Expanding Family Coverage:
States' Medicaid Eligibility Policies for Working Families in the Year 2000
by Matthew Broaddus, Shannon Blaney, Annie Dude, Jocelyn
Guyer, Leighton Ku,
and Jaia Peterson
Summary
| PDF of full report If you cannot access the files through the links, right-click on the underlined text, click "Save Link As," download to your directory, and open the document in Adobe Acrobat Reader. |
Since 1996, changes in federal law and policy have given states new opportunities to expand publicly-financed health insurance coverage to members of low-income working families with children, including parents. Nonetheless, the percentage of low-income parents who are insured by Medicaid fell by almost one-quarter from 1995 to 2000, according to Census data, and the share who are uninsured rose by 7 percent. While 12 states have substantially expanded low-income working parents' eligibility for Medicaid since 1997, income eligibility limits for parents in most states remain well below the poverty line, and about one-third of low-income parents remain uninsured. In light of the current recession, it seems likely that uninsurance rates for low-income parents will rise even further unless states are able to expand publicly-funded coverage.
Insurance coverage for low-income children, on the other hand, has improved considerably in recent years. The State Children's Health Insurance Program (SCHIP), created in 1997, offers states federal matching funds — with matching rates considerably higher than standard Medicaid rates — to expand health care coverage for children using Medicaid, a separate state children's health program, or a combination of the two. In response to this new opportunity, all states have expanded coverage for children since 1997; most states have elected to cover children in families with incomes up to 200 percent of the poverty line or higher. Census data reveal that the proportion of low-income children with publicly-funded coverage under Medicaid or SCHIP rose in 1999 and 2000 and that this resulted in a reduction in the percentage of low-income children who lack insurance coverage.
States now have a number of options to expand coverage for parents of children covered by Medicaid or SCHIP. Prior to the passage of the 1996 federal welfare law, parents usually had to receive cash welfare assistance to be eligible for Medicaid. The 1996 law created an important new opportunity for states to expand coverage for low-income working parents. Since then, modifications to federal waiver policies have created even more avenues to broaden "family-based coverage", i.e. publicly-financed coverage available to both the children and parents in low-income families. States now can cover low-income working parents who have no recent connection to cash welfare and can establish Medicaid income eligibility limits much higher than those that apply to welfare.
A growing number of states have adopted family-based expansion programs that cover parents, paralleling their coverage expansions for children under SCHIP. The expansions are designed to address the high rate of uninsurance among low-income working parents, as well as to strengthen the effectiveness of children's health initiatives. A growing body of research indicates that extending coverage to parents can increase the extent to which eligible children secure coverage and make use of needed services.
To better understand the actions states are taking to increase health insurance coverage for parents, the Center on Budget and Policy Priorities surveyed Medicaid eligibility staff in all 50 states and the District of Columbia to gather information about the eligibility rules that each state applies to families with children under Medicaid (and in a few cases, non-Medicaid public insurance programs). We asked the state officials to provide information on their policies for parents as of July 1, 2000. In some cases, the Center has learned of policy changes adopted by states since July 1, 2000; these changes are noted whenever possible. The tables in this report update and expand upon an earlier report issued by the Center on states' eligibility rules for parents as of the fall of 1999.(1)
- Prior to 1997, seven states had expanded Medicaid coverage for both parents and children to include families with incomes up to 100 percent of the federal poverty line or higher.(2) These states include Delaware, Hawaii, Minnesota, Oregon, Tennessee, Vermont, and Washington.
- Since 1997, an additional 12 states have raised income eligibility limits for parents up to or beyond 100 percent of the poverty line. These states include Arizona, California, Connecticut, the District of Columbia, Maine, Massachusetts, Missouri, New Jersey, New York, Ohio, Rhode Island, and Wisconsin.
Nevertheless, most states provide Medicaid coverage to low-income parents only if they have income far below the poverty line.
- More than half of the states provide coverage to a working parent with two children only if the parent's earnings fall below roughly $10,000 a year, an amount that leaves the family nearly $5,000 below the poverty line. In the typical (or median) state, a working parent with two children becomes ineligible for coverage when her earnings reach 69 percent of the poverty line.
- In some states, the eligibility cutoff for parents is even lower. In Alabama, for example, a parent with two children is ineligible for Medicaid if her earnings exceed $3,048 a year, an amount more than $11,500 below the poverty line.
By contrast, 37 states (including the District of Columbia) now provide coverage to children in families with income up to at least 200 percent of the poverty line.
In most states, low-income parents thus face the prospect that if they or other family members earn enough to lift their family to the poverty line, they must forego publicly-funded health insurance coverage. Since the availability of employer-based coverage at low-wage jobs is limited, poor parents who work are more likely to be uninsured than poor parents who do not work. In 2000, for example, nearly half (46 percent) of poor parents who secured most of their income from earnings were uninsured. In comparison, a little more than one-fourth (28 percent) of poor parents who relied primarily on unearned income lacked coverage.
Many states that have not broadly expanded income eligibility for parents have adopted more modest, but still significant, improvements in their eligibility rules for parents. This suggests that these states are interested in simplifying the application process for parents (as they have done for children), as well as in reinforcing the efforts of low-income parents to find and retain jobs and in improving the treatment of two-parent families.
- Sixteen states no longer administer an asset test when evaluating the eligibility of parents for Medicaid. In addition, a significant number of other states have increased the asset limit for Medicaid eligibility and/or have elected to disregard (that is, not count) the value of one car when calculating a family's assets.
- Only 12 states continue to impose the "100-hour rule," under which parents in two-parent families are ineligible for Medicaid if the principal wage earner works 100 or more hours per month. The remaining 38 states and the District of Columbia have substantially eliminated the 100-hour rule and generally treat two-parent families the same as single-parent families.
- Sixteen states have devised strategies to effectively waive the "three-out-of-six months requirement," under which families must have been eligible for Medicaid for at least three of the preceding six months to qualify for Transitional Medical Assistance (TMA). This requirement can make families that find work quickly (as the result of TANF policies aimed at promoting rapid attachment to the work force or for other reasons) ineligible for TMA.
- Fourteen states make TMA available to families for more than the mandated 12 months.
- Thirty-seven states have adopted 12-month continuous eligibility, which guarantees ongoing Medicaid eligibility for families with children for 12 months regardless of changes in income or other family circumstances in the interim.
The data in this report show that a substantial number of low-income parents lack insurance. The recent economic downturn and accompanying state budgetary problems are likely to aggravate the problem of uninsurance and to make it harder for states to address that problem by expanding Medicaid or SCHIP coverage for low-income parents.
Policy Changes in Public Coverage of Families and Children
The enactment of the State Children's Health Insurance Program (SCHIP) in 1997 gave states the opportunity to expand coverage to children in low-income families through Medicaid, a separate state children's health program, or a combination of both approaches. To give states a fiscal incentive to expand coverage for children, SCHIP increases the generosity of the federal government's contribution to the cost of covering children (i.e., the federal matching rate) relative to Medicaid.
In response to SCHIP, all states have adopted some kind of expansion in coverage for children, and 37 states (including the District of Columbia) have expanded coverage to 200 percent of the poverty level or higher.(3) As a result, nearly 95 percent of uninsured children in low-income families (defined as families with income below 200 percent of the poverty line, or $29,260 for a family of three in 2001) are income-eligible for publicly-funded coverage.(4)
Less widely recognized opportunities for states to expand coverage were created by the 1996 Personal Responsibility and Work Opportunity Reconciliation Act (PRWORA). While previously, families with children generally had to enroll in cash assistance in order to become eligible for Medicaid in most states, the 1996 welfare law "delinked" the two programs. It also gave states broad flexibility to raise the Medicaid income eligibility limits for low-income families with children (including parents) beyond old welfare levels to whatever level they consider appropriate, as well as to make other improvements in the coverage available to families with children. Even before 1996, states were required to expanded Medicaid eligibility for the children in low-income families beyond welfare levels.(5) Thus, the opportunity created by the welfare law primarily affects the extent to which the parents in low-income families with children can qualify for Medicaid.
As indicated by the tables in this report, a modest but growing number of states have expanded coverage for low-income working parents, along with their children. In most states, however, a wide disparity still exists between the eligibility rules for children and those for parents. This disparity has created a growing number of "split families," in which children may secure coverage but their parents may not. As a result of the failure to expand parent coverage along with children's coverage, the proportion of low-income working parents without insurance has remained high. In addition, new research indicates children are more likely to be enrolled in Medicaid and SCHIP if their parents also qualify, which suggests that leaving parents out of recent child health expansions may have impeded the effectiveness of these expansions in reaching uninsured children.
Insurance Coverage of Low-income Children Has Improved, While Parents' Coverage Has Worsened
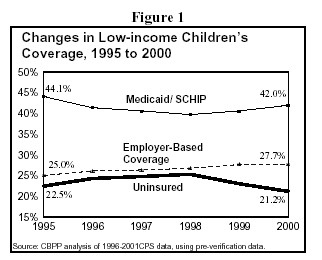
Analyses of recent data from the Census Bureau's Current Population Survey show that state efforts to expand coverage for low-income children using SCHIP funds have helped reduce the number of low-income uninsured children. However, low-income parents have lost health insurance coverage in recent years, and Medicaid coverage for parents in most states has remained quite restrictive.
Figure 1 shows that the percentage of low-income children who were uninsured rose from 1995 to 1998 but has declined since then. The primary reason for this recent improvement is the growth of Medicaid and SCHIP participation since 1998 due to SCHIP-funded expansions. The gains in coverage were concentrated among children with incomes between 100 and 200 percent of the poverty line, the income range in which children's eligibility expansions were concentrated.(6) These results demonstrate the success of state efforts to reduce the number of uninsured low-income children.
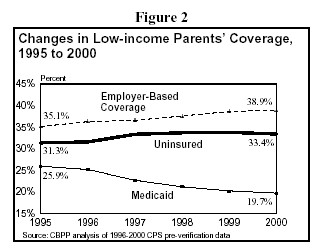
Unfortunately, public coverage of low-income parents has fallen sharply since 1995. As shown in Figure 2, the share of these parents receiving Medicaid fell from 26 percent in 1995 to 20 percent in 2000. Because of the loss of Medicaid coverage, low-income parents were significantly more likely to be uninsured in 2000 than they were in 1995 on average, despite the increase in employer-based coverage during this period.(7) About one-third of low-income parents lack health insurance coverage, a level considerably greater than the uninsurance rate for low-income children, one in five lack health insurance coverage. If the Medicaid eligibility of low-income parents had grown as extensively as that of children, it seems very likely that low-income parents' uninsurance rates would have fallen in the past couple of years instead of increasing.
The recent drop in the percentage of low-income parents enrolled in Medicaid probably has retarded efforts to enroll children in public insurance. Several analyses have demonstrated that efforts to expand parents' eligibility can stimulate greater enrollment of children.(8) These analyses also indicate that improved parent coverage can improve children's use of preventive health services.
| PDF of full report If you cannot access the files through the links, right-click on the underlined text, click "Save Link As," download to your directory, and open the document in Adobe Acrobat Reader. |
The decline in Medicaid enrollment by low-income parents was not caused by a tightening of Medicaid eligibility criteria; states generally kept their Medicaid income and resource thresholds for parents steady during this period, and sometimes increased them. The cause, rather, was a decline in participation among eligible parents, either because of heightened administrative barriers or because parents mistakenly believe they are not eligible for Medicaid if they are not getting a welfare check. Thus, the slippage in Medicaid coverage that began in the wake of welfare reform has continued.
End Notes
1. Center for Law and Social Policy and Center on Budget and Policy Priorities, State Policy Documentation Project: States' Implementation of Selected Medicaid Provisions of the Personal Responsibility and Work Opportunities Reconciliation Act of 1996, January 2000. (available at www.spdp.org).
2. Tennessee expanded eligibility in 1994 but has admitted relatively few low-income parents with incomes beyond the state's traditional Medicaid eligibility criteria in recent years.
3. Donna Cohen Ross and Laura Cox, Making It Simple: Medicaid for Children and CHIP Income Eligibility Guidelines and Enrollment Procedures, Center on Budget and Policy Priorities and Kaiser Commission on Medicaid and the Uninsured, October 2000.
4. Leighton Ku and Matthew Broaddus, Nearly 95 Percent of All Low-income, Uninsured Children Now Are Eligible for Medicaid or SCHIP, Center on Budget and Policy Priorities, September 2000. (Center reports are available at www.cbpp.org).
5. Even before PRWORA, states could provide Medicaid to a limited number of low-income families with children not receiving cash welfare. Most notably, states could establish a "medically needy" eligibility category for families with children. However, a state's income standards under this category could not exceed 133 percent of the state's AFDC income standards. Despite this constraint, in about a quarter of the states the medically needy eligibility category currently offers the most generous income standard for families with children.
6. The Census Bureau recently changed its method for counting the uninsured by adding a "verification question," which lowers the number of uninsured people. To measure insurance trends consistently from 1995 to 2000, we used the "pre-verification" version of the questions. The differences in insurance coverage patterns between 1995 and 2000 are statistically significant with 90 percent confidence. If we use the "post-verification" data, the share of low-income children who are uninsured in 2000 is slightly less, 20.1 percent.
7. As with the Census data for children, we used "pre-verification" responses to tabulate insurance trends consistently from 1995 to 2000 for parents. When the "post-verification" definitions of insurance are used, the percentage of low-income parents who were uninsured in 2000 is a little lower, 32.3 percent.
8. Leighton Ku and Matthew Broaddus, The Importance of Family-Based Insurance Expansions: New Research Findings About State Health Reforms, Center on Budget and Policy Priorities, September 5, 2000.