HOW MANY LOW-INCOME
MEDICARE BENEFICIARIES IN EACH STATE
WOULD BE DENIED THE MEDICARE PRESCRIPTION DRUG BENEFIT
UNDER THE SENATE DRUG BILL?
By
Leighton Ku
| PDF of
this report
Related Report:
Press Release: |
| If you cannot access the files through the links, right-click on the underlined text, click "Save Link As," download to your directory, and open the document in Adobe Acrobat Reader. |
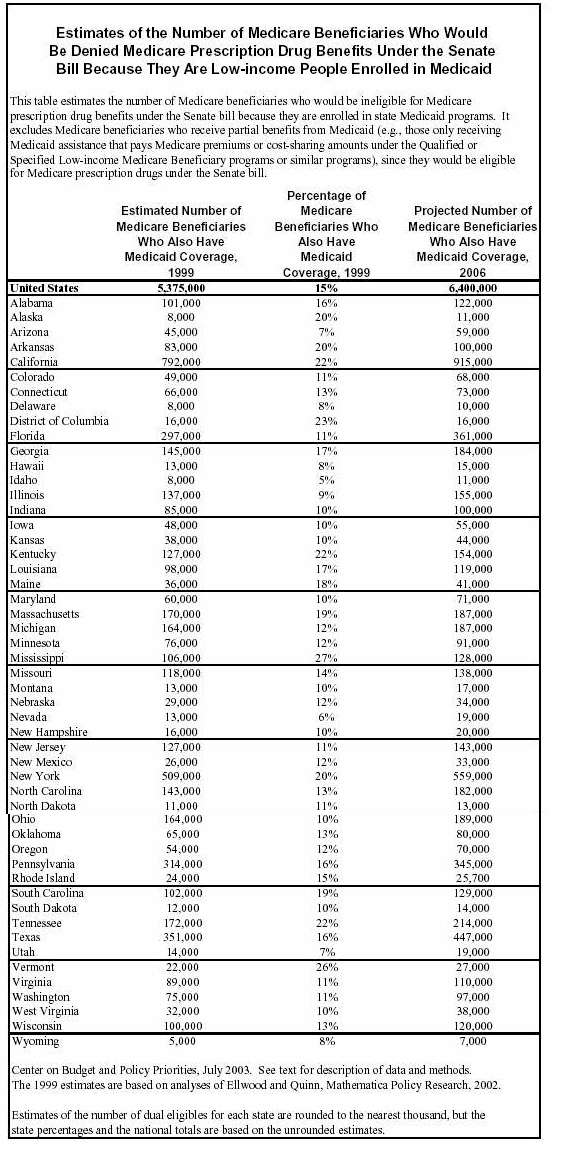
Contrary to longstanding Medicare principles under which all elderly and disabled beneficiaries are provided access to Medicare’s basic package of health care benefits, the prescription drug bill the Senate has approved would bar low-income beneficiaries from receiving Medicare’s prescription drug benefit if they also are enrolled in Medicaid.[1] Such a policy would affect millions of low-income seniors and people with disabilities eligible for both Medicare and Medicaid, a group that is known as the “dual eligibles” and that includes the poorest individuals whom Medicare serves. The Congressional Budget Office (CBO) has estimated that in 2006, when the Medicare prescription drug benefit would be implemented, this Senate provision would exclude 6.4 million low-income Medicare beneficiaries from the new drug benefit.
The millions of low-income Medicare beneficiaries who would be blocked from
eligibility for the Medicare drug benefit would receive prescription drug
coverage solely through Medicaid. By contrast, all other Medicare
beneficiaries would receive drug coverage through Medicare. The
differences are significant. Many state Medicaid programs impose limits
on the availability of prescription drugs in order to reduce their Medicaid
expenditures. As a consequence, many low-income Medicaid beneficiaries
likely would not have access to the same range of prescription drugs as their
more affluent peers.
Under the
Senate bill, states would continue to bear a major share of the cost of
prescription drugs for those low-income Medicare beneficiaries who also are
enrolled in Medicaid. These individuals would receive drug coverage through
Medicaid, and states pay an average of 43 percent of Medicaid benefit costs.
As a consequence, the Senate bill would create a perverse incentive for some
states to pare back Medicaid eligibility.[2]
By scaling back Medicaid eligibility, these states would lower their Medicaid
expenditures and shift prescription drug costs for people who would lose
Medicaid eligibility to Medicare, and hence to the federal government.[3]
The low-income seniors and people with disabilities who would no longer be
eligible for Medicaid would receive prescription drug coverage through
Medicare, but they could lose coverage for vital services that only Medicaid
covers, such as home and community-based care, nursing home care, and acute
care services such as vision, dental and hearing services.
The Medicare prescription drug legislation the
House of Representatives has approved contains a number of provisions that
raise serious concerns, including inadequate premium and cost-sharing
subsidies for low-income elderly and disabled people, dubious privatization
proposals and costly tax provisions that are largely unrelated to Medicare and
prescription drugs. However, the House bill maintains the longstanding
principle of the universality of Medicare benefits by ensuring that all
beneficiaries, including the dual eligibles, are eligible for the Medicare
drug benefit.
House and
Senate conferees have the opportunity to adopt the House provision providing
universal Medicare benefits, while adopting other, more beneficial provisions
from the Senate bill. Taken together, such changes would ensure that millions
of the poorest Americans have access to Medicare prescription drug benefits in
the future.
State-by-State Estimates This analysis provides estimates of the number of low-income
elderly and disabled Medicare beneficiaries in each state and the
The 1999 estimates are based primarily on analyses by
Under
both the Senate and House bills, the Medicare prescription drug benefit
would not be implemented until 2006. By that time, the number of
dual-eligible beneficiaries will be considerably larger. CBO projects there
will be 6.4 million such beneficiaries in 2006, a figure 19 percent greater
than the estimate for 1999. We trended the 1999 state estimates forward to
generate state projections for 2006, based on both Census Bureau projections
of changes in each state’s elderly population and the CBO estimate that there
will be 6.4 million dual eligibles in 2006.
Under the Senate bill, thousands of low-income Medicare
beneficiaries in every state would be denied the Medicare prescription drug
benefit. We project that 100,000 or more Medicare beneficiaries would be
ineligible for the Medicare drug benefit (in 2006) in 23 states. These states
are: 1999 Estimates. None of the standard Medicaid statistical
reports identify the number of dual eligibles. The Ellwood/Quinn estimates are
based on analysis of administrative data from the Medicaid Statistical
Information System (MSIS) for the first quarter of 1999, which includes
millions of eligibility records from nearly all states in the nation.[5]
Their detailed analyses help separate those dual eligibles who are “full” dual
eligibles from those who have Medicaid coverage just for Medicare cost-sharing
(i.e., Medicaid pays their Medicare cost-sharing charges but provides no other
coverage).[6]
Under the Senate bill, people with full Medicaid coverage would be ineligible
for the Medicare prescription drug benefit. Those covered through Medicaid
for Medicare cost-sharing only would be eligible for the Medicare drug
benefit.
Two
technical problems arise with the MSIS data. First, in many states, the
specific status of some dual eligibles cannot be determined from these data;
it is not clear in these cases whether the individual was a full dual eligible
or a “partial” dual eligible (i.e., an individual with Medicaid coverage only
for the Medicare cost-sharing charges). We examined data from states with a
very low proportion of these “unknown” cases and found that in these states,
an average of 87.5 percent of all dual eligibles were classified as full
dual eligibles. In the four states where the portion of “unknown” cases
was high ( The Ellwood/Quinn study also lacked data on the overall number of
dual eligibles in a few states ( Data on the number of Medicare beneficiaries in each state are based on CMS
data on the number of Medicare Part B enrollees in each state in 1999. 2006 Projections. To project the number of dual eligibles
in each state in 2006, we trended the 1999 estimates forward, using the CBO
estimate of 6.4 million full dual eligibles as a national target.
State-specific trend factors were based on Census Bureau projection of changes
in the number of persons 65 or older in each state.[8]
We prorated the growth rates the Census Bureau has projected so that the 2006
state estimates sum to 6.4 million at the national level. The actual number of dual eligibles in each state in 2006 will
vary from these estimates because of demographic, economic or policy changes
that will occur over the next few years, but these projections provide a
credible approximation of the number of people who would be affected when the
Medicare prescription drug benefit takes effect in 2006, if the Senate’s
approach of excluding full dual eligibles is adopted.
End Notes:
[1] For a more detailed
discussion, see
[2]
As of 2001, the Medicaid eligibility criteria for seniors and people with
disabilities in 19 states were broader than the federal minimum Medicaid
eligibility criteria. The federal minimum income limit for Medicaid for
the elderly and disabled is only about 74 percent of the poverty line for
an individual. Most of the 19 states with broader eligibility criteria
extend Medicaid coverage to elderly and disabled people with incomes
between 74 percent and 100 percent of the poverty line. National
Association of State Medicaid Directors, Aged, Blind and Disabled
Eligibility Survey,
[3] States could find shifting such costs to the
federal government particularly attractive because a key factor driving
state Medicaid expenditures upward is the rising cost of care for seniors
and people with disabilities, which is attributable in large part to gaps
in Medicare coverage for services such as prescription drug costs and
long-term care. Because of these gaps in Medicare coverage, Medicaid has
been bearing an increasing share of the total costs of health coverage for
seniors and the disabled, while Medicare’s share has been falling over
time. See Leighton Ku, “The Medicaid-Medicare Link: State Medicaid
Programs Are Shouldering a Greater Share of the Costs Of Care for Seniors
and People with Disabilities,” Center on
[4] Marilyn Ellwood and Brian
Quinn, “Background Information on Dual Eligibles in MSIS, FY 1999,”
[5]
These 1999 MSIS data are the most recent data that have been published to
date. The Urban Institute is now analyzing 2000 MSIS data and may release
enrollment estimates at some point.
[6] The “partial dual
eligibles” include groups such as Qualified or Specified Low-income
Medicaid Beneficiaries (QMBs and SLMBs). These are beneficiaries for whom
Medicaid pay some or all of the Medicare cost-sharing expenses.
Individuals who receive more limited Medicaid coverage would be eligible
for Medicare drug benefits under the Senate bill.
[7] The underlying assumption
is that most state data systems can typically identify partial dual
eligibles, such as QMBs or SLMBs, because these groups receive far fewer
benefits than full dual eligibles, but sometimes have problems
distinguishing between specific categories of full dual eligibles, who
receive more similar benefits. Thus, the unknown groups are nearly all
full dual eligibles whose specific Medicaid eligibility codes are missing.
[8] Census Bureau, Population
Projections for States by Selected Age Groups and Gender: 1995 to 2025,
2003.