IMPROVING RURAL PARENTS' HEALTH
INSURANCE COVERAGE:
A FACT SHEET
Lack of health insurance is a serious problem in rural America. Expanding coverage not only would benefit the low-income rural residents who would gain insurance, but also would strengthen the overall rural health system by increasing health care providers' revenues, thereby helping other rural residents.
The proposal to expand coverage for parents would provide funding to states to help insure parents, in a fashion similar to the provision of funds to states under the State Children's Health Insurance Program (SCHIP). It would be an important step in reducing problems of uninsurance and poor access to health care in rural areas. The National Rural Health Association recently noted that an important strategy to improve the rural health care system is to "expand insurance coverage for the poor and near-poor. . . . It seems appropriate that, in this time of great national prosperity, further reducing the ranks of the uninsured would be a top national policy priority."(1)
Rural Residents Are More Likely to be Uninsured; Many Rely on Public Insurance
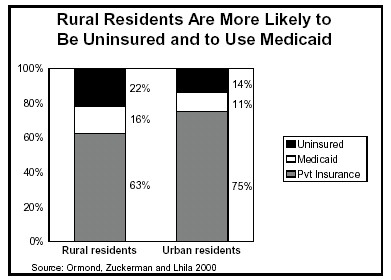 A study from the Urban Institute found that 22 percent of people under age 65
in rural areas were uninsured, compared to 14 percent of urban residents.(2)
Moreover, people in rural areas were less likely than urban residents to see a doctor or
nurse.
A study from the Urban Institute found that 22 percent of people under age 65
in rural areas were uninsured, compared to 14 percent of urban residents.(2)
Moreover, people in rural areas were less likely than urban residents to see a doctor or
nurse.
Many rural residents work in agriculture, forestry, fishing, or related industries that are less likely to offer private employer-sponsored health insurance than other industries, like manufacturing. Many rural residents have multiple part-time or seasonal jobs, which also lowers job-related coverage.(3) In addition, average incomes generally are lower in rural areas than in urban ones, depressing insurance coverage.
The difficulties in securing employer-sponsored insurance make public programs like Medicaid and SCHIP all the more important for low-income rural residents. The Urban Institute study found that one-sixth (16 percent) of non-elderly people living in rural areas obtained insurance through Medicaid or similar state programs, compared to 11 percent of urban residents. People living in rural areas are already familiar with public insurance programs and could readily take advantage of expanded public coverage.
Increasing Insurance Coverage Can Strengthen the Rural Health Care System
Increasing insurance coverage among low-income families can increase revenues for rural hospitals, clinics, physicians, dentists, and other health care providers. In so doing, it can reduce the burden of providing uncompensated care (such as treating uninsured persons) and help ensure that providers can continue to serve other patients, including those on Medicare and those with private insurance.
States Could Adopt Policies to Make It Easier to Enroll Rural Families
The parent expansion proposal would help states expand coverage of low-income parents under their Medicaid or SCHIP programs. Since the states would earn the "enhanced" federal matching rate for coverage expansions, it would cost them much less than if they expanded coverage as a regular Medicaid expansion. With the enhanced federal match, a state's share of expenses is 30 percent less than under its regular Medicaid match. For example, under a Medicaid expansion, Montana would pay 27 percent of the total cost; with the enhanced match, the state's share would fall to 19 percent. New Hampshire, a more prosperous rural state, would pay 50 percent of the total cost under Medicaid, but just 35 percent with an enhanced match.
In addition, states have the flexibility to adopt other policies that would make it easier to enroll rural families, such as eliminating asset tests for families. Farm families often are ineligible because their savings are too high after the crops are sold, even though the savings are depleted later in the year, or because they own vehicles that exceed the prescribed value, but are still needed because of their rural locale.
States also could make it easier to apply for health insurance by permitting mail-in applications and not requiring face-to-face interviews, so people do not need to travel to the welfare or other eligibility office. Since rural areas often have few eligibility offices, low-income families sometimes must travel long distances to apply.
References
1. National Rural Health Association, "The Need for Responsive Rural Health Delivery Systems," Kansas City, MO, July 2001.
2. Barbara Ormond, Stephen Zuckerman, and Aparna Lhila, "Rural/Urban Differences in Health Care Are Not Uniform Across States," Assessing the New Federalism Brief B-11, Urban Institute, May 2000. In these analyses, "urban" refers to people living in metropolitan areas, which include both cities and their suburbs; "rural" refers to those in non-metropolitan areas that are not adjacent to metropolitan areas.
3. National Rural Health Association, "Access to Health Care for the Uninsured in Rural and Frontier America," Kansas City, MO, 1999.