Medicaid Spending: Rising Again, but
Not to Crisis Levels
by Leighton Ku and Jocelyn Guyer
Overview and Summary
| View PDF version If you cannot access the file through the link, right-click on the underlined text, click "Save Link As," download to your directory, and open the document in Adobe Acrobat Reader. |
State and national policymakers are expressing concern about reports that the pace of Medicaid spending increases is rising again after a four-year lull. This analysis examines the dimensions of the projected increases in Medicaid costs and the factors behind these anticipated cost increases.
The latest projections from the Congressional Budget Office (CBO) forecast that federal Medicaid expenditures will rise at an annual rate of growth of 8 percent to 9 percent over the next several years. This exceeds the rate of increase in Medicaid expenditures over the past few years, but is below the program's average annual expenditure growth rate of 11 percent between 1980 and 2000.
Over the short term, a portion of the projected growth can be attributed to adoption by a number of states of "creative financing arrangements," which allow a state to recycle federal Medicaid funds into its general revenue fund and use them for any purpose, including purposes unrelated to health care. Analyses of the CBO estimates indicate that greater use by states of creative financing arrangements resulted in $1.8 billion in increased federal expenditures last year, an amount more than twenty times larger than the increase in expenditures attributable to growth in the number of children in Medicaid (and nine times larger than the growth attributable to the combined number of children and adults added to the caseload). In a recent report, CBO called the increased use of creative financing arrangement the "most notable" factor behind federal Medicaid spending growth last year. CBO projects that creative funding arrangements, which accounted for about one-fifth of the increase in federal Medicaid expenditures in 2000, will account for a substantial share of the increase in federal Medicaid costs again in 2001, but not in years after that.
Creative financing arrangements push up federal Medicaid expenditures while sparing (and in some cases, reducing) state expenditures. As a result, federal Medicaid costs have been rising faster than state costs. Data from the National Association of State Budget Officers indicate that while federal Medicaid expenditures rose 7.3 percent during state fiscal year 1999, Medicaid expenditures financed from state general funds grew 5.6 percent. (Figures sometimes cited as representing increases in state Medicaid expenditures that count funds used in creative financing arrangements as state costs — even though these funds typically do not come from state general funds and do not represent true costs to a state — tend to overstate growth in state Medicaid expenditures.)
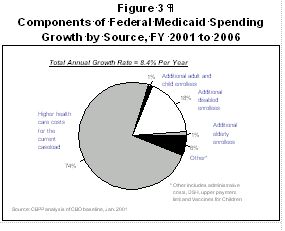
Over the longer run, the key factors underlying the projected growth in Medicaid expenditures are increased utilization of health services and health care inflation, including increases in the cost of prescription drugs. Analyses of the CBO estimates indicate that nearly three-fourths of the projected increase in federal Medicaid expenditures over the next five years will be attributable to these factors. The remaining one-fourth of the projected increase in federal costs is due to all other factors combined, including increases in enrollment, growth in administrative costs, and higher payments to disproportionate share hospitals.
In this respect, the expected trends in Medicaid spending mirror trends in private-sector spending on health care services. The private sector, too, has experienced significant increases in health care costs per enrollee. Medicaid appears to have been moderately more successful than the private sector in holding down such costs in recent years. Medicaid spending per beneficiary increased by four percent between 1999 and 2000, compared to an 8.3 percent increase in the cost of premiums for employer-based coverage. Private health insurance expenditures are expected to continue to outpace Medicaid spending growth through 2003.
The Role of Enrollment Increases Among Children and Parents
Some states have reported that a substantial share of their recent Medicaid spending growth has resulted from enrolling more children in coverage. Analyses of the new CBO projections, however, indicate that this is not a significant factor behind the projected increases in Medicaid expenditures nationally, nor will enrollment of more parents be a large factor.
Specifically, the new estimates anticipate that six percent of the increase in federal Medicaid expenditures during the current year will be attributable to the enrollment of more children (and an additional two percent due to increases in the number of adults enrolled). CBO projections show states will add 900,000 children and 200,000 adults to coverage in fiscal year 2001, but this new enrollment will cause federal Medicaid expenditures to rise only 0.8 percent. CBO also anticipates that after fiscal year 2001, enrollment of children in Medicaid will remain largely flat, while enrollment of adults will increase modestly. In combination, increased enrollment by these groups by is expected to cause Medicaid expenditures to increase an average of just 0.1 percent per year between fiscal years 2001 and 2006.
Medicaid Costs for the Elderly and Disabled
Care for disabled and elderly beneficiaries is expected to have a much more powerful effect on Medicaid expenditure growth, both because those beneficiaries are considerably more expensive to serve on average and because the number of disabled beneficiaries is expected to grow faster than the number of other types of beneficiaries. Nearly three-quarters of the projected increase in federal Medicaid spending from 2001 to 2006 — 74 percent — is related to the provision of health care to disabled and elderly beneficiaries. CBO estimates show that more than half of the total increase in Medicaid expenditures in these years will result from higher average health care costs per enrollee for the current number of disabled and elderly beneficiaries, while about one-fifth of the overall increase in Medicaid costs will be due to the cost of serving additional elderly and disabled beneficiaries.
One issue that is not expected to have significant impact is the imposition of federal mandates. Hardly any new mandates have been added in recent years.
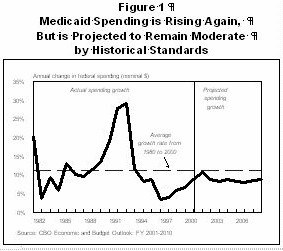
Projected Medicaid Expenditure Growth
On January 31, 2001, CBO released its new "baseline" projections for federal Medicaid spending. The baseline reflects CBO's estimates of how much Medicaid will cost the federal government over the next several years in the absence of any policy changes. As Figure 1 shows, CBO projects the rate of Medicaid expenditure growth will rise from 8.7 percent in federal fiscal year 2000 to 10.6 percent in 2001 and then return to 8.7 percent for 2002. After 2002, CBO estimates the annual growth rate will remain in the range of eight to nine percent per year.(1)
Many state-level projections also forecast a rise in the rate of growth of Medicaid expenditures. This has led a number of state policymakers to voice warnings about their Medicaid budgets.(2) It also is one reason the nation's governors recently called for a restructuring of Medicaid.(3) In a recent survey by the National Conference of State Legislatures, about half of the states cited higher-than-expected Medicaid spending or Medicaid shortfalls as an important legislative issue for their 2001 legislative sessions.(4)
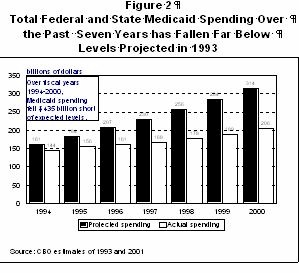
Medicaid Spending Is Much Lower Than Once Projected; Lower-than-expected Medicaid Costs Have Contributed to the Federal Budget Surplus The growth in Medicaid expenditures in recent years has been much more modest than seemed possible several years ago. Estimates that CBO issued in 1993 projected that the federal government and the states together would spend $1.6 trillion on Medicaid from 1994 to 2000. Cumulative federal and state Medicaid spending for this period was more than $400 billion below that projected level and federal spending alone was almost $250 billion below the earlier projection. Indeed, despite the resurgence in Medicaid spending growth last year, total Medicaid expenditures still were $108 billion less in fiscal year 2000 than CBO had projected in 1993.
The much-lower-than-expected Medicaid expenditures contributed significantly to the overall improvement in the federal budget outlook. The cumulative level of federal budget deficits and surpluses for fiscal years 1994 through 2000 was $2.3 trillion better than CBO had predicted in 1993. The reduction in Medicaid expenditures, as compared to the expenditure levels CBO had projected in 1993, accounted for 11 percent of this improvement. Lower-than-expected Medicaid expenditures thus played a significant role in the movement from federal budget deficits to budget surpluses, in conjunction with a stronger-than-expected economy, higher-than expected revenues, and policy changes (especially changes in the 1993 budget reconciliation act). Source: Congressional Budget Office, The Economic and Budget Outlook: Fiscal Years 1994-1998, Jan. 1993. |
New Projections Follow Several Years of Unusually Low Growth Rates
The new, higher growth rates in Medicaid have generated concern partly because they follow a four-year period of low Medicaid spending increases. From 1995 to 1999, federal Medicaid spending increased an average of 4.9 percent annually. Federal and state officials hoped these low growth rates would continue.
This 4.9 percent rate of growth, however, was well below the historic rate of increase in federal Medicaid expenditures. Between 1980 and 2000, federal Medicaid expenditures rose an average of 11.2 percent annually. In this context, the current projection of 8.4 percent average annual growth from fiscal year 2001 to fiscal year 2006 seems relatively moderate, although it is well above the growth rates of the past few years. While some have expressed concern that Medicaid spending growth may be approaching a crisis, the projected spending increases are not close to those of the early 1990s, when Medicaid expenditures grew very rapidly.
What Is Driving the Projected Rise in Medicaid Expenditure Growth Rates?
To understand the relative importance of different factors in shaping Medicaid expenditure growth, we examined the components of Medicaid spending growth from 2001 to 2006, using CBO's projections. CBO projects that federal Medicaid spending will be $64 billion higher in 2006 than in 2001 (in nominal dollars, not adjusted for inflation). As Table 1 shows, total federal Medicaid spending is projected to rise an average of 8.4 percent annually. Changes in the cost of providing health benefits to the current caseload will, by themselves, increase costs by an average of 6.2 percent per year. That is, CBO projections indicate that the higher costs related to health care inflation and changes in health service utilization for the current number of recipients will be responsible for almost three-quarters (74 percent) of the total Medicaid expenditure increase. In contrast, spending growth related to additional enrollees will average only 1.7 percent per year. This is just one-fifth of the total growth in cost, with almost all of that growth being due to projected increases in the number of disabled enrollees. Changes in other costs, such as administrative expenses, upper payment limit arrangements, disproportionate share hospital (DSH) payments and Vaccines for Children, will add 0.5 percent more in expenses per year, which is equivalent to 6 percent of the total growth. These data are shown in Figure 3.
The Increasing Cost of Providing Health Care Services
As shown above, the principal reason that Medicaid expenditures are expected to rise is the escalating cost of providing health care services, including changes both in utilization and in the price of health services. This problem is not confined to Medicaid: the rate of health care spending has begun to increase in both the public and private sectors. According to the Kaiser Family Foundation's annual survey of employer health benefits, between 1994 and 1998, the United States enjoyed the lowest rate of increase on record in the cost of employer-based health insurance.(5) Then, in 1998, the pace of cost increases began to grow again, as costs jumped 3.7 percent from the preceding year. From the spring of 1999 to the spring of 2000, premiums increased an additional 8.3 percent. In fact, Medicaid appears to have been moderately more successful than the private sector in recent years in holding down the cost of serving beneficiaries. Medicaid spending per beneficiary increased by 4 percent between 1999 and 2000, compared to the 8.3 percent increase in the cost of premiums for employer-based coverage.(6) The Health Care Financing Administration's (HCFA's) national health expenditure projections also indicate that medical expenditures for private health insurance will continue to grow faster than Medicaid expenditures through 2003.(7)
 The
increase in per-person health care expenditures is probably attributable to changes in
both health care utilization and health care prices. Because of the expansion of Medicaid
managed care, in which states pay monthly capitation fees to managed care firms,
distinguishing the effects of increases in utilization from the effects of increases in
price is not possible.
The
increase in per-person health care expenditures is probably attributable to changes in
both health care utilization and health care prices. Because of the expansion of Medicaid
managed care, in which states pay monthly capitation fees to managed care firms,
distinguishing the effects of increases in utilization from the effects of increases in
price is not possible.
One reason for the resurgence of health care inflation in both Medicaid and the private sector is that cost containment measures that began to be instituted in the mid-1990s are now largely in place. Turning to managed care may yield savings for employers and publicly-financed programs initially but does not necessarily slow the long-term rate of expenditure growth. In addition, payment rates to health care providers and managed care firms could be held down for a certain period, but now providers and health plans are demanding higher payments to "catch up" after years of low payments and some financial losses.(8)
| Category of Spending | Average
Annual Projected Growth in Medicaid Expenditures, |
||
Average Annual Increase in Costs Related to Serving the Current Caseload |
Average Annual Increase in Cost from Serving Additional Enrollees |
Total |
|
| Health Benefit Costs for Aged Enrollees |
1.8% 2.8% |
0.1% 1.5% |
1.9% 4.3% |
| Subtotal, Health Benefit Costs | 6.2% |
1.7% |
7.9% |
| Other Costs Administrative expenses, DSH, upper payment limit arrangements, Vaccines for Children) |
0.5% |
0.5% |
|
| Total Average Annual Expenditure Growth (total increase of $64 billion) |
6.7% |
1.7% |
8.4% |
Higher Prescription Drug Costs
Increases in outpatient prescription drug expenditures are a major reason that Medicaid costs are expected to increase significantly. HCFA projects that Medicaid prescription drug expenditures will rise about 70 percent faster than overall Medicaid expenditures between 2001 and 2006.(9)
Analyses by the Urban Institute have found significant increases both in the use and price of medications, particularly by aged and disabled Medicaid beneficiaries.(10) Since Medicare — the other major federal health insurance program for senior citizens and many disabled people — does not cover prescription drugs, the increasing cost of prescription drugs for aged and disabled people who are enrolled in both Medicaid and Medicare falls heavily on Medicaid. In 1998, prescription drug expenditures rose 15 percent in fee-for-service Medicaid, while estimated drug expenditures in Medicaid managed care rose 47 percent. Overall, Medicaid prescription drug costs rose 20 percent in 1998, more than three times the six percent increase in Medicaid expenditures for other kinds of health benefits that year. (On the other hand, it is possible that more effective use of prescription drugs may help reduce medical costs, by reducing the severity of diseases or the risk of hospitalization. This analysis examines prescription drug costs only and does not include possible offsetting reductions in other medical costs.)
The spiraling cost of prescription drugs fuels overall health care costs, not just those of Medicaid. One recent study estimated that 44 percent of the increase in private health insurance premiums in 1999 was due to rising prescription drug costs.(11)
The Rising Cost of Covering Disabled and Elderly Beneficiaries
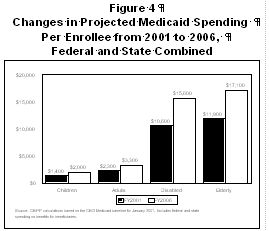
Under CBO's baseline, it is clear that the increasing cost of serving disabled and elderly beneficiaries drives much of the projected growth in Medicaid spending. These groups already are much more expensive to cover than other kinds of enrollees because they tend to have significant health care needs. Over the next several years, increases in the cost of caring for disabled and elderly beneficiaries will account for the majority of projected Medicaid spending growth. Based on the CBO projections, the average cost (state and federal combined) of covering a disabled Medicaid beneficiary is expected to rise from $10,600 in fiscal year 2001 to $15,600 in fiscal year 2006. The cost of covering an elderly Medicaid beneficiary is projected to increase from $11,900 to $17,100 during this period. In comparison, the average cost of covering a child on Medicaid is expected to increase from $1,400 to $2,000 (see Figure 4).
 Moreover,
CBO projects somewhat greater growth in the enrollment of disabled individuals than in the
enrollment of people in other categories, partly because of expected increases in the
number of disabled people as the baby-boom generation ages. As people age, the risk of
becoming disabled rises; in the next several years, the baby-boomers will age, but most
will still not have reached the age of 65, when Medicare will help pick up coverage. The
projections for increases in the number of disabled Medicaid beneficiaries parallel
projected changes in the number of disabled people served by the Supplemental Security
Income program. CBO projects that the number of disabled Medicaid enrollees will increase
about 3.5 percent annually from 2001 to 2006, while the number of adults and children on
Medicaid will grow one percent or less. Because of the often-costly health care needs of
disabled individuals, increases in the enrollment of such individuals will account for
almost one-fifth of the total increase in projected Medicaid expenditures from 2001 to
2006.
Moreover,
CBO projects somewhat greater growth in the enrollment of disabled individuals than in the
enrollment of people in other categories, partly because of expected increases in the
number of disabled people as the baby-boom generation ages. As people age, the risk of
becoming disabled rises; in the next several years, the baby-boomers will age, but most
will still not have reached the age of 65, when Medicare will help pick up coverage. The
projections for increases in the number of disabled Medicaid beneficiaries parallel
projected changes in the number of disabled people served by the Supplemental Security
Income program. CBO projects that the number of disabled Medicaid enrollees will increase
about 3.5 percent annually from 2001 to 2006, while the number of adults and children on
Medicaid will grow one percent or less. Because of the often-costly health care needs of
disabled individuals, increases in the enrollment of such individuals will account for
almost one-fifth of the total increase in projected Medicaid expenditures from 2001 to
2006.
Overall, higher spending for disabled and elderly beneficiaries dominates projected Medicaid expenditure growth. Figure 5 shows that spending for these two groups is responsible for 74 percent of the expected increase in federal Medicaid expenditures between 2001 and 2006. As shown in Table 1, most of this increase in cost stems from growth in the anticipated expense of serving the current number of disabled and elderly enrollees rather than from caseload growth.
Creative Financing Arrangements
 In the
short term, a significant factor behind Medicaid expenditure growth is states' increasing
use of "creative financing arrangements." These arrangements allow a state to
recycle federal Medicaid funds into the state's general revenue fund and use them for any
purpose it desires, including initiatives neither related to health care nor authorized by
Congress. Some states have opted to invest these additional federal funds in health care
initiatives, while others have used the funds to reduce the state's share of health care
expenditures.(12)
In the
short term, a significant factor behind Medicaid expenditure growth is states' increasing
use of "creative financing arrangements." These arrangements allow a state to
recycle federal Medicaid funds into the state's general revenue fund and use them for any
purpose it desires, including initiatives neither related to health care nor authorized by
Congress. Some states have opted to invest these additional federal funds in health care
initiatives, while others have used the funds to reduce the state's share of health care
expenditures.(12)
States have been able to use creative financing arrangements through either the Medicaid disproportionate share hospital (DSH) component of Medicaid or through what are known as "upper payment limit" (UPL) arrangements. Creative financing arrangements that employ DSH or UPL mechanisms use a type of "round trip" funding mechanism that can be illustrated in a hypothetical example. Consider a state with a 60 percent Medicaid matching rate that increases Medicaid payments to hospitals by $100 million but requires the hospitals to transfer $100 million back to the state Medicaid agency. Because there is a Medicaid payment of $100 million, the federal government makes $60 million in matching payments to the state. Since the state did not incur any net expenditures (because the hospitals transferred the $100 million back to the state), the state gains a windfall of $60 million in additional federal funds that it can use for any purpose. In many such cases, the arrangements ensure that the health care providers that participate receive some net increase in payments.
While the regulatory provisions for DSH and UPL arrangements differ, either approach can be designed by states to leverage additional federal funds with no additional state expenditures, through artificially high payments to health care providers coupled with a requirement that the providers transfer some or all of the money back to the state.(13) The key distinctions between UPL and DSH arrangements are: 1) that DSH payments can be made only to hospitals, while UPL payments can be made to either hospitals or nursing homes; and 2) that growth in DSH payments was curbed in the 1990s through a series of federal laws enacted between 1991 and 1997 while UPL arrangements began proliferating in the late 1990s and are only now becoming subject to more federal controls and regulations.
According to the Congressional Budget Office, UPL arrangements were the "most notable factor" behind the increase in Medicaid spending in fiscal year 2001. CBO estimates that federal spending on UPL arrangements grew $1.8 billion in fiscal year 2000, constituting about one-fifth of the total increase in federal Medicaid expenditures that year. In fiscal year 2001, UPL arrangements are again expected to play a role in driving federal Medicaid spending growth that is second only to health care inflation. CBO anticipates that federal spending on UPL arrangements will jump $1.9 billion this year, accounting for more than one-sixth of overall Medicaid spending growth.
Legislation enacted in December 2000 (the Medicare, Medicaid and SCHIP Benefit Improvement and Protection Act) requires HCFA to issue a regulation that restricts but does not terminate state UPL arrangements. As a result of the new regulation, which took effect on March 13, 2001, CBO anticipates that growth in federal payments for UPL arrangements will slow in the future, with total payments for such arrangements rising by only $400 million over the next three years, from $6.5 billion in fiscal year 2001 to $6.9 billion in fiscal year 2004. After fiscal year 2004, federal spending on UPL arrangements is expected to fall modestly and eventually level off at around $6 billion a year.(14) The new law also increased the maximum level of Medicaid DSH allotments for fiscal years 2001 and 2002 and gave states more flexibility in designing DSH arrangements in the two succeeding years. The Medicaid DSH changes will enable states to secure additional federal funding through DSH arrangements.
What Is Not Driving the Projected Rise in Medicaid Expenditure Growth Rates
Since concern about the growth in Medicaid spending tends to increase pressures to alter the program, it is important to highlight two areas that are expected to contribute relatively little to the program's growth: increasing enrollment of children in Medicaid and coping with mandates imposed by the federal government.
Increasing Enrollment of Children and Parents
Some state officials have said they believe their success in enrolling more children and expanding coverage for parents is a major source of cost increase, and a few have suggested states may need to reduce their efforts to simplify Medicaid (or SCHIP) enrollment procedures or to cover more parents. Both the historical data and the CBO projections indicate, however, that expansions of coverage for children or parents are contributing relatively little to the growth in Medicaid expenditures. Because the per capita costs of child or adult coverage are so much lower than the costs of serving elderly or disabled beneficiaries, expansions of child or adult coverage have relatively modest effects on overall Medicaid costs.
Last year, states increased the number of children in Medicaid by roughly 100,000. The number of adults in Medicaid grew 100,000, as well. Of the $9.4 billion increase in federal Medicaid expenditures that occurred in fiscal year 2000, less than one percent — about $80 million — was attributable to the cost of enrolling new children, while the cost of additional adults was about $120 million. Together, these two groups pushed overall federal Medicaid spending up by just two-tenths of one percent. In comparison, states' use of UPL arrangements increased federal spending by $1.8 billion in 2000, an amount more than twenty times larger than the increase in expenditures attributable to growth in the number of children served (and nine times the cost of additional children and adults combined).
This year, states are expected to experience greater success in enrolling additional children and adults in coverage. According to CBO, the number of children and adults on Medicaid is likely to grow by about one million people (900,000 children and 200,000 adults) in fiscal year 2001. Nevertheless, the cost of covering these new beneficiaries will represent only a small fraction of the overall growth in federal Medicaid expenditures; six percent of the total increase is attributable to the new children while two percent are due to additional adults. The new child and adult enrollees are expected to cause federal Medicaid spending to increase by less than one percent (0.8 percent), or $1 billion. The expansion of UPL arrangements is expected to cause federal outlays to increase about twice as much this year ($1.9 billion).
After fiscal year 2001, CBO anticipates the enrollment of children in Medicaid will remain largely flat and the enrollment of parents will increase modestly. (The lack of growth in the number of children on Medicaid is due to demographic projections of a slight reduction in the total number of children over the next several years). In combination, these groups are expected to cause average annual Medicaid costs between fiscal year 2001 and 2006 to increase by under one-tenth of one percent (0.1 percent) and to account for just one percent of the overall increase in Medicaid expenditures during this five-year period. (Even if states are more successful than anticipated under CBO's baseline in enrolling children or expanding parent eligibility, leading to higher-than-anticipated caseloads, this still would not have a major impact on overall Medicaid expenditure growth since the per capita costs of serving children or adults are relatively low.)
Federal Mandates
Some state policymakers have expressed the belief that federal mandates are contributing to the growth in state Medicaid spending. But the new CBO projections of more rapid growth in Medicaid spending cannot be attributed to federal mandates. Federal Medicaid policy during the second half of the 1990s was distinguished by expanded state flexibility and relaxed federally-mandated responsibilities. Examples include elimination of the Boren amendment (which affected reimbursement rates for hospitals and nursing homes), increased flexibility for states to implement Medicaid managed care and the proliferation of waivers.
Furthermore, no major mandated eligibility expansions have been imposed in recent years. The 1997 Balanced Budget Acts expanded benefits to help low-income Medicare beneficiaries meet their cost-sharing requirements, but these were fully federally funded. The last major mandatory expansion in Medicaid eligibility — covering school-aged children with incomes below the poverty line — was enacted in 1990 and is almost completely phased in. Except for a relatively small change enacted in December 2000 that revises how states must pay federally qualified health centers, recent federal legislation has contained no increases in mandated benefits or payment rates.(15)
The fact that the pace of Medicaid expenditure growth is quickening despite expanded state flexibility suggests that flexibility alone cannot contain Medicaid costs. Most of the fundamental forces that propel Medicaid expenditures — such as health care inflation, the aging of the population, and increases in the number of people who are disabled — are largely beyond the control of state or federal health officials. State flexibility is not a magic policy wand that can, by itself, still the rising budget waters.
Effects on State Medicaid Spending
How do increases in the growth rate of federal Medicaid spending affect the states? Since the federal government and the states split the cost of financing Medicaid, one might expect growth in federal Medicaid expenditures to be matched by a corresponding growth in state Medicaid expenditures. States' increasing use of creative financing arrangements can alter that relationship, however, by creating a misleading impression of increased state spending when such arrangements actually are creating a windfall for a state (see example on page 10). One indication that the use of creative financing arrangements has, in fact, led to disparities in federal-versus-state Medicaid expenditure growth comes from data gathered by the National Association of State Budget Officers. These data show that federal Medicaid expenses grew 7.3 percent in state fiscal year 1999 while the amount paid from state general funds rose 5.6 percent.(16)
Nevertheless, a large number of states are now facing Medicaid budget shortfalls — in other words, their current spending is higher than the amount appropriated. In the National Conference of State Legislatures' 2001 fiscal survey, conducted in December 2000, some 23 states and the District of Columbia reported Medicaid shortfalls or higher-than-anticipated expenditures.(17)
The other half of the states did not report such problems and are not experiencing shortfalls now. Indeed, many states are considering expansions of Medicaid or SCHIP coverage, such as expanding eligibility for parents of low-income children, eliminating asset tests for families, or making it easier for children to apply for Medicaid.
Many of the states that are experiencing Medicaid budget problems are considering three responses or a combination thereof:
1. Containing costs. Perhaps the area in which states are making the greatest effort to contain costs is prescription drug prices. Options that states are considering include: seeking supplemental rebates from drug manufacturers, shifting toward the use of generic drugs, requiring prior authorization, increasing the use of pharmaceutical benefits management firms, and reducing fees paid to pharmacists.(18) Some states also have proposed holding the line on reimbursement rates for certain types of health care providers, such as nursing homes or hospitals. In addition, several states are considering trimming optional services, such as chiropractic services or dental or vision care for adult recipients. Of greater concern, a few states are even contemplating efforts to reduce caseloads by scaling back eligibility or reducing outreach efforts. For example, the Idaho legislature recently voted to terminate child outreach funds and Florida is considering a proposal to reduce the Medicaid eligibility of pregnant women.
2. Obtaining more federal dollars. Although recent federal legislation and regulations have limited the scope of states' use of upper payment limit arrangements, a number of states have instituted such arrangements since September 2000 or have applied to do so and will collect more federal funds in 2001 and 2002.(19) States that initiated creative financing arrangements before October 1999 will be able to phase them down slowly over several years. In addition, states will be able to expand their Medicaid DSH arrangements because of the federal legislation enacted in December 2000 and to collect more federal matching funds as a result.
Texas Medicaid Budget Problems Related to Large Tax Cut and Budget Gimmick Sometimes Medicaid budget problems are caused partly by accounting gimmicks. For example, in its 1999-2001 biennial budget, Texas financed only 23 of 24 months’ worth of certain large Medicaid expenditures, shifting the obligations for the missing month into the new budget cycle. This has worsened the situation for the state’s new budget biennium, since the state now has to find funds to cover the earlier expenses, as well as meeting higher projected Medicaid expenditures for the 2001-2003 period. Like other states, Texas has been faced with escalating health care costs, including costs for prescription drugs. The leftover expenses have made it more difficult for Texas to pursue efforts to simplify the enrollment of children in Medicaid, such as permitting mail applications or extending eligibility for a full year, or to increase payment rates to health care providers, which have changed little over the past decade. State Representative Garnet Coleman explained that the decision to fund only 23 of 24 months of Medicaid costs was done to help ease the passage of a large state tax cut. State Senator Chris Harris commented that, "We made tax cuts because we thought we had this huge surplus. I might have voted a little differently on all those tax cuts had I realized that we were only funding 23 months of these programs." Source: Jim Yardley, "Some Fault Bush Tax Cuts for Lean Days in Texas," New York Times, Feb. 12, 2001. |
Also of note, the federal government has recently begun to approve waivers for states to use SCHIP funds to expand eligibility for low-income parents. Many states that have expanded health insurance coverage for parents now will be able to use SCHIP funding, which has a higher federal matching rate, for this purpose. This reduces state expenditures. Waivers recently approved for Wisconsin, Rhode Island, and New Jersey, for example, help reduce state expenditures by shifting the costs of coverage for some parents from Medicaid to SCHIP.
3. Using tobacco settlement funds or other state resources. Most states have other funds that could be used to cover their additional Medicaid costs. Each year, states will receive more than $8 billion from the tobacco lawsuit settlement. (Most of these funds are based on the multi-state settlement; the funds for Texas, Florida, Mississippi, and Minnesota are based on separate state settlements.) Much of this money — including, in some states, tobacco settlement funds from prior years — remains unallocated or is being used for purposes not related to health care.(20)
In February, the National Conference of State Legislatures reported that revenue projections for two-thirds of the states were at or above prior targets. While many states are projecting higher-than-expected budget expenditures, often due at least in part to increases in Medicaid costs, most have been able to rearrange their budgets. The NCSL survey indicates that few states expected to tap their budget reserves to accommodate their fiscal needs. In fact, 18 states reported they expected to cut taxes during this legislative session.(21) Although Medicaid increases were reported as a source of concern in about half the states, state policymakers in most areas appear to be coping with the situation.
Conclusions
Despite widespread concern about the resurgence in Medicaid expenditure growth, the program is not out of control. The rate of Medicaid spending growth has increased in the past couple of years, but CBO projects that the expenditure growth rate will moderate and stabilize in the near future at a level that is below the historical average, although above the rate of growth in Medicaid expenditures in the latter half of the 1990s.
Most of the recent and projected growth in Medicaid expenditures is driven by the same factors that the private sector confronts: a resurgence in the underlying price of health services and increases in health care utilization. Like the private sector, Medicaid faces a particular challenge in responding to the growth in prescription drug costs, especially since Medicaid carries disproportionate responsibility for insuring some of the groups that rely most heavily on prescription drugs. In the short term, unlike the private sector, Medicaid also must contend with states' use of creative financing arrangements, which increase federal Medicaid expenditures without necessarily offering commensurate benefits to Medicaid beneficiaries.
Overall, the expenditure data do not demonstrate a compelling need for a radical restructuring of the program. Nor do they show that efforts to expand coverage for children or parents are leading to major increases in program costs. But the increase in the rate of growth of Medicaid expenditures is likely to change the policy and budgetary landscape for the next few years. Federal and state policymakers, who increasingly are expressing interest in shrinking the ranks of the uninsured, will need to ensure that adequate federal and state budget resources are available for Medicaid, which remains the mainstay of health insurance coverage for low-income Americans.
End Notes
1. Unless otherwise noted, all figures describing projected growth in Medicaid spending are based on the new CBO Medicaid baseline, issued in January 2001. CBO projects federal Medicaid spending at the national level. While states submit short-term projections to the federal government, they are not estimated comparably and are not typically used for policy analysis. Thus, this paper focuses on national estimates and projections, rather than the trends in individual states.
2. The federal government and the states share of the cost of financing Medicaid. Under a matching formula, the federal government reimburses states for anywhere from 50 percent to 77 percent of the cost of providing Medicaid services. The state's share of the total cost thus ranges from 23 percent to 50 percent; states with lower per capita incomes contribute less. Across the nation, states contribute an average of 43 percent of the total costs, while the average federal share is 57 percent.
3. Robert Pear, "Governors Offer 'Radical' Revision of Medicaid Plan," New York Times, February 25, 2001.
4. National Conference of State Legislatures, "State Fiscal Outlook for 2001," Jan. 4, 2001. Also see "State Fiscal Outlook for 2001: February Update," Feb. 28, 2001.
5. Henry J. Kaiser Family Foundation, Employer Health Benefits: 2000 Annual Survey, September 2000.
6. Note that comparisons between Medicaid and private insurance costs should be interpreted cautiously because Medicaid generally offers a broader benefit package (e.g., including long-term care and prescription drugs) and has lower copayments than private insurance and covers a different mix of beneficiaries.
7. Office of the Actuary, HCFA, "National Health Care Expenditures Projections: 2001-2010," March 2001.
8. Henry J. Kaiser Family Foundation, op cit., page 12. Brian Bruen and John Holahan, "Medicaid Spending Growth Remained Modest in 1998, But Likely Headed Upward," Urban Institute, Washington, DC: Kaiser Commission on Medicaid and the Uninsured, Feb. 2001.
9. Office of the Actuary, HCFA, op cit.
10. Brian Bruen, "Medicaid and Prescription Drugs: An Overview," Urban Institute, Washington, DC: Kaiser Commission on Medicaid and the Uninsured, October 2000. Also, Bruen and Holahan, op cit.
11. Christopher Hogan, Paul Ginsburg, and Jon Gabel, "Tracking Health Care Costs: Inflation Returns," Health Affairs 19(6):217-23, Nov./Dec. 2000.
12. Because of the fungibility of money, it is difficult to determine exactly how these funds are used.
13. Leighton Ku, "Limiting Abuses of Medicaid Financing: HCFA's Plan to Regulate the Medicaid Upper Payment Limit," Center on Budget and Policy Priorities, Sept. 27, 2000. Jocelyn Guyer, Andy Schneider and Michael Spivey, Untangling DSH: A Guide for Community Groups to Using the Medicaid DSH Program to Promote Access to Care, Boston, MA: The Access Project, 2000.
14. Health Care Financing Administration, "Medicaid Program; Revision to Medicaid Upper Payment Limit Requirements, Final Rule," Federal Register 66(9):3148-77, Jan. 12, 2001.
15. There are costs associated with the Supreme Court's decision in Olmstead v. L.C. (which establishes new standards for when states should provide home- and community-based care to people with disabilities) and with implementation of medical reporting standards under the Health Insurance Portability and Accountability Act of 1996. These costs are probably small and are difficult to measure.
16. National Association of State Budget Officers, 1999 State Expenditure Report, June 2000. Available at www.nasbo.org.
17. National Conference of State Legislatures, op cit.
18. Andrew Caffrey, "States Seek to Curb Medicaid Costs," Wall Street Journal, Feb. 7, 2001.
19. States that have recently been approved by HCFA for an upper payment limit arrangement or have a pending application include Alaska, Arkansas, Florida, Georgia, Illinois, Iowa, Kansas, Kentucky, Louisiana, Michigan, Missouri, Montana, New Jersey, New York, North Carolina, Pennsylvania, South Carolina, South Dakota, Tennessee, Virginia and Wisconsin.
20. For more information about tobacco settlements, see the Campaign for Tobacco-Free Kids' website (tobaccofreekids.org/reports/settlements/settlement2001.pdf).
21. Ten states expected to increase taxes, according to the NCSL survey.
 There are a
number of reasons why Medicaid spending grew more slowly than expected. These include
legislative changes to contain Medicaid disproportionate share hospital (DSH) spending,
lower-than-expected underlying health care inflation, proliferation of Medicaid managed
care efforts, a drop in the number of eligible beneficiaries (due primarily to the strong
economy), and a drop in the enrollment of eligible families with children (due primarily
to welfare reform).
There are a
number of reasons why Medicaid spending grew more slowly than expected. These include
legislative changes to contain Medicaid disproportionate share hospital (DSH) spending,
lower-than-expected underlying health care inflation, proliferation of Medicaid managed
care efforts, a drop in the number of eligible beneficiaries (due primarily to the strong
economy), and a drop in the enrollment of eligible families with children (due primarily
to welfare reform).