CDC DATA SHOW MEDICAID AND
SCHIP PLAYED A CRITICAL COUNTER-
CYCLICAL ROLE IN STRENGTHENING HEALTH INSURANCE COVERAGE
DURING THE ECONOMIC DOWNTURN
by
Leighton
Ku
| PDF of full report |
| If you cannot access the files through the links, right-click on the underlined text, click "Save Link As," download to your directory, and open the document in Adobe Acrobat Reader |
The Centers for Disease Control and Prevention (CDC) have released data from the National Health Interview Survey for 2002 and the first quarter of 2003 that document significant changes in Americans’ health coverage during the recent economic downturn.
- The number and percentage of children and of non-elderly adults with private health insurance coverage decreased between 2001 and 2002. The percentage of children with private coverage fell from 66.7 percent in 2001 to 63.9 percent in 2002; for adults, it slipped from 73.7 percent to 72.3 percent. These reductions were largely the result of rising unemployment and rising health insurance costs, which made it more difficult for workers and their dependents to maintain private health insurance coverage. Preliminary data for the first quarter (January to March) of 2003 indicate levels in early 2003 were essentially unchanged from 2002.
- In response to these economic challenges, the number and percentage of children and non-elderly adults covered by public health insurance — primarily Medicaid or the State Children’s Health Insurance Program (SCHIP) — increased in 2002. The percentage of children covered by public programs rose from 23.6 percent in 2001 to 27.1 percent in 2002. The percentage of non-elderly adults covered rose from 9.4 percent to 10.3 percent.
- About 2.5 million more children and 1.6 million more non-elderly adults had health insurance coverage in 2002 because Medicaid and SCHIP expanded during the economic downturn. In other words, the number of people without health insurance would have been about four million larger if public insurance coverage had not expanded to meet the surge in need to offset much of the drop-off in private coverage.
- Among children, the increase in public insurance coverage completely offset the drop-off in private insurance coverage. The percentage of children without insurance declined from 11.0 percent to 10.5 percent, although the change was not statistically significant. Preliminary data suggest the percentage of uninsured children continued to decline in the first quarter of 2003, primarily due to continued increases in public coverage.
- The percentage of low-income children (those with incomes below 200 percent of the poverty line or about $30,520 for a family of three) who were uninsured has declined. This continued a longer trend that began after the SCHIP was created in 1997 of increases in the number and percentage of low-income children with health insurance. Between 1997 and the first quarter of 2003, the percentage of uninsured low-income children dropped by about one-third, signaling a major success in public policy efforts to reduce the number of uninsured children in the United States.
- By contrast, among non-elderly adults, the growth in public coverage was not large enough to offset the loss of private coverage. The percentage of adults without health insurance rose from 18.3 percent in 2001 to 19.1 percent in the first quarter of 2003.
During the economic downturn, Medicaid has played an important role as a “counter-cyclical” program that expands to meet rising needs when the economy is weak. Medicaid also continued to address other important needs, such as providing medical and long-term care to low-income elderly and disabled beneficiaries, a population whose needs are less affected by the business cycle.
Medicaid’s ability to cover more uninsured, low-income people when the economy weakened is directly related to its structure as an entitlement program. Had federal funding been capped under a block grant, states would not have had the financial resources to meet the additional demands of the large number of people who lost private insurance coverage or fell into poverty as a result of the economic slump. If Medicaid and SCHIP had not been able to respond by expanding enrollment in 2002, the number of uninsured Americans would have been several million larger.
Trends from the National Health Interview Survey
The National Health Interview Survey (NHIS) is a nationally representative survey conducted by the National Center for Health Statistics, an arm of the CDC. Since last year, CDC has been making preliminary data from the survey available to the public more rapidly. These CDC reports are generally available sooner than data about health insurance coverage from the Census Bureau’s better-known Current Population Survey.
Table 1 summarizes data from the CDC report.[1] The percentage of children with private health insurance coverage dropped from 66.7 percent in 2001 to 63.9 percent in 2002. There appeared to be a slight rebound in private coverage in the first quarter of 2003, but the change was not statistically significant.[2] The loss or private coverage was offset by growth in public insurance coverage, which rose from 23.6 percent in 2001 to 27.1 percent in 2002 and a further apparent, but not statistically significant, rise in the first quarter of 2003. Overall, the trend indicates a significant reduction in the percentage of children who are uninsured through the first quarter of 2003.
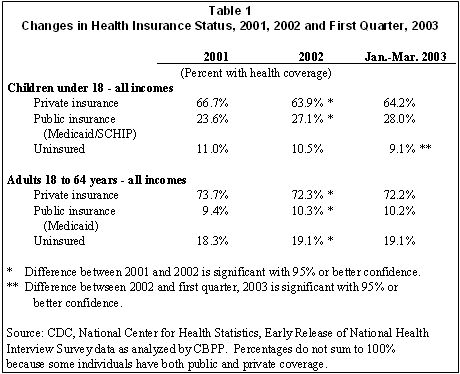
Likewise, the share of non-elderly adults with private health insurance coverage slipped from 73.7 percent in 2001 to 72.3 percent in 2002. This was partially offset by an increase in public coverage, which rose from 9.4 percent to 10.2 percent. Despite the growth in Medicaid coverage of adults, the overall story here is that the percentage of non-elderly adults who were uninsured grew from 18.1 percent in 2001 to 18.8 percent in 2002. The picture has remained the same in the first quarter of 2003.
These changes in the number of people covered by public insurance occurred in the absence of major changes in eligibility for Medicaid or SCHIP. Few states increased eligibility for either program in 2002 or early 2003, although some states simplified procedures for enrollment or renewal of children’s health insurance. The changes in enrollment in public coverage appear to have been driven primarily by economic changes that occurred between 2001 and 2002, such as increases in the number of people with low incomes and increases in the number of people unable to obtain private insurance coverage.
As seen in Table 1, a larger share of children are covered by public programs than adults, and children’s enrollment in public programs grew more in 2002 and early 2003 than adults’ enrollment did. A key reason is that eligibility for public insurance coverage for children is generally far more generous than for adults and states have made it easier for children to enroll. In 2003, for example, the income eligibility limit for children in a median state is 200 percent of the poverty line ($30,520 for a family of three) while the corresponding median income limit for a parent is only 71 percent of the poverty line ($10,800 for a family of three), a level about one-third as high as for children.[3] In addition, relatively few states provide coverage for non-disabled childless adults, no matter how poor they are.
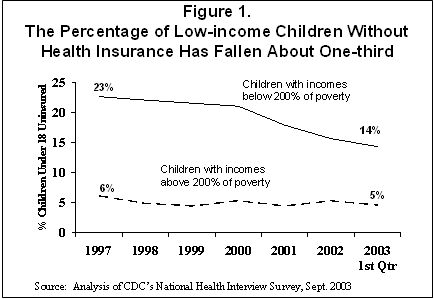
The growth in public insurance coverage of children that occurred recently is a continuation of a multi-year effort to expand health insurance coverage among low-income children. Congress enacted the SCHIP program in 1997, and the percentage of low-income children who are uninsured has fallen by about one-third since then, as shown in Figure 1. In comparison, there has been little change in insurance coverage for higher-income children.
The reduction in the ranks of uninsured low-income children is attributable not only to enrollment in SCHIP (which primarily serves children with incomes between 100 and 200 percent of the poverty line), but also to efforts to improve and simplify enrollment of children in Medicaid (which primarily serves children with incomes below the poverty line). These trends mark a major public policy success and a successful effort by health policy-makers to lower the number of children with health insurance coverage. These findings have been corroborated by recent analyses by researchers from the Urban Institute who also report significant reductions in the number of low-income children who are uninsured.[4]
The Census Bureau just released findings from its Current Population Survey that the number of Americans without health insurance rose from 41.2 million in 2001 to 43.6 million in 2002.[5] The new Census results about health insurance coverage trends are similar to those of CDC; both surveys show private health insurance coverage has fallen during the economic downturn, but this reduction was fully offset by expansions in public insurance coverage of children and partially offset by expansions in public coverage of adults.
What Would Have Happened If Public Coverage Had Not Grown?
Three economic factors combined to push down private insurance coverage in 2002. First is the economic downturn, propelled in part by the tragic events of September 11, 2001. The average civilian unemployment rate rose from 4.7 percent in 2001 to 5.8 percent in 2002. Many of those who became unemployed — and their dependents — lost employer-sponsored health insurance coverage. Second, private health insurance costs escalated rapidly, growing an average 12.7 percent higher in 2002.[6] In response to these rising costs, many businesses have raised premiums, deductibles or other cost-sharing for employees, so that fewer employees can afford private health insurance. And, third, some small businesses stopped offering health insurance, largely because of the skyrocketing costs.
The data for the first quarter of 2003 suggests that lack of health insurance coverage among adults remains a problem. Unemployment levels remain high and private health insurance costs continue to soar, rising 13.9 percent in 2003.[7] It appears that the percentage of children who are uninsured continued to decline in the first quarter of 2003, primarily because public insurance enrollment continued to grow.
If public insurance coverage had not expanded in response to the surge in needs, millions more low-income Americans would have been uninsured. If the percentage of children and non-elderly adults covered by Medicaid or SCHIP had remained the same in 2002 as in 2001, there would have been 1.6 million fewer adults and 2.5 million fewer children covered by public insurance.[8] (This NHIS-derived estimate that four million more people were covered by public programs in 2002 is close to administrative data showing that Medicaid covered about 3.2 million more people in June 2002 than in June 2001 and that SCHIP programs covered about 0.6 million more children, not including those already counted as Medicaid beneficiaries in Medicaid-SCHIP expansion programs, in 2002 than 2001.[9]) Most of the four million additional people covered would have been uninsured had it not been for the availability of Medicaid and SCHIP.
Medicaid’s Responsiveness Related to Its Entitlement Status
Covering more people costs more money. As a result of both rising enrollment and rising per capita health care costs, Medicaid expenditures rose more than 13 percent between 2001 and 2002.[10] Because Medicaid is structured as an entitlement program, federal funding levels automatically grow when there is greater need. The federal government matches actual state Medicaid expenditures; federal funding to a state is not capped by some predetermined grant limit. (This also means that, in better times, when state Medicaid expenditures are lower than expected as a result of gains in employment and income, the federal government realizes savings, as well.)
The funding flexibility offered by an entitlement is particularly important during economic downturns when Medicaid expenditures must accommodate increased needs, or when other unanticipated emergencies arise. For example, the attacks of September 11th resulted in dramatic changes in New York City’s Medicaid program that would probably not have been possible if federal funding were capped under a block grant. Not only did the September 11th tragedy cause economic dislocation and lead to the unemployment of tens of thousands of New Yorkers, but it also destroyed New York City’s Medicaid eligibility computer systems, making it impossible to process applications for health insurance. Medicaid officials acted promptly to create a temporary, simplified system to enroll people in Medicaid, called Disaster Relief Medicaid, in response to the increased demands for insurance coverage and the inability to process applications in the usual system.[11] This temporary system, which ran from late 2001 through 2002, provided an emergency response to an unanticipated crisis and also required additional funding, that might not have been available if federal funds for New York’s Medicaid program were capped under a block grant.
If funding for Medicaid had been capped under a block grant, as proposed by the Bush Administration earlier this year, the program almost certainly could not have been as responsive as it was in 2002 in meeting the needs to cover more uninsured low-income Americans. Data from other social programs provide evidence regarding how entitlement programs respond in a counter-cyclical fashion to meet increased demands for aid when the business cycle has turned down. In Medicaid and the Food Stamp Program — both entitlements — enrollment has grown in response to higher needs.[12] In contrast, caseloads in the TANF block grant have been falling despite the poor economy and high unemployment levels,[13] and limited funding for child care from TANF and the Child Care Block Grant is leading to reductions in the number of children in working families who receive child care assistance.[14]
Conclusions
The data from the CDC survey show that private health insurance coverage declined substantially during the downturn of 2002 and remain low (in historical terms) in early 2003. But this was largely offset by increases in coverage from Medicaid and SCHIP. The net effect is that the overall number of uninsured low-income children actually has declined, while the number of uninsured adults rose, but much less than it would have otherwise. The CDC data indicate that about 2.5 million more children and 1.6 million more non-elderly adults had coverage because the percentage of people covered by public programs rose in 2002.
Meeting these higher health coverage needs costs more money but is a worthwhile investment. A recent report by the Institute of Medicine, part of the National Academy of Sciences, noted the value to the nation of health insurance coverage: “The economic vitality of the country is diminished by productivity lost as a result of the poorer health and premature death or disability of uninsured workers.” The report also points out that the poorer health of children and adults may contribute to higher expenditures for Medicare, Social Security Disability and the criminal justice system, because of the increased toll of poor physical and mental health that can occur when people lack health insurance coverage.[15]
A large number of studies from economists and researchers around the nation also has shown that Medicaid is a good investment for states and creates economic activity and jobs. State investments in Medicaid draw down federal matching funds, and the combination of state and federal funds provides income to local hospitals, clinics and other health care providers, who use these funds to make purchases and pay their employees. One study estimated that on average in 2003, a $10 million investment of state funds in Medicaid generates $34 million in economic activity in the state and supports 370 jobs.[16]
The CDC data document the contribution that Medicaid and SCHIP made in maintaining health insurance coverage in 2002. This trend is likely to have continued into 2003: unemployment levels remain elevated, and health care costs continue to rise at double-digit rates. This suggests there will be further reductions in private health insurance coverage this year and that the need for greater Medicaid and SCHIP coverage will continue. Preliminary estimates from states indicate that Medicaid enrollment will grow about 7.8 percent in FY 2003.[17] The 2003 growth rate is lower than the level in 2002, but is still relatively high and demonstrates the continuing response of Medicaid enrollment to the weak economy.
In response to state concerns about budget shortfalls during the current economic downturn and difficulties in meeting increasing Medicaid costs, Congress enacted state fiscal relief measures earlier this year, including a temporary increase in the federal Medicaid matching rate and $10 billion in other fiscal grants to states. These measures are helping states facing budgetary difficulties in 2003 and 2004. Many states have been able, with these funds, to avert or lessen the severity of Medicaid cutbacks that they otherwise would have instituted and that would have further increased the ranks of the uninsured.[18] Moreover, the fiscal relief legislation gives states an incentive to avoid restricting Medicaid eligibility from September 2003 through June 2004; states that restrict eligibility during that period would lose most of the additional federal Medicaid funds.
This federal fiscal relief expires in mid-2004. State budget outlooks remain dire in many states, and unemployment remains high. If state budget conditions and general employment growth do not improve significantly before the fiscal relief ends and the fiscal relief is not extended until a stronger economic recovery takes hold, larger cuts in the provision of health insurance coverage through Medicaid could begin being implemented about a year from now.
End Notes:
[1] Centers for Disease Control and Prevention, National Center for Health Statistics, Early Release of Selected Estimates Based on Data from the January-March 2003 National Health Interview Survey, September 30, 2003 (available at www.cdc.gov/nchs/about/major/nhis/released200309.htm). This report includes data from the first quarter of 2003. It also makes technical changes in the estimates for earlier years because CDC revised the survey weights to correspond with the 2000 Census.
[2] Because data for the first three months of 2003 are based on a sample size that is about one-quarter of a full year’s sample, estimates for the quarter are less accurate than for the full year and are more subject to sampling error. The statistical significance tests shown in Table 1 compensate for the differences in the precision of full-year vs. quarterly data.
[3] Donna Cohen Ross and Laura Cox, Preserving Recent Progress on Health Coverage for Children and Families: New Tensions Emerge, Kaiser Commission on Medicaid and the Uninsured, July 2003.
[4] Genevieve Kenney, Jennifer Haley and Alexandra Tebay, “Children’s Insurance Coverage and Service Use Improve,” Snapshots of America’s Families No. 1, Urban Institute, July 2003.
[5] Robert Mills, Health Insurance Coverage in the United States: 2002, Current Population Reports P60-223, U.S. Census Bureau, September 2003. A key difference between the insurance measures of the NHIS and those of the Current Population Survey is that NHIS asks whether a person has insurance coverage at the time of the interview, and interviews are conducted continuously throughout the year. The Current Population Survey is conducted in March and asks whether a person had insurance at any time during the prior year. The 2002 NHIS thus reports insurance status at a point in time during 2002, while the March 2003 Census data report whether a person had any insurance during calendar year 2002.
[6] Kaiser Family Foundation and Health Research and Education Trust, “Employer Health Benefits: 2002 Summary of Findings,” August 2002.
[7] Kaiser Family Foundation and Health Research and Education Trust, “Employer Health Benefits: 2003 Summary of Findings,” August 2003.
[8] The estimates were computed by multiplying the increase in the percentage covered by public insurance between 2001 and 2002 by the number of adults and children in 2002.
[9] Eileen Ellis, et al. Medicaid Enrollment in 50 States: June 2002 Data Update, Kaiser Commission on Medicaid and the Uninsured, July 2003. Centers for Medicare and Medicaid Services, “Fiscal Year 2002 Number of Children Ever Enrolled in SCHIP — Preliminary Data Summary,” January 2003.
[10] The growth in Medicaid expenditures was only partially caused by enrollment growth and only a relatively small share of the expenditure increase was related to growth in enrollment of children and non-elderly, non-disabled adults. A larger share of the increases in Medicaid expenditures is attributable to the rising costs of care for elderly and disabled beneficiaries, including both higher costs per capita for those beneficiaries and higher enrollment. See Leighton Ku and Matthew Broaddus, “Why Are States’ Medicaid Expenditures Rising?” Center on Budget and Policy Priorities, January 13, 2003.
[11] Michael Perry, New York’s Disaster Relief Medicaid: Insights and Implications for Covering Low-income People,” Kaiser Commission on Medicaid and the Uninsured and United Hospital Fund of New York, August 2002.
[12] Joseph Llobrera, “Food Stamp Caseloads Are Rising,” Center on Budget and Policy Priorities, forthcoming revision, September 2003.
[13] U.S. Department of Health and Human Services Press Release, “HHS Releases Data Showing Continuing Decline In Number Of People Receiving Temporary Assistance,” Sept. 3, 2003 and Shawn Fremstad, “Falling TANF Caseloads Amidst Rising Poverty Should Be a Cause for Concern,” Center on Budget and Policy Priorities, revised Sept. 5, 2003.
[14] Sharon Parrott and Jennifer Mezey, “New Child Care Resources Are Needed to Prevent the Loss of Child Care Assistance for Hundreds of Thousands of Children in Working Families,” Center on Law and Social Policy and Center on Budget and Policy Priorities, July 15, 2003.
[15] Institute of Medicine, National Academy of Sciences, Hidden Costs, Value Lost: Uninsurance in America, executive summary, June 2003.
[16] Families USA, Medicaid: Good Medicine for State Economies,” Jan. 2003. At least ten state-specific reports about the economic impact of Medicaid have been conducted by economists and researchers in the past two years. For information about these state studies, please contact the author of this analysis.
[17] Vernon Smith, et al., States Respond to Fiscal Pressure: State Medicaid Spending Growth and Cost Containment in Fiscal Years 2003 and 2004: Results from a 50 State Survey, Kaiser Commission on Medicaid and the Uninsured, September 2003.
[18] Vernon Smith, et al., op cit.