser Commission on Medicaid and the Uninsured, May 2010.
[2] The Urban Institute estimates of the cost to states of the Medicaid expansion do not take into account the savings to states from no longer having to subsidize the same level of uncompensated care. Kaiser Family Foundation, Transcript for Briefing on “Medicaid Expansion in Health Reform: National and State Estimates of Coverage and Cost,” May 26, 2010.
