CONGRESSIONAL BUDGET OFFICE ESTIMATES REVEAL
SEVERITY OF MEDICAID CUTS IN HOUSE-PASSED RECONCILIATION BILL
By Edwin Park
| PDF of full report Categories: |
| If you cannot access the files through the links, right-click on the underlined text, click "Save Link As," download to your directory, and open the document in Adobe Acrobat Reader. |
|
KEY FINDINGS • The House-passed reconciliation bill would result in a net cut in Medicaid of $42.5 billion over ten years. |
Under the terms of the budget resolution, the House of Representatives was required to achieve through the reconciliation process at least $14.7 billion in savings over five years to programs under the jurisdiction of the House Energy and Commerce Committee, with at least $10 billion in savings assumed to come from the Medicaid program. On November 18,, the House of Representatives narrowly passed its overall reconciliation package. Analysis of the CBO estimates related to the Medicaid provisions of the House-passed bill reveals:[1]
-
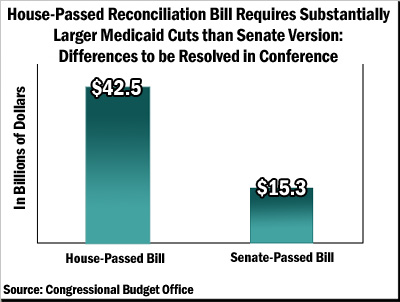
The Medicaid provisions of the House-passed bill would result in a net reduction in federal Medicaid expenditures of $8.6 billion over the next five years and $42.5 billion over 10 years (see Figure 1).[2]
-
Medicaid provisions that would either increase what low-income beneficiaries must pay out of their own pockets for health care or scale back the health care services that Medicaid covers would account for $6.4 billion in reduced federal Medicaid expenditures over five years — and $29.6 billion in reductions over ten years.[3]
-
These provisions constitute the majority — 58 percent — of the $50.8 billion in gross Medicaid cuts over ten years in the House reconciliation legislation. (Over five years, these provisions account for 50 percent of the gross Medicaid reductions.)[4]
-
By contrast, only $2.2 billion of the Medicaid savings over five years, and $8.0 billion in savings over ten years, would come from provisions to reduce Medicaid costs by moderating the prices that Medicaid pays for prescription drugs (see Figure 2). These provisions, which would not adversely affect beneficiaries, account for less than one-sixth (16 percent) of the gross Medicaid reductions over the ten-year period.
-
In addition, the House-passed reconciliation bill includes no Medicare savings whatsoever, even though the Medicare Payment Advisory Commission (MedPAC, Congress’ official expert advisory body on Medicare payments) recently recommended billions of dollars in savings by curbing excessive and unwarranted Medicare payments to managed care plans (see Figure 2).[5]
Senate Package Poses Sharp Contrast
In contrast to the House bill, the Senate-passed reconciliation bill achieved its target of $10 billion in savings from programs under the jurisdiction of the Senate Finance Committee primarily by reducing excessive payments to Medicare managed care plans and lowering the costs that Medicaid pays for prescription drugs.[6] By taking this approach, the Senate bill was able to protect vulnerable, low-income beneficiaries. In essence, the Senate saved money primarily by cutting the cost of the health care provided under Medicare and Medicaid, rather than by cutting back beneficiaries’ access to that care.
- The Senate-passed reconciliation package would reduce net Medicaid costs by $15.3 billion over 10 years, or about one-third as much as the House package (see Figure 1).[7] (Over five years, the Medicaid reductions in the Senate package would be less than half those in the House measure.) The Senate package includes no provisions to increase beneficiary cost-sharing or scale back covered health care services.
-
Instead, the Senate package would do much more than the House package to moderate prescription drug costs in the Medicaid program. CBO estimates that the Senate bill’s provisions related to Medicaid drug pricing would save $8.2 billion over five years and $24.8 billion over 10 years, triple the comparable savings in the House bill over 10 years (see Figure 2).
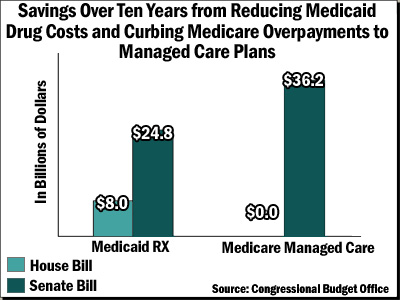
- The Senate package also includes two provisions to reduce overpayments to Medicare managed care plans, in line with the Medicare Payment Advisory Commission’s recommendations. These provisions would produce savings in Medicare of $11.9 billion over five years and $36.2 billion over ten years (see Figure 2).[8]
-
Together, the Senate’s Medicaid drug pricing provisions and its Medicare managed care plan provisions account for nearly 81 percent of the Senate bill’s gross reductions over ten years in health care entitlements. By contrast, under the House bill, the savings from moderating prescription drug prices would account for 16 percent of the gross cuts in health care entitlements, and no savings would be secured by curbing excessive Medicare provider payments.
The CBO estimates highlight the stark differences between the two measures. The House package contains much larger reductions in Medicaid and secures the bulk of these savings through provisions that would make low-income parents, children, and elderly and people with disabilities pay more to get health care services or reduce the health care services for which they are covered. Essentially, the House bill would protect managed care companies and drug manufacturers (most of the savings it does secure from lowering drug prices would come from scaling back payments to pharmacists rather than increasing the rebates that drug companies pay Medicaid), while hitting many low-income beneficiaries hard.
More than two decades ago, Ronald Reagan’s budget director David Stockman said that when cutting the budget, policymakers should focus on “weak claims,” not “weak clients” (that is, on demands on federal resources that are weak on the merits regardless of whether those claims come from powerful people, rather than on “weak clients” who are easier to cut because they lack money and influence). In passing its budget reconciliation legislation, the Senate followed Mr. Stockman’s admonition. The House-passed measure did the opposite.
End Notes:
[1] See Congressional Budget Office, “Reconciliation Recommendations of the House Committee on Energy and Commerce,” October 31, 2005; Congressional Budget Office, “Preliminary Estimate of Modifications to Medicaid Provisions of the House Energy and Commerce Committee’s Reconciliation Recommendations,” November 17, 2005; and Congressional Budget Office, “Revised CBO Estimate of Section 3105 of H.R. 4241, the Deficit Reduction Act of 2005,” December 7, 2005.
[2] This figure includes $2.5 billion in additional Medicaid funding for states to provide Medicaid coverage to survivors of Hurricane Katrina but does not include $90 million in funding provided outside of the Medicaid program for the establishment and operation of state high-risk pools.
[3] These provisions include new state options to charge premiums and increased copayments for Medicaid beneficiaries and to reduce the benefits that Medicaid covers. See Victoria Wachino, “Energy and Commerce Committee Bill Imposes New Costs on Low-Income Medicaid Beneficiaries,” Center on Budget and Policy Priorities, October 28, 2005.
[4] In addition to the $2.5 billion in temporary Medicaid funding for states directly affected by Hurricane Katrina, the House bill also includes $1.8 billion over five years and $5.9 billion over ten years in new Medicaid spending, although one spending provision in particular (for “Health Opportunity Accounts”) represents dubious policy. In any event, these additional costs are outweighed by additional beneficiary reductions from denying long-term care coverage to substantial numbers of people through changes in Medicaid’s transfer-of-asset rules. Those changes would save $2.2 billion over five years and $5.8 billion over ten years. Some of those who would be denied coverage are people of adequate means who do not need Medicaid assistance for long-term care. Many others who would be denied long-term care coverage, however, are people who are in need of such assistance and would be disqualified as a result of the more punitive, blunt-instrument approach to asset transfers that the House bill takes. See Edwin Park, “Health Opportunity Accounts for Low-Income Medicaid Beneficiaries: A Risky Approach,” Center on Budget and Policy Priorities, revised November 1, 2005. For a discussion of the risks that changes in asset transfer rules can pose if the changes are not designed carefully, see Victoria Wachino, Leighton Ku, Edwin Park and Judith Solomon, “An Analysis of the National Governors Association’s Proposals for ‘Short-Run Medicaid Reform’,” Center on Budget and Policy Priorities, October 14, 2005.
[5] For an analysis of the MedPAC recommendations, see Edwin Park, “Adopting MedPAC Recommendations to Reduce Excessive Medicare Managed Care Plan Payments Could Yield Large Budget Reconciliation Savings,” Center on Budget and Policy Priorities, October 12, 2005.
[6] See Congressional Budget Office, “Reconciliation Recommendations of the Senate Committee on Finance,” October 27, 2005 and Congressional Budget Office, “Estimated Budgetary Effects of Amendments to Title VI of S. 1932, the Deficit Reduction Omnibus Reconciliation Act of 2005, as Passed by the Senate,” November 18, 2005. The provisions related to Medicaid and Medicare in the Senate-passed reconciliation bill are estimated to reduce federal spending by $9.3 billion over five years and $53.4 billion over 10 years.
[7] This figure also includes $165 million in savings over 10 years to the State Children’s Health Insurance Program (SCHIP).
[8] One provision would eliminate the so-called “stabilization fund” to ensure that regional Preferred Provider Organizations (PPOs) are not paid more than other Medicare managed care plans. The other provision would appropriately set payment rates to Medicare managed care plans that reflect the health status of their enrollees, by phasing out the current so-called “hold harmless” policy. Both provisions were specifically recommended by the MedPAC in its June 2005 report to Congress. See Medicare Payment Advisory Commission, “Report to Congress: Issues in a Modernized Medicare Program,” June 2005.
