|
January 29, 2006
NEW CONGRESSIONAL BUDGET OFFICE ESTIMATES INDICATE MILLIONS OF LOW-INCOME BENEFICIARIES WOULD BE HARMED BY MEDICAID PROVISIONS IN BUDGET BILL
By Edwin Park
On January 27, the Congressional Budget Office issued a new analysis of the Medicaid provisions of the budget reconciliation conference agreement,[1] on which the House of Representatives is expected to vote February 1. The conference agreement, which the Senate passed 51-50 in late December with Vice President Cheney breaking the tie, includes significant changes in the Medicaid program that will affect millions of low-income beneficiaries.[2] The just-released CBO analysis finds that the bill’s Medicaid changes would have the following effects.
1. Higher Co-payments and Premiums. Under the conference agreement, states would be permitted to increase co-payments substantially and to impose premiums on many beneficiaries, including some children. CBO estimates these co-payment and premium increases would reduce Medicaid expenditures by $1.9 billion over five years and $9.9 billion over ten years. Some 70 percent of these savings would be due to higher co-payment changes, with the remainder resulting from higher premiums. According to CBO:
- Under the conference agreement, 13 million beneficiaries (20 percent of Medicaid beneficiaries) will face higher co-payments for medical services other than prescription drugs by fiscal year 2015. (CBO projects that states will impose increases in co-payments on more beneficiaries as time goes by and that the number of affected beneficiaries will rise throughout the coming ten-year period.)
- Nine million of these beneficiaries, about 4.5 million of whom are children, will face co-payment charges for the first time. (Children are exempt from co-payments under current Medicaid rules.) CBO estimates that states containing half of all Medicaid beneficiaries nationwide will impose co-payment charges for one or more health care services on beneficiaries, such as children, who currently are exempt from such charges.
- Some 20 million Medicaid beneficiaries also will face higher co-payments for prescription drugs by 2015. Children who currently are exempt from co-payments will account for about one-third of these 20 million affected beneficiaries. Almost half of the 20 million beneficiaries —nearly 10 million — will be individuals with incomes below the poverty line.
- Some 80 percent of the savings that result from the increases in co-payments will come from decreased use of medical services, rather than from collection of increased co-payments. This CBO finding is consistent with a substantial body of research, which shows that increases in co-payments lead many low-income beneficiaries to forgo needed health care services and medications.
- CBO also estimates that three-quarters of states imposing higher cost-sharing will, for the first time, allow providers to deny needed services to beneficiaries who cannot make the higher co-payments. A provision of the reconciliation bill would authorize states to take such action. Under current law, Medicaid beneficiaries who cannot make required co-payments remain financially responsible to the provider but are not denied the needed health care service or prescription drug.
- CBO also projects that some of the savings from increased co-payments and will be offset partially by higher Medicaid expenditures for emergency room visits, because some beneficiaries who are unable to make their co-payments, and who forgo needed care, eventually will have to seek emergency care.
- States will charge premiums to about 1.3 million Medicaid beneficiaries by fiscal year 2015. Most of these individuals will be adults and children. Currently, states generally cannot impose premiums for Medicaid coverage.
- Unable to afford these premiums, 65,000 individuals will lose Medicaid coverage entirely. Children will account for 60 percent of the individuals who are unable to pay their premiums and are denied Medicaid coverage as a consequence.
These estimates may understate the effects on low-income families and individuals. CBO acknowledges it is uncertain how states will respond to the new co-payment and premium options and the extent to which states will make far-reaching changes. If more states elect to increase co-payments and impose premiums than CBO has assumed, or states set the charges higher than CBO has assumed, more Medicaid beneficiaries will be adversely affected and lose access to medically necessary services and prescription drugs.
CBO’s estimates could turn out to understate the effects for another reason, as well. Previous research suggests that CBO’s projections regarding how many beneficiaries will lose coverage when premiums are imposed are conservative. CBO estimates that in 2015, about 1.3 million beneficiaries who are charged premiums for Medicaid coverage will face premiums equal to between one and three percent of their income, and that 65,000 such individuals will lose coverage as a consequence. Prior research on the effect of premiums on low-income beneficiaries in Medicaid and related health care programs indicates that premiums at these levels could lead to reductions in coverage for between 16 and 49 percent of those affected, or between 210,000 and 640,000 people.[3]
2. Reduced Benefits: The conference agreement would allow states to reduce the health care services that Medicaid covers for various beneficiaries, including many non-disabled working-poor parents. CBO estimates these provisions would result in $1.3 billion in reduced Medicaid expenditures over five years and $6.1 billion over ten years. According to CBO:
- About 1.6 million beneficiaries will have their Medicaid benefits scaled back by 2015, as a result of these provisions.
- The scaled-back benefit packages will reduce per capita health expenditures among affected adult beneficiaries by about one-third, with reductions being made in services such as dental care, vision care, mental health services, and certain therapies. Various other services will continue to be covered but be restricted in amount, duration and scope.
- As with the co-payment and premium provisions, CBO acknowledges it is uncertain how many states will opt to reduce their Medicaid benefits and to what extent. Depending on state decisions, the number of Medicaid beneficiaries who face reduced benefits could be considerably higher, especially if state budgets tighten during an economic downturn and this leads more states to impose such reductions.
- The CBO estimates do not take into account potential reductions in health care services for low-income children enrolled in Medicaid. The conference agreement permits states to provide scaled-back benefit packages to children, as long as the states that do so “wrap around” these scaled-back benefits packages with the same health care services now guaranteed to children on Medicaid under the program’s Early and Periodic Screening, Diagnostic and Treatment (EPSDT) component. This approach, however, is unlikely to work well in practice: examination of how wrap-around coverage works for children in Medicaid managed care plans shows that such coverage can be ineffective and that children in managed care often go without some needed care as a result.
3. Asset Transfer Rules: The conference agreement establishes highly restrictive asset-transfer rules for people needing nursing home care. These provisions produce savings of $2.4 billion over five years and $6.4 billion over ten years. According to CBO:
- Some 130,000 individuals, or about 15 percent of new recipients of Medicaid nursing home coverage each year, will ultimately face a delay in obtaining such coverage as a result of the new rules.
- The delays in coverage for affected recipients will range up to one year or more.
Overall CBO Cost Estimates Show How Conference Negotiators Catered to Special Interests in the Health Care Area
When the conference negotiators worked behind closed doors to secure much of the conference agreement’s health care savings through Medicaid co-payment and benefits provisions that affect low-income beneficiaries, they omitted or largely gutted a series of provisions included in the Senate-passed reconciliation bill that would have achieved substantial savings by curtailing excessive payments to Medicare managed care plans and securing better prices for Medicaid in obtaining prescription drugs.[4] Conference negotiators could have adopted those Senate provisions and significantly reduced Medicare and Medicaid expenditures without harming large numbers of beneficiaries with very limited incomes, as the Senate bill did. Instead, they elected to cater to special interests such as managed care plans and pharmaceutical companies while reducing beneficiaries’ access to care.
- The Senate-passed reconciliation package would have reduced overpayments to Medicare managed care plans by a total of $11.9 billion over five years and $36.2 billion over ten years, according to CBO. The Senate bill achieved this result through two provisions — the elimination of a $10 billion stabilization fund to encourage regional Preferred Provider Organizations (PPOs) to participate in Medicare and the phase-in of risk-adjusted payments to Medicare managed care plans. These Senate provisions would have implemented recommendations of the Medicare Payment Advisory Commission (MedPAC), Congress’ official expert advisory body on these issues. At the behest of managed care plans, however (which lobbied intensively on these issues, and which also make large campaign contributions), conference negotiators dropped the provision eliminating the stabilization fund altogether and partially gutted the risk-adjustment provision.[5] As a result, the final conference agreement includes only $6.5 billion in Medicare managed care savings over five years and $4.1 billion over ten years — $32.1 billion less in savings over ten years than the Senate-passed bill would have generated. (See Figure 1.)
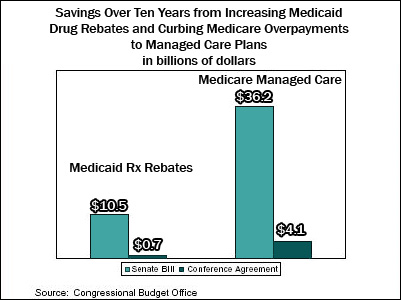
- The Senate bill also would have increased the rebates that drug manufacturers pay to Medicaid by $3.9 billion over five years and $10.5 billion over ten years. Those savings were primarily the result of two provisions: an increase in the minimum rebates that manufacturers of brand-name and generic drugs pay, and the extension of the rebates to drugs dispensed through Medicaid managed care plans. These provisions were included in the Senate bill to secure better pharmaceutical prices for Medicaid. However, the conference agreement contains only two very minor rebate provisions (which already were included in the House bill) that produce savings of just $220 million over five years and $720 million over ten years. This is $9.8 billion less in savings over ten years than the Senate bill contained (see Figure 1).
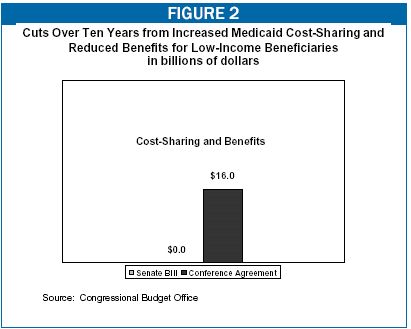
- Because the Senate bill was able to garner reasonable savings from reining in excessive federal payments to Medicare managed care plans and moderating the high charges that Medicaid now pays for prescription drugs, that bill included no Medicaid provisions that would adversely affect beneficiaries by increasing co-payments or premiums or reducing covered benefits. In comparison to the Senate bill, the conference agreement added $16 billion over ten years in Medicaid cost-sharing and benefit cuts, while dropping or sharply curtailing the Senate provisions related to drug companies and Medicare managed care plans and thereby giving up $42 billion in savings over ten years that the Senate bill included. (See Figure 2.)
- The CBO estimates show that about 75 percent of the five-year and ten-year Medicaid savings in the reconciliation conference agreement are due to provisions that directly affect beneficiaries — the provisions related to increased co-payments and premiums, reductions in benefits, the new asset transfer rules, and a provision that will cause some beneficiaries to lose coverage by requiring all U.S. citizens who apply for or receive Medicaid to produce birth certificates or passports to prove their citizenship status.
The CBO estimates highlight the stark choices that conference negotiators made. Essentially, the conference agreement protected managed care companies and drug manufacturers while adopting measures that CBO’s estimates indicate will impose hardship on millions of low-income Medicaid beneficiaries, including children, parents, elderly people, and people with disabilities.
End Notes:
[1] See Congressional Budget Office, “Additional Information on CBO’s Estimate for the Medicaid Provisions in S. 1932, the Deficit Reduction Act of 2005, January 27, 2006
[2] For an overview of the Medicaid provisions adversely affecting low-income Medicaid beneficiaries in the conference agreement, see Sharon Parrott, Edwin Park, and Robert Greenstein, “Assessing the Effects of the Budget Conference Agreement on Low-Income Families and Individuals,” Center on Budget and Policy Priorities, revised January 9, 2006.
[3] See Leighton Ku and Teresa Coughlin, “Sliding-Scale Premium Health Insurance Programs: Four States’ Experiences,” Inquiry, 36: 471-480 (Winger 1999-2000).
[4] See Parrott, Park, and Greenstein, op. cit. For the CBO cost estimates of the Medicare and Medicaid provisions of the Senate reconciliation bill, see Congressional Budget Office, “Reconciliation Recommendations of the Senate Committee on Finance,” October 27, 2005 as modified by Congressional Budget Office, “Estimated Budgetary Effects of Amendments to Title VI of S. 1932, the Deficit Reduction Omnibus Reconciliation Act of 2005,” November 18, 2005. For the final CBO cost estimates of the reconciliation conference agreement, see Congressional Budget Office, “Congressional Budget Office Cost Estimate for S. 1932, the Deficit Reduction Act of 2005,” January 27, 2006.
[5] See Parrott, Park, and Greenstein, op. cit. and Jonathan Weisman, “Closed-Door Deal Makes $22 Billion Difference: GOP Negotiators Criticized for Change in Measure on HMOs,” Washington Post, January 24, 2006. |

